Glucagonoma Misdiagnosis
Maurizio De Rocco Ponce* and Carlo Foresta
Department of Medicine, University Hospital of Padova, Italy
Submission: March 04, 2017; Published: April 06, 2017
*Corresponding author: Maurizio De Rocco Ponce, Department of Medicine, University Hospital of Padova, via Giustiniani 2- 35128 Padova, Italy, Email: maurizioderocco@msn.com
How to cite this article: Maurizio D R P, Carlo F. Glucagonoma Misdiagnosis. J Endocrinol Thyroid Res. 2017; 1(4): 555567. DOI:10.19080/JETR.2017.01.555567
Abstract
Context: Glucagonomas are very rare tumors of pancreatic alfa-cells secreting glucagon which is responsible for symptoms that often patient complain. The diagnosis of glucagonoma relies on the presence of characteristic clinical features and elevated serum glucagon but the definitive diagnosis requires histology of the mass. Necrolytic migratory erythema is the most specific sign of glucagonoma and the presenting symptom in up to 90% of patients.
Case description: We describe a case of glucagonoma presenting with a typical glucagonoma syndrome including necrolytic migratory erythema. Despite its typical presentation, it has been misdiasgnosed for a long time primarily because of its slow onset and also because of the presence of glutamic acid decarboxylase (GAD) antibodies that misled the clinician to a diagnosis of latent autoimmune diabetes of the adults (LADA) instead of recognizing diabetes as paraneoplastic symptom.
Conclusion: An adult-onset diabetes in subjects not suspicious for insulin resistance (i.e. lean subjects) should be undergo further investigation for other possible underling conditions in which diabetes represent a symptom and not a disease in its own. Although its low frequency, glucagonoma should be kept it in mind as a possible diagnosis in order to recognize its symptoms when come across.
Introduction
Glucagonomas are very rare tumors of pancreatic alfa-cells secreting glucagon which is responsible for symptoms that often patient complain. The incidence of glucagonomas is very low (about 1 in 20 million people per year). The diagnosis of glucagonoma relies on the presence of characteristic clinical features and elevated serum glucagon but the definitive diagnosis requires histology of the mass. Necrolytic migratory erythema is the most specific sign of glucagonoma and the presenting symptom in up to 90% of patients [1].
Presentation
A 63-years old white man was referred to the Division of Metabolic Diseases for diabetic failure. He was a normal-weight subject with a medical history of GAD-positive latent autoimmune diabetes of the adults (LADA) since 2011 treated with insulin detemir, carotid vasculopathy and a previous episode of deep venous thrombosis after a post traumatic tibial fracture in 2012 [2].
The patient complained about asthenia, weight loss of about 6kg in the last 3 months and the worsening of some skin lesions localized in the lower limbs, genital and perianal region. Such lesions had onset in milder form at least two years before associated with glycemic decompensation. He reported a recent entry in the emergency room for the same reason when he was discharged diagnosed with contact dermatitis and since then treated with corticosteroid ointments with little benefit [3,4].
On examination, the patient presented dehydrated with extensive erythematous-exudative skin lesions with exfoliation characters localized especially in the lower limbs, genital and perianal region with scrotal edema. Biohumoral exams showed hyperglycemia (220mg/dl), a mild normocytic normochromic anemia (Hb 11.1g/dl, MCV 85.6fl), leukopenia (2950 WBC/μl) with increased inflammatory markers (PCR 62mg/l), renal function and iones (Na, K, Ca, P and Mg) were in normal range (Figure 1).
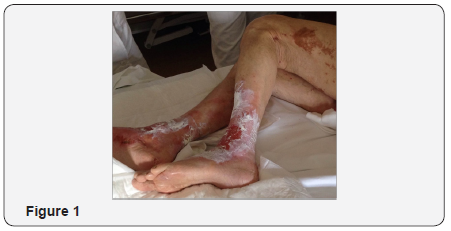
A dermatologic consultation deposed for a severe seborrhoeic dermatitis with Candida spp. Super infection, nevertheless a confirmation skin biopsy and further blood analysis were disposed. Meanwhile, an abdominal ultrasound tomography showed a solid mass with a diameter of 47mm in the tail of the pancreas and then a CT-scan confirmed the presence of a solid lesion of 58x37mm with irregular profile, a small calcification within it and discreet enhancement both in the arterial and in the venous phase; no signs of other lesions were found. Blood analysis showed a mild elevation of chromogranine A (141.7ug/l) and elevated glucagone (363ng/l) while zinc was normal (10,9umol/l). Finally skin biopsy histology was defined suggestive, even though not conclusive, for necrolytic migratory erythema. The patient underwent a distal splenopancreasectomy with intraoperative histology of the mass that stained positive for glucagon, chromogranine and neuron-specific enolasis staining. The final diagnosis was then IIb-pancreatic glucagonoma (pT2, pN1, pM0). After surgery the patient recovered from skin lesions and a PET-CT confirmed neither relapse of the mass nor the presence of metastatasis and the patient gained thereafter a good metabolic control with Metformin (Figure 2).
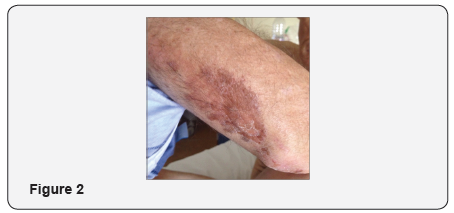
Discussion
Even if this case of glucagonoma presented with typical aspects of glucagonoma syndrome (diabetes onset, necrolytic migrant erythema, weight loss, anaemia and thrombotic complications), it was misdiagnosed for a long time. One reason is the slow onset of the whole cluster of signs and symptoms of the glucagonoma syndrome, which made them more difficult to link each other, but another reason is the presence of glutamic acid decarboxylase (GAD) antibodies.
As already demonstrated, GAD is expressed also in alfacells of pancreas islets and this explains how the neoplasia could induce GAD antibodies production. From this point of view the presence of GAD antibodies mislead the clinician to a wrong diagnosis of LADA instead of recognizing diabetes as paraneoplastic symptom.
References
- Wermers RA, Fatourechi V, Wynne AG, Kvols LK, Lloyd RV, et al. (1996) The glucagonoma syndrome. Clinical and pathologic features in 21 patients. Medicine (Baltimore) 75(2): 53-63.
- Kindmark H, Sundin A, Granberg D, Dunder K, Skogseid B, et al. (2007) Endocrine pancreatic tumors with glucagon hypersecretion: a retrospective study of 23 cases during 20 years. Med Oncol 24(3): 330-337.
- Echenique-Elizondo M, Tuneu Valls A, Elorza Orúe J, Martinez de Lizarduy I, Ibáñez Aguirre J (2004) Glucagonoma and pseudoglucagonoma syndrome. JOP 5(4): 179-185.
- Vives-Pi M, Somoza N, Vargas F, Armengol P, Sarri Y, et al. (1993) Expression of glutamic acid decarboxylase (GAD) in the alpha, beta and delta cells of normal and diabetic pancreas: implications for the pathogenesis of type I diabetes. Clin Exp Immunol 92(3): 391-396.






























