Matricide Related to Interferon Associated Psychosis
Mahe Vincent*, Bouthier Martin, Lucet Chloé and Fremont Patrick
Department of Psychiatry, GHEF Meaux, France
Submission: March 20, 2018; Published: April 23, 2019
*Corresponding author:Dr V Mahé, Department of Psychiatry, GHEF 6-8 Rue Saint-Fiacre, 77 100 MEAUX, France
How to cite this article: Mahe V, Bouthier M, Lucet C, Fremont P. Matricide Related to Interferon Associated Psychosis. J Forensic Sci & Criminal Inves. 2019; 11(4): 555819. DOI: 10.19080/JFSCI.2018.11.555819.
Abstract
The antiviral agent interferon is frequently associated with various psychiatric adverse reactions. Among the most severe psychiatric reactions, psychotic symptoms have been reported to appear in less than 1% of interferon treated patient, as well as homicidal attempts or thoughts. Psychotic symptoms may follow a chronic course, even after interferon treatment cessation. Only 6 cases of homicidal attempts or thoughts emerging during interferon treatment have been reported until now. In these cases homicidal concerns disappeared after interferon cessation, and no acting-out has been reported until now. We describe a first case of homicide committed by a 56 years old woman presenting a chronic psychosis during interferon treatment. Familial history of psychotic disorder and concomitant psycho-active drug abuse were associated. Our case confirms that interferon treatment may be associated with severe psychiatric reaction, even a possible personal vulnerability and a concomitant drug abuse may have played a contributing role. This demonstrates that the lack of previous personal psychotic history does not protect from severe psychiatric reaction with interferon treatment. Concomitant psychoactive drug abuse and familial history of psychotic disorder should be evaluated before interferon treatment initiation. Psychiatric care must be continued until significant clinical improvement, even after cessation of interferon treatment. Life-threatening persecutory ideas and misidentification delusion should draw attention for severe behavioural reactions. Key points Interferon treatment is associated with various psychiatric adverse reactions. Severe psychiatric reactions include psychosis and homicidal concerns. We report the first case of psychosis and homicide related to interferon treatment. Psychosis persisted after interferon treatment cessation. Precautions before initiation and after cessation of interferon treatment are suggested.
Keywords: Homicide; Interferon; Psychosis; Drug abuse; Misidentification; C hepatitis; Misidentification
Introduction
The antiviral combination of interferon alpha (INF) and ribavirin is a standard treatment of chronic viral C hepatitis. However, INF treatment is associated with various psychiatric adverse reactions including anxiety, depression, suicidal thoughts, suicide, bipolar disorder, delirium and psychosis [1]. A personal history of mental disorder has been reported as being an important predictive factor for occurrence of psychiatric symptoms associated with interferon therapy [1].
Among the most severe psychiatric adverse reactions, psychotic disorders have been evaluated to occur in less than 1% of INF treated patients [1,2]. Consequently, psychiatric status of patients must be closely evaluated before INF treatment and during the first weeks of treatment. Psychotic symptoms require psychiatric management, and discontinuation of interferon treatment may be warranted [1,3]. However, even after INF cessation, psychiatric symptoms may persist [2,4], following a chronic course [1,5-7]. Homicidal ideation and attempts have also been rarely reported in INF treated patients [8-11]. Homicidal ideation has been estimated to occur in less than 1% of INF treated patients [8], and only two cases of homicidal attempt in INF treated patient have been reported [10]. However, no homicide has been reported until now. We describe a first case of forensic matricide related to a psychosis associated with Interferon alpha2a and Ribavirin treatment.
Case Report
In December 2002, Mss A, 56 years old, killed her mother (91 years old) by burning her after provoking a voluntary and serious head trauma. The homicide was motivated by a wide delusional process including persecutory and life-threatening poisoning ideas, and a misidentification theme (she thought that her mother was substituted by a killer), constructed on pathological interpretations and auditory hallucinations. She was convinced that interferon was intended to poison her by her substituted mother. Due to chronic C hepatitis, Mss A has been treated by Interferon alpha2b and Ribavirin from 10 to 5 months before homicide. Indeed, 5 months after its initiation, treatment was disrupted after emergence of psychotic and depressive symptoms. She was treated with paroxetine and oxazepam but compliance was low, leading to persistence of psychotic symptoms until the crime. In addition, she used to smoke cannabis. After the crime, Mss A was hospitalized in psychiatry and successfully treated by antipsychotic and antidepressants, leading to full remission of psychotic symptoms. She was diagnosed as presenting a mental and behavioural disorder, psychotic subtype, due to a multiple psychoactive substance use (F 19-51) according to DSM IV TR criteria [9]. She had no previous history of psychotic disorder. She had a personal history of heroine consumption stopped many years ago. One brother had an history of psychotic disorder, not otherwise specified
Discussion
We describe a first case of homicide occurring during the course of a chronic delusional disorder associated with INF treatment. Concomitant cannabis use was noted. She had no personal psychotic antecedent. However, she had a familial history of psychotic disorder.
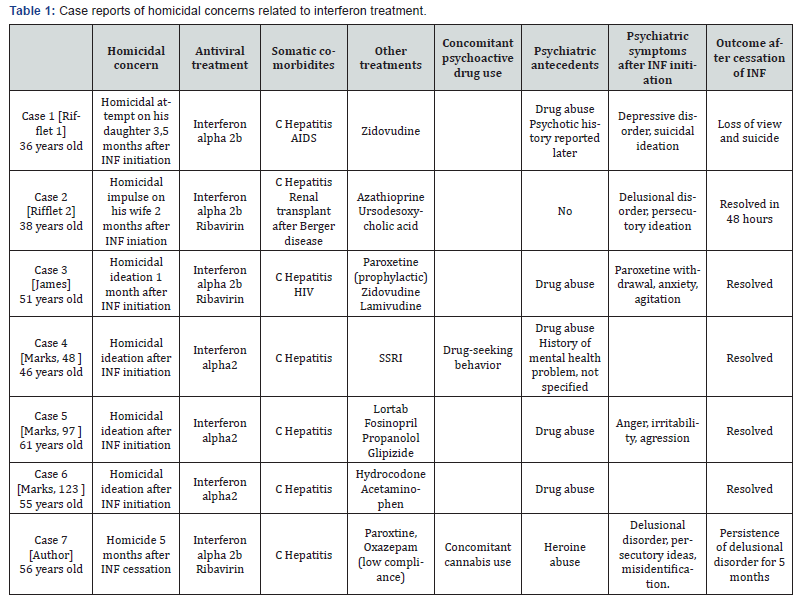
Homicidal ideation during INF treatment has been previously described in one case report [11], and has been estimated to occur in less than 1% on INF treated patients (3 cases on 460 INF-treated patients) [8]. And two case of homicidal attempts in INF treated patients have also been reported [10], for a total of 7 published cases of INF treated patients with homicidal concerns, including our case (Cf Table 1). Homicidal ideation/ attempt emerged as single or during a wider psychiatric disturbance including depressive disorder, delusional disorder, paroxetine withdrawal, anger, irritability. All patients had a previous history of drug abuse; only one patient had a previous history of psychotic disorder. In all cases, homicidal ideation/ attempt disappeared after cessation of INF treatment. It remains undetermined whether the rate of homicidal ideation in IFN treated patients is representative of the expected incidence rate for the general population, but chronological and clinical features suggest that interferon played a causative role in their emergence. Comorbidities, associated treatments and/or previous psychiatric history may had also play a contributive role in most of the reported cases.
Psychosis is a rare occurrence during INF treatment, estimated from less than 0.01% to less than 1% of INF treated patients. Persistence of psychotic symptoms after discontinuation of INF treatment has been reported [5,6], and appears to be not uncommon (7/10 patients were still psychotic after cessation of INF treatment) [2]. In these cases, continuation of psychiatric management is necessary after disruption of INF treatment.
From a larger point of view, schizophrenia and other psychoses are associated with violence and violent offending, particularly homicide [12]. However, among various triggers, most of the excess risk has been reported to be mediated by substance abuse comorbidity [13]. As antecedents of drug abuse is not uncommon in chronic C hepatitis patients, particular attention should be paid to possible persistent psycho-active drug abuse. In addition, delusional misidentification syndrome is considered as a risk factor for potential violence, including homicide [14], as well as life-threatening persecution ideas.
Even extremely rare, our forensic case illustrates strongly that INF may be associated with severe psychiatric adverse events, even after cessation. The extreme severity of this acting out may be considered as the result of the addition and combination of several risk factors including, familial history of psychotic disorder suggesting a possible personal vulnerability, concomitant psychoactive drug abuse, INF treatment, and clinical features of the psychotic disorder.
Conclusion
It must be noted that the lack of serious psychiatric antecedents is not protective from later serious adverse psychiatric reaction. Disruption of INF treatment does not induce systematically improvement of psychotic symptoms, and psychiatric management must be carefully conducted until significant improvement. Familial history of psychotic disorder should be taken into account before INF treatment initiation, as well as concomitant psychoactive drug abuse, especially in patients with a previous drug abuse history. In addition, emergence of delusional misidentification syndrome, as well as life-threatening persecutory ideas should awake for severe behavioral complications.
Homicide Related to Interferon Associated Psychosis
Highlights
Interferon treatment is associated with various psychiatric adverse reactions. Severe psychiatric reactions include psychosis and homicidal concerns. Psychosis may persist after interferon treatment cessation. We report a first case of homicide committed during the course of a chronic psychotic reaction associated with previous interferon treatment. Precautions before initiation and after cessation of interferon treatment are suggested.
References
- Hosoda S, Takimura H, Shibayama M, Kanamura H, Ikeda K, et al. (2000) Psychiatric symptoms related to interferon therapy for chronic hepatitis C: clinical features and prognosis. Psychiatry Clin Neurosc 54(5): 565-572.
- Fattovich G, Giustina G, Favarato S, Ruol A (1996) A survey of adverse events in 11,241 patients with chronic viral hepatitis treated with alpha interferon. J Hepatol 24(1): 38-47.
- Sockalingam S, Shammi C, Stergiopoulos V (2017) Managing the neuropsychiatric complications of hepatitis C treatment. Br J Hosp Med (Lond) 68(10): 520-525.
- Malek Ahmadi P, Hilsabeck RC (2007) Neuropsychiatric complications of interferons: classification, neurochemical bases, and management. Ann Clin Psychiatry 19(2):113-123.
- Schäfer M, Boetsch T, Laakmann G (2000) Psychosis in a methadone-substituted patient during interferon-alpha treatment of hepatitis C. Addiction 95(7): 1101-1144.
- Cheng YC, Chen CC, Ho AS, Chiu NY. Prolonged psychosis associated with interferon therapy in a patient with hepatitis C: case study and literature review. Psychosomatics 50(5): 538-542.
- Schaefer M, Mauss S (2008) Hepatitis C treatment in patients with drug addiction: clinical management of interferon-alpha-associated psychiatric side effects. Curr Drug Abuse Rev 1(2): 177-187.
- Marks D, Breggin P, Braslow D (2008) Homicidal Ideation Causally Related to Therapeutic medications. Ethical Human Psychology and Psychiatry 10(3): 134-145.
- (2000) American psychiatric Association. Diagnostic and statistical manuel of mental disorders. 4th ed., text revision. Washington DC: APA Press, USA.
- Rifflet H, Pol S, Vuillemin E, Oberti F, Duverger P, et al. (1998) Murderous impulses in two patients with chronic hepatitis C treated with interferon alpha. Gastroenterol Clin Biol 22(1): 105-106.
- James CW, Savini CJ (2001) Homicidal ideation secondary to interferon. Ann Pharmacother 35(7-8): 962-963.
- Sariaslan A, Lichtenstein P, Larsson H, Fazel S (2016) Triggers for Violent Criminality in Patients With Psychotic Disorders. JAMA Psychiatry 73(8): 796-803.
- Fazel S, Gulati G, Linsell L, Geddes JR, Grann M (2009) Schizophrenia and violence: systematic review and meta-analysis. PLoS Med 6(8): e1000120.
- Silva JA, Harry BE, Leong GB, Weinstock R (1996) Dangerous delusional misidentification and homicide. J Forensic Sci 41(4): 641-644.






























