Neurology in Endocrine Disorders
David Enrique Barbero Jiménez1*, Judit Villamor Rodríguez1, Maria de la Cruz Barbero Jiménez2 and Diego Domingo Merino3
1Departament of Neurology, Hospital Universitario de Guadalajara, Guadalajara, Spain
2Departament of Oncology, Hospital General Universitario de Nuestra Señora del Padro, Talavera de la Reina, Spain
3Departament of Hematology, Hospital Universitario Gregorio Marañón, Madrid, Spain
Submission: June 20, 2023; Published: July 27, 2023
*Corresponding author: David Enrique Barbero Jiménez, Department of Neurology, Hospital Universitario de Guadalajara, Guadalajara, Spain. Email: dbarberoj@sescam.jccm.es
How to cite this article: David Enrique Barbero Jiménez*, Judit Villamor Rodríguez, Maria de la Cruz Barbero Jiménez and Diego Domingo Merino. Neurology in Endocrine Disorders. J Endocrinol Thyroid Res. 2023; 7(3): 555713. DOI:10.19080/JETR.2023.07.555713
Abstract
Endocrine diseases can present initially with neurological symptoms. It is very important to consider diseases related to the endocrine system in the differential diagnosis of neurological clinic. There are very serious diseases that can present with neurological alterations such as hypoglycemia that can cause death if not diagnosed in time. The objective of this review is to carry out a description of the main endocrinological pathologies and their relationship with neurology.
Keywords: Hypoglycemia; Hypofunction; Adenohypophysis; Hyperprolactinemia
Pituitary Disorders
Panhypopituitarism
Intrinsic pituitary or hypothalamic lesions can cause pituitary hypofunction. Expansive pituitary lesions can lead to hypofunction of one or more hormones, although panhypopituitarism is rare. In large expansive lesions, an alteration of the neurohypophysis with the development of diabetes insipidus, along with dysfunction of one or several hormones of the adenohypophysis, may be observed. Additionally, a marked elevation of prolactin due to hypothalamic-pituitary stalk dysfunction is frequently found. However, pituitary lesions that can cause this clinical picture often generate dysfunction of neighboring structures, especially the optic chiasm with visual field disorders, or the oculomotor nerves within the cavernous sinus, causing diplopia.
Vascular lesions of the pituitary, particularly pituitary apoplexy, can cause a sudden and severe picture of panhypopituitarism along with symptoms of headache, meningeal irritation, visual disturbances, and decreased level of consciousness. Hypophysial ischemia can occur immediately in the postpartum and is known as Sheehan’s syndrome. This complication usually occurs in complicated deliveries with hypotension and obstetric hemorrhage. Ischemia usually leads to predominant hypofunction of the adenohypophysis, with the association of diabetes insipidus being rare. Subacute and chronic postpartum conditions with symptoms of persistent amenorrhea, decreased libido, and lack of lactation have also been described.
Pituitary Tumors
Most pituitary tumors are associated with lesions in the adenohypophysis. The clinical presentation is directly related to the size of the tumor and the (non)secretion of hormones. Microadenomas (less than 10 mm in size) produce symptoms related to hormonal production, while macroadenomas (larger than 10 mm in size) can cause dysfunction of the hypothalamic- pituitary stalk, hormonal hypofunction due to local compression of pituitary tissue, and even [1].
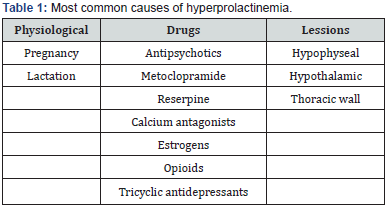
invasion of neighboring structures such as the cavernous sinus and optic chiasm. Prolactinomas are the most frequently observed hormonally secreting tumors. However, numerous causes of hyperprolactinemia, including physiological states, various medications, and lesions affecting the hypothalamic-pituitary region (Table 1), must be recognized. In any case, elevated levels of prolactin, especially above 200 μg/L, are usually associated with prolactinomas. The diagnostic test of choice for evaluating pituitary lesions is magnetic resonance imaging (MRI), usually with contrast. Hormone measurements are obviously useful for determining pituitary function and assessing the presence of a hypersecreting tumor. The treatment of pituitary tumors includes pharmacological therapy, radiation therapy, and surgery. Hyperprolactinemia usually responds to dopamine agonists such as bromocriptine and cabergoline. This treatment is often used for both macro- and microadenomas. In the former, it is used to reduce the size of the lesion, and in all cases, it aims to normalize prolactin levels and prevent its pathological consequences. Surgery is usually reserved for macroadenomas using a transsphenoidal surgical approach. The indication is clear in cases of local invasion, especially with involvement of the optic chiasm or cavernous sinus. Radiation therapy, either alone or in combination with surgery or medications, is usually reserved for cases with incomplete resection or high surgical risk that precludes intervention.
Thyroid Disorders
Hypothyroidism
Congenital hypothyroidism leads to a condition called cretinism, which encompasses a distinct phenotype along with notable mental retardation. However, neurologists often encounter acquired alterations in adulthood in the form of acute hypothyroidism or myxedema, as well as more chronic forms. The clinical picture of acute hypothyroidism usually manifests as a severe and rapidly progressive mental disorder with bradypsychia, drowsiness, and coma. Patients often present with hypothermia, hypotension, and metabolic disorders. It is a serious and potentially life- threatening condition if not promptly treated. Parenteral administration of T4 or T3 is an option, although caution must be exercised as it can trigger cardiac failure or ischemic heart disease if done too quickly. In the case of chronic hypothyroidism, the clinical presentation is more diverse and may include sensory neuropathy, nerve trunk entrapment such as carpal tunnel syndrome, cerebellar ataxia, and cognitive disorders. In these cases, treatment involves the use of oral levothyroxine [2].
Hyperthyroidism
Excessive thyroid hormone production results in a clinical picture of hypermetabolism with marked autonomic dysfunction. Patients often exhibit tachycardia, hypertension, sweating, tremors, and nervousness. In severe cases, it can be associated with mental status disturbances, including confusion and psychosis. Autoimmune hyperthyroidism is referred to as Graves’ disease, which presents as hyperthyroidism accompanied by cutaneous and ophthalmological symptoms. Graves’ ophthalmopathy, characterized by infiltration of orbital elements with edema and local fibrosis, is a notable feature, leading to exophthalmos and diplopia. The condition can be asymmetric between both orbits, and without treatment, it can lead to blindness due to various complications. Treatment includes not only antithyroid medications but also corticosteroids, radiotherapy, or surgical orbital decompression in extreme cases.
Thyrotoxic myopathy is a rare complication of hyperthyroidism characterized by painless progressive weakness of the pelvic musculature, and to a lesser extent, the shoulder musculature. Fasciculations or myokymia are not uncommon. Lastly, thyrotoxic periodic paralysis is an infrequent condition more commonly seen in individuals of Asian descent, characterized by episodes of diffuse muscle paralysis associated with exercise or meals. Attacks can be reduced with the use of propranolol, although proper treatment involves correcting the thyroid disorder. Hashimoto’s thyroiditis is an autoimmune condition affecting the thyroid gland, leading to either hypothyroidism or hyperthyroidism [3].
The presence of antithyroid antibodies is key to the diagnosis. This condition has been associated with various disorders such as myasthenia gravis and, particularly, recurrent encephalopathy that responds to immunosuppressive treatment. Hashimoto’s encephalitis typically presents in association with high titers of thyroid antibodies, with symptoms including confusion, disorientation, and subsequently decreased level of consciousness. The occurrence of movement disorders such as tremors or myoclonus is not uncommon. Neuroimaging is typically normal, showing diffuse slowing on EEG, and cerebrospinal fluid (CSF) analysis reveals elevated protein levels without significant pleocytosis. The treatment of choice is high-dose corticosteroid boluses, such as 1000 mg of methylprednisolone for 3-5 days. In the absence of response, other immunosuppressive therapies may be employed.
Parathyroid Gland Disorders
Hyperparathyroidism leads to a condition of hypercalcemia and, therefore, neurological, and systemic symptoms associated with this condition. Mild cases can cause symptoms such as constipation, nausea, vomiting, abdominal pain, eventually progressing to diffuse encephalopathy and weakness. Hypoparathyroidism is commonly associated with patients who have undergone thyroidectomy, which also involves the removal of the parathyroid glands. Pseudohypoparathyroidism refers to a condition in which parathyroid secretion is normal, but there is peripheral resistance to its action. Neurological effects are usually linked to the presence of hypocalcemia, but it is common to find intracranial calcifications, especially in the basal ganglia, in these patients without significant clinical symptoms. It has also been associated with idiopathic intracranial hypertension, although a clear causal mechanism between the two phenomena has not been established.
Blood Glucose Disorders
Hyperglycemia
Hyperglycemia occurring in the context of Diabetes Mellitus (DM) can lead to multiple complications in both the central and peripheral nervous systems. The most common complication of DM is peripheral neuropathy, which is the most common cause of neuropathy in the Western world. Symptoms typically affect the distal region of the limbs and include paresthesia, sensory loss, and neuropathic pain. In severe cases, it can progress to distal ulcers and arthropathy. Autonomic neuropathy is often an additional element to the above, although it can sometimes be the dominant manifestation. Clinical manifestations can vary and may include orthostatic hypotension, sweating disorders, changes in gastric emptying and constipation, and sexual dysfunction with impotence. Diabetic polyradiculopathy or diabetic plexopathy is an asymmetric subacute condition characterized by weakness, paresthesia’s, and neuropathic pain in the lower limbs. It typically begins unilaterally with a subacute onset followed by slow improvement over months [4].
In the central nervous system, the main morbidity associated with DM is its association with ischemic stroke, constituting a key risk factor. Diabetic ketoacidosis can mark the onset of DM, usually type 1, and lead to a severe and potentially life-threatening condition. Patients develop rapidly progressive encephalopathy that can lead to coma. Non-ketotic hyperglycemia can also cause severe encephalopathy and coma, usually associated with patients with type 2 DM as a complication of various systemic conditions. There is a described condition of movement disorders in patients with non-ketotic hyperglycemia, typically chorea or hemichorea. The condition tends to improve slowly after glucose correction.
Hypoglycemia
Severe hypoglycemia triggers acute encephalopathy. Initially, the patient may feel nervous and shaky, followed by a decrease in the level of consciousness. In these cases, focal neurological signs may appear, mimicking a focal ischemic stroke, leading to a mistaken diagnosis. Prolonged severe hypoglycemia can cause irreversible damage to the central nervous system, especially in the cerebral cortex and basal ganglia.
Disorders of the adrenal gland
The tumor secretion of catecholamines constitutes the main issue in pheochromocytoma. Patients often present with paroxysmal episodes characterized by a combination of headache, excessive sweating, tachyarrhythmias, and tremors. These symptoms coincide with the release of catecholamines into the bloodstream. The diagnosis is based on determining the levels of these substances, although their fluctuation in the bloodstream can be high. Hypofunction of the adrenal cortex leads to cortisol insufficiency, known as Addison’s disease. Occasionally, a similar disorder can be found when chronically suppressing adrenal function through the exogenous administration of corticosteroids. Patients typically experience generalized weakness, headaches, and mood disturbances such as depression or dysthymia. Characteristically, there is hyperpigmentation of the skin with diffuse darkening in certain regions such as elbows or hand creases, as well as in normally pigmented areas like the areolas of the breasts.
References
- Lewis PR, Timothy AP (2009) Merritt's Neurology. 12th (edn.), Lippincott Williams and Wilkins.
- Robert BD, Joseph J, John CM, Scott LP (2015) Bradley's Neurology in Clinical Practice. 7th (edn.), Elsevier.
- Makoto Ishii (2014) Neurologic Complications of Nondiabetic Endocrine Disorders. Continuum Neurology: neurology of Systemic Disease 20(3): 560-579
- Michael JA, Andrew SJ (2014) Aminoff's Neurology and General Medicine. 5th (edn.), Academic Press.






























