Thyroid Hormone Profile in Patients with Acute Coronary Syndrome
Vijay Kumar Sah1, Satyam Prakash2* and Suresh Chandra Kohli3
1Assistant Professor, Department of Internal Medicine, Janaki Medical College, Janakpur, Nepal 2Assistant Professor, Department of Biochemistry, Janaki Medical College, Janakpur, Nepal 3Professor, Department of Internal Medicine, Manipal College of Medical sciences,Pokhara, Nepal
Submission: June 21, 2017; Published: July 31, 2017
*Corresponding author: Satyam Prakash, Assistant Professor, Department of Biochemistry, Janaki Medical College Teaching Hospital, Tribhuvan University, Janakpur- 45600, Dhanusha, Nepal, Tel:+977-9841603704/+977-9844405444; Email: sprakashy2424@gmail.com
How to cite this article: Vijay K S, Satyam P, kohli S C. Thyroid Hormone Profile in Patients with Acute Coronary Syndrome .J Endocrinol Thyroid Res. 2017; 2(4):555592. DOI: 10.19280/JETR.2017.02.555592.
Abstract
Background and objectives: Thyroid hormone has an important role in the cardio¬vascular homeostasis. Small variations of the thyroid hormone within the physiological range have been linked to adverse cardiovascular prognosis. Several studies have reported changes in thyroid status in “Euthyroid sick syndrome” patients admitted with acute coronary syndrome. Therefore, this study was conducted to analyze the thyroid hormone profile in patients with ACS and to compare it between STEMI and NSTEMI/UA groups.
Materials and methods: A total of 100 patients were enrolled n this study and were divided into two groups as STEMI and NSTEMI/UA group. Thyroid function tests (fT3, fT4, TSH) were done by ELISA method within 24 hours of admission. The data were analyzed by SPSS version 17 software.
Results: Euthyroid Sick Syndrome was observed in 60%, subclinical hypothyroidism in 28% and subclinical hyperthyroidism in 8% of patients with abnormal thyroid hormone profile. A higher prevalence of abnormal thyroid hormone profile was seen in elderly age group >60 years (56%) followed by age group 40-60 years (36%) and 20-40 years (8%). A statistically higher prevalence of abnormal thyroid hormone profile was seen in STEMI group (72%) as compared to NSTEMI/UA group (28%). However, the difference in prevalence of ESS was not statistically significant between STEMI and NSTEMI/UA group.
Conclusion: The overall prevalence of abnormal thyroid hormone profile was statistically significant in the STEMI group, the prevalence of ESS did not show any statistically significant difference in STEMI and NSTEMI/UA groups.
Keywords: Acute coronary syndrome; Euthyroid sick syndrome; Thyroid hormone profile; Non ST segment elevation; Unstable angina
Introduction
Acute coronary syndrome has considerable effect on thyroid gland homeostasis with consequences in terms of morbidity and mortality [1]. Alteration in the level of serum thyroid hormone level has been described in several non thyroidal systemic illnesses including acute heart diseases [2,3]. Several studies have reported “Euthyroid sick syndrome” in patients admitted with acute coronary syndrome [2,4,5] the normal feedback control of the thyroid homeostasis is changed [6-9].
“Euthyroid Sick Syndrome” is characterized by decreased serum T3 and /or free T3, increased serum reverse T3(rT3), plus normal serum TSH, T4, and free T4 [2]. Patients belonging to the STEMI group showed early elevations, in addition to higher mean reverse T3(rT3) and lower mean T3 and free T3 levels [2]. This syndrome has been reported to be found in severe chronic heart failure [10,11], in acute myocardial infarction [6,12] and as a rapidly emerging phenomenon during open-heart surgery [13]. Additionally hypothyroidism is emerging as a risk for coronary artery disease [7].
Evaluation of thyroid hormone plasma levels has been done in a number of studies in patients presenting with Acute Coronary Syndrome and findings compared between Unstable Angina/Non-ST elevation MI (UA/NSTEMI) and ST Elevation acute MI (STEMI) groups [2,14]. Some studies have reported association of greater hormonal changes with more severe cardiac events (STEMI and Death) and patients with complications [2,14,15]. Implications of “Euthyroid Sick Syndrome” in terms of morbidityand mortality in ACS have also been studied by few workers [14]. An association of Euthyroid sick syndrome in ACS with poorer prognosis has been suggested in few studies [2,10] and has special significance in patients of ACS because low T3 levels in these patients signify severe disease and can be used as a marker for early invasive management in these patients [5,7].
The clinicians consider abnormalities of thyroid function test as significant coronary risk factors such as blood pressure, diabetic state, and cholesterol level during coronary care unit hospitalization [4]. Very limited data are available on altered serum levels of thyroid hormone in various clinical situation in Nepal [16-18]. Therefore, this hospital based study was undertaken to study the thyroid hormone profile in patients of ACS and to compare it in between STEMI and NSTEMI/UA groups.
Material and Methods
This hospital based cross-sectional study was conducted in Department of Internal Medicine, Manipal College of Medical Sciences/ Manipal Teaching Hospital Pokhara, Nepal in 2015 AD. Hundred consecutive cases of acute coronary syndrome admitted to Manipal Teaching Hospital were enrolled in this study. Ethical clearance was obtained from Institutional ethical committee of MCOMS and also written informed consent taken from all patients. All cases of ACS giving consent irrespective of gender, age, sex, race and ethnic group and clinical severity were included. Those patients who failed to give consent , thyroid disorders on treatment, suffering from other diseases such as neoplasia, chronic renal failure, chronic obstructive lung diseases, cirrhosis of liver and active infective conditions and the Patients taking Amiodarone, Lithium, Steroids or those who received iodinated contrast agent within the previous 2 weeks were excluded from this study. The data was collected and analyzed by SPSS-16.0 version software.
History and detailed clinical examination performed as per the working Performa. Cases showing abnormal thyroid hormone profile were grouped into Euthyroid Sick Syndrome (Low fT3, Normal fT4 and TSH), Subclinical Hypothyroidism (High TSH plus normal fT3 and fT4) and Subclinical Hyperthyroidism ( Low TSH plus normal fT3 and fT4) [19]. The study was carried out on the thyroid hormone profile in patients with ACS admitted to Manipal Teaching Hospital, Pokhara. Out of 100 ACS patients, 54 patients belonged to STEMI and 46 patients to NSTEMI/UA group. In patients presenting with symptoms of myocardial ischemia, angina pectoris or equivalent ischemic discomfort, the following investigations were done in all cases.
- 12- lead ECG (Electrocardiogram)
- Cardiac markers (CPK MB, Troponin I)
- Thyroid Function test (f T3, fT4, TSH) by ELISA method within 24 hours of admission.
- Complete blood count
- Random blood glucose level (Fasting and Post prandial in selected cases)
- Blood urea, serum creatinine, electrolytes (Na+, K+ )
- Fasting lipid profile
- X-ray Chest
- Echocardiography (in selective cases)/li>
The normal values of these tests in reference to Biochemistry department in Manipal Teaching Hospital are as mentioned below:
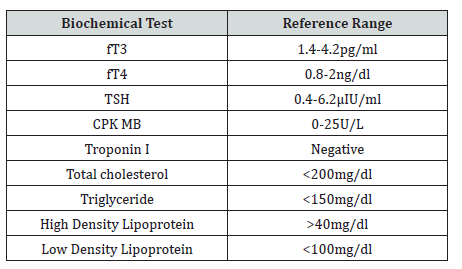
Depending on the ECG findings and result of cardiac markers, the patients of ACS were categorized into following two groups as per American Heart Association (AHA) criteria.
Group 1: Unstable angina/ non STEMI
Cases showing ST depression / T wave inversion with normal or elevated cardiac markers. At the time of presentation, patients with UA and NSTEMI can be indistinguishable and therefore are considered together in this guideline [20].
UA is defined as angina pectoris or equivalent ischemic discomfort with at least one of three features:
- It occurs at rest (or with minimal exertion), usually lasting >10 minutes.
- It is severe and of new onset (i.e., within the prior 4-6 weeks); and/or
- It occurs with a crescendo pattern (i.e., distinctly more severe, prolonged, or frequent than previously).
The diagnosis of NSTEMI is established if a patient with the clinical features of UA develops evidence of myocardial necrosis, as reflected in elevated cardiac biomarkers [21].
Group 2: ST elevation MI
Symptoms of myocardial ischemia in association with electrocardiographic (ECG) ST elevation and release of biomarkers of myocardial necrosis. New ST elevation at the J point in at least 2 contiguous leads of 2mm (0.2mV) in men or 1.5mm (0.15mV) in women in leads V2-V3 and/or of 1mm(0.1mV) in other contiguous chest leads or the limb leads [22]. The 12- lead ECG is a pivotal diagnostic tool. Level of serum cardiac biomarkers CK-MB and Troponin are elevated [23].
Results
Gender and age wise pattern in patients with acute coronary syndrome
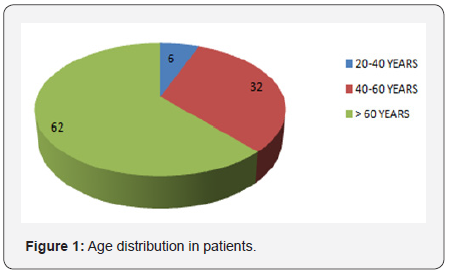
Altogether 100 ACS patients were enrolled in this study. Out of 100 patients, 58(58%) were males, 42(42%) were females, 62(62%) belonged to age group >60 years, 32(32%) belonged to age group 40-60 years and 6(6%) belonged to age group 20-40 years. The patients ranged between 35 years to 88 years of age. The mean age of the patients was 64.73±11.53 years. The results are shown in Figure 1.
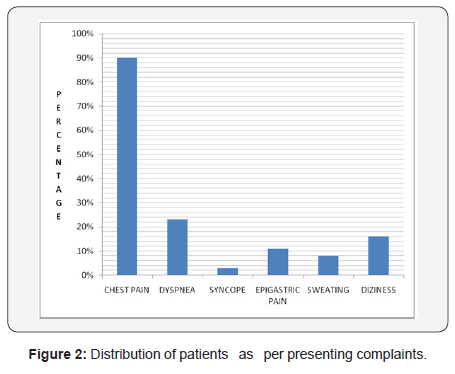
Distribution of patients according to symptoms in patients with ACS
Out of 100 ACS patients, 54 patients belonged to STEMI group and 46 patients to NSTEMI/UA group. Most of the patients presented with complain of chest pain. Similarly some of them also presented with complain like dyspnea, syncope, epigastric pain, sweating and dizziness. The results are shown in Figure 2. Of total, 46 patients were smokers and 26 patients used to take alcohol in their personal history.
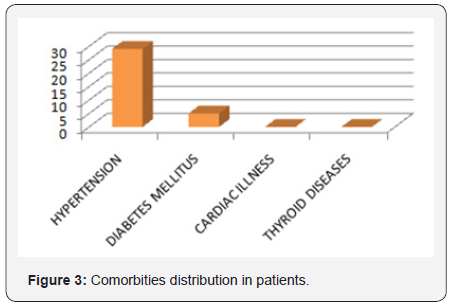
Comorbidities in ACS patients
Figure 3 shows 29 patients were known case of hypertension and 5 patients were known case of Diabetes. However no patients had any history of any cardiac or thyroid illness.
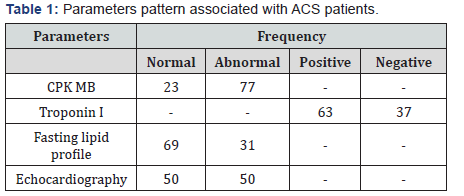
Different parameters associated with ACS patients
Table 1 showed that out of total, 23 patients had normal CPK MB whereas 77 patients had abnormal CPK-MB, 63 cases had positive Troponin I and 37 had negative Troponin I, 69 cases had normal fasting lipid profile while 31 had abnormal fasting lipid profile and 50 of the patients had normal findings on echocardiography while 50 had hypokinesia on echocardiographic findings.
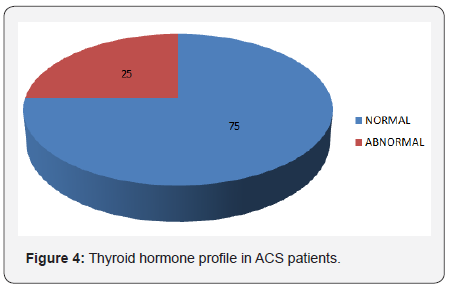
Thyroid hormone profile and ACS patients
Figure 4 shows out of 100 cases, 75(75%) had normal thyroid hormone profile and 25(25%) had abnormal thyroid hormone profile.
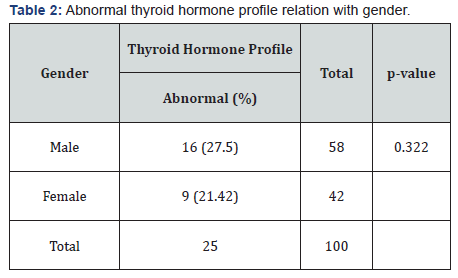
Abnormal thyroid hormone profile relation with gender and age groups
Out of 58 males, 16 (27.5%) had abnormal thyroid hormone profile and out of 42 females, 9 (21.42%) had abnormal thyroid hormone profile. There was no statistically significant difference in prevalence of abnormal thyroid hormone profile in males and females (p=0.322) as shown in Table 2. Out of 25 patients, 14(56%) were in age group above 60 years, 9(36%) were in age group 40-60 years and 2(8%) were in age group 20-40 years.
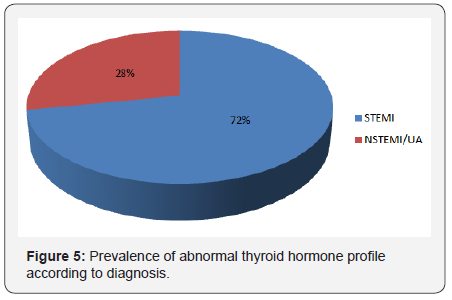
Abnormal thyroid hormone profile and ESS in STEMI and NSTEMI/UA group
Figure 5 shows a higher prevalence of abnormal thyroid hormone profile was seen in patients of STEMI group as compared to NSTEMI/UA group being 18 out of 25(72%) in STEMI group and 7 out of 25(28%) in NSTEMI/UA group. The difference is statistically significant (p=0.031). Out of total 15 patients with thyroid hormone profile of ESS, 10(66.67%) belonged to STEMI group while 5(33.33%) belonged to NSTEMI/UA group. The difference is not statistically significant (p = 0.217).
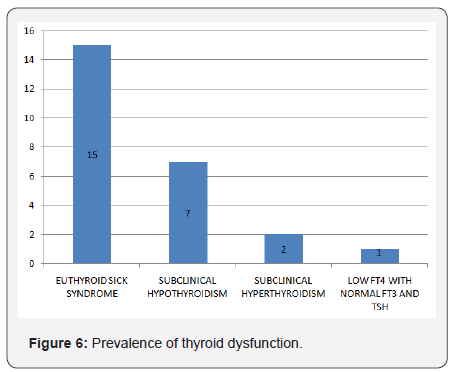
Types of thyroid dysfunction
Out of 25 patients with abnormal thyroid hormone profile, 15(60%) had Euthyroid Sick Syndrome, 7(28%) had subclinical hypothyroidism, 2(8%) had subclinical hyperthyroidism and 1(4%) had low fT4 with normal fT3 and normal TSH. The results are shown in Figure 6.
Discussion
The alteration in thyroid function is believed to be allied with the mechanism involved in maintaining energy in face of altered systemic homeostasis caused by the acute ischemic event [8] or directly related to inflammatory cytokines, acting as an inflammatory marker [9,10] or both. The effect of thyroid hormones heart failure [2,3] systemic arterial hypertension [4] atherosclerosis [5], dyslipidemia and cardiopulmonary surgeries has been documented in various studies [6-8].
This study depicts changes in thyroid hormone profile were observed in 25(25%) of the patients where 15(60%) had Euthyroid Sick Syndrome, 7(28%) had subclinical hypothyroidism, 2(8%) had subclinical hyperthyroidism and 1(4%) had low fT4 with nomal fT3 and normal TSH. In a study of 400 patients of ACS by Qari FA, thyroid dysfunction was reported in 23.3% of patients [4]. Khalil OA et al. [19] in their study of 196 patients of ACS, reported changes in thyroid hormone profile in 23% of their patients [22]. Mathur P et al. [24] in their study of 85 patients and Bayrak A et al. [5] in their study among 110 patients of ACS reported changes in thyroid hormone profile in 31.7% and 23.6% of patients respectively [5,24]. A prevalence of 25% reported in our study is almost in accord with the above studies. But in contrast to these studies, Adawiyah J et al. [25] reported a much higher prevalence of 53% of thyroid hormone dysfunction in their study among 85 patients [25]. The higher prevalence in their study is likely to be due to different inclusion criteria.
There was no statistically significant difference in prevalence of abnormal thyroid hormone profile in males and females group in this study being present in 27.5% in males and 21.42 % in females (p =0.322). Not many figures are available about difference in prevalence in males and females in other studies.
A higher prevalence of abnormal thyroid hormone profile was seen in patients of STEMI group as compared to NSTEMI/UA group being 18 out of 25 (72%) in STEMI group and 7 out of 25 (28%) in NSTEMI/UA group. The difference is statistically significant (p=0.031). Euthyroid Sick Syndrome was observed in 15 out of 25 patients (60%) showing abnormal thyroid hormone profile in our study. Khalil OA et al. [19] in their study reported Euthyroid Sick Syndrome in 68.9% cases while Adawiyah J et al. [25] found 43.5% of cases in the study [4,25]. Our findings are likely in accordance with findings of Khalil OA et al. [19]. But, Lower prevalence of Euthyroid Sick Syndrome have been reported in studies of other authors as 21.8% by Mathur P et al. [24], 21.67% by Potdar S et al. [26], 18.6% by Pimentel RC et al. [2], 10.2% by Qari FA [4] and 1.8% by Bayrak A et al. [5].
Out of total 15 patients with thyroid hormone profile of ESS, 10 (66.67%) belonged to STEMI group while 5(33.33%) belonged to NSTEMI/UA group. The difference is not statistically significant (p=0.217). Tuzun D et al. [3] in their study of 94 patients did not find any significant difference in prevalence of ESS between STEMI and NSTEMI/UA groups [3]. Higher prevalence 12 out of 18(66.66%) were in NSTEMI/UA group and it was 6 out of 18 (33.34%) in STEMI group in the study conducted by Mathur P et al. [24].
In our study, 7 out of 25(28%) had subclinical hypothyroidism. In agreement to our study, Khalil OA noted 24.5% had subclinical hypothyroidism [19]. Lovely NS et al. [27] reported hypothyroidism in patients suffering from ischemic heart disease [27]. In our study, 2 out of 25(8%) had subclinical hyperthyroidism. In agreement to our study Khalil OA et al reported 6.6% had subclinical hyperthyroidism [19].
Conclusion
Abnormal thyroid status increases risk of coronary artery disease and cardio¬vascular mortality affecting ventricular func¬tion, serum cholesterol levels, and heart rate and rhythm. The study depicts changes in thyroid hormone profile were observed in 25% of patients of ACS in our study. Euthyroid Sick Syndrome was observed in 60%, subclinical hypothyroidism in 28% and subclinical hyperthyroidism in 8% of patients with abnormal thyroid hormone profile. No gender difference was noted in abnormal thyroid hormone profile in male and female group. A higher prevalence of abnormal thyroid hormone profile was seen in elderly age group >60 years (56%) followed by age group 40-60 years (36%) and 20-40 years (8%). A statistically higher prevalence of abnormal thyroid hormone profile was seen in STEMI group (72%) as compared to NSTEMI/UA group(28%) (p=0.031) However the difference in prevalence of ESS was not statistically significant between STEMI and NSTEMI/UA group (p=0.217).
Limitation
A small sample size is a limitation of this study. Study of thyroid hormone profile in ACS patients in different earlier studies does not match with regard to the inclusion criteria used and the results therefore are not strictly comparable. Further larger studies with uniform inclusion criteria are required to get comparable results.
Acknowledgement
Authors debt their heartily thanks to Manipal College of Medical sciences/ Manipal Teaching Hospital Pokhara, Nepal for creating the research environment and completion of this research successfully.
References
- Danzi S, Klein I (2014) Thyroid disease and the cardiovascular system. Endocrinol Metab Clin North Am 43(2): 517-528.
- Pimentel RC, Cardoso GP, Escosteguy CC, Abreu LM (2006) Thyroid hormone profile in acute coronary syndromes. Arq Bras Cardiol 87(6): 688-694.
- Tuzun D, Bayram NA, Cicek OF, Ersoy R, Bozkurt E, et al. (2010) Are the thyroid functions associated with widespread of acute coronary syndromes? Endocrine Abstracts 22: 133.
- Qari FA (2015) Thyroid hormone profile in patients with acute coronary syndrome. Iran Red Crescent Med J 17(7): e26919.
- Bayrak A, Bayr A, Karabulut KU (2011) Effects of Thyroid hormones on major cardiovascular risk in acute coronary syndromes. Crit Care 15.
- Franklin JA, Gammage MD, Ramsden DB, Sheppard MC (1984) Thyroid status in patients after myocardial infarction. Clinical Sci 67(6): 585- 890.
- Chopra IJ, Hershman JM, Pardridge WM, Nicoloff JT (1983) Thyroid function in nonthyroid illnesses. Ann Intern Med 98(6): 946-957.
- Docter R, Krenning EP, de Jong M, henneman G (1993) The sick euthyroid syndrome: changes in thyroid hormone serum parameters and hormone metabolism. Clin Endocrinal (Oxf) 39(5): 499-518.
- Sypniewski E (1993) Comparative pharmacology of the thyroid hormones. Ann Thrac Surg 56(1 suppl): S2-S6.
- Wassen FW, Schiel AE, Kuiper GG, Kaptein E, Bakker O, et al. (2002) Induction of thyroid hormone-degrading deiodinase in cardiac hypertrophy and failure. Endocrinology 143(7): 2812-2815.
- Hamilton MA, Stevenson LW, Luu M, Walden JA (1990) Altered thyroid hormone metabolism in advanced heart failure. J Am Coll Cardiol 16(1): 91-95.
- Eber B, Schumacher M, Langsteger W, Zweiker R, Fruhwald FM, et al. (1995) Changes in thyroid hormone parameters after acute myocardial infarction. Cardiology 86(2): 152-156.
- Clark RE (1993) Cardiopulmonary bypass and thyroid hormone metabolism. Ann Thorac Surg 56(1 Suppl): S35-S42.
- Pavlou HN, Kliridis PA, Panagiotopoulos AA, Goritsas CP, Vassilakos PJ (2002) Euthyroid Sick Syndrome in acute ischemic syndromes. Angiology 53(6): 699-707.
- 15. Friberg L, Drvota V, Bjelak AH, Eggertsen G, Ahnve S (2001) Association between increased levels of reverse triiodothyronine and mortality after acute myocardial infarction. Am J Med 111(9): 699-703.
- Das BKL, Baral N, Shyangwa PM, Toora BD, Lamsal M (2007) Altered serum levels of thyroxine, triiodotyronine and thyroid stimulating hormone in patients with depression. Kathmandu University Med J 5(3): 330-334.
- Mittal A, Sathian B, Kumar A, Chandrasekharan N, Dwedi S (2010) The clinical Implications of thyroid hormones and its association with lipid profile. Nepal Journal of Epidemiol 1(1): 11-16.
- Yadav SC, Saldhana A, Majumdar B (2012) Status of thyroid Profile in Type-2 Diabetes Mellitus. Journal of Nobel Medical Coll 1(2).
- Khalil OA, Abdelaziz A, Ghoniem ME, Elagrody AI, Elgendy SA, et al. (2015) Thyroid dysfunction in acute coronary syndrome and its relation to morbidity and mortality. International Journal of Science and Res 4(7): 1564-1570.
- Anderson JL, Adams CD, Antman EM, Bridges CR, Califf RM, et al. (2011) ACCF/AHA focused update incorporated into the 2007 ACC/ AHA guidelines for the management of patients with unstable angina/ non–ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 123(18): e426-e579.
- Canon CP, Braunwald E (2015) Unstable angina and Non ST segment elevation Myocardial Infarction. In: Longo DL, Kasper DL, Jameson JL, Fauci AS, Hauser SL, et al. (Eds.), Harrison’s Principle of Internal Medicine. (18th edn), Mc Graw Hill, New York, USA.
- O Gara PT, Kushner FG, Ascheim DD, Casey DE, Chung MK, et al. (2013) ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/ American Heart Association Task Force on Practice Guidelines. Circulation 127(4): e362-425.
- Antman EM, Loscalzo J (2012) ST-Segment Elevation Myocardial Infarction. In: Longo DL, Kasper DL, Jameson JL, Fauci AS, Hauser SL, et al. (Eds.), Harrison’s Principle of Internal Medicine. (18th edn), Mc Graw Hill, New York, USA, pp. 2021-2024.
- Mathur P, Sud R, Yadav M, Bhattacharya J, singla S, et al. (2010) To study the thyroid hormone profile in patients of acute coronary syndromes. Japi Org 58.
- Adawiyah J, Norasyikin AW, Mat NH, Shamsul AS, Azmi KN (2010) The non-thyroidal illness syndrome in acute coronary syndrome is associated with increased cardiac morbidity and mortality. Heart Asia 2(1): 11-14.
- Potdar S, Patel H, Mehta N (2013) Evaluation of thyroid dysfunction in acute coronary syndrome. NJIRM 4(5): 65-71.
- Lovely NS, Begum Rokeya, Akhter QS, Sultana MS, Akhtar S (2011) Study of thyroid hormone status in ischemic heart disease. J Bangladesh Soc Physio 6(1): 27-31.






























