Impact of a Non-Invasive Respiratory Support Strategy and Switches in Therapy During Acute Respiratory Failure Due to SARS-COV-2
J Marin-Corral1,2*, FJ Parrilla-Gomez1*, A Castellvi-Font1, P Perez-Teran1, L Picazo1, S Pascual-Guardia3,4, A Rodriguez5, JC Ballesteros6, S Sancho7, L Socias8, E Diaz9,10, A Albaya-Moreno11, C de Haro4,9,10, O Roca4,9,10, MI Restrepo2,12**, JR Masclans1,13** and SEMICYUC COVID19 Group
1Critical Care Department, Hospital del Mar, Critical illness research group (GREPAC), Institut Hospital del Mar d’Investigacions Mediques (IMIM), spain
2Division of pulmonary diseases & Critical Care Medicine, South Texas Veterans Health Care System and University of Texas Health San Antonio, USA
3Respiratory Medicine Department-Muscle Wasting and Cachexia in Chronic Respiratory Diseases and Lung Cancer Research Group, Hospital del Mar, Spain
4Centro de Investigacion en Red de Enfermedades Respiratorias (CIBERES), Instituto de Salud Carlos III (ISCIII), Spain
5Critical Care Department, Hospital Universitari Joan XXIII, Spain
6Critical Care Department, Hospital de Salamanca, Spain
7Critical Care Department, Hospital La Fe, Spain
8Critical Care Department, Hospital Son Llatzer, Spain
9Servei de Medicina Intensiva, Parc Tauli Hospital Universitari, Spain
10Departament de Medicina, Universitat Autònoma de Barcelona, Spain
11Critical Care Department, Hospital de Guadalajara, Spain
12Division of Pulmonary & Critical Care Medicine, University of Texas Health San Antonio, USA
13Medicine and life science department (MELIS), Universitat Pompeu Fabra, Spain* and ** contributed equally to the work
Submission: August 01, 2023; Published: August 11, 2023
*Corresponding author: Francisco Jose Parrilla Gomez, MD, Critical Care Department, Hospital del Mar, Passeig Maritim 25-29, E-08003 Barcelona, Spain
How to cite this article: Francisco Jose Parrilla G, Joan Ramon Masclans E. Impact of a Non-Invasive Respiratory Support Strategy and Switches in Therapy During Acute Respiratory Failure Due to SARS-COV-2. Int J Pul & Res Sci. 2023; 6(4): 555694. DOI: 10.19080/IJOPRS.2023.06.555694
Online Supplement
Results
Descriptive data related to population
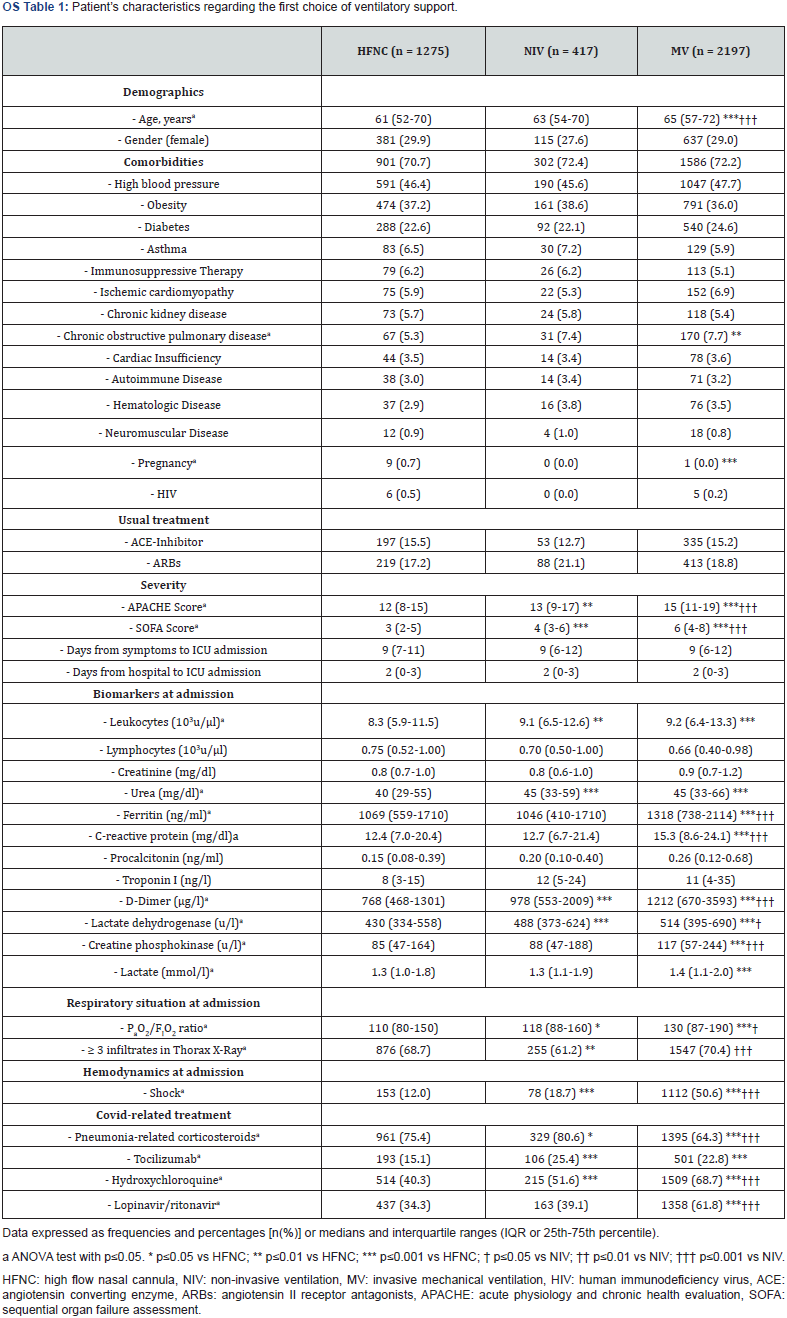
As shown in online supplement (OS) Table 1, in comparison with NIRS patients, patients who underwent MV on admission to the ICU were older and more severely ill, had higher levels of SARS-CoV-2-related analytical parameters, presented more shock on admission, had higher PaO2/FIO2 ratios, and more frequently received Covid-related treatments. NIV group patients had greater illness severity, with higher levels of SARS-CoV-2-related laboratory parameters and more shock on admission than the HFNC group. In contrast, they also presented higher PaO2/FIO2 ratios, a lower percentage of patients with ≥ 3 quadrants infiltrated on chest radiography at the same time, and more frequently received Covid-related treatments.
Descriptive data related to NIRS failure
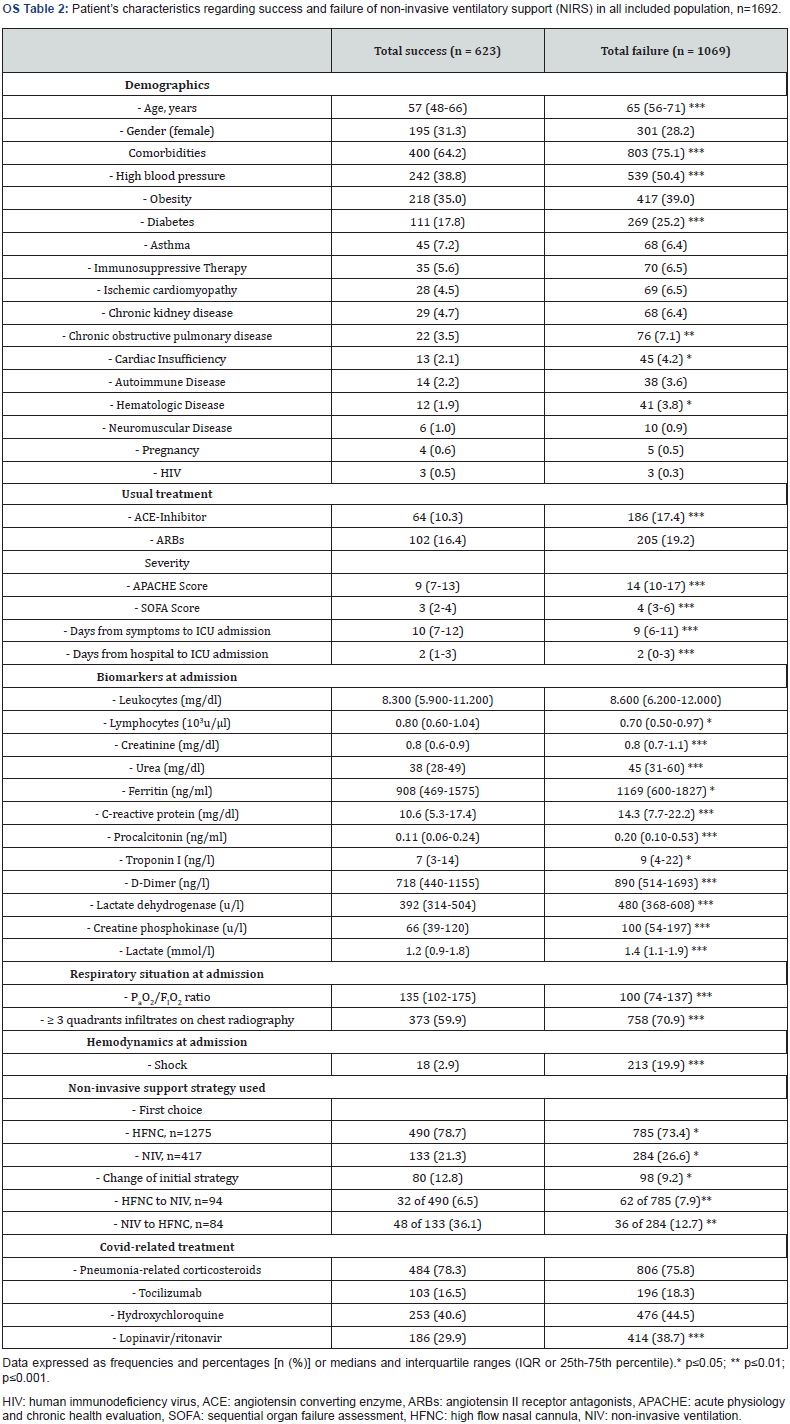
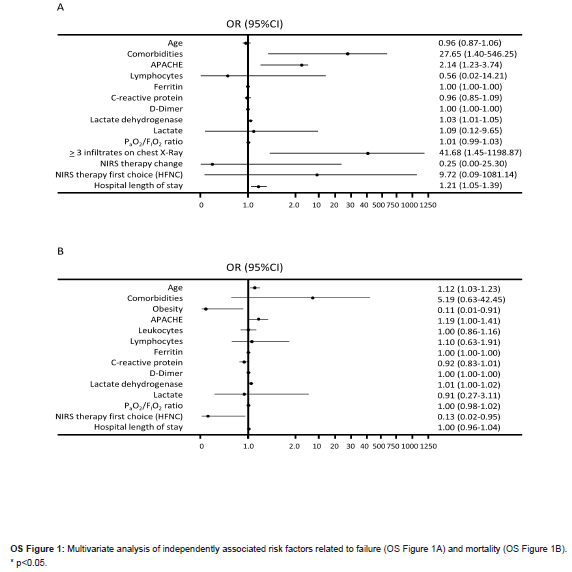
Patients who failed NIRS were significantly older, with more comorbidities and more severe disease, and had received more Covid-related treatments than those who succeeded (OS Table 2). NIRS failure patients had higher levels of SARS-CoV-2-related biomarkers at admission as well as worse respiratory and hemodynamic parameters, with a shorter delay time from symptoms onset and from hospital admission to ICU admission (OS Table 2). Presence of any comorbidity, APACHE score, lactate dehydrogenase (LDH), and presence of ≥ 3 quadrants infiltrated on chest radiography at ICU admission and hospital LOS were identified as risk factors independently associated with NIRS failure (OS Figure 1A).
In both groups, HFNC and NIV, patients who failed or switched NIRS therapy had more severe disease, more frequently received Covid-related treatments, had higher levels of SARS-CoV-2 related biomarkers, and had poor respiratory and hemodynamic parameters at admission compared to those who succeeded (Table 1). Compared to patients who switched NIRS from HFNC to NIV, patients who initially failed HFNC had more severe disease, a worse hemodynamic situation at admission with a higher presence of quadrants infiltrated on chest radiography, a lower presence of ischemic cardiomyopathy, higher levels of creatine phosphokinase, and were less likely to be treated with corticosteroids (Table 1). In the NIV group, in comparison to those who switched (NIV-to-HFNC), patients who failed had more severe disease with higher levels of several SARS-CoV-2-related laboratory parameters and worse hemodynamic and respiratory parameters at admission (Table 1).
Descriptive data related to NIRS mortality
Non-survivors were more likely to be older, had more comorbidities and chronic treatments, higher severity at admission, higher levels of SARS-CoV-2-related laboratory parameters and worse respiratory and hemodynamic parameters than survivors (Table 2). Survivors and non-survivors in each NIRS group, HFNC and NIV, presented for the most part the same characteristics as detailed above for the overall population (Table 2). The percentage of patients in whom initial NIRS strategy was switched was higher in survivors than in non-survivors in the NIV group (22.7 vs 13.3, p=0.033), but there were no differences in the HFNC group (6.7 vs 10.1, p=0.063). While age and LDH at admission were identified as risk factors, obesity and HFNC as first NIRS used were identified as protective factors independently associated with mortality (OS Figure 1B).
Analysis excluding DNI order patients
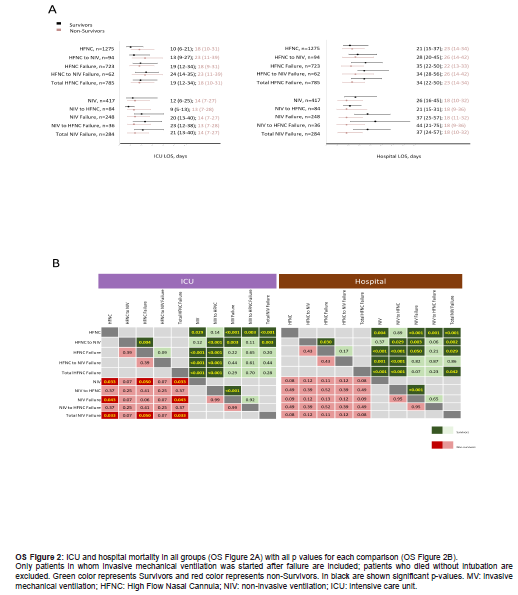
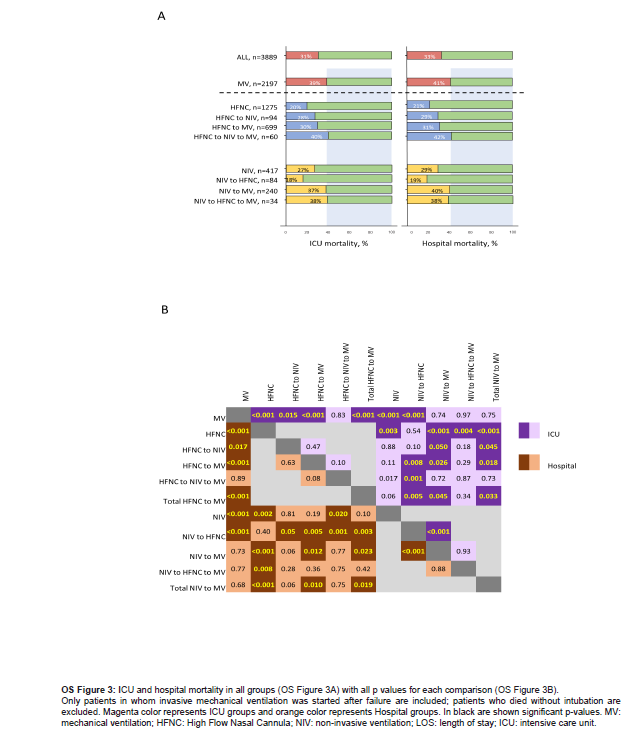
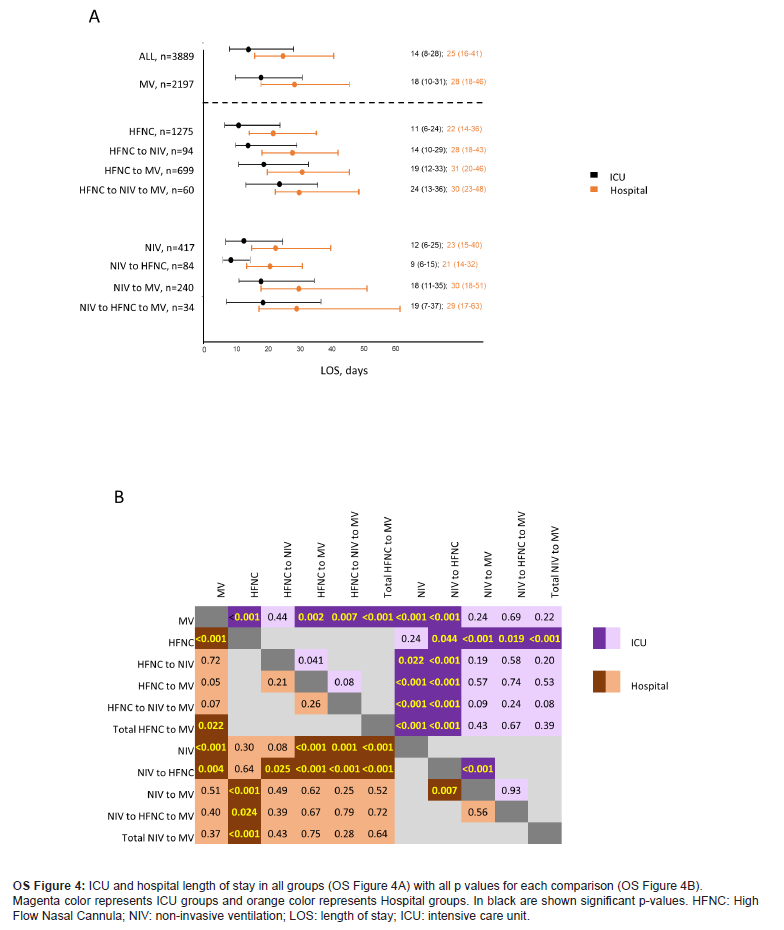
Figure 2 shows the percentage of patients who were mechanically ventilated or DNI order after NIRS failure or after NIRS switch failure. The proportion of patients switched from HFNC-to-NIV who failed and specifically needed MV was higher than those switched from NIV-to-HFNC (96.8% vs 94.4%, p=0.57). OS Figures 3 and 4 show ICU and hospital mortality rates and LOS only including patients who were mechanically ventilated after NIRS failure. The same differences in patterns between NIRS subgroups seen when all the population was included were also found in this sub analysis.
Overall ICU and hospital mortality and LOS were 31% and 33% (OS Figure 3) and 14 (8-28) and 25 (16-41) days (OS Figure 4) respectively. Patients undergoing MV at admission showed higher ICU mortality rates and LOS than those in whom NIRS was tried as first ventilation strategy [39% vs 22%, <0.001 and 18 (10-31) vs 12 (6-24); p<0.001] as well as compared with both NIRS groups separately: HFNC [20%, p<0.001; 11 (6-24), p<0.001) and NIV (27%, p<0.001; 12 (6-25), p<0.001] (OS Figures 3 and 4). While patients mechanically ventilated after HFNC failure showed lower ICU and hospital mortality rates than patients initially ventilated with MV (30% vs 39%, p<0.001 and 31% vs 41%, p<0.001), there were no differences in patients mechanically ventilated after NIV failure (37% 39%, p>0.05 and 40% vs 41%, p>0.05), or in mechanically ventilated patients after NIRS switch who failed. No differences were found in ICU and hospital mortality or LOS between any of subgroups requiring MV after NIRS failure and initially mechanically ventilated patients.