To Study the Usefulness of Cartridge Based Nuclear Acid Amplification Test [CBNAAT] in Bronchoalveolar Samples in the Diagnosis of Sputum Negative Patients with Presumptive Pulmonary Tuberculosis
Panda RK and Devi Jyoti Dash*
Department of Respiratory Diseases, Pt. J. N. M. Medical College, India
Submission: July 20, 2019; Published: September 09, 2019
*Corresponding author: Devi Jyoti Dash, Department of Respiratory Diseases, Pt. J. N. M. Medical College, Raipur, Chattisgarh, India
How to cite this article: Panda RK and Devi Jyoti Dash. To Study the Usefulness of Cartridge Based Nuclear Acid Amplification Test [CBNAAT] in Bronchoalveolar Samples in the Diagnosis of Sputum Negative Patients with Presumptive Pulmonary Tuberculosis. Int J Pul & Res Sci. 2019; 4(2): 555632. DOI: 10.19080/IJOPRS.2019.04.555632
Abstract
Background: About 40‑60% of patients with presumptive PTB may fail to produce sputum, or when it is available, AFB/CBNAAT may be negative on repeated smear examination. These patients can be diagnosed by flexible fibreoptic bronchoscopy.
Aims: This study was carried out to know the usefulness of bronchoscopy in sputum negative suspected pulmonary tuberculosis patients.
Materials and methods: We identified 68 consecutive cases of suspected pulmonary TB between Nov 2016 and July 2017, who had negative results on sputum smears examination by fluorescent microscopy/ZN staining on at least 2 samples or CBNAAT and did fibre optic bronchoscopy and sent bronchial aspirate for CBNAAT and AFB staining.
Results: Males constituted majority of our study population. The most common age group involved in the study was less than 30 years (35.2%). Cough was the most common symptom reported by 45 patients (66.1%). The past history of PTB was present 13 patients (19.1%). 27.9% of study population had consolidation on CXR. Out of 68 clinically suspected sputum negative-PTB patients, 32 patients (47%) were finally diagnosed as having microbiologically confirmed PTB.
Conclusion: CBNAAT done on bronchial aspirate can be an important adjunct to bacteriological confirmation of suspected cases who were otherwise sputum negative or not expectorating adequate sputum.
Keywords: Pulmonary tuberculosis, Tuberculosis control programme, Radiologically, Bronchoscopy, Pulmonary pathologies, Bronchoalveolar, Bronchial biopsies, Respiratory medicine
Introduction
Tuberculosis is a major health problem and the TB epidemic is larger than previously estimated. India accounts for one fourth of global TB burden i.e. 2.79 million out of 10.4 million new cases in 2017, and about 1.6 million died due to TB annually worldwide in 2017 [1].
Detecting patients with active Pulmonary Tuberculosis (PTB) disease is an important component of Tuberculosis (TB) control as early appropriate treatment renders these patients non-infectious and interrupts the chain of transmission of TB[2]. Under the programme conditions, such as those endorsed by the World Health Organization (WHO) and implemented successfully in high burden countries including Government of India’s Revised National Tuberculosis Control Programme (RNTCP), the diagnosis of PTB is based on sputum examination [3]. About 40‑60% of patients with active pulmonary tuberculosis suspected clinically or radiologically may fail to produce sputum, or when it is available AFB/CBNAAT may be negative on repeated smear examination [4]. Henceforth, more aggressive procedures need to be undertaken in these patients in order to establish the diagnosis.
Various methods have been employed to ascertain active TB disease in patients with suspected sputum negative PTB (Table 1). Flexible Fibre Optic Bronchoscopy (FOB) is a one of the important procedures utilized by physicians when the initial work-up of patients with suspected pulmonary pathologies remains inconclusive and to evaluate the tracheobronchial tree and also to obtain samples like bronchial aspirate, Bronchoalveolar Lavage (BAL) fluid, bronchial brushings, and bronchial biopsies [5]. FOB is considered as a safe diagnostic and interventional tool, even in young or extremely premature infants [6] and should be conducted on all patients without expectoration and negative sputum reports and that BAL performance should be a routine procedure as it is simple and usually uncomplicated technique [7].

Materials and Methods
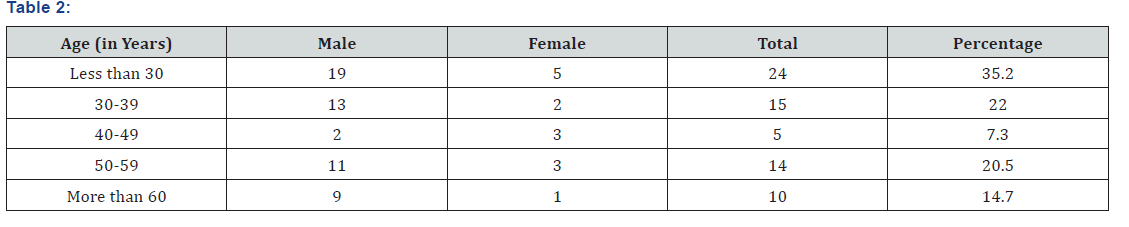
This prospective study was conducted in the department of respiratory medicine, Pt. J. N. M. Medical College, Raipur from November 2016 to July 2017. All consecutive patients with sputum negative presumptive pulmonary tuberculosis who attended the department of Respiratory medicine were selected for the study (Table 2). Informed consent was taken from the patients.
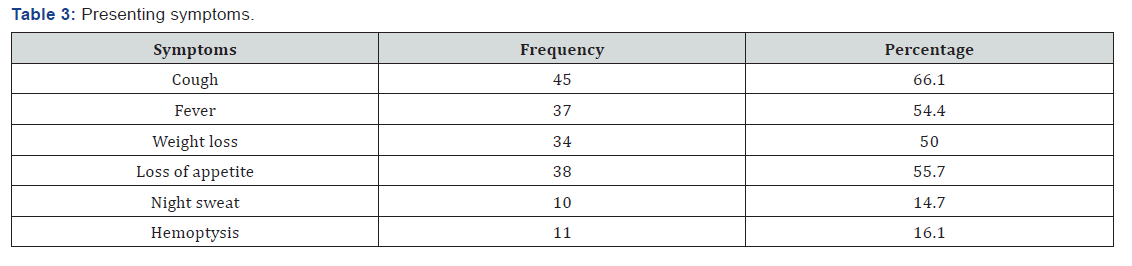
All patients with clinical history and physical findings or chest X‑ray lesions suggestive of pulmonary tuberculosis and with two consecutive sputum smear examinations negative for acid‑fast bacilli and CBNAAT were included in this study (Table 3). Patients with any contraindications for bronchoscopy procedure, those not giving consent and patients on anti‑tubercular treatment were excluded from the study.
After a detailed clinical history, thorough physical examination and routine investigations, assessment for the fitness of patients for bronchoscopy procedure was done. Written informed consent was obtained from all the patients undergoing bronchoscopy procedure. Fibreoptic bronchoscopy was performed using KARL STORZ bronchoscope introduced through trans nasal/oral route after proper lubrication with xylocaine ointment. All procedures were carried out as per the International recommendations [7,8]. A thorough examination of the bronchial tree was carried out and Bronchial Aspirate (BA) was collected. All these specimens were sent to the department of microbiology, with a code number where these samples were processed, stained and cultured.
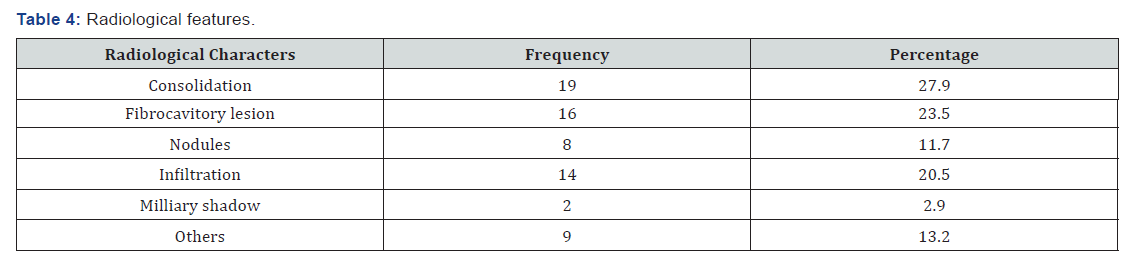
The data was analysed, and the results were given in percentage in accordance with previous related studies (Table 4). Different statistical aggregates like mean and median were used to analyse numerical parameters. Tabular representation of the results was done, and appropriate statistical methods were employed to ascertain the yield of the various specimens obtained after bronchoscopy.
Results
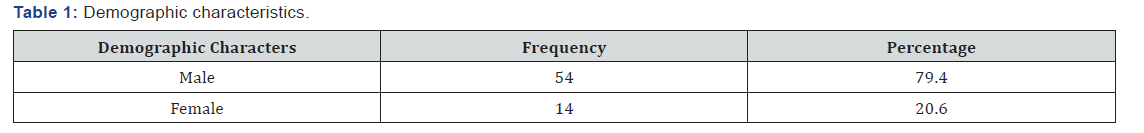
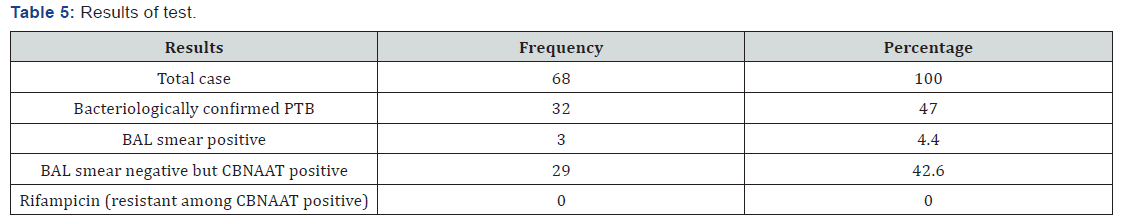
We included 68 patients in our study. Out of 68 patient’s majority were males (79.4%). The mean age of the patients was 36.8 years. Among 68 patients cough was the most common symptom being reported by 45 patients (66.1%), followed by fever in 37 patients (54.4%), weight loss was present in half of the patients and haemoptysis in 11 patients (16.1%). Chest x-ray was performed in all patients. Radiological features compatible with the diagnosis of tuberculosis included consolidation (27.9%), fabricator lesion (23.5%), nodular opacities (11.7%), military shadows (2.9%) and others (13.2%). Around 13 patients (19.1%) were previously treated for tuberculosis while the rest of the patients (81.9%) were never treated. In our study bronchoscopy was performed in all 68 patients and bronchial aspirate samples were collected and underwent smear microscopy and 3 smear samples came positive of AFB (Table 5). Among rest 65 samples mycobacterium tuberculosis was detected in 29 BAL samples and all 29 BAL samples were sensitive to Rifampicin. Rest 36 BAL samples were negative for mycobacterium tuberculosis by CBNAAT.
Discussion
Although the relative transmission rate of smear negative tuberculosis is lower than that of smear positive cases, it is still responsible for 17% of tuberculosis transmission [9]. The diagnosis of pulmonary TB in patients with negative expectorated sputum results remains challenging due to variable diagnostic yields of any single test [10].
Mycobacterial cultures are highly specific and gold standard but are expensive, laborious, requires trained personnel, not widely available and takes 6 - 8 weeks to give the results [11]. The Expert MTB/RIF assay is, however, a simple assay that can be performed with minimal training. The results are available within a couple of hours. This test was offered at WHO centres for TB control, so they are available free of charge to the patient [11].
In this study most of the cases (35.2%) presented in age group ‘less than 30 years’ followed by 30-39 years age group (22%). Mean age in our study was 38.2 years, similar to studies done by Vivek N. Iyer et al. [10]. had mean age of their patients 37 years and kanwal Fatima khalil et al. [12] mean age of study population was 38.56 years. While Poojan shrestha et al. [13] had Mean age 52 years.
In our study out of total 68 cases, 79.4% were male while 20.1% population were of female. Similar studies done by Vivek N. Iyer et al. [10] And by Poojan Shrestha [13] at el had also shows male predominance with 66.6% and 62.1% respectively. In contrast to kanwal Fatima khalil et al. [11] study shows female predominance (61.3%).
Most common symptom in our study was cough (66%%) followed by loss of appetite (69.4 %) and fever (54.4%). Cough was also chief presenting symptom in study done by Pierre Le Palud et al. (51.9%) [11] Vivek N. Iyer et al. [10] 60%, Poojan shrestha et al. [13] 71.7%, Sanjay awashiya et al. [9] 72.2%.
The most common lesions detected by chest imaging were consolidation (27.9%) followed by fibro cavitary diseases (23.5%). Similar findings also seen in study done by Sanjay awashiya et al. [9]. Whereas in study by Pierre Le Palud et al. [11]. nodules (53.7) were the most common radiological finding.
Out of 68 clinic-radiologically suspected patients, only 3 were BAL smear positive by ZN staining while another 29 were further detected by CBNAAT giving a total bacteriological figure of 32. similar study by Sanjay awashiya et al. [9], the yield by CBNAAT was 47.2% for smear-negative cases. Our results are little lower (44.6%).
Conclusion
In those cases of pulmonary tuberculosis who have either smear-negative or sputum-scarce disease, diagnostic bronchoscopy plays an important role. Also, CBNAAT had a superior diagnostic yield to detect Mycobacterium tuberculosis and rifampicin resistance. This test has the advantages of being inexpensive, requires less manpower and gives results on the same day. Hence, a positive Expert MTB/RI assay may be a useful adjunct to diagnosis and detection of MDR-TB in bronchial aspirate specimen.
Further research is needed evaluating the cost effectiveness, patient acceptability and impact on overall out-of-pocket expenditure of Expert testing provided at a direct cost to the patient, to determine the optimal sustainable use of this technology while maximizing equality of access.
(Table 1) Diagnostic methods used for the microbiological/ histopathological diagnosis in a patient with suspected pulmonary tuberculosis who is sputum smear-negative or produces inadequate sputum.
a) Sputum induction with hypertonic saline.
b) Transtracheal needle aspiration.
c) Radiologically guided transthoracic needle aspiration. Gastric lavage
c) Radiologically guided transthoracic needle aspiration. Gastric lavage
(a) Rigid bronchoscopy
2. Flexible fibreoptic bronchoscopy
(a) Bronchial aspirate
(b) Bronchial washings
(c) Bronchial brush smear
(d) Bronchoalveolar lavage
(e) Bronchial biopsy
(f) Transbronchial lung biopsy
3. Post-bronchoscopy sputum Others -
Peripheral blood examination using serological and molecular methods.
References
- (2017) Global TB report.
- Colebunders R, Bastian I (2000) A review of diagnosis and treatment of smear negative Pulmonary Tuberculosis. Int J Tuberc Lung Dis 4(2): 97-107.
- TB India 201 RNTCP Status Report. New Delhi: Central TB Division, Directorate General of Health Services, Ministry of Health and Family Welfare, Government of India.
- Harris AD, Mphases NB, Mundy C, Banerjee A, Kwanjana IH, et al. (2000) Screening tuberculosis suspected using two sputum smears. Int J Tuberc Lung Dis 4(1): 36‑40.
- Venkateshiah SB, Mehta AC (2003) Role of flexible brochoscopy in the diagnosis of pulmonary tuberculosis in immunocompetent individuals. J Bronchol 10(4): 300-306.
- Nussbaum E (2002) Pediatric fiberoptic bronchoscopy: Clinical experience with 2,836 bronchoscopies. Pediatr Crit Care Med 3(2): 171-176.
- Harrison BD (1993) Guidelines for care during bronchoscopy. British Thoracic Society. Thorax 48(5): 584.
- (2013) British Thoracic Society Guidelines on Flexible Bronchoscopy. Thorax 56 (1): 1‑21.
- Avashia S, Choubey S, Mishra S, Atul K (2016) To study the usefulness of CBNAAT (cartridge based nuclear acid amplification test) in BAL (bronchoalveolar lavage) samples in the diagnosis of smear-negative/non-sputum producing patients with suspected tuberculosis. J Evolution Med Dent Sci 5(1): 55-59.
- Iyer VN, Joshi AY, Boyce TG, Brutinel MW, Scalcini MC, et al. (2011) Bronchoscopy in suspected pulmonary TB with negative induced-sputum smear and MTD (®) Gen-probe testing. Respir Med 105(7): 1084-1090.
- Le Palud P, Cattoir V, Malbruny B, Magnier R, Campbell K, et al. (2014) Retrospective observational study of diagnostic accuracy of the Xpert® MTB/RIF assay on fiberoptic bronchoscopy sampling for early diagnosis of smear-negative or sputum-scarce patients with suspected tuberculosis. BMC Pulm Med 14: 137.
- Khalil KF, Butt T (2015) Diagnostic yield of Bronchoalveolar Lavage gene Xpert in smear-negative and sputum-scarce pulmonary tuberculosis. J Coll Physicians Surg Pak 25(2): 115-118.
- Shrestha P, Arjyal A, Caws M, Krishna GP, Abhilasha K, et al. (2015) The application of GeneXpert MTB/RIF for smear negative TB diagnosis as a Fee-paying service at a south Asian general hospital. Tuberculosis Research and Treatment 2015: 1-6.






























