A Tracheal Web as a Cause of Dyspnea in a Patient who had been treated for Asthma in the Past 35 years
Strouvalis Ioannis1*, Diamantea Filia2, Karagiannidis Napoleon2, Nikolopoulou Angeliki3 and Polychronopoulos Vlassios4
1Pulmonologist/Intensivist, Central Clinic of Athens, Greece
2Pulmonary Medicine, Sismanogleio Public Hospital, Greece
3Cardiologist, Attikon University Hospital, Greece
4Consultant Pulmonologist, Pulmonary Clinic, Hygeia Hospital, Greece
Submission: October 31, 2016; Published: November 18, 2016
*Corresponding author: Strouvalis Ioannis, Pulmonologist/Intensivist, ICU Director, Central Clinic of Athens, Greece, Tel:00306972841238; E-mail:drstrouvalis@yahoo.com
How to cite this article: Strouvalis I, Diamantea F, Karagiannidis N, Nikolopoulou A, Polychronopoulos V. A Tracheal Web as a Cause of Dyspnea in a Patient who had been treated for Asthma in the Past 35 years. Int J Pul & Res Sci. 2016; 1(1) : 555554. DOI:10.19080/IJOPRS.2016.01.555554
Abstract
A Tracheal Web is a soft tissue formation partially occluding the trachea lumen. It is of benign origin and can be either congenital or acquired – the latter mostly in patients with a history of prolonged intubation. Due to the symptoms that are consistent with obstructive lung disease, it can often be misdiagnosed as such. As a result some patients may have been categorized as asthmatics with minimal response to treatment, since the tracheal web causes a fixed obstruction pattern. We describe a case of a female 57 year old patient that had been under asthma treatment for 35 years and was admitted to Sismanogleio Public Hospital, Greece, due to dyspnea consistent with an asthma exacerbation.
Keywords: Tracheal web; Asthma; Fiberoptic bronchoscopy; Cauterization
Introduction
Laryngotracheal stenosis is a term that refers to a wide range of clinical conditions that apply to the narrowing of the airway. It can be of congenital or acquired origin, malignant or benign [1]. It can cause respiratory symptoms that can be often misdiagnosed as obstructive lung disease [2-4]. A rare laryngotracheal stenosis subtype is the tracheal web. We present a case of a 57-year old female patient with dyspnea who had been diagnosed with asthma since adolescence.
Case History
A 57 year old female patient presented to the ER with symptoms of lower respiratory system infection, probably of viral origin, and an asthma exacerbation. The patient had been diagnosed with asthma and allergic rhinitis in the past (35 years ago) and was under medication with beta 2-agonist and inhaled corticosteroids. She had also recently been diagnosed with GERD. She was admitted in our clinic for further investigation and treatment. During her hospitalization she reported recurrent episodes of shortness of breath and fatigue during the past years, especially after even mild physical activity. Physical examination revealed bilateral inspiratory and expiratory wheezes. Her chest X-ray was not suggestive of any pathologic findings (Figure 1).

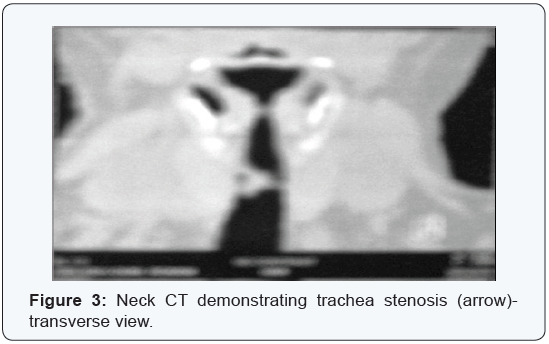
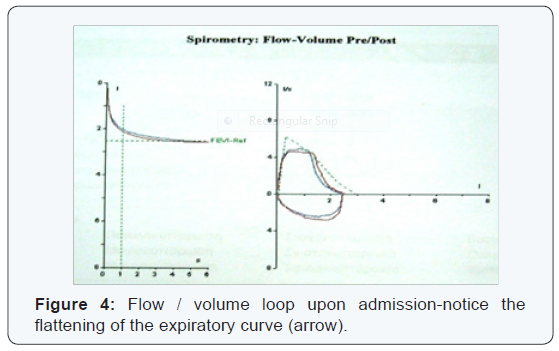
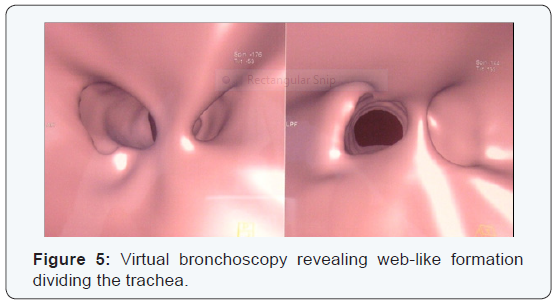
The flow-volume loop demonstated a flattening of the expiratory flow curve at the PEF level (Figure 4). Until the performance status of the patient could allow fiberoptic bronchoscopic evaluation, a virtual bronchoscopy was performed that revealed web-like formations that divided the upper trachea in two unequal segments (Figure 5).
The fiberoptic bronchoscopy that followed had similar findings; at about 2 cm below the vocal cords a diaphragmatic lesion was identified, in the form of scar tissue that divided the trachea in two parts (Figure 6,7). Beneath the dominant part the rest of the trachea was normal (Figure 8,9).
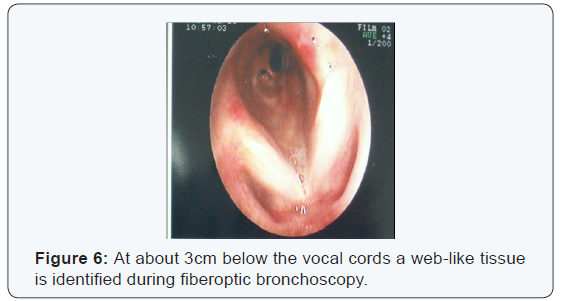
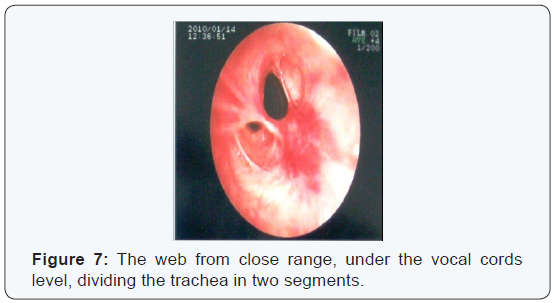
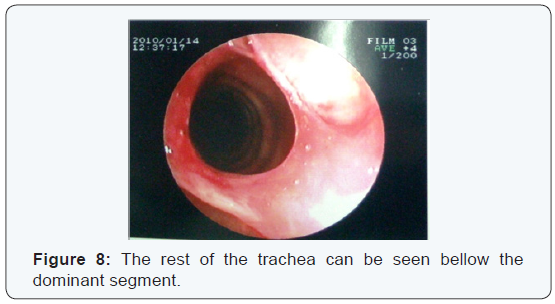
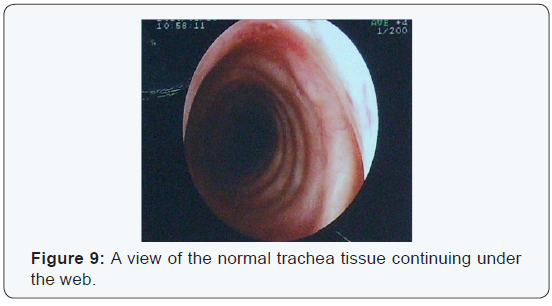
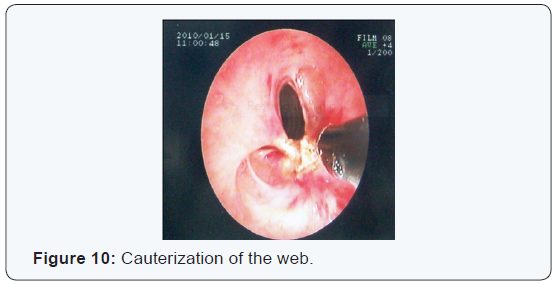
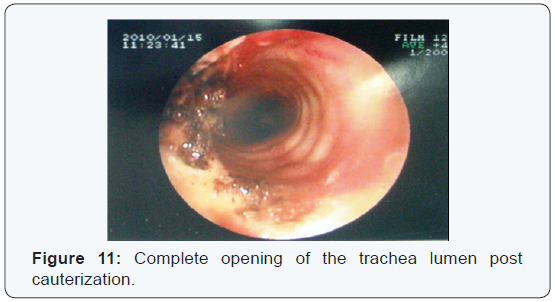
After identifying the lesion, it was removed by means of electric cauterization with practically complete opening of the trachea in full diameter (Figure 10,11). The patient was discharged from the hospital and was programmed for a follow up bronchoscope and PFT`S in 15 days. The follow up revealed a normal trachea diameter and significant improvement in PFT`S (Figure 12,13).


The patient reported a great improvement in her daily activities, with minimization of dyspnea during exercise and less need for inhalers. In the next follow up visits her dyspnea had practically resolved.
Discussion
Tracheal web is a benign subtype of tracheal stenosis. It is a rare malformation of the trachea resulting in narrowing and partial occlusion of the trachea lumen. In most cases it is congenital, while in adults it is more often acquired as a result of prolonged tracheal intubation [5]. It consists of soft tissue in the form of membrane that obstructs partially the trachea lumen at a level that can vary from intra to extra-thoracic trachea, thus causing symptoms as expiratory wheeze and/or stridor depending on the location of the lesion in the trachea lumen [6]. It is a rare condition, with an incidence of 1/104 births in its congenital form [7].
In some cases the condition is misdiagnosed and the respiratory symptoms as wheezing, stridor, dysponea and frequent respiratory tract infections are interpreted as indicators of obstructive lung disease. This for example may result in patients diagnosed with asthma that does not respond to treatment. In other cases the tracheal web is an accidental finding in adults with no prior symptoms that present an unexpected difficulty in intubation [8,9]. Differential diagnosis mainly includes Granulomatosis/polyangiitis, Amyloidosis, Tracheomalacia, benign tumors (i.e. Characinoid) and complete tracheal rings. The idiopathic form of tracheal stenosis has a strong female predominance and has also been associated with GERD [10].
A strong suspicion of upper airway obstruction can be taken into consideration if the PFT`S demonstrate a flattening of the inspiratory and/or expiratory curve with poor postbronchodilator response, while also important is the high FEV1/ PF ratio [11]. Diagnosis can be achieved by computed tomography and fibroptic bronchoscopy (gold standard), while the plain CXR is not usually diagnostic. Treatment is cauterization of the lesion via fibrotic bronchoscopy and in some cases with cryotherapy and balloon dilation, with good results and immediate clinical improvement.
Conclusion
A tracheal web is a condition that membranous soft tissue partially obstructs the trachea lumen, causing symptoms that can be misdiagnosed as obstructive lung disease, or in some cases causing no symptoms but presenting as unexpected intubation difficulty. In our case we dealt with a female patient with chronic dyspnea diagnosed with asthma and GERD that had a fixed obstruction pattern in the flow/volume curve and a poor response to treatment. The fact that, although diagnosed with asthma in the past 35 years, her symptoms diminished and her quality of life improved immediately after the bronchoscopic intervention , should provide food for thought for physicians who face the challenge of patients with a suspected obstructive lung disease that demonstrate a fixed obstruction pattern in PFT`S and poor response to treatment.
References
- Gelbard A (2014) Causes and Consequences of Laryngotracheal Stenosis. The Laryngoscope.
- Ricketti PA, Ricketti AJ, Cleri DJ, Seelagy M, Unkle DW et al. (2010) A 41-year-old male with cough, wheeze, and dyspnea poorly responsive to asthma therapy. Allerg Asthma Proc 31(4): 355-358.
- Parrish RW, Banks J, Fennerty AG (1983) Tracheal obstruction presenting as asthma. Postgrad Med J 59(698): 775-776.
- Galvin IF, Shepherd DR, Gibbons JR (1990) Tracheal stenosis caused by congenital vascular ring anomaly misinterpreted as asthma for 45 years. Thorac Cardiovasc Surg 38(1): 42-44.
- Kokkonouzis I, Mermigkis C, Psathakis K, Tsintiris K (2005) Postintubation tracheal web. J Broncho 12(4): 271-272.
- Legasto AC, Haller JO, Giusti RJ (2004) Tracheal web. Pediatr Radiol 34(3): 256-258.
- Nguyen NK (2006) Unexpected tracheal web encountered during difficult intubation in the operating room. Proc (Bayl Univ Med Cent) 19(3): 224-225.
- Al Badaai Y, Nguyen LH (2008) Difficult intubation due to undiagnosed congenital tracheal web. Int J Ped Otorhinolaryngology 72(9): 1437- 1439.
- Egawa A, Hirabayashi Y, Seo N (2011) Case of unexpected difficult intubation caused by asymptomatic congenital laryngeal web. Masui 60(10): 1211-1213.
- Al-Qadi MO, Artenstein AW, Braman SS (2013) The forgotten zone: Acquired disorders of the trachea in adults. Respir Med 107(9): 1301- 1313.
- Empey DW (1972) Assessment of upper airways obstruction. Br Med J 3(5825): 503-505.






























