Bayesian Structural Equation Modeling to Identify Factors Influencing Tuberculosis Treatment Adherence
Mahalingam Vasantha1*, Chinnaiyan Ponnuraja1, Malaisamy Muniyandi2, Adhin Bhaskar1 Manoharan Tamizhselvan1, Mariappan Muthu Vijayalakshmi1, and Perumal Venkatesan1
1Department of Statistics, ICMR-National Institute for Research in Tuberculosis, India
2Department of Health Economics, ICMR-National Institute for Research in Tuberculosis, India
Submission: April 04, 2023; Published: April 22, 2023
*Corresponding author: Mahalingam Vasantha, Department of Statistics, ICMR-National Institute for Research in Tuberculosis, Indian Council of Medical Research, No.1, Mayor Sathyamoorthy Road, Chetpet, Chennai 600031, India, Email: drvasantha.m.icmr@gmail.com
How to cite this article: Vasantha M, Ponnuraja C, Muniyandi M, Adhin Bhaskar, Tamizhselvan M, Muthu Vijayalakshmi M, Venkatesan P.. Bayesian Structural Equation Modeling to Identify Factors Influencing Tuberculosis Treatment Adherence. Int J Pul & Res Sci. 2023; 6(4): 555691. DOI: 10.19080/IJOPRS.2023.06.555691
Abstract
Adherence to anti-Tuberculosis (TB) treatment is vital for curing TB patients and avoids drug resistance TB. Structural Equation Model (SEM) is a powerful tool for modeling latent variables and to control measurement errors. Bayesian SEM (BSEM) gives better estimates of the latent variable compared to conventional frequentist approaches to SEM. To our knowledge the use of BSEM to identify the significant latent constructs influencing the TB patients’ adherence to anti-TB treatment was not studied so far. A total of 725 pulmonary TB patients who were registered with Directly Observed Treatment Short course (DOTS) at Government health facilities in Tiruvallur district, south India under National Tuberculosis Elimination Programme were used for this analysis. In this study, a model of adherence to anti-TB treatment of TB patients using BSEM was explored which used to identify the relationship between adherence to anti-TB treatment and the latent variables “socio-economic”, “habits”, “problems” (problems in taking treatment) and “DOT” (treatment related variables). The latent variables “DOT” (0.199, p<0.005) and “problems” (-0.202 p<0.01) were significantly associated with adherence variable. The latent variable “DOT” had a positive effect while “problems” had a negative effect on adherence to anti-TB treatment. Hence reducing the patient’s specific problems might encourage treatment regularity under guided supervision.
Keywords: Tuberculosis; Adherence; Structural equation model; Bayesian SEM; Latent variable
Abbreviations: TB: Tuberculosis; SEM: Structural Equation Model; DOTS: Directly Observed Treatment Short course; MDR: Multi Drug Resistant; NTEP: National Tuberculosis Elimination Programme; RNTCP: Revised National Tuberculosis Control Programme; PPPV: Posterior Predictive P-value CI: Credible Interval
Introduction
Although tuberculosis (TB) is a preventable and curable disease, it is still one of the leading causes of morbidity and mortality in spite of recent progress of drug development and management of anti-TB treatment regimen [1]. Globally, there were estimated 10 million new TB cases and 5,58,000 Resistant to Rifampicin (RR-TB). Out of this, 1,60,684 cases were diagnosed as Multi Drug Resistant TB (MDR-TB) [2]. The low adherence of TB treatment could lead to poor treatment outcome and multi drug resistant (MDR) TB. Consequently, this emphasizes TB patients should not miss any dose of anti-TB treatment. TB patients’ adherence to anti-TB treatment is ensured through the significant component of DOTS (Directly Observed Treatment Short course) where every dose is given under direct observation [3]. Non-adherence to anti-TB treatment is the prime factor to drug resistant, relapse, treatment failure and death [4,5]. Numerous studies reported about the association of major components such as socio-economic character, lifestyle, treatment taking behaviour of the TB patients and health service centres etc. with patients’ adherence to anti-TB treatment [3,5-7].
Treatment adherence is a multi-dimensional concept influenced by different latent variables which can be divided in to five dimension such as socio-economic, health care system, health condition of patient, treatment therapy and patients related factors [8]. The use of latent variables is relevant and popular when risk factors of interest can’t be obtained with a single exact measurement. In most substantive research, it is important to establish an appropriate model to evaluate a series of simultaneous hypotheses about the impact of latent variables and manifest variables on the other variables and take the measurement errors into account. Structural equation modeling is a well-recognized technique in medical research for identifying complex relationship between latent variables and observed variables [9]. Latent variables are hypothesized to explain the co-variances in the observed indicators variables. In structural equation model (SEM), interest focuses on latent constructs, rather than on the observed indicator variables used to measure the constructs.
Meulemans et al. used SEM to identify the factors leading to non-compliance with DOT [10]. Nyamathi et al. assessed the predictors of latent TB infection treatment completion using SEM [11]. Bayesian SEM (BSEM) gives better estimates of the latent variable compared to conventional frequentist approaches to SEM [12]. The rationale and methodological details of BSEM are discussed in the literature [13-16]. BSEM with dichotomous variables was applied to study about non-adherence to medication of hypertensive patient [16]. To our knowledge the use of BSEM to identify the significant latent constructs influencing the TB patients’ adherence to anti-TB treatment was not studied so far. In the current study, we hypothesized to identify the factors influencing adherence of anti-TB treatment using BSEM with dichotomous variables.
Methodology
Study design
This is a modeling study of treatment adherence using BSEM approach for secondary data.
Source of data
This is a secondary data analysis of a total of 725 new smear positive pulmonary TB patients who were registered with DOTS programme in Tiruvallur district, south India under National Tuberculosis Elimination Programme (NTEP) formerly known as Revised National Tuberculosis Control Programme (RNTCP) were used for this analysis [3]. All these patients were treated under the direct observation of a DOT provider.
Tool used for data collection
ICMR-National Institute for Research in Tuberculosis, Chennai, India developed patient information form which is the semi-structured interview schedule. This tool includes information on socio economic demographic characteristics of patients, lifestyle characteristics, patient related problems, treatment related factors and whether the patients took treatment under supervision. This tool was used by trained field staff at patients’ residence and collected information. The written consent was obtained from TB patients aged more than 18 years. The study was approved by the Institutional Ethics Committee of the ICMR-NIRT. We used this data for the current study purpose.
Model specification
In this study, there were eleven independent variables which formed four independent latent variables. This includes eight dichotomous variables such as tobacco smoking, drinking alcohol, substance abuse, DOT interfering daily activities, problems in taking drugs, difficulty in accessing health facility, loosing wages and DOT provider living in the patients’ area. Further, the patients were given treatment at various DOT centres and these centres were grouped into a binary variable as government and non-government DOT centres. The variable “education” was classified into literate and illiterate as a binary variable and the variable “occupation” was classified into employed and unemployed as binary variable. The socio-economic variables such as education and occupation were intended to measure the latent variable “socio-economic”.
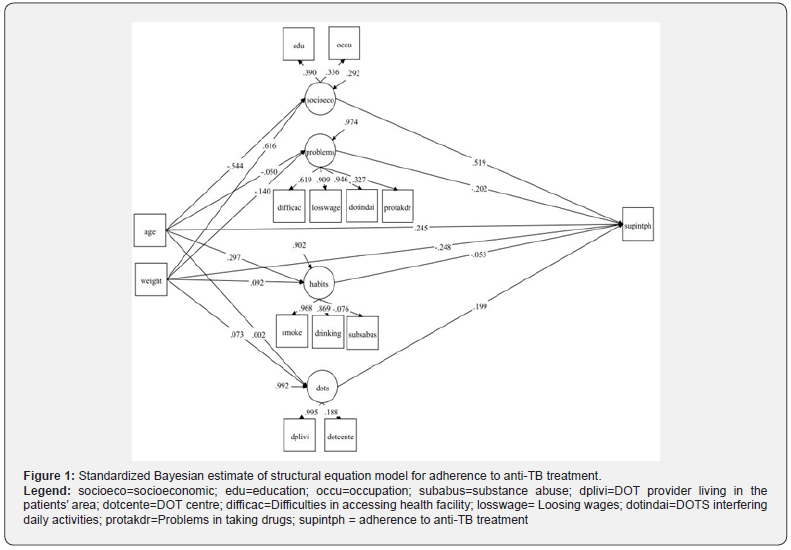
The variables smoking, drinking and substance abuse were selected as indicators for the latent variable “habits”. The four variables DOT interfering daily activities, problems in taking drugs, difficulty in accessing health facility and loosing wages formed the latent variable as “problems”. The two variables type of DOT center and DOT provider living in the patients’ area were chosen as indicators for the latent variable “DOT”. Body weights at the time of initiation of treatment and age in years were taken as covariates. (Figure 1) depicts path diagram and SEM with the outcome variable adherence predicted by the four latent variables socio-economic, habits, problems, and DOT. In this study, it was hypothesized that the latent variables socio-economic, habits, problems, and DOT which were influencing factors for adherence to TB treatment. The path diagram of the model is given in (Figure 1).
BSEM model
The BSEM models with dichotomous variables using Markov Chain Monte Carlo algorithms were constructed for analyzing the influencing latent variables for adherence to TB treatment using Mplus version 7.1. The non-informative prior which is default in Mplus was used for BSEM. For BSEM, the model convergence was assessed by the trace plots and estimated potential scale reduction (EPSR). Convergence of the sequence has been achieved where the ESPR values are less than 1.2. A Posterior predictive p-value (PPPV) is used to test the goodness of fit of the posited model.
Results
Profile
The base line characteristics of the TB patients are given in (Table 1). At the initiation of treatment, socio demographic profiles of the 725 patients were: 190 (26.2) were females; 401 (55.3%) were ≤42 years old; 289 (39.9%) were illiterates; 202 (27.9%) were unemployed; 343 (47.3%) were smokers and 270 (37.2%) were alcohol users.

BSEM Results
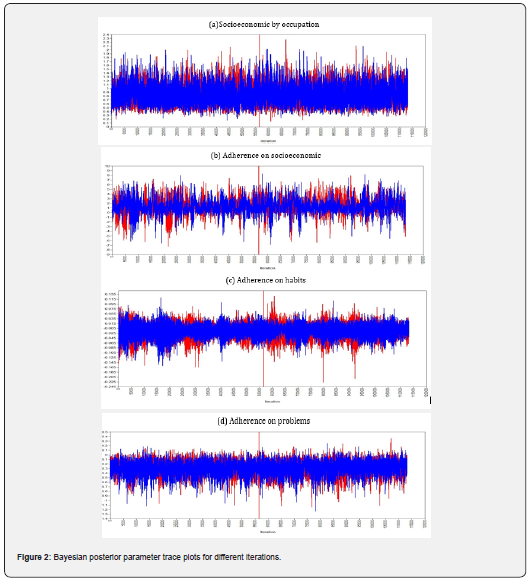
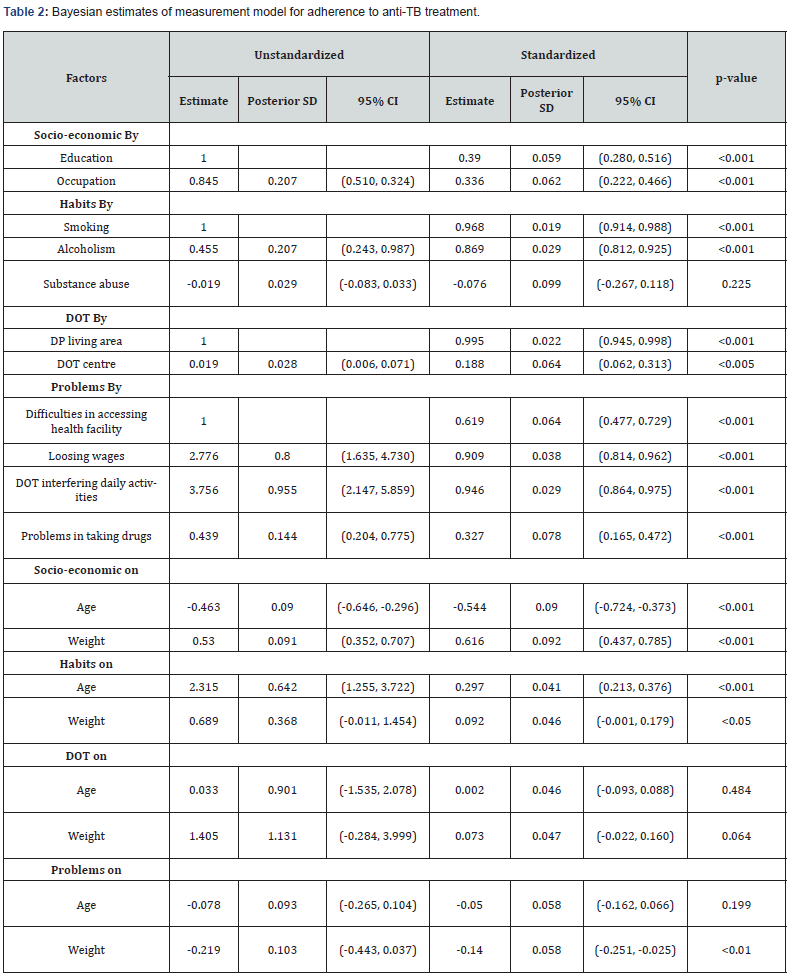
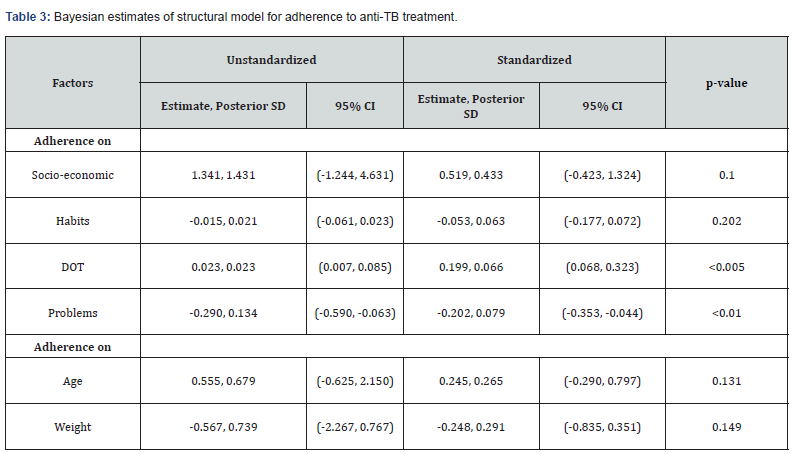
To obtain the Bayesian estimates, 57,000 observations were collected after discarding the first 57,000 burn-in iterations. The Bayesian estimates that were obtained by using 57,000 observations after convergence are reported in (Table 2 and 3). The posterior estimates of the parameters for measurement and structural models and their 95% posterior credible intervals (CI) are presented in (Table 2 and 3). PPPV for the model fit assessment was 0.058. The PPPV was reasonably close to the nominal 5% level. ESPR values are less than 1.2 after 55,950 iterations. Trace plots were also examined to verify convergence of the sampler. The trace plots are shown in (Figure 2) and it gives convergence plots which show a tight horizontal band for the parameter presented. The tight band indicates the parameters likely converged properly.
Bayesian Structural Model
The standardized estimate of structural equation for adherence of anti-TB treatment of the patients is
η = 0.519ξ1 - 0.0535 ξ2 + 0.199ξ3 - 0.202ξ (1)
The latent variables “DOT” and “problems” were significantly associated with adherence variable. The standardized estimate of the latent variable “DOT” on adherence is 0.199; 95% CI: (0.068 - 0.323); p<0.005 and the estimate of the latent variable “problem” on adherence is -0.202; 95% CI: (-0.353 - -0.044); p<0.01. The latent variable “DOT” had a positive effect while the latent variable “problems” had negative effect on adherence to anti-TB treatment. From the above structural equation, it was understood that TB patients with lesser problems were more likely to adhere to the anti-TB treatment. Hence reducing the patient’s specific problems might encourage treatment regularity under guided supervision (Table 3).
Bayesian Measurement Model
Among the factor loadings of variables, excluding substance abuse were significantly associated with their respective latent variables. The estimate of factor loading for education and occupation on the latent variable “socio-economic” (socio-economic status) were 0.390; 95% CI: (0.280-0.516); p<0.001 and 0.336; 95% CI: (0.222-0.466); p<0.001 respectively. It was found to be statistically significant in measuring the latent variable “socioeconomic”. The estimate of smoking and drinking on the latent variable “habits” were as 0.968; 95% CI: (0.914-0.988); p<0.001 and 0.869; 95% CI: (0.812-0.925); p<0.001 respectively. It was found to be significant with the latent variable habit. The factor loading of DOT provider living in the patients’ area and DOT center were statistically significant in measuring the latent variable DOT.
The estimate of DOT provider living in the patients’ area and DOT center on the latent variable “DOT” were 0.995; 95% CI: (0.945-0.998); p<0.001 and 0.188; 95% CI: (0.062-0.313); p<0.005. The estimate of difficulties in accessing health facility, loosing wages, DOT interfering daily activities, and problems in taking drugs on the latent variable “problems” were 0.619; 95% CI: (0.477-0.729); p<0.001, 0.909; 95% CI: (0.814-0.962); p<0.001, 0.946; 95% CI: (0.864-0.975); p<0.001 and 0.327; 95% CI: (0.165-0.472); p<0.001 respectively and found to be significantly influencing the latent variable problems (Table 2). The variables age and weight were significantly associated with the latent variables socio-economic and habits.
Discussion
The study is the first of its kind to apply latent variable modeling using Bayesian approach to explore for adherence of TB patients to anti-TB treatment. The finding of this study supports our theoretical model as conceptual framework for the prediction of medication adherence. The main finding of our study is that the latent variables “DOT” and “problems” were significantly influencing the adherence of anti-TB treatment. The structural and measurement equations obtained from this study were valuable statistical models to identify the latent variables influencing adherence of TB patients to anti-TB treatment. Though, the percent age of adherence was 66% in this study, TB patients with problems failed to adhere the anti-TB treatment. Hence reducing the patient’s specific problems might encourage treatment regularity under guided supervision.
Our findings corroborate with the previous studies done in India and parts of the world using SEM model for latent TB treatment reported that nurse case managed program, older age, less heroin and cocaine use, and TB knowledge were significantly associated with treatment adherence [11]. Another study for TB treatment reported that the latent constructs of stigmatization are associated with treatment adherence [10]. The current study results were corroborated with the findings from similar other studies using traditional statistical methods [17-20]. A study from China, 2009 found that Heavy financial burdens, lack of social support, adverse drug reactions and personal factors were related with non-adherence to anti-TB treatment [17]. According to an Indonesian study, the TB patients’ reasons for non-adherence to treatment were lack of money to pay for consultation fees and transportation charges, feeling better during treatment, and not gratified with the behavior of the health care staff [18].
Ershova et al. reported that the patients who did not complete treatment successfully and pervious history of defaulting from TB treatment were associated with poor treatment outcome [19]. Utilization of community health workers improved TB treatment adherence in both urban and rural areas whereas it was best in urban compared to rural area [20]. The two limitations of this study: First, the prior used for analyses was non-informative that is default in Mplus software which may impact our results. Secondly the percentage of missed drug was not able to assess from this data.
Conclusion
The Novel approach of the study was that from our knowledge we used first time BSEM to identify the latent constructs which influence the TB treatment adherence. BSEM is a powerful statistical computing tool for more accurate analysis of more complex data. The latent variable “DOT” had a positive effect while “problems” had a negative effect on adherence to anti-TB treatment. There is a need to take action on reducing the patient’s specific problems. This might encourage treatment regularity under direct supervision. This will provide strong scientific evidence to the policy makers to take appropriate action.
Acknowledgement
The authors acknowledge the ICMR-National Institute for Research in Tuberculosis, Chennai for permitting us to use the data for modeling.
References
- Maartens G, Wilkinson RJ (2007) Tuberculosis. Lancet. 370(9604): 2030-2043.
- (2018) Global Tuberculosis Report. World Health Organization (WHO).
- Gopi PG, Vasantha M, Muniyandi M, V Chandrasekaran, R Balasubramanian, et al. (2007) Risk factors for non-adherence to directly observed treatment (DOT) in a rural tuberculosis unit, south India. Indian J Tuberc 54(2): 66-70.
- Jakubowiak W, Bogorodskaya E, Borisov S, I Danilova, E Kourbatova (2009) Treatment interruptions and duration associated with default among new patients with tuberculosis in six regions of Russia. IJlD 13(3): 362-368.
- Munro SA, Lewin SA, Smith HJ, Mark E Engel, Atle Fretheim, et al. (2007) Patient adherence to tuberculosis treatment: A systematic review of qualitative research. PloS Med 4(7): e238.
- Bagchi S, Ambe G, Sathiakumar N (2010) Determinants of poor adherence to anti-tuberculosis treatment in Mumbai, India. Int J Prev Med 1(4): 223-232.
- Mkopi A, Range N, Lwilla F, Saidi E, Alexander S, et al. (2012) Adherence to Tuberculosis Therapy among Patients Receiving Home-Based Directly Observed Treatment: Evidence from the United Republic of Tanzania. PLoS One 7(12): e51828.
- Mathes T, Jaschinski T, Pieper D (2014) Adherence influencing factors-a systematic review of systematic reviews. Arch Public health 72(1): 37.
- Beran TN, Violato C (2010) Structural equation modeling in medical research: a primer. BMC Res Notes 3: 267.
- Meulemans H, Mortelmans D, Liefoogh R, P Mertens, SA Zaidi, et al. (2002) The limits to patient compliance with directly observed therapy for tuberculosis: a socio-medical study in Pakistan. Int J Health Plann Manage 17(3): 249-267.
- Nyamathi A, Stein JA, Schumann A, Tyler D (2007) Latent variable assessment of outcomes in a nurse managed intervention to increase latent tuberculosis treatment completion in homeless adults. Health Psychol 26(1): 68-76.
- Lee SY (2007) Structural equation modeling: A Bayesian Approach. John Wiley & Sons Ltd.
- Lee SY, Shi JQ (2000) Bayesian analysis of structural equation model with fixed covariates. Structural Equation Modeling 7(3): 411-430.
- Muthen LK, Muthen BO (2013) MPlus user’s guide. Seventh edition.
- Scheines R, Hoijtink H, Boomsma A (1999) Bayesian estimation and testing of structural equation models. Psychometrika 64: 37-52.
- Lee SY, Song XY (2003) Bayesian analysis of structural equation models with dichotomous variables. Stat Med 22(19): 3073-3088.
- Xu W, Lu W, Zhou Y, Zhu L, Shen H, et al. (2009) Adherence to anti-tuberculosis treatment among pulmonary tuberculosis patients: a qualitative and quantitative study. BMC Health Serv Res 9: 169.
- Widjanarko B, Gompelman M, Dijkers M, Vander WMJ (2009) Factors that influence treatment adherence of tuberculosis patients living in Java, Indonesia. Patient Prefer Adherence 3: 231-238.
- Ershova JV, Podewils LJ, Bronner LE, Stockwell HG, Dlamini S, et al. (2014) Evaluation of adherence to national treatment guidelines among tuberculosis patients in three provinces of South Africa. S Afr Med J 104(5): 362-368.
- Ongango JR, Mwachari C, Kipruto H, Karanja S (2014) The Effects on Tuberculosis Treatment Adherence from Utilising Community Health Workers: A Comparison of Selected Rural and Urban Settings in Kenya. PLoS One 9(2): e88937.






























