Arterial Blood Gas Sampling: The Relationship between Palpation Technique and Student Success using a Training Simulator
Salvatore A Sanders1,2*, Kelly L Colwell2 and Katie A Snyder2,3
1College of Graduate Studies, Youngstown State University, United States
2Department of Health Professions, Youngstown State University, United States
3Respiratory Care, University Hospitals Portage Medical Center, United States
Submission: August 03, 2023; Published: August 15, 2023
*Corresponding author: Salvatore A Sanders, PhD, RRT, CPFT, Youngstown State University, College of Graduate Studies, 1 University Plaza, Youngstown, OH, 44444, United States
How to cite this article: Sanders, SA, Colwell, KL Snyder, KA. Arterial Blood Gas Sampling: The Relationship between Palpation Technique and Student Success using a Training Simulator. Int J Pul & Res Sci. 2023; 6(4): 555695. DOI: 10.19080/IJOPRS.2023.06.555695
Abstract
Introduction: Arterial blood gas (ABG) sampling procedures are performed by health care professionals. The palpation technique used when performing an arterial puncture is often not described or is depicted as a technique using two fingers placed perpendicular to the artery. Use of a single finger aligned linearly (SAL) palpation technique might be simpler and more precise. This study was conducted to determine if the palpation technique utilized (SAL or MAP) can affect the number of punctures attempts necessary to obtain an arterial blood sample.
Materials and Methods: Fifty respiratory care student volunteers were randomly assigned to one of two groups. Participants were taught either the MAP technique or SAL technique. After instruction and practice each participant’s performance was evaluated utilizing a training simulator. Participants also completed a perception survey.
Results: Participants largely perceived that the training prepared them to obtain an arterial sample. Linear regression and binary linear regression analysis were conducted. The MAP technique significantly predicted the number of attempts required to obtain a sample. The effect of the MAP technique was significant, indicating that this technique decreased the odds of obtaining a sample on the first attempt by approximately 78.26% compared to the SAL technique.
Discussion and Conclusion: The results suggest that moving from the MAP to the SAL technique will improve the odds of obtaining a sample on the initial puncture attempt and decrease the number of attempts required for successful ABG sampling. Potential implications for patients, students and instructors are discussed.
Keywords: Arterial; Blood; Gas; Sampling; Technique
Abbreviations: ABG: Arterial Blood Gas; SAL: Single Finger Aligned Linearly; MAP: Multi-Finger Aligned Perpendicularly
Introduction
Health care professionals including physicians, nurses, paramedics and respiratory therapists may obtain arterial blood for analysis. Arterial blood gas (ABG) analysis is indicated to assess oxygenation, ventilation and to determine acid-base balance. Samples are commonly obtained from the radial artery. Other sample sites include the brachial and femoral arteries. This research [1] focuses on sampling from the radial artery. The technique to palpate the artery when performing an arterial puncture is often not described in procedures [2-5]. When it is described or illustrated it is often a technique in which two fingers [6,7]-or less often, a single finger [8] - are utilized to palpate the artery and the finger(s) are aligned perpendicular to the artery.
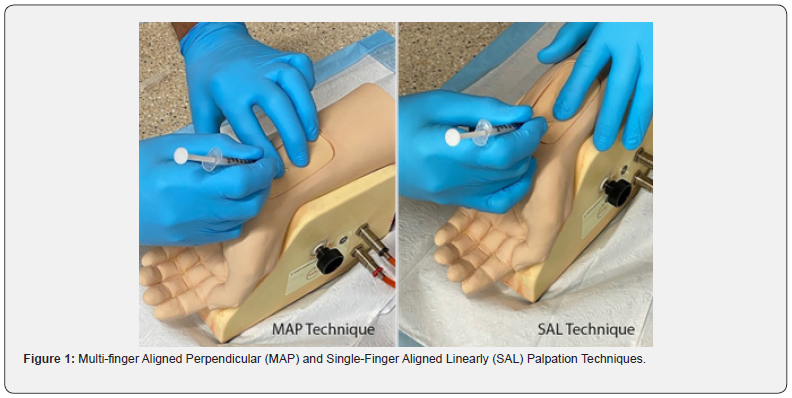
It makes intuitive sense that a single finger technique might be simpler to palpate and mentally visualize the artery and that if the finger is aligned linearly with the artery, that the center of the fingernail might provide a precise target. This single-finger, aligned linearly (SAL) palpation technique was compared to a palpation technique using multiple-fingers, aligned perpendicular to the artery (MAP), which is often taught to respiratory care students (Figure 1). One of the investigators had shown this single finger, aligned linearly (SAL) technique to people who were having difficulty consistently obtaining samples using more traditional palpation methods. Anecdotal observations showed that the technique improved consistency of obtaining a sample on the first attempt. The authors conducted this study to answer the research question: Can the technique used to palpate the artery affect the number of puncture attempts needed to obtain an arterial blood sample?
Materials and Methods
Adult students enrolled in a respiratory care program who were being trained to perform arterial blood gas sampling were invited to voluntarily participate in an arterial blood gas (ABG) palpation technique study which was approved by the Institutional Review Board of Youngstown State University in Youngstown, Ohio where this study was conducted. Participants read and signed a consent form prior to the start of the study. The consent form explained the study, confidentiality of individual participant’s results, and described the expectations of participants. Participants were randomly assigned to one of two groups, as evenly as possible. Participants in one group were taught the traditional, multi-finger aligned perpendicularly (MAP) palpation technique. The participants in the other group were instructed on the single finger aligned linearly (SAL) palpation technique. The students were separated into two groups based on the palpation technique to be taught.
Participants in each group viewed an instructional video demonstrating the technique assigned and then observed a live demonstration of the same palpation technique as part of the ABG sampling procedure. Demonstrations, training and evaluations were conducted using a Kagaku Kyoto arterial puncture training simulator, (mannequin arm with pulsating, red-colored fluid) and the Portex Pro Vent arterial blood gas sampling kit. The participants in each group were advised and agreed not to watch or practice any technique other than the technique they were trained in during the study. After participants in both groups had a practice period that averaged twelve days, each participant was evaluated by an instructor on his/her performance of the assigned technique (MAP or SAL) utilizing the ABG training simulator, ABG syringe and supplies.
The instructor recorded the number of punctures attempts each participant needed to obtain a sample from the simulator. The evaluation of the participants’ performance in the MAP technique group was done on a single day by the group instructor/supervisor. The evaluation of performance of participants in the SAL technique group was also completed in a single day by the instructor/supervisor of that group. When the study was concluded, a subject perception survey was completed by each participant. After the performance and perception results were obtained, participants were offered the opportunity to be trained and gain experience with the other palpation technique initially not shown to their group. Training in both palpation techniques was provided to participants after their performance was evaluated and data collection was completed.
Results
Fifty adult students volunteered to participate in this study. The participants were randomly assigned into one of two groups. One group was taught the traditional multi-finger aligned perpendicularly (MAP) palpation technique (n=24). The other group was instructed on the single finger aligned linearly (SAL) palpation technique (n=26). The participants in the MAP group were predominantly female (88%), all had some college education, two had earned an associate degree and one had earned a bachelor’s degree. They ranged in age from 20 to 46 years of age with a mean age of 23 years. Participants in the SAL group revealed similar characteristics. They were predominantly female (88%), all had some college education and two had earned an associate degree and two had earned a bachelor’s degree.
Most participants in both the MAP (n = 22, 92%) and SAL (n = 23, 88%) groups indicated that they did not have prior experience performing ABG punctures. The perceptions of participants in both groups were similar. The participants largely perceived the training (including the hands-on practice) prepared them to obtain an arterial sample from a patient (MAP: strongly agreed (n=17, 71%) agreed (n=6, 25%) or neural (n=1, 4%); SAL: strongly agreed (n=23, 88%) agreed (n=2, 8%) or neutral (n=1, 4%)). All participants in both MAP and SAL groups agreed or strongly agreed that the instruction provided was clear and easy to understand. The training for the participants in both groups was provided by experienced Registered Respiratory Therapists.
Students trained in the MAP technique strongly agreed (n=7, 35%) or agreed (n=13, 65%) that they had self-efficacy for successful ABG sampling (were confident that they could obtain a sample from most patients on their first puncture attempt). Similarly, those trained to use the SAL technique strongly agreed (n=9, 39%) or agreed (n=14, 61%) that they had self-efficacy for successful ABG sampling. Data analysis was conducted and reports and results for this study were drafted in part using Intellectus Statistics Online computer software [9]. Summary statistics were calculated for attempts needed to obtain a sample split by technique. Attempts required by those trained in the MAP technique were greater than those trained in the SAL technique. For those trained in the MAP technique, the observations of Attempts averaged 1.62 (SD = 1.13, SEM = 0.23, Min = 1.00, Max = 6.00, Skewness = 2.60, Kurtosis = 7.28). For participants trained in the SAL technique, the observations of Attempts averaged 1.12 (SD = 0.33, SEM = 0.06, Min = 1.00, Max = 2.00, Skewness = 2.41, Kurtosis = 3.80). The summary statistics can be found in (Table 1).
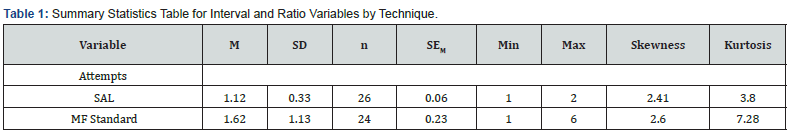
Note: ‘-’ indicates the statistic is undefined due to constant data or an insufficient sample size.
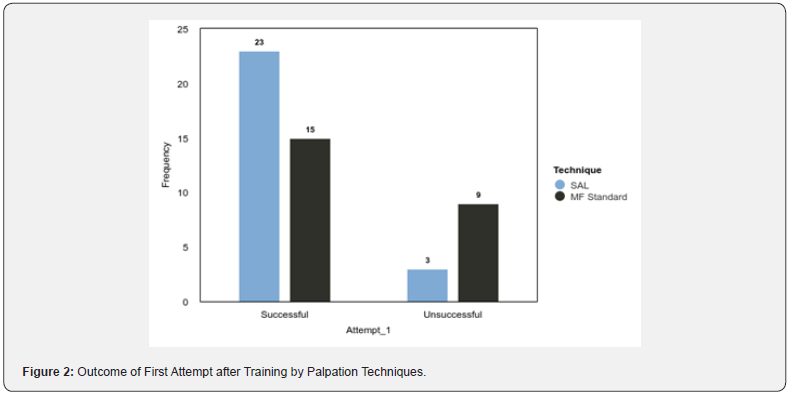
Linear regression and binary linear regression analysis were conducted (alpha = 0.05). The results of the linear regression model were significant, F (1,48) = 4.82, P = .033, R2 = 0.09. The MAP technique significantly predicted attempts, B = 0.51, t (48) = 2.20, P = .033. Moving from the SAL to the MAP technique will increase the mean number of attempts needed to obtain a sample by an average of 0.51 (Table 2). The binary logistic regression model was also significant, χ2 (1) = 4.76, P = .029. The effect of the MAP technique was significant, B = -1.53, OR = 0.22, P = .040, indicating that the MAP technique decreases the odds of obtaining a sample on the first attempt by approximately 78.26% relative to the SAL technique (Table 3). A bar plot of participants’ performance on their first evaluated attempt after training and practice is illustrated in (Figure 2).
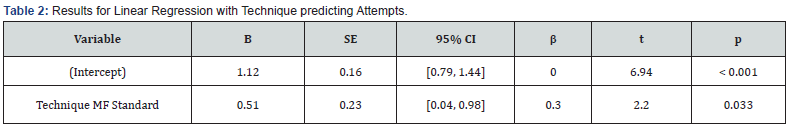
Note: Results: F (1,48) = 4.82, p = .033, R2 = 0.09
Unstandardized Regression Equation: Attempts = 1.12 + 0.51*Technique MF Standard
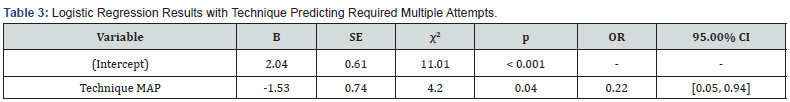
Note: χ2(1) = 4.76, p = .029, McFadden R2 = 0.09
Discussion
The results of this study suggest that the palpation technique used can affect the number of puncture attempts needed to obtain an arterial blood sample for blood gas analysis. The palpation technique employed explained about 9% of the variance in the number of attempts needed to obtain a sample utilizing a radial artery mannequin/simulator. The results were significant. The model predicts that moving from the MAP technique-often taught to respiratory care students-to the SAL technique will decrease the number of attempts needed to obtain a sample. Although that decrease is small (0.51 attempts on average) patients would benefit from a palpation technique that minimizes the number of punctures necessary to obtain a sample. The results also indicate that moving from the MAP technique to the SAL technique will increase the odds of obtaining a sample on the first puncture attempt by seventy-eight percent.
Similarly, patients would likely benefit from improved odds that the person sampling their arterial blood would be successful on their first attempt. This research was conducted with a limited number of students from a single respiratory care program. Further testing in a laboratory setting with students from other health care professions and from other educational institutions would allow the findings to be generalized. This study was conducted in a controlled lab setting utilizing a simulator. The authors have received approval to conduct a similar study in a clinical setting within a multi-hospital healthcare system to determine if use of the SAL palpation technique will minimize the number of attempts needed to obtain arterial blood samples from patients.
Conclusion
Early success in learning can lead to remarkable and important things in the future for students [10]. Early success in performing procedures is paramount in establishing students’ confidence for obtaining ABG samples and if changing how students are instructed to palpate the artery can lead to increased odds of success on the first attempt and decrease the number of attempts required to obtain a sample, and negate more expensive equipment options such as ultrasound or doppler methods, then perhaps these are reasons enough to explore different techniques including the SAL technique.
References
- Sanders SA, Colwell KL, Snyder KA (2022) Arterial Blood Gas Sampling: Does Palpation Technique Make a Difference? Respir Care 67(Suppl 10): 3756457.
- (1992) AARC clinical practice guideline. Sampling for arterial blood gas analysis. American Association for Respiratory Care. Respir Care 37(8): 913-917.
- Davis MD, Walsh BK, Sittig SE, Restrepo RD (2013) AARC clinical practice guideline: blood gas analysis and hemoximetry: 2013. Respir Care 58(10): 1694-1703.
- Hill S, Moore S (2018) Arterial blood gas sampling: using a safety and pre-heparinised syringe. Br J Nurs 27(14): S20-S26.
- Jensen PR, Markewitz BA (2018) Improved Success Rate of Arterial Puncture for Blood Gas Analysis Through Standardization. Lab Med 49(2): 175-178.
- Danckers M, Fried ED (2022) Arterial Blood Gas Sampling. Medscape.
- Dev SP, Hillmer MD, Ferri M (2011) Arterial puncture for blood gas analysis. New Engl J Med 364(5): e7.
- (2010) WHO Guidelines on Drawing Blood: Best Practices in Phlebotomy. World Health Organization.
- Intellectus Statistics Online computer software 2021. Intellectus Statistics.
- Finley G (2002) Early Success, Encouragement Add Up to Math Ph.D.’s. Black Issues High Educ 19(14): 8.






























