Implications of Non-invasive Mechanical Ventilation in Lung Transplantation. Old and New Frontiers?
Gema Tirado–Conde1, Gema Tirado–Conde1 José M Naranjo 2 and Antonio M Esquinas3
1Clinical Management Unit of Respiratory Medicine, Complejo Hospitalario Universitario de Granada, Spain
2Department of Thoracic Surgery and Lung Transplantation, Hospital Universitario Puerta de Hierro, Spain
2Department of Intensive Care Unit, Hospital General Universitario Morales Meseguer, Spain
Submission: November 25, 2016; Published: January 05, 2017
*Corresponding author: Dr. Gema Tirado Conde, MD, PhD, Consultant and Chest Physician in Clinical Management Unit of Respiratory Medicine. Hospital Universitario “Virgen de las Nieves”. Avda. de las Fuerzas Armadas, s/n. ZIP CODE: 18014; Granada, Spain, Tel: +34 956 005 002; +34 645619550; E-mail:
How to cite this article: Gema T–C, Marina O A, José M N, Antonio M E. Implications of Non-invasive Mechanical Ventilation in Lung Transplantation.002 Old and New Frontiers?. Int J Pul & Res Sci. 2017; 1(1): 555555. DOI:10.19080/IJOPRS.2017.01.555555
Abstract
As lung transplantation has become more successful, the selection criteria have broadened; however, some relative contraindications to lung transplantation are controversial. Some programs consider mechanical ventilation to be a major contraindication to lung transplantation because airway colonization with bacteria may lead to nosocomial infection and respiratory muscle deconditioning may necessitate prolonged postoperative ventilatory support. Non-invasive mechanical ventilation is accepted as a bridge to lung transplantation, but there is little evidence to support its use outside this setting. Use of non-invasive positive pressure ventilation (NPPV) has been reported as a means of avoiding orotracheal intubation in cases of respiratory failure, and in cases of refractory hypoxia; and several longitudinal randomised studies have shown its superiority over conventional ventilation.
Keywords:Non-invasive ventilation; Non-invasive positive pressure ventilation; Acute respiratory distress syndrome; Cystic fibrosis; Lung protective ventilation; Mechanical ventilation; Airway lesions; Tidal volume; Ventilator induced lung injury
Introduction
In 1909, Meltzer and Auer published a study on continuous breathing without respiratory movements obtained by introducing a continuous stream of air and anaesthetic vapour into the trachea [1]. This can be seen as the origin of mechanical ventilation, as it preceded the subsequent development of methods for applying intermittent positive pressure and orotracheal tubes with pilot balloon. In the last 30-40 years, important progress has been made due to better understanding of the Pathophysiology of breathing, the emergence of new specialists in intensive respiratory care, and technological development. Several alternatives breathing support strategies have been designed that have reduced the associated complications.
Purpose of Ventilation
The study adopted a case study research design. Theresearcher applied survey approach with purposive samplingto select 27 respondents from police investigators involvedin the investigations [36]. The conducted extensive review ofliterature and obtained various preliminary factors to be tested[37]. Hypothesis formulated to be tested for each factor was:Null Hypothesis, H0: The identified factors have no significantinfluence on effectiveness of murder procedures at profiling;Alternative Hypothesis, H1: The identified factors havesignificant influence on effectiveness of murder procedures atprofiling; the researcher used questionnaires and interviewguides to help in data collection. The questionnaires closed endedquestions with Likert rating of 1-5 in addition to structuredopen-ended questions at the end. Necessary permissions weresought from the National Commission of Science, Technologyand Innovation and from county and police authorities as wellas the respondents. Ethical guidelines for social research wereadhered to during the process [38]. The researcher interviewed some directors of the company to gain insights into the problem.Sensitivity of the issue was a major limitation in the research.
Face and content validity of the research instruments wasachieved when they were subjected to review by an authoritywith good professional and research standing and found to bevalid. The instruments were then tested and adjustments madeaccording to recommendations given by experts whose opinionwas sought by the researcher. Secondary data collection frompublications, books, news reports, police preliminary reportswas done. Secondary data from county criminal investigations office (CCIO) in the county (Murang’a County) where the KihiuMwiri Company was located proved useful in giving insights intothe study. Media reports also gave highlights into the problemand led the researcher to follow up and obtain even case numbersto verify the prosecution process and identify gaps. Quantitativedata was analysed using descriptive statistics where mean,mode and standard deviation were obtained [39]. One samplet-test was performed and significance levels of the results noted.Correlation analysis of variables was carried out to give insightinto how the factors relate to effectiveness of murder profiling.
Indications of Ventilation
Mechanical ventilation is an intervention that enables adequate gas exchange during certain acute events. It is indicated in the following circumstances:
- Insufficient alveolar ventilation, with elevated PCO2.Rapid elevation of PCO2 is accompanied by significantrespiratory acidosis; a more gradual increase can becompensated and better tolerated. There is no clear cut-offpH value beyond which a patient requires ventilation. Zwillchsuggested 7.30 [2], below which morbidity and mortality aresignificant.
- Diminished or unstable ventilation: manifests as aslower respiratory rate or even apnoea. It occurs in situationssuch as head trauma, drug overdoses or cerebrovascularaccidents. There is a risk of apnoea, so ventilation is indicatedeven when there is no hypercapnia.
- Severe hypoxaemia, which does not resolve with theadministration of oxygen through a mask
- Insufficient pulmonary expansion: can cause atelectasisand pneumonia. It can occur during general anaesthesia,trauma or acute restrictive pulmonary disease.
- Insufficient respiratory muscle function: such as inGuillen-Barré syndrome.
- Excessive respiratory effort: which the patient cannotmaintain. During an acute disorder, it usually starts withtachypnoea.
Complications of Mechanical Ventilation
Complications can be due to the underlying condition,its severity, the intensive care setting and mechanicalventilation itself.
- Altered ventilation-perfusion ratio: perfusion increasesin dependent lung regions, while ventilation increases in therest.
- Reduced alveolar perfusion: high-pressure valuesin the airways, especially with hypovolaemia, can causecompression in the pulmonary capillaries, transformingfunctioning alveolar-capillary units into physiological deadspaces.
- Altered circulation: as intra-thoracic pressure increases,venous return diminishes, which in turn diminishes cardiacoutput and renal perfusion. This is further aggravated in thecase of hypovolaemia.
- Liver and kidney dysfunction: the use of PEEP has beenassociated with reduced portal and renal flow rates, whichcan cause dysfunction in these organs.
- Increased intracranial pressure: an increase in intrathoracicpressure causes reduced venous drainage from thehead.n
- Gastric distension: due to swallowing air becauseof leaks around the balloon in patients with orotrachealintubation.
- Altered acid-base balance: usually due to sub-optimalventilator adjustment.
- Air entrapment, dynamic hyperinflation and auto-PEEP: when the expiratory flow is blocked, exhalationmay not have completed before the next inhalation starts.Pulmonary volume and alveolar pressure, therefore, arestill high at the end of the exhalation, resulting in the samephysiological effects as excessive PEEP.
- Barotrauma: manifest as pneumothorax,pneumomediastinum or subcutaneous emphysema. Thecause is usually interstitial alveolar rupture, with subsequentdissection to the mediastinum or elsewhere.
- Volutrauma (ventilator-induced lung damage): theprecise mechanism is not clear, but it is associated withalveolar over distension.
- Nosocomial pneumonia: from oropharyngeal germs.
- Air way lesions: lesions caused during orotrachealintubation, tracheal stenosis, bronchoaspiration, andtracheal-oesophageal fistula.
- Muscle weakness: due to long-term use of musclerelaxants.
- Reduced oxygenation in ventilated patient: thereare several causes, such as ventilator or circuit problems,unfavourable evolution of the patient’s primary process, theonset of a new medical problem, or certain manoeuvres andinterventions.
Non-Invasive Positive Pressure Ventilation (NPPV)
The use of continuous positive airway pressure (CPAP) inthe airways was first suggested in 1981 to treat obstructivesleep apnoea [3]. The application of CPAP through a mask forthis purpose was the first step in the development of NPPV forpatients with chronic respiratory failure. Generally speaking,there are two NPPV techniques: positive pressure appliedcontinuously to the airway throughout the respiratory cycle(CPAP); or positive pressure applied intermittently. In CPAP,breathing is spontaneous and generated solely by the respiratorymuscles. Intermittent positive pressure systems, meanwhile, areapplied in one of two ways:
- pressure support ventilation, in which a certainpressure is applied to the airway during inhalation toimprove spontaneous breathing. The respiratory rate isdetermined by the patient and the tidal volume by theamount of inspiratory support pressure and factors such asinspiratory and respiratory effort. It is activated either whensystem pressure decreases or flow increases;
- bi-level positive airway pressure, which is similar toCPAP, but with pressure support. Inspiratory and expiratorypressure can be adjusted and the ventilator switches frominhalation to exhalation when flow changes are detected.
The difference between inspiratory and expiratory pressureis the non-invasive pressure support. Positive pressure can beapplied at the end of exhalation (PEEP) with either of these twomethods. The success of NPPV largely depends on the patient’sability to cooperate and synchronise his or her breathing with theventilator because, unlike invasive ventilation, the patient doesnot receive muscle relaxants. This type of ventilation was initiallyused in patients with neuromuscular disorders and chest walldiseases, subsequently extending its use to other disorders [4].The use of NPPV was first described in 1989 to circumvent theneed to intubate patients with acute respiratory failure [5] and itwas subsequently described in COPD exacerbations [6] reducingventilation time and duration of ICU admission, suggesting thatNPPV could reduce ventilator-induced morbidity and the cost ofCOPD exacerbations. Subsequent studies of patients with COPDexacerbations [7,8] support the use of NPPV to circumventorotracheal intubation.
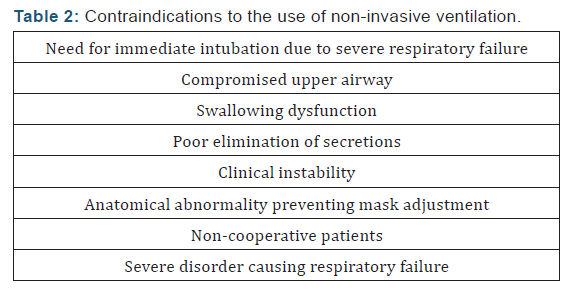
Use of NPPV has also been described in acute respiratoryfailure due to causes other than COPD: in patients with acutedecline due to restrictive thoracic diseases [9] hypoxemicrespiratory failure without hypercapnia (pneumonia, ADRS,cardiogenic oedema) [10] acute respiratory failure in theimmediate post-operative period following extubation [11]; inpatients who require orotracheal intubation and mechanicalventilation, NPPV can be used in the “weaning” process [12]and also in patients with respiratory failure who are notsuitable for orotracheal intubation [13]. Appropriate patientscreening is crucial to ensure the success of NPPV (Table 1) andto prevent use when contraindicated (Table 2). Unlike invasiveventilation, non-invasive techniques do not require an artificialairway (endotracheal tube or tracheostomy). A good interface isessential. Both nasal and oronasal and facial masks can be used.Nasal masks leave the mouth uncovered, enabling the patient totalk and eat, but air loss through the mouth is common. Whatevertype is chosen, it should always be a good fit.
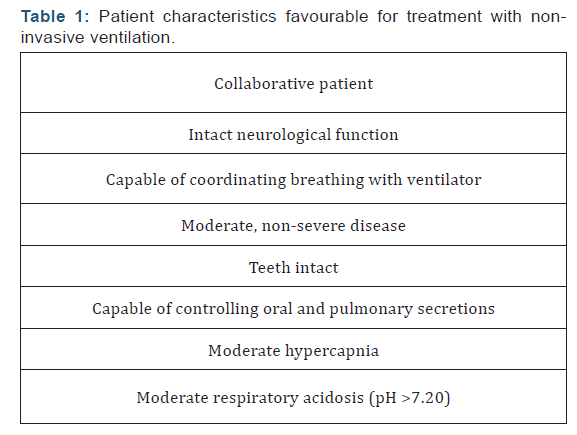

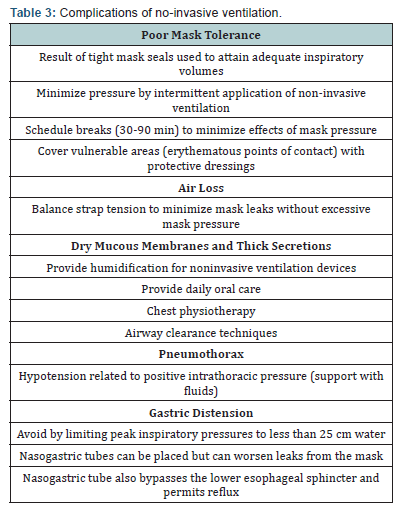
To facilitate tolerance, it is good idea to initially use lowpressure. Initial pressure support could be 4-10 cm H2O, PEEP:2-4 cm H2O, inspiratory pressure: 8-12 cm H2O and expiratorypressure: 2-4 cm H2O. The initial tidal volume ranges from 10 to15 ml/kg. As patient tolerance increases, inspiratory pressureor tidal volume can be gradually increased to enable smallreductions in PCO2 (5-10 mmHg). If oxygenation is still low,expiratory pressure can be increased. Patients who respond wellto the system will present lower respiratory rate, heart rate andPCO2 after a few hours. The possible complications are shownin Table 3. Several studies have shown the efficacy of NPPVfor preventing nosocomial pneumonia and other orotrachealintubation complications [14-16]. As these patients are notsedated, complications due to immobilisation are prevented andadequate nutrition is ensured. ICU stays can be prevented. Itdoes, however, have some disadvantages: no airway protectionand no direct access to the trachea for aspiration.
Lung Transplantation
The first references to lung transplantation date from the1940s and 1950s, when authors such as Vladimir Demikhov andDominique Metras demonstrated the viability of the surgicaltechnique in experimental animals [17]. Subsequently, in1963, James Hardy performed the first single lung transplantin humans. The patient was a death row inmate who had beendiagnosed with squamous cell carcinoma in the left lung andemphysema. He only survived for 18 days, and died from kidneyfailure [18]. Further attempts were made in the following years,but they systematically failed due to infections, graft rejectionand problems related to bronchial anastomosis healing. Itwas not until the 1980s when the Toronto group, under theleadership of Joel Cooper, performed the first successful single(1983) and double (1986) lung transplants, thus establishingthe procedure as treatment for end-stage lung diseases [19].Since then there has been significant progress in both surgicaltechnique and overall patient management, and the procedurecan now be safely performed with greater short- and mediumtermsurvival rates. It is currently a valid therapy for some endstagelung diseases with less than 2 years of life expectancy forwhich there are no further medical options.
The diseases that most often require this procedure are:emphysema-like COPD with or without alpha-1-antitripsin deficit,interstitial diseases such as idiopathic pulmonary fibrosis, septicconditions such as cystic fibrosis or bronchiectasis, and primarypulmonary hypertension. The current trend is to perform doublelung transplantation, especially in young patients, as they providebetter quality of life and long-term survival, despite greater perioperativemorbidity/mortality [20]. During surgery, the airwayis routinely intubated with a left-sided double lumen tube thatenables independent ventilation of both lungs. Immediatelyafter surgery, patients are ventilated with a standard technique.FiO2 is necessary to maintain the PO2 at over 70 mmHg. The tidalvolume is 12-15 ml/kg and PEEP is 5-7.5 cm H2O. The patient isextubated when there is adequate gas exchange and mechanicalrespiration, usually after 24-48 hours. PEEP is not needed inCOPD patients who receive a single lung, and a lower tidalvolume is used. This reduces hyperinflation of the native lungand minimises compression of the transplanted organ.
Air entrapment by the native lung can cause other problems,such as high airway pressure, CO2 retention and hypotensiondue to reduced venous return. Volume reduction in the nativelung is required in extreme cases to relieve compression in thetransplanted organ. Mechanical ventilation is maintained forlonger, at least 48-72 hours, in patients with vascular pulmonarydiseases who have received a single organ transplant, duringwhich time they are sedated and receive muscle relaxants,remaining in a position in which the native lung is lower,thus maintaining inflation and drainage of the grafted organ.Standard tidal volume is used but PEEP increases to 7.5-10 cmH2O. Mechanical ventilation is prolonged in case of primary graftdysfunction, rejection or infection. In these cases a tracheotomyshould be performed as soon as possible, making the patientmore comfortable, increasing his or her mobility, and enablingoral nutrition.
Use of NPPV in Lung Transplantation
As with any other type of surgery, respiratory complicationscan arise in the post-operative period, such as atelectasis,pneumonia, pulmonary oedema and acute respiratory failuredue to different causes, including pulmonary thromboembolism.Post-operative respiratory failure can be defined as the need tomaintain mechanical ventilation for longer than usual for thesurgery in question, or the need to re-intubate an extubatedpatient [21]. In lung transplantation other specific problemscan also arise, such as vascular or airways complications(stenosis, dehiscence), primary graft dysfunction, pneumoniaand rejection. Nevertheless, acute respiratory failure is the maincause of post-transplant mortality [22]. Special mention shouldbe made of airway anastomoses, specifically dehiscence. In thesecases, either invasive or non-invasive positive pressure canhinder management. In severe cases in which a patient cannot beventilated because all or most of the tidal volume is lost throughdehiscence, the only solution is differential ventilation througha double lumen tube: optimal ventilation in the dehiscence-freelung and ventilation with the lowest possible pressure in theother lung.
Disorders where NPPV can be used have already beenmentioned above. NPPV has been described in general surgeryfor preventing acute post-operative respiratory failure(prophylactic use) or for treatment of this condition when itpresents [23,24], and it can be used both with continuous (CPAP)and intermittent positive pressure. The expected benefits are:increased lung gas volume, improved gas exchange, reducedatelectasis, reduced respiratory effort, and circumvention ofinvasive ventilation. In the case of lung transplantation, use ofNPPV to avoid orotracheal intubation in cases of respiratoryfailure has been reported. A study published in 2000 [14]randomised 40 solid organ recipients (lung, liver or kidney) withacute hypoxemic respiratory failure to be treated with NPPVor conventional therapy. There was a sustained, statisticallysignificant improvement in oxygenation in the NPPV group,with less need for invasive ventilation. The incidence of sepsiswas also lower, as was ICU mortality rate, although there wasno difference in hospital mortality rate. Another observationalstudy conducted in 2001 [25], in which 21 patients undergoingbilateral lung transplant presented acute respiratory failureafter extubation, found that NPPV circumvented the need forendotracheal intubation in 85% of all cases. Rocco, et al. [25]described a series of 21 patients (18 with cystic fibrosis) who,after undergoing double lung transplant developed respiratoryinsufficiency requiring ventilation support.
After being treated with NPPV through a facemask,orotracheal intubation was avoided in 18 patients, who weredischarged from the ICU. Of the 3 who required intubation, 1survived and the other 2 died from septic shock. It has beensuggested that NPPV can reduce extra vascular pulmonaryfluid and restore pulmonary volume, reducing dyspnoea andrespiratory effort. In 2009, Feltraco, [26] reported the use ofNPPV for the treatment of refractory hypoxia due to primarygraft dysfunction, describing two cases. In general, respiratorysupport is well tolerated and resolves atelectasis and infiltrates,thereby avoiding orotracheal intubation. The use of NPPVassociated with changes from a prone to supine position, oreven combined with Trendelenburg, improves the ventilationperfusionratio, suggesting that it could also be used for otherlung conditions, which involve areas of dorsal-basal non-recruitable atelectasis.
High frequency percussive ventilation is a method that canbe applied by intubation or a facemask [27]. It is a time-cycled,limited pressure mode of ventilation. Cycles are delivered athigh frequency (200-900 cycles per minute) in stages. This giveslow volume, high rate ventilation that produces a more uniformgas exchange and better distal ventilation, while facilitatingelimination of secretions. High frequencies (300-600 cyclesper minute) facilitate oxygenation, while low frequencies (180-240) facilitate CO2 elimination. Feltraco [28] described itsuse, combined with postural changes, in three patients whopresented respiratory failure after extubation following doublelung transplantation, thereby avoiding re-intubation in all three.Phrenic nerve injuries during lung transplantation can be due todirect damage caused during mediastinal dissection or distensionwhile manipulating the pericardium and hypothermia. Aftersurgery, they can give rise to complications such as atelectasis,pneumonia, hypoxaemia and hypoventilation, increasingduration of mechanical ventilation and ICU admission. NPPVhas been reported to reduce this time, and can even be appliedoutside the ICU [29].
NPPV has also been used during the pre-transplant period.Ventilator dependence has traditionally been considered arelative contraindication for transplantation, as the procedure isassociated with a higher mortality rate in such patients [30,31].The presence of microbial colonisation of the airway increasesthe risk of post-operative pneumonia. Prolonged immobility canalso reduce a patient’s physical strength, increasing the risk ofpost-operative complications. However, up to 3% of transplantshave been performed in the US on ventilator-dependent patients[32]. Ideally, in the case of invasive ventilation, the aim shouldbe to extubate once the patient has overcome exacerbation andperform the transplant when he or she is no longer ventilatordependent.Only in carefully selected cases can transplantationbe considered in patients who present progressive, irreversiblerespiratory failure as the result of the evolution of their condition.
The possibility of transplanting a ventilator-dependentpatient is considered when respiratory failure is the resultof the irreversible evolution of the underlying condition,and other causes (such as respiratory infection, pulmonarythromboembolism, heart failure, etc.) have been ruled out,providing the surgery can be performed before the onset ofthe aforementioned complications derived from mechanicalventilation, basically pneumonia and decline in physical status.Pulmonary conditions are the main cause of morbidity-mortalityin cystic fibrosis, and the use of NPPV has been reported toprolong the life of end-stage patients until a donor appears,avoiding the complications of invasive ventilation. Efrati, et al.[33] described a series of 9 patients: four successfully underwenttransplant and 3 died on the waiting list. The other two were stillalive when the paper was published. Significant increase in bodymass index, improvement in pH and PCO2, and better sleepsquality and everyday activities, with no ventilation-relatedcomplications, have been reported. Further studies describe thesuccessful use of NPPV while waiting for lung transplant [34-37]particularly in cystic fibrosis patients.
Conclusion
In the last 30-40 years, important progress in respiratorysupport has been made due to better understanding of thephysiology of breathing, the emergence of new specialists inintensive respiratory care, and technological development.Several alternative respiratory support methods have reduced thecomplications associated with invasive mechanical ventilation.The diseases that most frequently require lung transplantationare: emphysema-like COPD with or without alpha -1- antitrypsindeficit, interstitial diseases such as idiopathic pulmonaryfibrosis, septic diseases such as cystic fibrosis or bronchiectasisand primary pulmonary hypertension. The current trend is toperform double lung transplants, especially in young patients, asthey provide better quality of life and long-term survival, despitegreater peri-operative morbidity/mortality. In the case of lungtransplantation, use of NPPV has been reported as a means ofavoiding orotracheal intubation in cases of respiratory failure,and in cases of refractory hypoxia; and several longitudinal,randomised studies have shown its superiority over conventionalventilation.
References
- Meltzer SJ, Auer J (1909) Continuous respiration without respiratorymovements. J Exp Med 11(4): 622-625.
- Zwillich CW, Pierson DJ, Creagh CE, Sutton FD, Schatz E, et al. (1974)Complications of assisted ventilation. A prospective study of 354consecutive episodes. Am J Med 57(2): 161-170.
- Sullivan CE, Issa FG, Berthon-Jones M, Eves L (1981) Reversal ofobstructive sleep apnoea by continuous positive airway pressureapplied through the nares. Lancet 1 (8225): 862-865.
- Hill NS (1993) Noninvasive ventilation. Does it work, for whom, andhow? Am Rev Respir Dis 147(4): 1050-1055.
- Meduri GU, Conoscenti CC, Menashe P, Nair S (1989) Noninvasiveface mask ventilation in patients with acute respiratory failure. Chest95(4): 865-870.
- Brochard L, Isabey D, Piquet J, Amaro P, Mancebo, et al. (1990)Reversal of acute exacerbations of chronic obstructive lung disease byinspiratory assistance with a face mask. N Engl J Med 323(22): 1523-1530.
- Kramer N, Meyer TJ, Meharg J, Cece RD, Hill NS (1995) Randomized,prospective trial of noninvasive positive pressure ventilation in acuterespiratory failure. Am J Respir Crit Care Med 151(6): 1799-806.
- Brochard L, Mancebo J, Wysocki M, Lofaso F, Conti G, et al. (1995)Noninvasive ventilation for acute exacerbations of chronic obstructivepulmonary disease. N Engl J Med 333(13): 817-822.
- Meduri GU, Abou-Shala N, Fox RC, Jones CB, Leeper KV, et al. (1991)Noninvasive face mask mechanical ventilation in patients with acutehypercapnic respiratory failure. Chest 100(2): 445-454.
- Wysocki M, Tric L, Wolff MA, Millet H, Herman B (1995) Noninvasivepressure support ventilation in patients with acute respiratory failure.A randomized comparison with conventional therapy. Chest 107(3):761-768.
- Benhamou D, Girault C, Faure C, Portier F, Muir JF (1992) Nasal maskventilation in acute respiratory failure. Experience in elderly patients.Chest 102(3): 912-917.
- Nava S, Ambrosino N, Clini E, Prato M, Orlando G, et al. (1998)Noninvasive mechanical ventilation in the weaning of patients withrespiratory failure due to chronic obstructive pulmonary disease. Arandomized, controlled trial. Ann Intern Med 128(9): 721-728.
- Freichels TA (1994) Palliative ventilatory support: use of noninvasivepositive pressure ventilation in terminal respiratory insufficiency. AmJ Crit Care 3(1): 6-10.
- Antonelli M, Conti G, Bufi M, Costa MG, Lappa A, et al. (2000)Noninvasive ventilation for treatment of acute respiratory failure inpatients undergoing solid organ transplantation: a randomized trial.JAMA 283(2): 235-241.
- Antonelli M, Conti G, Rocco M, Bufi M, De Blasi RA, et al. (1998)A comparison of noninvasive positive pressure ventilation andconventional mechanical ventilation in patients with acute respiratoryfailure. N Engl J Med 339(7): 429-435.
- Nourdine K, Combes P, Carton MJ, Beuret P, Cannamela A, et al. (1999)Does noninvasive ventilation reduce the ICU nosocomial infectionrisk? A prospective clinical survey. Intensive Care Med 25(6): 567-573.
- Konstantinov IE (1998) A Mystery of Vladimir P. Demikhov: The 50thAnniversary of the First Intrathoracic Transplantation. Ann ThoracSurg 65(4): 1171-1177.
- Hardy JD, Eraslan S, Webb WR (1964) Transplantation of the lung. AnnSurg 160: 440–448.
- Toronto Lung Transplantation Group (1986) Unilateral lungtransplantation for pulmonary fibrosis. N Engl J Med 314(18): 1140-1145.
- Force SD, Kilgo P, Neujahr DC, Pelaez A, Pickens A, et al. (2011) Bilaterallung transplantation offers better long-term survival, compared withsingle-lung transplantation, for younger patients with idiopathicpulmonary fibrosis. Ann Thorac Surg 91(1): 244-249.
- Chiumello D, Chevellard G, Gregoretti C (2011) Non-Invasiveventilation in postoperative patients: a systematic review. IntensiveCare Med 37(6): 918-929.
- Cooper JD, Patterson GA, Trulock EP (1994) Results of singleand bilateral lung transplantation in 131 consecutive recipients.Washington University Lung Transplant Group. J Thorac CardiovascSurg 107(2): 460-470.
- Ferreyra G, Long Y, Ranieri VM (2009) Respiratory complications aftermajor surgery. Curr Opin Crit Care 15(4): 342-348.
- Jaber S, Chanques G, Jung B (2010) Postoperative noninvasiveventilation. Anesthesiology 112(2): 453-461.
- Rocco M, Conti G, Antonelli M, Bufi M, Costa MG, et al. (2001) Noninvasivepressure support ventilation in patients with acute respiratoryfailure after bilateral lung transplantation. Intensive Care Med 27(10):1622-1626.
- Feltracco P, Serra E, Barbieri S, Persona P, Rea F, et al. (2009) Noninvasiveventilation in prone position for refractory hypoxemia afterbilateral lung transplantation. Clin Transplant 23(5): 748-750.
- Lucangelo U, Fontanesi L, Antonaglia V, Pellis T, Berlot G, et al.(2003) High frequency percussive ventilation (HFPV). Principles andtechnique. Minerva Anestesiol 69(11): 848-851.
- Feltraco P, Serra E, Barbieri S, Milevoj M, Michieletto E, et al. (2012)Noninvasive High-Frequency Percussive Ventilation in the PronePosition after Lung Transplantation. Transplant Proc 44(7): 2016-2021.
- Berk Y, van der Bij W, Erasmus ME, Wijkstra PJ (2006) Non-invasiveventilation in phrenic nerve dysfunction after lung transplantation: anattractive option. J Heart Lung Transplant 25(12): 1483-1485.
- American Thoracic Society (1998) International guidelines for theselection of lung transplant candidates. Am J Respir Crit Care Med158(1): 335-339.
- Hosenpud JD, Bennett LE, Keck BM, Boucek MM, Novick RJ (2001)The Registry of the International Society for Heart and LungTransplantation: eighteenth official report. J Heart Lung Transplant20(8): 805-815.
- O’Brien G, Criner GJ (1999) Mechanical Ventilation as a Bridge to LungTransplantation. The Journal of Heart and Lung Transplantation 18(3):255-265.
- Efrati O, Modan-Moses D, Barak A, Boujanover Y, Augarten A (2004)Long-term non-invasive positive pressure ventilation among cysticfibrosis patients awaiting lung transplantation. Isr Med Assoc J 6(9):527-530.
- Quaranta AJ, Roy B, O’Brien G, Kreimer DT, Krachman S, et al. (1996)Noninvasive positive pressure ventilation as bridge therapy to lungtransplantation or volume reduction surgery. J Resp Crit Care Med153(4): A608.
- Piper AJ, Parker S, Torzillo PJ, Sullivan CE, Bye PT (1992) Nocturnalnasal IPPV stabilizes patients with cystic fibrosis and hypercapnicrespiratory failure. Chest 102(3): 846-850.
- Hobson ME, Madden BP, Steven MH, Tsang VT, Yacoub MH (1991)Noninvasive mechanical ventilation for cystic fibrosis patients: apotential bridge to transplantation. Eur Resp J 4(5): 524-527.
- Felten ML, Moyer JD, Dreyfus JF, Marandon JY, Sage E, et al. (2016)Immediate postoperative extubation in bilateral lung transplantation:predictive factors and outcomes. Br J Anaesth 116(6): 847-854.






























