Postmortem Blood Culture Profile in Sudden Cardiac Death: An Exploratory Study
Noé López-Amador1, Jorge Alberto Alfonso-Bravo1, Karina Ortíz-Valdez1 and Octavio Carvajal-Zarrabal2*
1Institute of Forensic Medicine, University of Veracruz, Mexico
2Biochemical and Nutrition Chemistry Area, University of Veracruz, México
Submission: September 20, 2017; Published: September 27, 2017
*Corresponding author: Octavio Carvajal-Zarrabal, Biochemical and Nutrition Chemistry Area, University of Veracruz, SS Juan Pablo II s/n, 94294 Boca del Río, Veracruz., México, Tel: 52-229-9218741; Email: ocarvajal@uv.mx
How to cite this article: L�pez-Amador N, Alfonso-Bravo JA, Ortiz-Valdez K, Carvajal-Zarrabal O. Postmortem Blood Culture Profile in Sudden Cardiac Death: An Exploratory Study. J Forensic Sci & Criminal Inves. 2017; 5(3): 555665. DOI: 10.19080/JFSCI.2017.05.555665
Abstract
The main objective of this work was to explore the bacteriological profile of postmortem blood cultures in a small case series of medico legal autopsies diagnosed with sudden cardiac death compared to non-cardiac origin deaths. Cardiac injury markers were determined in blood samples by an immunoassay kit in both groups to reinforce sudden cardiac death diagnosis. In sudden cardiac death group (n=20), cultures were positive to Escherichia coli (50%; 10/20), Staphylococcus aureus (20%; 4/20), Klebsiellapneumonie (20%; 4/20), Candida albicans (15%; 3/20) and Staphylococcus epidermis (10%; 2/20). Non-cardiac origin death group (n=8) were positive to E. coli (25%; 2/8). Sudden cardiac death cases showed significant (p<0.05) higher levels of cardiac troponins I and T compared to control. Postmortem blood cultures in this study had a sensitivity of 100%, a specificity of 75%, a positive predictive value of 91% and a negative predictive value of 97%. Although the sample size was small; we conclude that a positive postmortem blood culture isolating pathogenic bacteria is a marker of systemic infection and it conditions a higher risk of sudden cardiac death in chronic patients.
Keywords: Sudden cardiac death; Postmortem blood culture; Troponins; Postmortem bacteremia; Staphylococcus aureus; Klebsiellapneumonie
Introduction
Sudden cardiac death (SCD) causes over 17 million deaths annually or 30% of all global mortality, one of the highest incidences worldwide. Ventricular tachyarrhythmia is present in 80% of the cases as the main cause, and it means 40-50% of all cardiovascular deaths [1]. Infectious diseases have been associated with cardiac illness leading to SCD, in a wide range of agents, such as parvovirus B19, human immunodeficiency virus (HIV), tuberculosis, lactococcus, B-group streptococci, influenza A/H1N1, Rickettsia, Epstein-Barr virus (EBV) and staphylococcal disease. All these agents induce cardiovascular pathology by causing endocarditis/endarteritis, affecting cardiac rhythm and enhancing prothrombotic states; affecting both adults and children by equal. Molecular mechanisms underlying SCD associated to infectious diseases remains to be unclear [2-10].
Postmortem bacteremia (PB) may occur during early postmortem changes because these changes facilitate the access of the human microbiota to capillary circulation. Thus, postmortem blood cultures (PMBC) growing non-pathogenic bacteria should be considered caused by PB, but not necessarily a case of sepsis [11]. In the other hand, growing of pathogenic bacteria in a PMBC should become suspicious of sub-acute or chronic systemic infectious disease (e.g. bacterial endocarditis) [12]. Frequently, viral myocarditis cases show no gross signs of cardiac pathology, until microscopic inflammatory cell infiltrated is observed in histopathologic study. In these cases, viral cultures and serology must be performed [13]. The main objective of this work was to explore the bacteriological profile of PMBC in a small series of medico legal autopsy cases diagnosed with SCD compared to non-cardiac origin deaths (NCOD).
Method
Subjects and protocol
The study was conducted at the Medical Examiner's Office of the Institute of Forensic Medicine at the Universidad Veracruzana (UV). In all SCD cases, the fainting of the patients was witnessed by third parties, occurring either at home or on the public road. We also included cases in which patients went to a hospital after developing cardiac symptoms, dying while they were transferred to an emergency room, not being admitted for this reason. These clinical backgrounds required a forensic autopsy per legal procedures. Main diagnosis of these cases was compatible with cardiogenic shock, per external and internal signs of acute cardiac failure observed during autopsy by the medical examiner. The study also included eight bodies with a diagnosis of violent death (NCOD) admitted for a judicial autopsy, as control group. All recommendations of the Research Commission at the Instituto de MedicinaForense and the Ethics Committee of the Universidad Veracruzana were followed. The inclusion criteria involved corpses with a postmortem interval of up to 8-h determined through the clinical history and an evaluation of early postmortem changes. The bodies arrived at the autopsy room and were kept at room temperature of 21°C given by the air-conditioning. Forensic autopsies were performed in the following 2-h of arrival, collecting and processing blood samples with priority. To reinforce the diagnosis of SCD, we used immunoassay method, the same one used in clinical practice using commercial kits, accessible to any laboratory to determine troponins and other cardiac injury biomarkers. Degradation of the protein can modify the reading, and this occurs with the decrease in the pH levels and the progressive bacterial enzymatic activity in postmortem intervals greater than 8-h, for this reason, we did not include cases with a longer postmortem interval.
Blood sampling and cultures
Blood samples were taken from the pulmonary artery using an aseptic puncture technique. Briefly, dissection of the body was performed by a technician cleaning the skin with ethanol 70%, changing to sterile gloves and using sterilized surgical instruments when entering to thoracic cavity, exposing the pulmonary artery to the sample collector. By aseptic technique, sample collector used a heat seal on the site of puncture to prevent external contamination just before puncturing and filling of a commercial vacuum system without anticoagulant (Vacutainer ™ , Becton-Dickinson). Blood sample was taken to laboratory and incubated in a bacteriological stove for 24-h at 36°C in stabilizing medium (liquid phase: 30 ml biotriptase, Sodium Polyanethole Sulfonate 0.04%; solid phase: 25 ml biotriptase, agar). After incubating, the sample was inoculated in four culture plates, each containing one of the following media: blood-agar, MacConkey-agar, manitol salt-agar, chrome- agar. Once inoculated, plates were placed in stove at 36°C, for incubating up to 72-h. After this time, if there was no bacterial growing, the result was considered negative. If bacterial growing was detected in mannitol-salt agar, we used coagulase test for identification of Staphylococcus Sp. Identification of all microorganisms was made per characteristics of growth and morphology of each species.
Analysis of cardiac injury biomarkers
All determinations for cardiac injury markers were performed on blood samples obtained from pulmonary artery, as explained before, using heparin and ethylenediaminetetraacetic acid (EDTA) as an anticoagulant. Also, another sample without anticoagulant was taken in each case. Samples were stored at 80°C for further analysis. The MB fraction of creatine kinase, myoglobin, and troponin I was determined with the fluoro immunoassay method using Alere Triage ® MeterPro equipment (Alere Cologne, Germany). Troponin T was determined by an immunoassay method using a Roche Cobas ® h 232 Troponin T analyzer (USA). An enzymatic colorimetric method (Bayer, Germany) and RA-50 Chemistry Analyser equipment (Bayer, Germany) were used for the determination of lactate dehydrogenase.
Statistical analysis
Data were expressed as means standard deviation (x + SD). Statistical significance was determined by variance analysis procedures, with a post hoc Tukey multiple range test for comparison of means (p < 0.05). Data were analyzed using an iBMCSPSSc, " Escherichia coli," "Klebsiella pneumoniae" Package, version 20, 2011.
Results
Differences between bacteriological profile of SCD cases compared to NCOD cases
SCD group had 20 cases, from subjects deceased by acute cardiac failure (i.e. cardiogenic shock) diagnosed per medical examiner after autopsy performance. There were 14 males and 6 females in this group, with an age-rank within 37 to 81 years, (Mean: 58.7 ± 12.8). All cultures for this group grew one or more microorganisms. The genus and the different isolated species are summarized in Table 1. The most common grampositive bacteria species identified were Staphylococcus aureus and Staphylococcus epidermis. The most common gram-negative bacteria were Escherichiacoli, and Klebsiellapneumoniae. In addition, within the unicellular microorganism's fungi or yeasts, Candida albicans was also isolated.
NCOD group, used as control, had a total of 8 cases deceased by polytrauma (2/8; 25 %), asphyxia (4/8; 50 %) and sharp force injury (2/8; 25 %) (Table 2) All cases of this group were male. Age-rank oscillated from 21 to 59 years (Mean: 36.3 ± 11.4). Only two of these cultures (asphyxia) were positive, growing colonies of E. coli, but no other microorganism was detected in blood cultures of this group.
Overall, five bacterial species were isolated from autopsy cases diagnosed with SCD and one species of cases with diagnosis NCOD (Table 3). All of the pathogens Escherichiacoli were present 50% (10/ 20) of cases. Staphylococcus aureus and Klebsiellapneumoniae, each species was present in 20% (4/20) of SCD cases. Interesting, three of these SCD cases presented mixed blood cultures of Candida albicans coexisting with E. coli (15%). Staphylococcus epidermis was isolated in 2/20 cases (10%). In the case of the control group, E.coli represented 25%. Some blood cultures had more than one bacterial species, so the percentage of the sum is greater than 100.
Biochemical analysis of cardiac injury markers
To reinforce SCD diagnosis, we determined cardiac injury markers in blood samples obtained from all cases of this study using commercial kits for creatine kinase MB (CK-MB), myoglobin (MB), lactate dehydrogenase (LDH), cardiac troponin I (cTn-I) and cardiac troponin T (cTn-T), as described in methods. Surprisingly, we found CK-MB levels significant (p <0.01) higher in NCOD than SCD group; nevertheless, cTnI and cTnT levels raised significant (p< 0.05) higher in SCD group compared to control. Average values of cardiac injury markers compared between groups are shown in Table 4.
Discussion
This study aimed to explore the bacteriological profile of PMBC in SCD cases compared to NCOD cases. We found data suggesting that SDC cases are prone to develop PB. Several studies had described the presence of bacteremia or systemic infectious disease in life-threatening complications, including SCD [14,15]. It has been proposed that sudden unexpected death in infancy (SUDI) is caused by common bacterial toxins produced mainly, but not exclusively, by upper respiratory tract bacteria [16]. Our results suggest this is possible for adults too. Microorganisms isolated from these cultures have different implications depending on context. E. coli was the most frequent characterized bacteria in SDC blood cultures; however, this bacterium is part of the gut microbiota in humans. A few hours after death, E. coli reaches gross vessels and disseminate by entering to capillaries of the intestinal mucous membrane, according to postmortem bacterial transmigration theory [11]. We could consider that cultures positive to this bacterium are frequent for this reason and does not mean necessarily a systemic disease. Instead, E. coli is one of the most commonly isolated bacteria in urinary tract infections, and could induce sepsis, depending on predisposing factors (e.g. chronic illness like diabetes and carcinoma) and virulence of strains; as well as genome differences between E. coli isolated from septicemia cases has been reported previously [17]. This fact should be considered in cases where inflammatory and degenerative changes in kidney parenchyma are observed during autopsy. Bacterial cultures should be practiced from kidney tissue in these cases [13].
Our results found that S. aureus and K. pneumoniae are the second most commonly isolated microbes from our SDC cases. This result is like others describing bacteremia in natural death cases of patients with multiple diagnostics of chronic pathology [12]. Both bacteria are pathogenic and could cause system pathology (e.g. urinary tract/upper and lower airway infections) as well as an acute or chronic disease [18,19]. They are antibiotic resistant, making eradication difficult [20,21]. Enzymes like coagulase, produced by S. aureus, favors disseminated intravascular coagulation by converting fibrinogen to fibrin. Other molecules on the bacteria surface induce inflammatory states in organs and tissues of the host (e.g. myocardium and endothelium) [22,23]. All these facts contribute to increase the SCD risk [16].
S. epidermis, a non-usually pathogenic germ that forms part of human skin microbiota, is often isolated in contaminated cultures. This bacterium could reach systemic circulation by means of a skin injury (e.g. ulcers, wounds, eschars, abrasions). Once in the blood stream, this bacterium turns pathogenic causing systemic disease depending on host conditions [24,25]. We found two cases positives to S. epidermis. We cannot rule out the possibility of sample contamination. However, one of these cases was an 81-years old male with presence of skin lesions, explaining this result (Table 1).
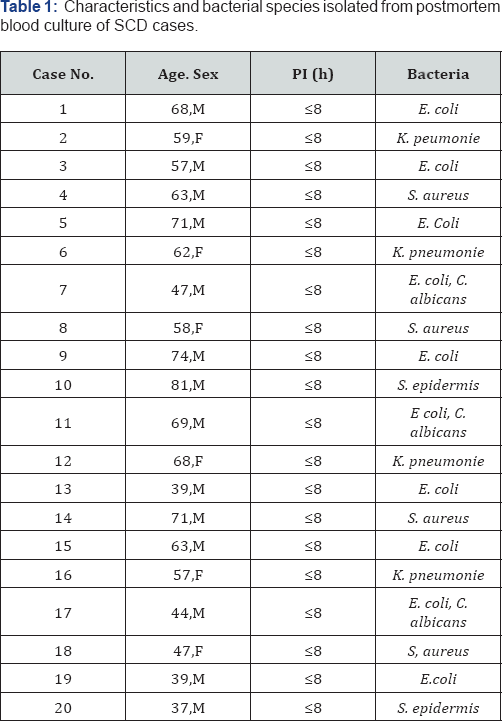
Postmortem interval (PI); Escherichia coli (E. coli); Klebsiellapneumonie (K. pneumonie); Candidaalbincas (C. albicans); Staphylococcusaureus (S. aureus); Staphylococcus epidermis (S. epidermis).
We obtained two positive cultures for C. albicans, one of the most common opportunistic germs in microbial pathology isolated in the blood stream [26,27]. These cases coexisted with positive cultures for E. coli, in vitro association of this germs has been reported to improve resistance and virulence of bacteria through fungal glucans [28]. Chronic patients often had a degree of impaired immune response, and we believed this condition elicits co infection. At last, we found these cases were afflicted by metabolic syndrome according to medical records. None of the NCOD cases had a culture positive for pathogenic bacteria, being positive for two cases of E. coli. Despite this, we consider the need of a larger control group, without impairing a longer case series for a more representative study. Also, the average age in both groups was significantly different (SCD: 58.7 ± 12.8, vs NCOD: 36.3 ± 11.4; p<0.01) and this fact influence clinical backgrounds, being older patients the most exposed to chronic illness and systemic infections.
Finally, we measured cardiac injury markers to reinforce SCD diagnosis. As expected, SCD group raised significant higher levels of cardiac troponins than NCOD. This data supports the acute cardiac failure diagnosis determined by medical examiner after practicing medico legal autopsy of these cases. Biochemical assays are an easier and faster way to confirm the diagnosis, compared to histological techniques, despite the cost. The significant higher levels of CK-MB in NCOD cases do not affect diagnosis since cardiac troponins are highly specific and sensitive for cardiac injury in vivo and postmortem [29,30]. Besides CK-MB levels are higher in death by asphyxia [31] and 50% of the control cases died in this manner (Table 2). Curiously, two of the four asphyxia cases were positive for E. coli.
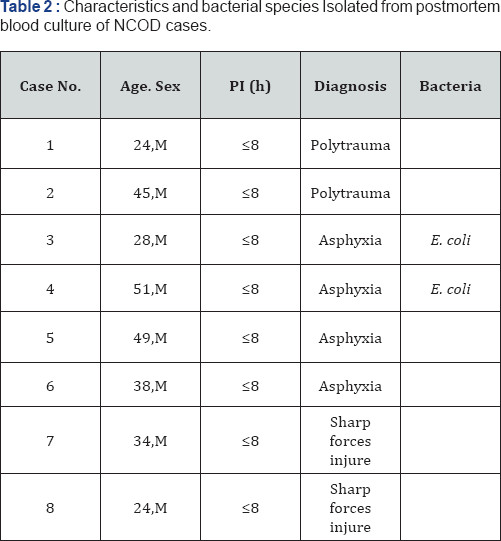
Postmortem interval (PI); M (Male); Escherichia coli (E. coli).
On the other hand, the value of a pathological test is best expressed in terms of sensitivity and specificity. This allows that values of predictive positive (PPV) and negative (NPV) value be calculated at different probability to priority levels. In this study, we report a series of cases in which blood cultures were obtained at < 8 hours after death. Of 28 cases in 6 (21.4%) there was no bacterial growth, 19 (67.9%) grew a simple microorganism and in 3 cultures produced 2 microorganisms (10.7%). In 20 cases, the postmortem diagnosis indicated acute cardiac failure; all these cases gave positive blood cultures. In the 8 cases, the diagnosis indicated non-cardiac death, 2 cultures were positive and 6 negative. From these figures, a positive blood culture can be calculated as a marker of asubacute systemic infection, when the isolated microbe is known to be pathogenic. Therefore, this series of cases had a sensitivity of 100%, a specificity of 75% and a PPV of 91%, and an NPV of 97%. In addition, in SCD cases were met microorganisms in blood that were not expected and apparently unrelated to the cause of death (E. coli, S. epidermis, and C. albicans). However, S. aureus and S. pneumoniae were found, which their presence correlates with the cause of death.
In Summary, our study shows that in this small case series, SCD trends to be positive for PMBC compared with NCOD. In these cultures, E. coli is commonly isolated and this germ is usually part of gut microbiota in humans, but in some circumstances, it could induce systemic disease, as well as other non-pathogenic or opportunistic germs (e.g. S. epidermis, C. albicans). "S. aureus "and "K. pneumoniae"are the most frequent pathogenic bacteria isolated in these cases, and these bacteria are directly related to systemic and chronic diseases. In this order of ideas, clinicians must diagnose opportunely subacute infections of these or other pathogenic germs and eradicate them to avoid elevated risk of sudden cardiac death in chronic patient. In this study, the degree of bacterial detection ranged from 25 to 100% positive samples at < 8 hours, with species of five main groups of bacteria coming from postmortem fluid (pulmonary artery blood).Within the most pathogenic S.aureus and K.pneumoniae were found. Also, SCD cases showed significantly higher postmortem levels of troponin I (cTn-I) and troponin T (cTn-T). Our results suggest that the usefulness of blood cultures and biomarkers of cardiac damage obviously contributes as an aid tool to detect potentially infectious deaths in case of uncertain deaths and detection of deaths due to unexpected or sudden deaths. This information can be valuable for daily practice and future studies in the value of bacteriology autopsy, forensic biochemistry, and criminal medicine.
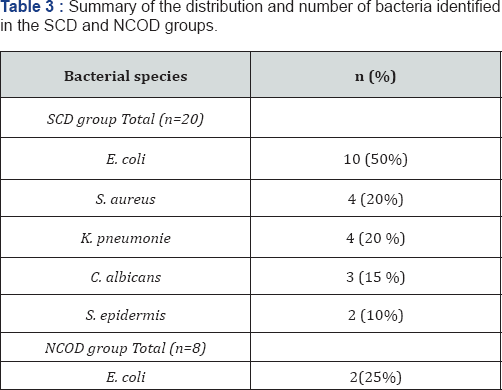
All isolated bacterial species were reported and more than one bacterial species was occasionally identified, observing the percentage of sum greater than 100%. The values are displayed as absolute numbers and percentages (%).
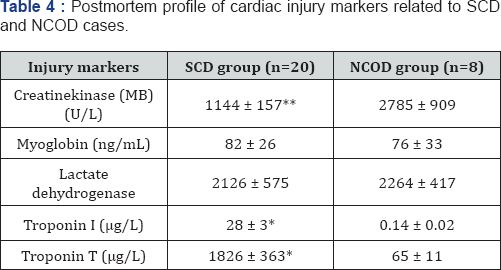
Values are mean ± SD. *P<0.05; **P<0.01 vs corresponding data in NCOD group.
References
- Mehra R (2007) Global public health problem of sudden cardiac death. J Electrocardiol 40(6 Suppl): S118-S122.
- Juhasz Z, Tiszlavicz L, Kele B, Terhes G, Deak J, et al. (2014) Rudas, Sudden cardiac death from parvovirus B19 myocarditis in a young man with brugada syndrome. J Forensic Leg Med 25: 8-13.
- Moyers BS, Secemsky EA, Vittinghoff E, Wong JK, Havlir DV, et al. (2014) Effect of left ventricular dysfunction and viral load on risk of sudden cardiac death in patients with human immunodeficiency virus. Am J Cardiol 113: 1260-1265.
- Liu A, Hu Y, Coates A (2012) Sudden cardiac death and tuberculosis - how much do we know? Tuberculosis 92: 307-313.
- Taniguchi K, Nakayama M, Nakahira K, Nakura Y, Kanagawa N, et al. (2016) Sudden infant death due to lactococcal infective endocarditis. Leg Med (Tokyo) 19: 107-111.
- Kawaguchi T, Hama M, Abe M, Suenaga T, Ishida Y, et al. (2013) Sudden unexpected neonatal death due to late onset group B streptococcal sepsis--a case report. Leg Med (Tokyo) 15: 260-263.
- Gdynia G, Schnitzler P, Brunner, E, Kandolf R, Blaker H, et al. (2011) Sudden death of an immunocompetent young adult caused by novel (swine origin) influenza A/H1N1-associated myocarditis. Virchows Arch 458: 371-376.
- Nilsson K, Lindquist O, Pahlson C (1999) Association of Rickettsia helvetica with chronic perimyocarditis in sudden cardiac death. Lancet 354: 1169-1173.
- Farina A, Maggiolini S, Di Sabato M, Gentile G, Meles E, et al. (2011) Aborted sudden death from Epstein-Barr myocarditis. J Cardiovasc Med 12: 843-847.
- Anguera I, Quaglio G, Ferrer B, Nicolás JM, Paré C, et al. (2001) Sudden death in Staphylococcusaureus-associated infective endocarditis due to perforation of a free-wall myocardial abscess. Scand J Infect Dis 33: 622-625.
- Morris JA, Harrison LM, Partridge SM (2007) Practical and theoretical aspects of postmortem bacteriology. Curr Diagn Pathol 13: 65-74.
- Sunagawa K, Sugitani M (2017) Postmortem detection of bacteremia using pairs of blood culture samples. Leg Med (Tokyo) 24: 92-97.
- Dowling G (2005) Sudden Natural Death, In: D Dolinak, EW Matshes, Lew EO (Eds.), Forensic Pathology: Principles and Practice. Elsevier Academic Press. San Diego, California. USA, pp. 71-116.
- Rae N, Finch S, Chalmers JD. Cardiovascular disease as a complication of community-acquired pneumonia. Curr. Opin. Pulm. Med. 2016; 22:212-218. Brown AO, Millett ER, Quint JK, Orihuela CJ (2015) Cardiotoxicity during invasive pneumococcal disease. Am J Respir Crit Care Med 191: 739-745.
- Morris JA, Harrison LM, Biswas J, Telford DR (2007) Transient bacteraemia: a possible cause of sudden life threatening events. Med Hypotheses 69: 1032-1039.
- Chakraborty A, Adhikari P, Shenoy S, Saralaya V (2015) Genomic analysis and clinical importance of Escherichia coli isolate from patients with sepsis. Indian J Pathol Microbiol 58: 22-26.
- Bowles D, Perrin K (2014) A retrospective case series of 44 patients with community-acquired Staphylococcus aureus pneumonia. N Z Med J 127: 74-83.
- Lin WH, Kao CY, Yang DC, Tseng CC, Wu AB, et al. (2014) Clinical and microbiological characteristics of Klebsiellapneumoniae from community-acquired recurrent urinary tract infections. Eur J Clin Microbiol Infect Dis 33: 1533-1539.
- Chen X, Sun K, Dong D, Luo Q, Peng Y, et al. (2016) Antimicrobial Resistance and Molecular Characteristics of Nasal Staphylococcus aureus Isolates From Newly Admitted Inpatients. Ann Lab Med 36: 250-254.
- Chaudhary P, Bhandari D, Thapa, K, Thapa P, Shrestha D, et al. (2016) Prevalence of Extended Spectrum Beta-Lactamase Producing Klebsiella Pneumoniae Isolated From Urinary Tract Infected Patients. J Nepal Health Res Counc 14: 111-115.
- Shankar-Sinha S, Valencia GA, Janes BK, Rosenberg JK, Whitfield C, et al. (2004) The Klebsiellapneumoniae O antigen contributes to bacteremia and lethality during murine pneumonia. Infect. Immun 72: 1423-1430.
- Kim CK, Karau MJ, Greenwood-Quaintance KE, Tilahun AY, Krogman A, et al. (2015) Superantigen-producing Staphylococcus aureus elicits systemic immune activation in a murine wound colonization model. Toxins 7: 5308-5319.
- Otto M (2009) Staphylococcus epidermidis--the 'accidental' pathogen. Nat Rev Microbiol 7: 555-567.
- Heikkonen L, Palmu A, Böstman O (1986) Multiresistant Staphylococcus epidermid is as a pathogen. Ann Clin Res 18: 80-83.
- Shigemura K, Osawa K, Jikimoto T, Yoshida H, Hayama B, et al. (2014) Comparison of the clinical risk factors between Candida albicans and Candida non-albicans species for bloodstream infection. J Antibiot (Tokyo) 67: 311-314.
- Rajendran R, Sherry L, Nile CJ, Sherriff A, Johnson EM, et al. (2016) Biofilm formation is a risk factor for mortality in patients with Candida albicans bloodstream infection-Scotland, 2012-2013.Clin Microbiol Infect 22: 87-93.
- De Brucker K, Tan Y, Vints K, De Cremer K, Braem A, et al. (2015) Fungal β;-1,3-glucan increases ofloxacin tolerance of Escherichia coli in a polymicrobial E. coli/Candida albicans biofilm, Antimicrob. Agents Chemother 59: 3052-3058.
- Priori SG, Aliot E, Blomstrom-Lundqvist C, Bossaert L, Breithardt G, et al. (2002) Task force on sudden cardiac death of the European Society of Cardiology: Summary of recommendations. Ital Heart j suppl 3(10): 1051-1065.
- Antman E, Bassand JP, Klein W, Ohman M, Lopez-Sendon JL, et al. (2000) Myocardial infarction redefined- a consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction. J Am Coll Cardiol 36: 959-969.
- Zhu BL, Ishikawa T, Michiue T, Li DR, Zhao D,et al. (2007) Postmortem cardiac troponin I and creatinekinase MB levels in the blood and pericardial fluid as markers of myocardial damage in medicolegal autopsy. Leg Med (Tokyo) 9: 241-250.






























