Hypertensive Pulmonary Edema, Variable Atrial Fibroflutter Block, Combined Brugada Syndrome, and Diverse Ischemia in COVID Pneumonia; Prognostication and Outcome
Yasser Mohammed Hassanain Elsayed*
Critical Care Unit, Kafr El-Bateekh Central Hospital, Egyptian Ministry of Health (MOH), Egypt
Submission: February 01, 2024; Published: March 22, 2024
*Corresponding author: Yasser Mohammed Hassanain Elsayed, Critical Care Unit, Kafr El-Bateekh Central Hospital, Egyptian Ministry of Health (MOH), Damietta, Egypt
How to cite this article: Yasser Mohammed Hassanain Elsayed*. Hypertensive Pulmonary Edema, Variable Atrial Fibroflutter Block, Combined Brugada Syndrome, and Diverse Ischemia in COVID Pneumonia; Prognostication and Outcome. Int J Pul & Res Sci. 2024; 7(2): 555706. DOI: 10.19080/IJOPRS.2024.07.555706
Abstract
Rationale: Hypertensive pulmonary edema is a deadly complication of hypertensive crises. It is one of the most serious presentations in the emergency department for hypertensive patients. Arrhythmias such as atrial fibrillations are commonly recognized sequels in COVID-19 patients. Brugada syndrome (BrS) is a genetic disorder with abnormal electrical activity within the heart that carries a higher risk for ventricular fibrillation and sudden death. There is a strong relevance between COVID-19 infection and ischemic heart disease.
Patient concerns: A 78-year-old, retired Officer, married Egyptian male patient was presented to the intensive care unit with hypertensive pulmonary edema, variable atrial fibro flutter block, Brugada syndrome, and suspected COVID-19 pneumonia.
Diagnosis: Hypertensive pulmonary edema, variable atrial fibro flutter block, combined Brugada syndrome, and diverse ischemia in COVID pneumonia.
Interventions: Chest CT, electrocardiography, and oxygenation.
Outcomes: Good outcomes with gradual response in the presence of numerous noteworthy serious risk factors were the results.
Lessons: The association of COVID pneumonia with hypertensive crises, pulmonary edema, bilateral pleural effusion, variable-block atrial fibro flutter, Brugada syndrome, and diverse ischemia in the elderly patient is highly interesting and remarkable. An elder age, combined Brugada syndrome, diverse ischemic heart disease, variable atrial fibro flutter block, pleural effusion, and COVID-19 pneumonia are constellation serious risk factors. Combined Brugada syndrome is newly described.
Keywords: COVID-19 pneumonia; Ischemic heart disease; Hypertensive crises; Brugada syndrome; Hypertensive pulmonary edema
Abbreviations: AF: Atrial Fibrillation; BrS: Brugada Syndrome; COVID-19: Coronavirus Disease 2019; ECG: Electrocardiogram; ICU: Intensive Care Unit; IHD: Ischemic Heart Disease; O2: Oxygen; PVCs Premature Ventricular Contractions; SCD: Sudden Cardiac Death; SGOT: Serum Glutamic-Oxaloacetic Transaminase; SGPT: Serum Glutamic-Pyruvic Transaminase; SHD: Structural Heart Disease; VR: Ventricular Rate
Introduction
Hypertensive crises with acute elevations in blood pressure that are associated with end-organ damage such as myocardial infarction, cerebrovascular accident, pulmonary edema, or renal failure are called is defined as a hypertensive emergency [1]. Hypertensive crises represent the most immediate danger to those afflicted and the most dramatic proof of the lifesaving potential of antihypertensive therapy [2]. Hypertensive crises are present when markedly elevated blood pressure or > 180/120mmHg are common issues in the emergency department [3-5]. Prompt diagnosis, based primarily on signs and symptoms is essential. Appropriately aggressive therapy will often result in a satisfactory outcome [4]. Arrhythmias are commonly recognized sequels in COVID-19 patients, with atrial fibrillation (AF) being the most common form. Electrical, calcium handling, and structural remodeling have represented keystones in understanding AF pathogenesis [6].
The underlying pathogenesis of AF in COVID-19 patients is still idiopathic [6]. According to current literature, AF was detected in 19% to 21% of COVID-19 patients [6]. Thrombosis is one of the most common cardiovascular complications among COVID-19 patients [7]. Multiple mechanisms have been suggested for cardiac damage in the COVID-19 epidemic. The systemic inflammatory response in severe COVID-19 is the producing high levels of cytokines causing cytokine-release syndrome (CRS) that can injure multiple tissues, involving vascular endothelium and cardiac myocytes [8]. Brugada syndrome (BrS) is a genetic disorder with abnormal electrical activity within the heart. The syndrome carries a higher risk for ventricular fibrillation (VF) and sudden cardiac death (SCD) in structural heart disease (SHD) [9]. BrS represent about 4-12% of all SCDs and ~20% of SCDs in patients with no SHD. The frequently implicated gene is SCN5A which encodes the cardiac sodium channel [9].
Case Presentation
A 78-year-old, retired Officer, married Egyptian male patient was presented to the intensive care unit (ICU) with tachypnea, palpitations, and angina chest pain. Generalized body aches, cough, fatigue, anorexia, and loss of smell were associated symptoms. The patient started to complain of fever 5 days ago. He has direct contact with a confirmed case of COVID-19 pneumonia 15 days ago. The patient denied a history of other relevant diseases, drugs, or other special habits. Informed consent was taken. Upon general physical examination, generally, the patient appeared centrally cyanosed, irritable, orthopnic, tachypneic, and distressed with a regular rapid pulse rate of VR; 110bpm, blood pressure (BP) of 200/120mmHg, respiratory rate of 23bpm, a temperature of 37°C, and pulse oximeter of oxygen (O2) saturation of 87%. Coarse generalized chest crepitations were heard on chest auscultations.
Currently, the patient was admitted to ICU for acute hypertensive pulmonary edema with angina, and variable atrial fibro flutter block. Initially, the patient was treated with O2 inhalation by O2 system line (100%, by nasal cannula, 8L/min) one sublingual isosorbide dinitrate tablet (5mg), 3 frusemide IV amp (40mg), sublingual captopril tablet (25mg), and continue nitroglycerine IVI (10mg/50 ml solvent, 5ug/min and titrated according to BP) were given. The patient was maintained treated with cefotaxime; (1000mg IV TID), azithromycin tablets (500mg, OD), oseltamivir capsules (75mg, BID only for 5 days), hydrocortisone sodium succinate (100mg IV BID), and paracetamol (500mg IV TID as needed). After controlling the BP, SC enoxaparin 80mg, BID), aspirin tablet (75mg, OD), clopidogrel tablets (75mg, OD), captopril tablets (25mg; BID), and diltiazem tablets (60mg, OD), warfarin tablet (5mg, OD), amiodarone tablets (200mg; BID), frusemide IV amp (40mg IV TDS), and atorvastatin tablets (20mg, OD) were added.
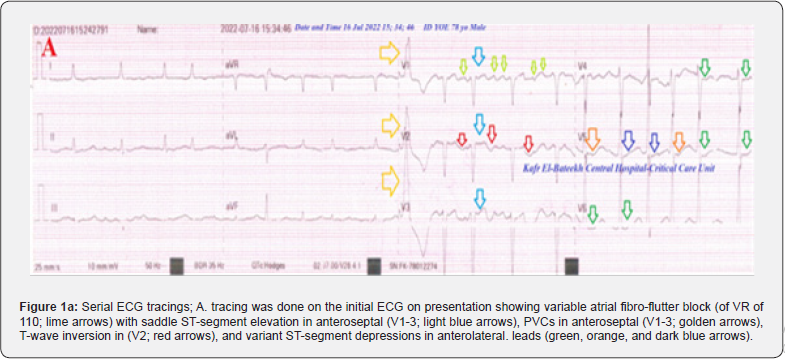
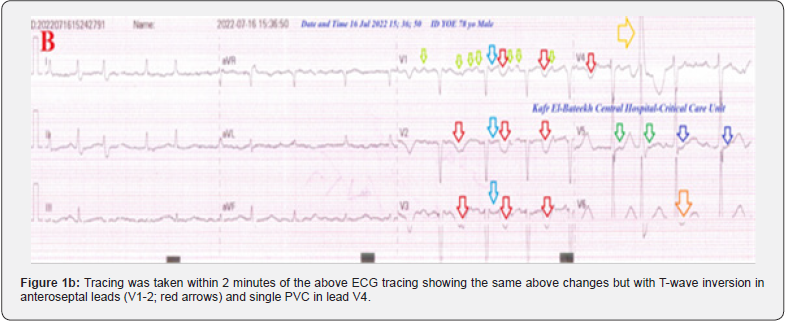
The patient was daily monitored for temperature, pulse, blood pressure, ECG, and O2 saturation. The initial ECG tracing was done on the initial ECG on presentation showing variable atrial fibro-flutter block (of VR of 110) with saddle ST-segment elevation in anteroseptal (V1-3), premature ventricular contractions (PVCs) in anteroseptal (V1-3), T-wave inversion in (V2), and diverse ST-segment depressions in anterolateral leads (Figure 1a). The second ECG tracing was taken within 2 minutes of the above ECG tracing showing the same above changes but with T-wave inversion in anteroseptal leads (V1-2) and single PVC in lead V4 leads (Figure 1b). The third ECG tracing was taken within 13 hours of treatment showing controlled variable atrial fibro flutter block (of VR of 78) with still saddle ST-segment elevation in anteroseptal (V1-3) and T-wave inversion in anterolateral (V2-4) leads. There is an improvement in the above variant ST-segment depressions and the disappearance of PVCs (Figure 1c).

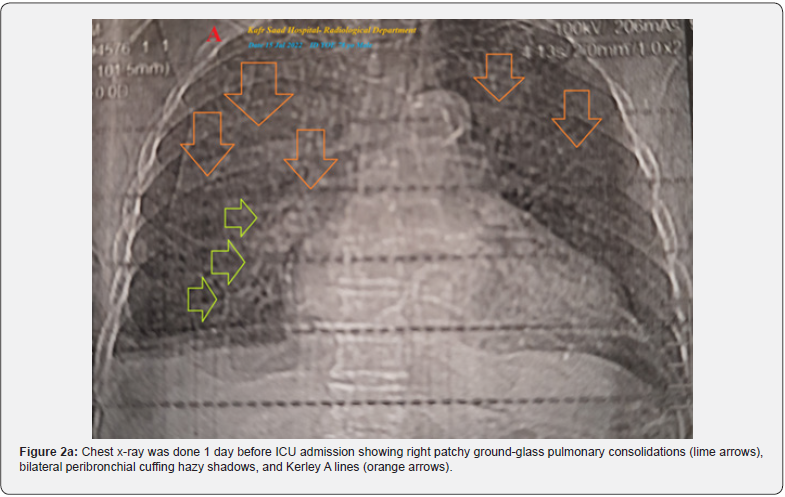
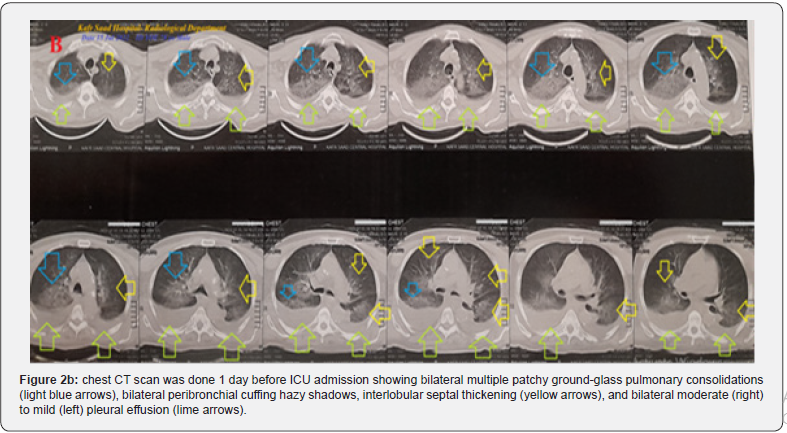
The plain chest-XR film was done 1 day before ICU admission showing right patchy ground-glass pulmonary consolidations, bilateral peribronchial cuffing hazy shadows, and Kerley A lines (Figure 2a). The chest CT was done 1 day before ICU admission showing bilateral multiple patchy ground-glass pulmonary consolidations, bilateral peribronchial cuffing hazy shadows, interlobular septal thickening, and bilateral moderate (right) to mild (left) pleural effusion (Figure 2b). The initial complete blood count (CBC); Hb was 13.2g/dl, RBCs; 4.05*103/mm3, WBCs; 12.7*103/mm3 (Neutrophils; 86.3 %, Lymphocytes: 9.2%, Monocytes; 3.5%, Eosinophils; 1% and Basophils 0%), and Platelets; 188*103/mm3. CRP was high (6g/dl). SGPT (69U/L) and SGOT were slightly high (49U/L). Serum albumen was normal (4.0gm/dl). Serum creatinine (1.2mg/dl) and blood urea were normal (39mg/dl). RBS was normal (171mg/dl).
Plasma sodium was high (148mmol/L). Serum potassium was normal (3.6mmol/L). Ionized calcium was slightly low (1.0mmol/L). The troponin test was negative. ABG showed partially compensated respiratory alkalosis. Hypertensive pulmonary edemas, variable atrial fibro flutter block, Brugada syndrome, and diverse ischemia in COVID pneumonia was the most probable diagnosis. Within 48 days of the above management, the patient finally showed nearly dramatic clinical and mostly electrocardiographic improvement. The patient was discharged after clinical stabilizations and continued on aspirin tablets (75mg, OD), clopidogrel tablets (75mg, OD), captopril tablets (25mg; BID), diltiazem tablets (60mg, OD), warfarin tablets (5mg, OD), amiodarone tablets (200mg; OD), frusemide tablets (40mg OD), oral nitroglycerine capsule (2.5mg, twice daily), and atorvastatin tablets (20mg, OD). Further recommended cardiac and chest follow-up was advised.
Discussion
Overview
a) A 78-year-old, retired Officer, married Egyptian male patient was presented to the intensive care unit (ICU) with hypertensive pulmonary edema, bilateral pleural effusion, variable atrial fibro flutter block, diverse ischemic heart disease (IHD), Brugada syndrome, and suspected COVID-19 pneumonia.
b) The primary objective for my case study was the presence of hypertensive pulmonary edema, bilateral pleural effusion, variable atrial fibro flutter block, diverse IHD, Brugada syndrome, and suspected COVID-19 pneumonia in ICU.
c) The secondary objective for my case study was the question of; how would you manage this case in the ICU?
d) Interestingly, the presence of the positive history of contact with a confirmed COVID-19 case, bilateral ground-glass consolidation, and some laboratory COVID-19 suspicion on top of clinical COVID-19 presentation with fever, dry cough, generalized body aches, anorexia, and loss of smell will strengthen the higher suspicion of COVID-19 diagnosis.
e) Saw-toothed appearance in V1 with fibrillation waves and variable numbers of p-waves in R-R interval supporting the diagnosis of variable atrial fibro flutter block.
f) It is commonly associated with atrial fibrillation, but the incidence and the prevalence of atrial flutter are less known when compared with atrial fibrillation. Atrial flutter is more frequent in patients with underlying diseases such as COPD, pulmonary hypertension, and acute pulmonary edema. Atrial flutter is more common in males than in females. The variable conduction in atrial flutter is mostly due to Wenckebach phenomenon. Elder age has an increased risk of atrial fibrillation and atrial flutter [10].
g) Variant IHD was described [11]. The presence of angina with down-sloping, horizontal or straight, and up-slopping ST-segment depression in anterolateral (V4-6) with T-wave inversion in anteroseptal (V1-3) leads suggesting the diagnosis of diverse IHD.
h) Three types of ECG patterns have been scientifically reported in patients with Brugada syndrome: coved ST elevations more than 2mm associated with an inverted T wave (type I), saddleback-shaped ST elevation more than 2mm (type II), and saddle-back shaped ST elevations less than 2mm (type III) [12]. So, the current type in this case report is mostly combined Brugada syndrome (type I and II).
i) Acute pulmonary embolism was the most probable differential diagnosis for the current case study.
j) I can’t compare the current case with similar conditions. There are no similar or known cases with the same management for near comparison.
k) The only limitation of the current study was the unavailability of echocardiography.
Conclusion and Recommendation
The association of COVID pneumonia with hypertensive crises, pulmonary edema, bilateral pleural effusion, variable atrial fibro flutter block, Brugada syndrome, and diverse ischemia in the elderly patient is highly interesting and remarkable. An elder age, combined Brugada syndrome, diverse ischemic heart disease, variable atrial fibro flutter block, pleural effusion, and COVID-19 pneumonia are constellation serious risk factors. Combined Brugada syndrome is newly described.
Acknowledgment
I wish to thank the team nurses of the critical care unit in Kafr El-Bateekh Central Hospital who make extra ECG copies for helping me. I want to thank my wife for saving time and improving the conditions for supporting me.
References
- Varon J, Marik PE (2003) Clinical review: The Management of Hypertensive Crises. Crit Care 7(5): 374-384.
- Kaplan NM (2006) Hypertensive Crises, Kaplan's Clinical Hypertension. (9th edn), Lippincott Williams & Wilkins (8): 609-639.
- Hebert CJ, Vidt DG (2008) Hypertensive crises. Prim Care 35(3): 475-487.
- McRae RP Jr, Liebson PR (1986) Hypertensive Crisis. Med Clin North Am 70(4): 749-767.
- Milan A, Puglisi E, Ferrari G, Fabbri A, Rabbia F, et al. (2010) Hypertensive Emergency and Urgency: Clinical Update. G Ital Cardiol (Rome) 11(11): 835-848.
- Gawałko M, Kapłon-Cieślicka A, Hohl M, Dobrev D, Linz D (2020) COVID-19 Associated Atrial Fibrillation: Incidence, Putative Mechanisms and Potential Clinical Implications. Int J Cardiol Heart Vasc 30: 100631.
- Kwenandar F, Japar KV, Damay V, Hariyanto TI, Tanaka M, et al. (2020) Coronavirus Disease 2019 and Cardiovascular System: A Narrative Review. Int J Cardiol Heart Vasc 29: 100557.
- Basu-Ray I, Almaddah Nk, Adeboye A, Michael PS (2020) Cardiac Manifestations of Coronavirus (COVID-19). StatPearls.
- Elsayed YMH (2019) An Electrocardiographic Triple Rhythm of Sinus Arrhythmia, Brugada Syndrome, And Early Repolarization with A Diverse Outcome. WW Med 1(9): 303-306.
- Rodriguez ZM, Goyal A, Maani CV (2022) Atrial Flutter. In: StatPearls [Internet].
- Elsayed YMH (2021) A COVID-19 Extensive Bilateral Pneumonia, Variants Ischemic Heart Disease, and Movable-Weaning Phenomenon of Hypocalcemia or Yasser’s Phenomenon; Dramatic Reversal at Home Management. J Clin Images Med Case Rep 2(2): 1035.\
- Sarquella-Brugada G, Campuzano O, Arbelo E, Brugada J, Brugada R (2016) Brugada Syndrome: Clinical and Genetic Findings. Genet Med 18(1): 3-12.






























