- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Forensic, Medicinal Deployment of Methamphetamine, for Metacognition, CBT, Relapse Prevention Innovation and Sexual Traumas
Stephen Mihailides*, Joe Graffam, Allan Wragg Andyjim Sinclair and Aikaterini Sisko
Department of Psychological Sciences, Australia
Submission: December 10, 2018; Published: December 20, 2018
*Corresponding author:Stephen Mihailides, Department of Psychological Sciences, Australia J Forensic
How to cite this article: Stephen M, Joe G, Allan W A S, Aikaterini S. Forensic, Medicinal Deployment of Methamphetamine, for Metacognition, CBT, 002 Relapse Prevention Innovation and Sexual Traumas. J Forensic Sci & Criminal Inves 2018; 11(2): 555809. DOI: 10.19080/JFSCI.2018.11.555809.
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Abstract
The adaptive formulations of stimulant pharmacology are the focus of this work. The capacity for stimulant for treating trauma psychopathologies is outlined in order to formulate the bases of structured clinical trials. Innovations presented also include formulation of five psychopharmacological treatment principles as basis of a relapse-prevention innovation, for new tools to concurrently redress stimulant abuse. The stimulant science is developed within combination metacognitive-CBT based frameworks. New treatment principles integrate recent advances in appreciation of methamphetamine’s pharmaceutical role in the metacognition of agency [1,2]. Disabuse of amphetamine science is developed by focus upon objective features of the hundred-year journal history. Pharmaceutical science is organised within a treatment paradigm drawing on Bandura’s [3] theory of triadic reciprocal determinism. Bandura’s work is presented in an alliance with the principles of metacognitive therapy (MCT), [4]. Psychopharmacological treatment concepts are then summarised within the fortified cognition hypothesis, with a particular focus on an advancement for treating sexual traumas. Conclusions develop foundations for the relapse-prevention innovation by recognising the utility of awe when metacognition is active. Methodising the appearance of affective awe, for the post-stimulant treatment, is central in the relapse-prevention innovation and premise for hypotheses for clinical trials.
Keywords: Methamphetamine; Psychosexual trauma; Psychopharmacological Intervention; Metacognitive therapy
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Introduction
Formulating treatment concepts that deploy methamphetamine and metacognition for psychopharmacological interventions has an evidence-base about metacognition and its role in agency [1-3]. Hart et al. [1], Hart et al. [2], and Kirkpatrick et al. [3] developed the pharmacological science noting the benefit of methamphetamine for metacognitive functioning. From that foundation, three domains of therapeutic utility are defined. Pharmacological theory outlines the known treatment benefits recorded for over a century of prior methamphetamine science. From that evidence base, five treatment principles for the psychopharmacological modality are developed. The treatment principles are grounded within the overarching framework of Albert Bandura’s theory of Triadic Reciprocal Determinism [4]. In an alliance of grounding, Albert Bandura’s ideas are developed within Wells and Matthews [5] metacognitive theory and applied to methamphetamine science for treatment concepts. The proposed role of stimulant-fortified metacognition for accelerating resolution of psychosexual traumas is emphasised in the treatment innovation. Materials are summarised within this framework under the fortified-cognition hypothesis. The third focus of the review is upon relapse-prevention, emphasising awe and its affective footprint during and post pharmacological support, for mounting metacognition post dosing, in an adaptation to practice reversing existing dependency
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Pharmacological Treatment Concepts
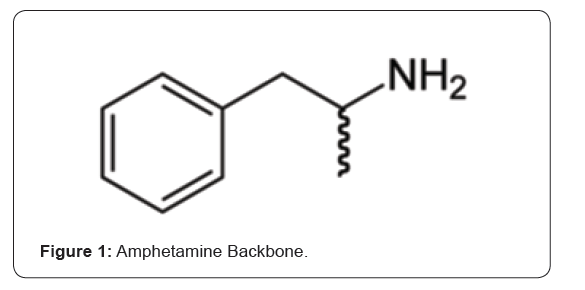
Pharmacological theory about stimulants has existed for over a century. The biochemistry of stimulants is reviewed prior to applying that to the development of treatment principles for methamphetamine in the review body. Amphetamines, as a family of related substances, in general, have widespread use in a number of clinical conditions including narcolepsy, orthostatic hypotension, nasal congestion, migraine, asthma, hyperactivity and obesity [6-8]. There is some evidence to suggest that depression is more responsive to dopaminergic agents, with stimulants as useful chemical treatments for depressions in bipolar conditions [6,9,10]. Mechanism of action, outlined in the vigilance model of affective disorders, proposes that the pharmaceutical support of stimulants [9,10] stabilises brain autoregulatory vigilance (brain arousal) through the creation of a stimulating environment. The noradrenergic system is well recognised as implicated with phasic arousal in vigilance [10]. A great deal is known about the organic chemistry of amphetamine derivatives. Manufactured substances co-occur with many naturally occurring proto-alkaloids such as mescaline and ephedrine that exist in the plant kingdom. The alkaloid backbone for amphetamine is as follows: (Figure 1) Modification of an alkaloid at the aromatic ring end (left of picture) or amino group (top right of picture) end can considerably change the pharmacological specificity of the compound [7,8]. Amphetamine is a strong central nervous system stimulant and is also an anorectic agent (i.e. appetite suppressant).
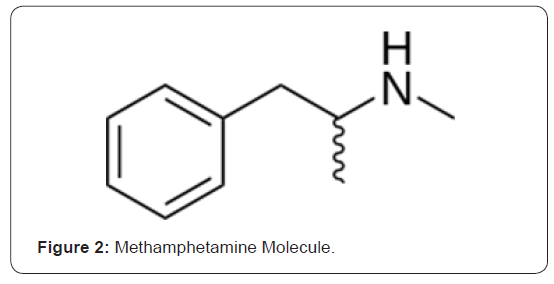
The addition of the hydroxy group on the beta carbon (see the peak, to the right of the aromatic ring) reduces both stimulant and anorectic effects. By contrast, addition of a second alpha methyl group, as is the case in methamphetamine, preferentially increases the stimulant properties of an alkaloid (that is, removing a H bonded to the nitrogen, N, and replacing that with methyl, —CH3, represented, by convention as a “—” in chemical formulae). See (Figure 2), below. Insertion of functional groups on the side chain of amphetamine, or at the terminal amino group, or that target the aromatic ring create anorectic derivatives with reduced stimulant and cardiovascular effects. Aromatic ring substitution by functional groups such as methoxy groups (—O—CH3) have been shown to dramatically alter the pharmacological specificity of the drug, shifting it from a catecholaminergic agent to one that exerts its primary effects upon serotonergic systems [7,8,11]. Methamphetamine, as a psychomotor stimulant, was first synthesised in 1893 (such as was cited by [12]. It has anti-fatigue reinforcing effects and at very high dose it induces psychosis. Methamphetamine enhances release, and blocks reuptake of dopamine (DA), norepinephrine (NE) and serotonin (5-HT), and is also a monoamine oxidase inhibitor [7,8,11]. As a result of those effects, methamphetamine acts as an indirect agonist of monoaminergic receptors. At low dose, methamphetamine causes increased motor activity. At high dose, effects include stereotypical movements, and interference with food and water activities that are related to DA, NE and 5-HT systems. In addition, antagonists of dopamine D2 receptors Dopamine receptor antagonists, haloperidol and chlorpromazine decrease violence [8,11].
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Dose-Related Information
Dose and chronicity of use are two important pharmacological parameters, part of the science of pharmacokinetics, impacting a compound’s effects upon behaviour, affect and cognition. In order to understand how to apply methamphetamine to treatment frameworks, it is important to understand the pharmacological processes that define the dose-related effects of non-harmful, medicinal applications of stimulant. Dependency, criminality and abuse-related aggression occur for regular users of high, not medicinal doses of methamphetamine [7] and [13], who cite Arnold et al. 1973, Maletzky 1974; Conners 1969; Conners 1972, Winsberg et al. 1972; Winsberg et al. 1974. At very high doses, it causes dilated pupils, flushing, restlessness, dry mouth, bruxism, headache, tachycardia, bradycardia, tachypnea, hypertension, hypotension, hyperthermia, diaphoresis, diarrhea, constipation, blurred vision dizziness, twitching, insomnia, numbness, palpitations, arrhythmias, tremors, acne, pallor, seizures, acute myocardial infarction, cerebrovascular accidents and death [6,14]. Research exploring the relationship between dose, methamphetamine and aggression reveals that the stimulant has a biphasic effect upon aggressive behaviour [13]. Evidence for that is primarily based on experimental animal studies, and for methamphetamine, those are prolific (e.g., see the metaanalysis by Scott, et al. [15]. Meta-analysis reports varying effects of dose, ranging from no increase, increase, but also dose-related decrease in aggressive behaviour for optimal range of biphasic stimulation. It is withdrawal-related aggression and people’s violence histories where there is serious dependency that emerge in explanations of behaviour, however, as noted in Turning Point materials for the National drug strategy [16]: Although there is a perception that all methamphetamine users are violent, this is not the case. Rates of violent crime, although higher than the general population, tend to be restricted to methamphetamine-dependent, multiple drug users with a history of violence. Violence, when it does occur, usually happens when people are paranoid or psychotic. Therefore, hostility and violence is often time-limited, and tends to occur only when symptoms are acute (p. 10) Chronic, high-dose use is also known to be neurotoxic. [12].
The neurotoxicity in methamphetamine abuse is a major area of risk associated with misuse of the substance. Long-term, high-dose use of methamphetamine is neurotoxic to dopamine and serotonin systems [6,12]. Three lines of evidence support the neurotoxicity hypothesis. In the first, it has been established that levels of dopamine activity affect the enzyme for synthesis of dopamine in a rate-limiting step. Long-term methamphetamine use decreases enzyme-synthesis. In the second line of evidence, the number of reuptake sites for dopamine is reduced in longterm high-dose use, and in the third, neuronal degradation has been demonstrated in dopamine rich areas of the brain. For serotonin (5-HT) systems, multiple dosing results in longlasting reduction in tryptophan hydroxylase activity, an enzyme associated with synthesis of 5-HT, as well as 5-HT content and uptake sites on neurons. However, evidence exists to suggest effects are reversible for all neurotransmitter systems at the one-year time interval [6,12]. Thus, adherence to dosing at optimal levels, over the shorter term and with pauses between short, acute-phase usage are means for preventing aggression and neurotoxicity of drug misuse.
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Pharmacological Treatment Knowledge
There is nothing really new is the assertion that amphetamines and their derivatives have both known and potentially new treatment potentials for a variety of conditions. For example, in a publication by Bradley [cited in 42], there were identified beneficial treatment effects noted by administration of amphetamine to aggressive, irritable and hyperactive boys, purportedly repeatedly confirmed by double-blind, placebo controlled studies. Reductions in aggressive behaviour and improved social interactions were found at doses with 10 to 40 mg/day of d- or l-amphetamine for boys and girls, 5 to 14 years of age, who had been diagnosed with hyperkinetic, autistic, explosive, unsocialised or as emotionally disturbed [13, who cite Arnold et al. 1973; Maletzky 1974; Conners 1969; Conners 1972; Winsberg et al. 1972; Winsberg et al. 1974]. Medicinal effects for methamphetamine are predicted for aggression (at low dose, pursuant to its biphasic effects), for hyper-somniacs, and for a motivational condition. It is already currently used for attentional deficits such as Attention Deficit Hyperactivity Disorder (ADHD), and Attention Deficit Disorder (ADD), under the brand name Digoxin. See RxList the Internet Drug Index, URL provided in reference list). As an anorectic agent, it is also expected to have utility for treating subtypes of obesity, but because of its pharmacokinetic properties (it is an especially powerful CNS stimulant), particularly for a subclass of obesity with a co-morbid medical condition where CNS stimulation is indicated.
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
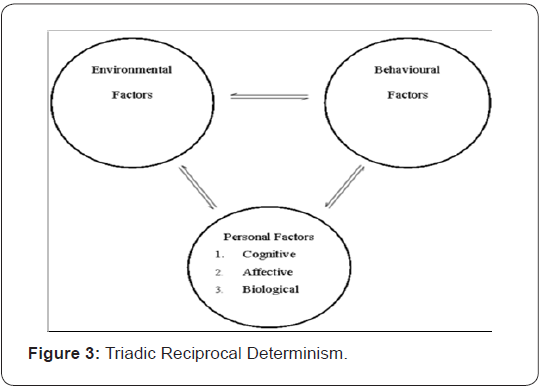
Treatment principles can deploy stimulants as adjuncts to psychological therapies, via stimulant’s effects upon motivation, affect, cognition and behaviour. Sexual pathologies that cause hyposexual functioning may be remedied by stimulant through its adjunctive impacts on parasympathetic functioning. Medicinal impacts require optimal-range dosing, but for new treatment areas where new knowledge is required to establish dose structure. The known dose range for prior science, as the lower of the bi-phasic dose ranges is not comprehensive knowledge, and so premises need for clinical trials, to establish dose optimisation for the new psychopharmacological hypotheses presented, shortly. Therefore, treatment hypotheses, developed within the metacognitive and cognitive-behavioural tradition guides the development of five new treatment principles, as premise for structured clinical trials to develop a new dose science. The underlying fundament of new formulations for sexual traumas, premise that hate crimes are deeply causal in sexual trauma. Thus, new science focuses on allying behavioural and cognitive principles for maximising a person’s capacity to divest themselves of hate and of victimisation, by empowering them to form a healthy emotional character with reconstituted sexual competence and confidence. The grounding basis for the position derives support from Albert Bandura’s Triadic Reciprocal Determinism [4], a broad framework that combines influences of personal, environmental and behavioural factors (Figure 3) into a general treatment delivery framework. Three levels of analysis are subsumed by cognitive, affective and biological processes. Albert Bandura’s model asserts that intervention may be effected by interceding at any or all points in the system of interacting triadic components. Figure 3. summarises principles in the visual mode (Figure 3). The fortified-cognition hypothesis, within this framework, posits that pharmacological support by a stimulant can fortify cognition, and through that, be the basis from which to mount a formalised psychological treatment, in a multidisciplinary-alliance model of intervention. The idea is not new. Anti-depressant medications, for example, are deployed in an isomorphic fashion see Hetrick et al. [17], for a review on this area for Post-Traumatic Stress Disorder). Treatment frameworks using selective serotonin reuptake inhibitors (SSRIs), create fortified psychogenic states upon which further treatment gains can be made. The treatment literature recognises the potential benefits for such multi-disciplinary interventions in the literature on relapse rates for medicated-only clients [18], versus clients treated with combination medication and cognitive-behavioural psychological therapies.
Principle 1: Understanding how stimulant fortifies cognitionAntifungal resistance
During mild to moderate levels of intoxication, the psychological effects of methamphetamine include alertness, euphoria, increased concentration, energy, self-confidence, sociability, improved self-esteem and empowered libido. The libidinal support is extremely important in a trauma support framework where a sexual or emotional trauma causes hyposexual arousal. Of course, emotional work remains a fundament of any intervention, however bolstering that with sexual capacitation is also vital. Intranasal delivery has been observed to improve the metacognition of agency in a doubleblind controlled study [2,3]. Judgments of agency increased, with improvement upon task performance observed for dose ranges as described in the study. Kirkpatrick et al. [3] also observed dissociation of dose dependency for the positive subjective effects of the substance. Therefore, this contribution to a person’s metacognition is important for the psychological treatment formulation. The forensic literature provides information about non-optimal, high-dose of methamphetamine and its impact upon cognition [19-27] [15,28], and see also Degenhardt et al. [29] for prevalence estimates.
The literature is repetitious, and typically imbalanced in its failure to recognise the concurrent, century-old, available medicinal science for stimulants. Likewise, the forensic literature fails to register equivalence of methamphetamine in its membership in the stimulant family (e.g. brand names, Ritalin, Duromine, Adderall, Dynavel XR). However, forensic data, though biased in a risk-centric dialogue, are useful for appreciating high dose and associated pathology. At high dose, it can induce grandiosity and excessive feelings of power, and invincibility including mania and psychosis. For optimised dose, methamphetamine’s augmentation of metacognition allies it to that family of psychological therapies that deploy metacognition [30] in the well-established metacognitive therapies [5]. The associated During fortified states of cognition, a fortified metacognitive faculty can be harnessed with the support of a therapist. Accelerated rates of insight-development, synchronised with the principles of treatment formulations of intervention for metacognitive therapies, predict shortened treatment times wherever metacognition is applied to a treatment focus. Increased efficiency is expected for any pleasure and mastery components defined during intervention on any cognitive-behavioural foci. This is especially likely given the enhanced language learning and enhanced memory effects noted for this stimulant in prior studies [31,32]. See, Hart et al. [2] for a theoretical review of a further sixteen methamphetamine studies that identify increments to visuospatial perception; reaction time, vigilance, learning/memory; sustained attention, information processing, perceptual speed, psychomotor function, conceptual ability and metacognition.
Principle 2: Optimise exposure by harnessing both sympathetic and parasympathetic arms of the autonomic nervous system
Ordinary cognitive-behavioural exposure deployed insession operates by facilitation of relief of fear by the application of imaginal and in-vivo graded-exposure tasks in the therapeutic alliance between client and therapist. Brewin’s [33] mapping system, implicates neuropsychological relationships between autobiographical memory, visual memory, and the mid-brain structures of the hippocampus and amygdala in the trauma response. Elevations in fear reflect increased activity on the sympathetic arm of the autonomic nervous system [34] implicating the hypothalamic-pituitary axis (HYPAC), activating the adrenal glands, elevating cortisol and suppressing immunity [35]. Fear extinction during exposure therapy is thought to occur via the hippocampus-dependent form of encoding of autobiographical memory, effective during between-session habituation of CBT. Exposure therapy via therapeutic habituation is thought to lessen the more fear-based automatic, imagebased over-activity of the amygdala-dependent form or memory encoding. Sexual arousal activates the parasympathetic nervous system with concurrent dampening of the sympathetic nervous system. Any therapeutic alliancing of the parasympathetic and sympathetic systems, through deployment of behavioural tasks to both arms of the autonomic system, is thus an obvious way to reclaim wellness more quickly. De-activating the sympathetic nervous system by adapting pleasure and mastery-based tasks as sexual components, to the more traditional graded exposures, is expected to enhance fear-extinction. Further, because a sexual trauma typically occurs through violating sexual acts, a priority exists to define corrective sexual pleasure and mastery scheduling with the therapeutic CBT-metacognitive focus in order to restore sexual agency.
Principle 3: Stimulants accelerate resolution of psych affective and psychosexual trauma
The success of another stimulant, (±3,4-methylenedioxy-Nmethamphetamine, or MDMA, ‘ecstasy’) has been demonstrated in a clinical trial, for treatment of emotional traumas [36]. Previously, during the early- to mid-part of the 20th century [37] it was a valid adjunct to psychotherapy before partisan lobby groups had it illegalised. The recent clinical trials restore scripted access to this stimulant. MDMA, a compound closely related to methamphetamine, differs only by way of bearing a dioxol functional group (—O—C—O—) on the aromatic end of the amphetamine backbone. MDMA, known as an empathogen and entactogen, facilitates enhanced intimacy and empathy (it is empathogenic). It augments pleasurable, tactile contact between people (that is, it is an entactogen). Methamphetamine is less empathogenic, although at optimal dose it sustains empathic function, and it is not less entactogenic than MDMA. Methamphetamine enhances confidence and elevates libidinal drive, in an accompanied lowering of inhibitions and anxiety. Methamphetamine transiently repairs mood, self-esteem and confidence. The libidinal enhancement is not particular to methamphetamine. In an experimental study, [38] administered the stimulant Ritalin (methylphenidate, for treating ADHD) to participants and demonstrated enhanced libidinal drive.
The stimulant psych affective and psychosexual effects of optimised dose, especially the trauma-resolution enhancements (Principle 2), and the improvement in libido and confidence, ideally match the treatment foci central for psychological therapies targeting sexual traumas. The metacognitive therapies, especially, are expected to be an efficient mode for integrating stimulant-augmented sexual psychogenic states into treatment. Pleasure and mastery scheduling, for graded exposure, developed in therapy, can be reviewed after each deployment of dose-facilitated sexual engagement. This aspect of intervention in informed by our recent advances in the understanding tremorgenic conditions, as characterised where there are elevations state-psychopathy [39,40]. In particular, during trauma resolution it is stimulant-facilitated CBT-metacognitive sexual trauma therapies, that have great potential to reconstitute empathic functioning, with a wider range of durability in the reconstituted empathy. The CBTmetacognitive alliance, deploying stimulant to quell sympathetic nervous system activity, permits a re-adaptation to more varied emotional ranges, for improved sexual and affective problem solving. It is methamphetamine’s capacity to open an episode of sexual plasticity that is so pivotal in its capacity to facilitate sexual wellness. The person’s acquisition of wisdom through grounding metacognition facilitates re-engagement with sexual tasks during sexual character reconstitutions. Of especial relevance, the metacognitive therapies, together with libidinal enhancement of stimulant also provide particular utility for decoding and resolving the impacts of abuse, violence and hatred that so often co-occur with sexual abuse. Sexual traumas often leave the person afflicted with mood disturbance, then residual chronic hatred, rage, and the learned helplessness of the encasing rumination of cycles. In Mihailides, Galligan and Bates [39,40] the basis for divesting the afflictions of predatory vanity that impacted mental health after sexual abuse, are also the basis to inform metacognitive therapies under new guidelines. For example, methamphetamine deployed as a sexual fortifier to person with sexual trauma enables a means for a treatment worker to carefully partition the placement of hatreds inflicted upon a person during the crime. This enables efficient sexual divestment of that hatred and greatly accelerates maturation of empathic perspective taking agency, for the formerly helpless person. That is, was it hatred of the client direct, or hatred for the person’s role, merits of achievement, or of their culture that were central when the sex crime ignited a chronic sexual trauma
Principle 4: Generalisability of treatment goal setting
Treatment goal setting has nomothetic features, as outlined especially in Principle 2. That feature of methamphetaminebased psychopharmacological intervention is one about treatments that focus on sexual development. Mental wellness is strengthened where sexual identity and sexual functioning have acquired resilience in its foundations. Sexual capacity is one of two primary assets of mental health, with the second arm being about affective performance. These two primary arms of wellness also imply that personal development should also have idiographic features. That individual focus is to accommodate the significant variation in personality and presentation of the affective symptoms that accompany a sexual trauma. Therefore, treatment goal setting for sexuo-affective pathology must be responsive, multiply to reflect the way socio-affective and socio-sexual pathologies interact. Thus, treatment formulations for self-esteem, anxiety-resolution, and mood-resolution components should reflect attention to metacognitive features of the sexual, not just the affective cognitions.
Principle 5: Decoding cognition during methamphetamine affected versus methamphetamine-free states
The therapist’s role is pivotal in how the client’s metacognition is harnessed. Trauma is accompanied by cognitive distortions as so noted in the basic diagnostic criteria of PTSD in the Diagnostic and Statistical Manual-5 [41]. In an artificially fortified, chemically induced state, cognitive distortions are expected to intrude upon the nature, quality and kind of materials garnered from the person concerned. The therapist’s role, by assisting the individual to juxtapose information derived from the medicated versus non-medicated state, is a guided metacognitive development. Resolving doserelated cognitive distortions, whilst setting harm-mitigating and health-promoting therapeutic sexual goals recommended, are about short, acute-phase dosing, not continuous dosing. That is, treatment is structured as a pulsing of a series of single optimal doses, followed by cessation of intake and resumption of normal life. Dosing should coincide with structured therapeutic tasks. A prescribed period between dosing is recommended, with phase-out or maintenance-prompted medication after the core exposure scheduling is complete.
This particular structure is expected to maximise retention of gains of the fortified cognition after cessation of use. Thus, the model of treatment emphasises resolution of dependency and of sexual hatreds in its tenets. There may be requirement for concurrent access of the person to sleeping medication, because stimulants have the potential to disrupt sleeping patterns, when deployed in acute dosing, before tolerance to the drug occurs. Morning dosing is encouraged to minimise disruption to sleeping patterns, because methamphetamine has a half-life of about twelve hours. Matters of deepening appreciation of differential diagnosis, for the potential provision of concurrent mood stabilising medications, is the purview of clinical trials. As is the case with every diagnostic condition in the DSM-5, heterogeneity is expected in populations suffering from mental illness, especially where there is dual diagnosis.
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Relapse-Prevention Innovation and Guided Stimulant Use
McKetin, et al. [42] state that “…whereas most methamphetamine users take the drug infrequently” (p. 358). In a noteworthy addition to their comments, authors state: “such recreational patterns of stimulant use have become increasingly apparent in many parts of the world, particularly in the context of dance events”, (p. 358). McKetin et al. [42] note that socially patterned use is “not typically associated with severe harms” (p. 358), although statistics for recreational-only use were not apparent in their work. They, instead, cite numbers of global users at fifteen to sixteen million. It is quite unfortunate that due to the drug’s illegal status, such recreational users cannot derive the protective benefits from ritualised, mentored, or responsibly formulated social norms. Such norms do not yet exist. Instead, methamphetamine stigma and courtesy stigmatisation of those who support users, are the prevailing social norms. Methamphetamine stigma, not resolved in practitioners, constitutes an iatrogenic factor when stigmatised user groups receive advice or support from such professionals. Users, afraid of prosecution, are less likely to mount protective processes around their social use. Although neurobiological theory [43,44] implicates the limbic system, (an organisation of brain structures for affective recognition and memory, including the hippocampus and amygdala) with onset of dependency, such theories struggle to explain why the majority of users do not develop dependency. Likewise, Marlatt and Gordon [45] in their relapse prevention modelling approach the treatment of dependency after its onset, without emphasising the factors that kept the non-dependent group pathology free. Andrews and Bonta [46], and their pivotal contribution to the forensic psychological literature emphasise a risk/needs formulation with five rehabilitation principles for extant offending populations [47-50].
Their work does not assist understanding of the known epidemiology of methamphetamine use, notably, that most people do not develop dependency [51-54]. The Fortified Cognition hypothesis for stimulant theory, lends itself to innovation for the field of relapse prevention. Its core foundation is grounded in metacognitive functioning, applied during optimised dosing. This nootropic function of the stimulant is hypothesised to rouse affective awe. That is because nootropic or metacognitive insights have vivid impacts during the recognition of insight, and new ideas. Awe for the detection of invention, innovation is associated with vitality and vigour of wellness. Pending writing pursues those hypotheses for an overlooked emotion, awe, and its relationship to both metacognition and emergence of stable low-end, normal stimulant use. By contrast, onset of dependency implies a distinct affective footprint for those affected stimulant users [55-58]. It is suspected that dependency-vulnerability is about the sudden onset of clarity during optimal dosing, as metacognition is enhanced mounting awe, but where awe becomes fused with the dopamine-related pleasure effects during use. Such an emphasis places fusion of awe with certain beliefs as cognitive distortions [59-64]. That is, pleasure and awe are distinct. That is, pleasure is not happiness. Thus, it is expected that there are individual differences in the cognitive footprint of awe brought by people to stimulant use at its onset. Therefore, the central focus of future writing develops ideas about awe’s footprint, and how it appears in adaptive functioning, especially during cessation of use. The temporal appearance of awe in the spectrum of pre- and post-use effect of distinction, premises that human affective instincts and metacognitive grounding, can be methodised to quell dependency [65-67]. It is anticipated that awe unifies with human spiritual nootropic agency about how to increment wellness post use. In particular, methodising metacognitive intervention so that post-use awe increments the sense of novelty, wellbeing and agency for new life focus is defined as first priority for theoretical advancement. Referencing treatment Principle 4 in particular, it is expected that methodising post-use awe requires the idiographic focus, in order to understand the emotions of the unique lives, and how to invest awe into lateral thinking for metacognitive work [68,69]. Awe is affected that operates adjunctively to any other emotion. For example, awes about grief, versus awes about mastering another’s hate for us elicit quite distinct cognition. Awe’s utility extends as well into shame resolution, because it guides mastery and fortitude for striving towards gratitude from painful originating emotions. Awe’s adaptability to emotional problem solving is wide, thus, awe for metacognitive work permits hypotheses to be developed, and method for reversing advanced, serious dependency as well as less serious dependency. It is especially awe for its potential to empower metacognitions that despatch any helplessness, or poverty of mood that predicates methamphetamine as useful, because of the stimulant’s bolstering of metacognition.
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
Conclusion: Implications for Policy and Law Reform
One hundred years of pharmacokinetics has demonstrated that methamphetamine as a stimulant, when prescribed correctly, has beneficial impacts on cognition and behaviour. However, methamphetamine-stigma and courtesystigmatisation about forwarding clinical reforms have halted the advancement of stimulant science. Thus, the treatment potential for methamphetamine have been subjected, preventing the identification of uses of stimulant. Whilst methamphetamine abuse is a serious matter for a person and his community, that should encourage, not impede the development of robust, evidence-based science. The view asserted in this review emphasised the quarantining of methamphetamine stigma, so that the important psychopharmacological, and relapse-prevention innovations could be developed. A guided, sensible stimulant use regime as prelude to clinical trials. Randomised, double-blind treatment trials require careful theoretical pre-development, due to the forensic context. It is especially important to observe the hate-based dialogue about methamphetamine to understand where that impedes progress in constructive ways.
A criminal industry has been created and that has impeded medicinal deployment of innovations in methamphetamine science. Further, criminalisation instead creates a resourceintensive and costly, enforcement industry that seeks to tackle a problem downstream. Structuring law and policy systems that assist with resolution of the social problems is required to advance social health. Legalised manufacture of methamphetamine as Desoxyn, with greater protection and clear clinical foundations for prescribed medical uses requires systemic law and policy reforms. Education of the populace, in order to shift attitudes and raise awareness about the area is required, as is systemic law reform. New foundations of stimulant science for structured scripted uses assists with social wellness and cohesion. It is also expected that the well-end of the population of infrequent users of stimulant, the recreational group, can also be assisted by having medicalised referral pathways as preventative of harm. Recreational users, who are well, probably access the nootropic of the pharmacy without therapist input. However, formalised guidance of its features is to be encouraged, under supervision. Given this review’s development of concurrent remedy to methodise extinction of advanced dependency, by metacognitive adaptation, our work also respects the urgencies, even of the hate-rage dialogues by those who demonise stimulant users.
- Review Article
- Abstract
- Introduction
- Pharmacological Treatment Concepts
- Dose-Related Information
- Pharmacological Treatment Knowledge
- The Fortified-Cognition Hypothesis and Psychopharmacological Treatment Potential of Methamphetamine
- Relapse-Prevention Innovation and Guided Stimulant Use
- Conclusion: Implications for Policy and Law Reform
- References
References
- Hart CL, Gunderson EW, Perez A, Kirkpatrick MG, Thurmond A, et al. (2008) Acute physiological and behavioral effects of intranasal methamphetamine in humans. Neuropsychopharmacology 33(8): 1847-1855.
- Hart CL, Marvin CB, Silver R, Smith EE (2012) Is cognitive functioning impaired in methamphetamine users? A critical review. Neuropsychopharmacology 37(3): 586-608.
- Kirkpatrick MG, Metcalfe J, Greene MJ, Hart J (2008) Effects of intranasal methamphetamine on metacognition. Psychopharmacology 197(1): 137-144.
- Bandura A (1986) Social Foundations of Thought and Action: A Social Cognitive Theory. Englewood Cliffs, Prentice-Hall, New Jersey, USA.
- Wells A, Matthews G (1996) Modelling cognition in emotional disorder: The S-REF model. Behaviour Research and Therapy 34(11-12): 881-888.
- Asghar K, DeSouza E (1989) Pharmacology and Toxicology of Amphetamine and Related Designer Drugs. National Institute on Drug Abuse Research Monograph 94.
- Feldman RS, Meyer JS, Quenzer LF (1997) Principles of Neuropsychopharmacology. Sinauer Associates, Massachusetts, USA.
- Karch SB, Drummer O (2012) Pathology of Drug Abuse, (5th edn), CRC Press, Australia.
- Carlson PJ, Merlock MC, Suppes T (2004) Adjunctive stimulant use in patients with bipolar disorder: treatment of residual depression and sedation. Bipolar Disorders 6(5): 416-420.
- Hegerl U, Hensch T (2014) The vigilance regulation model of affective disorders and ADHD. Neurosci Biobehav Rev 44: 45-57.
- Siebel TM, Mange SA (2009) The montana meth project: 'Unselling' a dangerous drug. Stanford Law & Policy Review 20: 405-416.
- Marshall JF, O Dell SJ (2012) Methamphetamine influences on brain and behavior: unsafe at any speed? Trends Neurosci 35(9): 536-545.
- Mihailides S, Galligan R, Bates G (2017) Reconceptualising psychopathy. Journal of Forensic Psychology 2(2): 1-12.
- Hammer MR (2007) A Key to Methamphetamine-Related Literature, Version 1.0.1. Division of HIV Prevention, AIDS Institute, Department of Health, New York State, USA.
- Shucksmith N (1984) The Seventh Sense. SCRE Publications.
- Kalechstein AD, Yoon JH, Croft DE, Jaeggi, S, Mahoney JJ, et al. (2011) Low dose, short-term rivastigmine administration does not affect neurocognition in methamphetamine dependent individuals. Pharmacology, Biochemistry and Behavior 99(3): 423-427.
- Huang YS, Tang TC, Yen CF (2011) Effects of motivational enhancement therapy on readiness to change MDMA and methamphetamine use behaviors in Taiwanese adolescents. Subst Use Misuse 46(4): 411-416.
- Papageorgiou C, Wells A (2000) Treatment of recurrent major depression with Attention Training. Cognitive and Behavioural Practice 7(4): 407-413.
- Bell S, Lucke, JC, Hall WD (2012) Lessons for enhancement from the history of cocaine and amphetamine Use. American Journal of Bioethics: Neuroscience 3(2): 24-29.
- Carroll KM, Rawson RA (2005) Relapse Prevention for Stimulant Dependence. In: Marlatt A, Donovan DM (Eds.), Relapse prevention: Maintenance strategies in the treatment of addictive behaviors (2nd edn), Guilford Press, New York, USA, pp. 130-150.
- De Sandre PL (2006) Methamphetamine emergencies. Journal of Gay & Lesbian Psychotherapy 10(3-4): 57-65.
- Marlatt GA, Gordon JR (1985) Relapse Prevention: Maintenance Strategies in the Treatment of Addictive Behaviors. Guilford Press, New York, USA.
- Fanflik PL, Johnson NE, Troutman DR, Skinnger FC (2006) Drug Prosecution and Prevention Across the Nation: Prosecutors' Perceptions of Drug-Related Crime and Strategies to Combat the Problem in Their Communities. National District Attorneys Association, USA.
- Miczek KA, Tidey JW (1989) Amphetamines: Aggressive and social behavior. National Institute on Drug. Abuse Research Monograph Series 94: 68-100.
- Roe S, Man L (2006) Drug Misuse Declared: Findings from the 2005/06 British Crime Survey. Home Office Statistical Bulletin, England and Wales, UK.
- Otto MW, Smits JA, Reese HE (2006) Combined Psychotherapy and Pharmacotherapy for Mood and Anxiety Disorders in Adults: Review and Analysis. Focus 4: 204-214.
- Wells A, Fisher P, Myers S, Wheatley J, Patel T, et al. (2009) Metacognitive Therapy in Recurrent and Persistent Depression: A Multiple-Baseline Study of a New Treatment. Cognitive Therapy and Research 33(3): 291-300.
- Smout MF, Longo M, Harrison S, Minniti R, Wickes W, et al. (2010) Psychosocial treatment for methamphetamine use disorders: A preliminary randomized controlled trial of cognitive behavior therapy and acceptance and commitment therapy. Substance Abuse 31(2): 98-107.
- Degenhardt L, Bucello C, Calabria B, Nelson P, Roberts A, et al. (2011) What data are available on the extent of illicit drug use and dependence globally? Results of four Systematic reviews. Drug Alcohol Dependence 117(2-3): 85-101.:
- Seiden LS, Kleven MS (1989) Drugs: Toxicity and resulting behavioural changes in response to pharmacological probes. In: Asghar K, De Souza (Eds.), Pharmacology and Toxicology of Amphetamine and Related Designer Drugs, National Institute on Drug Abuse Research monograph 94.
- Breitenstein C, Wailke S, Bushuven S, Kamping S, Zwitserlood P, et al. (2004) D-amphetamine boosts language learning independent of its cardiovascular and motor arousing effects. Neuropsychopharmacology 29(9): 1704 -1714.
- Zeeuws I, Soetens E (2007) Verbal memory performance improved via an acute administration of D-amphetamine. Human Psychopharmacology 22(5): 279–287.
- Brewin CR (2001) A cognitive neuroscience account of posttraumatic stress disorder and its treatment. Behaviour Research and Therapy 39(4): 373-393.
- McCarty C, Yzerbyt VY, Spears R (2002) Stereotypes as Explanations the formation of meaningful beliefs about social groups. Cambridge University Press, Australia.
- Chivers Wilson KA (2006) Sexual assault and posttraumatic stress disorder: A review of the biological, psychological and sociological factors and treatments. McGill Journal of Medicine 9(2): 111-118.
- Nicosia N, Pacula RL, Kilmer B, Lundberg R, Chiesa J (2005) The Economic Cost of Methamphetamine Use in the United States. The Meth Project Foundation and the National Institute on Drug Abuse, RAND Drug Policy Research Center. A Joint Endeavour within RAND Health and Infrastructure, Safety, and Environment.
- Bernschneider Reif S, Oxler F, Freudenmann RW (2006) The origin of mdma ("ecstasy")--separating the facts from the myths. Pharmazie 61(11): 966-972.
- Washton A, Zweben JE (2009) Cocaine and Methamphetamine Addiction: Treatment, Recovery and Relapse Prevention. Norton, New York, USA.
- Mihailides S, Galligan R, Bates G (2017b) The Quarantine Vector and Psychopathy Induction. Journal of Forensic Psychology 2: 128.
- Milivojevic D, Milovanovic SD, Jovanovic M, Svrakic DM, Svrakic NM, et al. (2012) Temperament and character modify risk of drug Addiction and influence choice of drugs. American Journal on Addictions 21(5): 462-467.
- American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders: DSM-5 (5th), Arlington, VA: American Psychiatric Association.
- McKetin R, Hickey K, Devlin K, Lawrence K (2010) The risk of psychotic symptoms associated with recreational methamphetamine use. Drug and Alcohol Review 29(4): 358-363.
- Bryant B, Knights K (2007) Pharmacology for Health Professionals (2nd edn), Mosby Elsevier, Sydney, Australia.
- Bullock S, Manias E, Galbraith A (2007) Fundamentals of Pharmacology (5thedn), Prentice Hall, USA.
- Lloyd C (2010) Sinning and Sinned Against: The Stigmatisation of Problem Drug Users. UK Drug Policy Commission, London, USA.
- Andrews D, Bonta J (1994) The psychology of criminal conduct. Anderson Publishing Co, Cincinnati, Ohio, USA.
- Australasian Legal Information Institute (2003) Cases and Legislation, University of Sydney & University of New South Wales, Australia.
- Cobb SJ, Woods SP, Matt GE, Meyer RA, Heaton RK, et al. (2007) Neurocognitive effects of methamphetamine: A critical review and meta-analysis. Neuropsychol Rev 17(3): 275-297.
- Fisher PL, Wells A (2008) Metacognitive Therapy for Obsessive-Compulsive Disorder: A case series. J Behav Ther Exp Psychiatry 39(2): 117-132.
- Griffin D, Kahnaman D (2002) Heuristics and Biases the Psychology of Intuitive Judgment. In: Gilovich (T) (Ed.), Cambridge University Press, Australia.
- Heather N, Wodak A, Nadelmann EA, O Hare P (1993) Psychoactive Drugs and Harm Reduction: From Faith to Science. Whurr Publishers, London.
- Hetrick SE, Purcell R, Garner B, Parslow R (2012) Combined pharmacotherapy and psychological therapies for post traumatic stress disorder (PTSD) (Review). Cochrane Collaboration.
- Jenner L, Lee N (2008) Treatment Approaches for Users of Methamphetamine: A Practical Guide for Frontline Workers. Australian Government Department of Health and Ageing: Canberra, Australia.
- Karch SB (2007) Drug abuse handbook. (2nd edn), CRC Press, Boca Raton, Florida, US.
- Mausbach BT, Semple SJ, Strathdee SA, Zians J, Patterson TL (2007) Efficacy of a behavioral intervention for increasing safer sex behaviors in HIV-negative, heterosexual methamphetamine users: Results from the Fast-Lane Study. Annals of Behavioral Medicine 34(3): 263-274.
- McCorry LK (2007) Physiology of the autonomic nervous system. American journal of pharmaceutical education 71(4): 78-89.
- Melnikova N, Welles WL, Wilburn R, Rice WJ, Stanbury M (2011) Hazards of Illicit Methamphetamine Production and Efforts at Reduction: Data from the Hazardous Substances Emergency Events Surveillance System. Public Health Reports, Supplement 126(1): 116-123.
- Mihailides S, Galligan R, Bates G (2017) Adaptive Psychopathy: Empathy and Psychopathy are Not Mutually Exclusive. Journal of Forensic Psychology 2: 125.
- Mithoefer MC, Wagner MT, Mithoefer AT, Jerome L, Doblin R (2011) The safety and efficacy of ±3,4-methylenedioxymethamphetamine-assisted psychotherapy in subjects with chronic, treatment-resistant posttraumatic stress disorder: the first randomized controlled pilot study. J Psychopharmaco 25(4): 439-452.
- Previc F (2011) Dopamine, altered consciousness, and distant space with special reference to shamanic ecstasy. In: Etzel C, Winkelman M (Eds.), Altering consciousness: Multidisciplinary perspectives (Vols 1 and 2): History, culture, and the humanities; Biological and psychological perspectives. Santa Barbara, Praeger, California, USA, pp. 43-61.
- Randrianame M, Szendrei K, Tongue A (1983) The Health and Socioeconomic Aspects of Khat Use. International Council on Drug and Addictions: 140-143.
- Reinarman C, Levine HG (1997) Crack in America: Demon Drugs and Social Justice. University of California Press, USA.
- RxList the Internet Drug Index. Desoxyn (Methamphetamine Hydrochloride) Drug Information: User Reviews, Side Effects, Drug Interactions and Dosage.
- Scott JC, Woods SP, Matt GE, Meyer RA, Heaton RK, et al. (2007) Neurocognitive effects of methamphetamine: a critical review and meta-analysis. Neuropsychol Rev 17(3): 275-297.
- Volkow ND, Wang G, Fowler JS, Telang F, Millard J, et al. (2007) Stimulant-induced enhanced sexual desire as a potential contributing factor in HIV transmission. The American Journal of Psychiatry 164(1): 157-160.
- Wells A, King P (2006) Metacognitive Therapy for Generalized Anxiety Disorder: An open trial. Journal of Behavior Therapy and Experimental Psychiatry 37(3): 206-212.
- Wells A, Welford M, King P, Papageorgiou C, Wisely J, et al. (2010) A pilot randomized trial of metacognitive therapy vs applied relaxation in the treatment of adults with generalized anxiety disorder. Behaviour Research and Therapy 48(5): 429-434.
- Wells A, Papageorgiou C (2001) Brief Cognitive Therapy for Social Phobia: A case series. Behaviour Research and Therapy 39(6): 713-720.
- Wells A, White J, Carter K (1997) Attention Training: Effects on anxiety and beliefs in panic and social phobia. Clinical Psychology and Psychotherapy 4(4): 226-232.






























