- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Deadly High Altitude Pulmonary Disorders: Acute Mountain Sickness (AMS); High Altitude Pulmonary Edema (HAPE) and High Altitude Cerebral Edema (HACE): A Clinical Review
Michael Obrowski1* and Stephanie Obrowski2
1Doctor of Medicine (M.D. – 2000); Assistant Professor of Anatomy; CEO, Chief Physician and Surgeon of Wilderness Physicians, European Union
2Doctor of Medicine (M.D. – 2019); Medical University of Łódź; President of Wilderness Physicians, European Union
Submission: January 26, 2016; Published: January 26, 2016;
*Corresponding author: Michael Obrowski, M.D., Doctor of Medicine (M.D. – 2000); Assistant Professor of Anatomy; CEO, Chief Physician and Surgeon of Wilderness Physicians, European Union, 43C Żeligowskiego Street, #45, Łódź, Poland 90-644, E-mail:drobrowski@gmail.com
How to cite this article: Michael O, Stephanie O. Deadly High Altitude Pulmonary Disorders: Acute Mountain Sickness (AMS); High Altitude Pulmonary Edema (HAPE) and High Altitude Cerebral Edema (HACE): A Clinical Review Int J Pul & Res Sci. 2016; 1(1) : 555553. DOI:10.19080/IJOPRS.2016.01.555553
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Abstract
Mountain Sickness, also called High Altitude Sickness, is specifically a triad of different disorders, in order of increasing seriousness: Acute Mountain Sickness (AMS); High Altitude Pulmonary Edema (HAPE) and High Altitude Cerebral Edema (HACE). These three disorders, with relatively unimportant small variations seen in some Pulmonology Textbooks, because these are so serious, they are all potentially deadly pulmonary disorders and we will discuss these three major, deadly disorders. Each one, starting with AMS, can progress rapidly to HAPE and then HACE. The two authors of this article have over half a century of high altitude mountaineering experience. They have also had and still do have, for the last twenty years, an NGO, Non-Profit Medical Organization (Wilderness Physicians www.wildernessphysicians.org) that specifically deals with outdoor medical issues, wilderness search and rescue, providing hospital level care in the wilderness and also disaster medicine. Since spring is rapidly approaching and many “weekend backpackers” will start going into the mountains, we present this paper with the truths and fallacies of this triad of disorders to refresh the memories of physicians who treat these disorders, either in the field or in the hospital.
Keywords: Acute Mountain Sickness; High Altitude Pulmonary Edema; High Altitude Cerebral Edema; Pneumomediastinum; Rhabdomyolysis; Deep Vein Thrombosis; Pulmonary Embolism; Vasospasms of Cerebral Arteries
Abbreviations: AMS: Acute Mountain Sickness; HAPE: High Altitude Pulmonary Edema; HACE: High Altitude Cerebral Edema; DVT: Deep Vein Thrombosis; PE: Pulmonary Embolism
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Introduction and Facts Regarding AMS
The mildest form of altitude sickness is Acute Mountain Sickness (AMS). Where and how does acute mountain sickness happen? Most people in “relatively” good physical condition, remain feeling well up to altitudes of about 2500meters (8200 feet), the equivalent barometric pressure to which most modern airplane cabins are normally pressurized. However, even at around 1500meters (4920 feet) above sea level, patients may notice more breathlessness than normal during exercise and night vision may become impaired due to lack of oxygen to the ocular apparatus. Above 2500meters (8200 feet), the symptoms of altitude sickness usually become more noticeable.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What are Other Names for AMS?
Acute Mountain Sickness is sometimes colloquially referred to as altitude sickness or mountain sickness; in South America it is called Soroche, in China it is called Jíxìng Gāoyuán Bìng and in Nepal it is called Tīvra Pahāḍa Rōga.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
How are the Symptoms of AMS Recognized?
The most prominent symptom of AMS is usually a severe headache. Most people also experience nausea, vomiting, dehydration, lethargy, dizziness and poor sleep patterns. Symptoms are very similar to a severe, alcohol-induced hangover.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Who gets AMS?
Anyone who travels to altitudes over 2,500meters (8,200 ft.) is at risk for AMS. Normally it does not become noticeable until the patient has been at that altitude for a few hours. Part of the mystery of acute mountain sickness is that it is difficult to predict who will be affected. There are many stories of fit and healthy people being badly limited by symptoms of acute mountain sickness, while older companions have felt fine.
There are a number of factors that are linked to a higher risk of developing the condition. The higher altitude you achieve and the faster your rate of ascent, the more likely you are to get acute mountain sickness. If you have a previous history of suffering from acute mountain sickness, then you are probably more likely to get it again. Older people tend to get less AMS – but this could be because they have more common sense and ascend less quickly. Physical fitness is a suspected key factor, obviously because the patient is in better condition. Smokers are at a much higher risk of AMS due to already having decreased lung function and lung elasticity, combining that with low oxygen concentration at higher altitude increases the probability of AMS, HAPE and HACE [1].
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What Causes Altitude Sickness?
There is much less oxygen high in the mountains so it is reasonable to accept the fact that travelling to high altitude will cause people to feel sick. The problem is, how this shortage of oxygen actually leads to altitude sickness is not fully understood. Some scientists believe that it is due to swelling of the brain but the evidence for this hypothesis is not conclusive. The theory is that in susceptible individuals, swelling could cause a small increase of the pressure inside the skull and lead to symptoms of acute mountain sickness. The swelling may be due to increased blood flow to the brain or any increased permeability [2] of blood vessels in the brain caused by a decrease in the pO2. Altitude sickness has three forms. Mild altitude sickness is called acute mountain sickness (AMS) and is quite similar to a hangover - it causes headache, nausea and fatigue. This is very common: some people are only slightly affected, others feel very sick. However, if a patient has AMS, this should be taken as a warning sign that this patient is at risk of developing the serious forms of altitude sickness: HAPE and HACE. Both HAPE and HACE can develop rapidly and be fatal within hours.
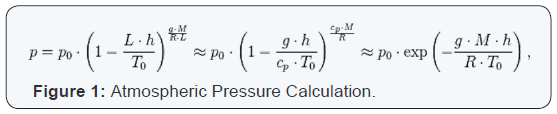
Atmospheric Pressure (also called Barometric Pressure) at sea level is 14.7 psi (101.3 kPa). For calculating any atmospheric pressure within the troposphere (from the surface of the earth up to an altitude of about 12 miles or 20 km.) use this simple formula [3] Figure 1.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Where the Constant Parameters are as Described Below

This ability to calculate the atmospheric pressure can quite accurately help with treatment of the patient, however we will repeat this several times, the single most important treatment is to evacuate the patient down the mountain.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What are the treatments for AMS?w
It is better to prevent acute mountain sickness than to try and treat it! The patient needs to follow the “Golden Rule of Mountaineering” and ascend slowly, which will give their body time to acclimatize as they ascend. They will be less likely to develop AMS. If a back packer has been climbing for any amount of time, they will see the most experienced (and smartest) mountaineers climbing at a SLOW, steady pace. This is not because they are old and decrepit, this is because they are smart and are slowly acclimatizing to the increase in altitude. However, if a mountaineer needs to go up more quickly, they could consider taking a drug called acetazolamide (also known as Diamox). Acetazolamide is a carbonic anhydrase inhibitor that is used for the medical treatment of glaucoma, epileptic seizures, idiopathic intracranial hypertension, altitude sickness, cystinuria (a rare condition in which stones made from an amino acid called cysteine form in the kidney, ureter, and bladder), periodic paralysis, central sleep apnea and dural ectasia (a widening of the dural sac surrounding the spinal cord).There is now good evidence that acetazolamide reduces symptoms of AMS in trekkers and mountaineers, although it may have some unusual side-effects such as causing the extremities to tingle or food, especially fluids, taste strange.
As with any of the three forms of altitude sickness, if the patient has acute mountain sickness, the best treatment is descent. Painkillers may ease the headache, but they will not treat the condition. Acetaminophen (Paracetamol) is the safest, avoid these pain killers if they have codeine in them, as there are no definitive studies on the effect of codeine on AMS. The patient may be extremely thirsty, however increasing fluid intake should be done with caution, as an increased intravascular volume can exacerbate HAPE and HACE. If possible, a 22 Gauge (25 mm.) I.V. Catheter (Venflon®) should be securely placed and either flushed with heparin and capped off or if a long transport down the mountain is expected in a Gamow Bag or on a stretcher, you can give 0.9% Normal Saline at a TKO (To Keep Open) rate or D5W, also at a TKO rate. Avoid colloids because again, the effects of colloids on the brain in HACE have not been extensively studied. Acetazolamide may be helpful, especially if the patient needs to stay at the same altitude. DO NOT however delay descending with the patient in order to place an I.V. Catheter. The priority is to get the patient to descend as rapidly as possible and the patient should be strongly encouraged to descend, regardless of the reason they need to stay up high, as they may rapidly develop HAPE or HACE and die. Resting for a day or two at a lower altitude might give their body time to acclimate and then they can attempt to increase their altitude again, but even slower than before. It is not clearly understood why, but once a patient has had AMS, they are more susceptible to reoccurrences. It is essential that the patient should NEVER go up higher, instead of lower, if they have AMS as they will exacerbate the symptoms and risk rapidly progressing to HAPE or HACE. This triad always has to be thought of concomitantly during the treatment of anyone with the initial symptoms of AMS.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
The Golden Rules of AMS to tell Patients
- If you feel unwell, you have altitude sickness until proven otherwise
- Do not ascend further if you have any symptoms of altitude sickness
- If you are getting worse then descend immediately
- Do not descend alone, you don’t know what may happen
- Don’t die of altitude sickness.
Every year, people die of altitude sickness. All of these deaths are preventable. If the person is travelling above 2500 meters (8200 feet), this information could save their life.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What causes altitude sickness?
Two things are certain to make altitude sickness very likely - ascending faster than 500 meters = 1,965 feet) per day and exercising vigorously (ie: backpacking). Physically fit individuals are not protected – even Olympic athletes get altitude sickness. Altitude sickness happens because there is less oxygen in the air that you are breathing at high altitudes.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Altitude Sickness Prevention
Gain altitude slowly, take it easy and give your body time to get used to the altitude. The body has an amazing ability to acclimatize to altitude, but it needs time. For instance, it takes about a week to adapt to an altitude of 5000 meters (16,404 feet), two weeks is better. When these two authors hiked up to “Base Camp Everest South”(28°0′26″N 86°51′34″E) (5364 meters = 17,598 feet) they took two weeks of slow backpacking from Kathmandu to Base Camp Everest South. To save time and energy before beginning the trek to Everest Base Camp, it is possible to take a plane to Lukla, but not recommended by these doctors due to the sudden increase in altitude. Nevertheless, the two authors of this article trekked from Kathmandu 1,400 meters (4,620 ft.) to Lukla at 2,843 meters (9,383 ft.) and rested overnight. From Lukla, they trekked upwards to the City of Namche Bazaar, which is often called the Sherpa Capital of Nepal because this is where most Everest Expeditions hire their Sherpas and get supplies. Namche Bazaar is situated at 3,440 meters (11,286 ft), following the Valley of the Dudh Kosi River. It took about two days of easy hiking to reach this village, which is a central hub of the area and full of wonderful local people. Typically at this point, climbers allow another day of rest for acclimatization, which the two authors did. When the locals found out we were doctors, they came to us with every ailment imaginable – but it was a wonderful experience and these terribly poor people paid us in some of the most wonderful food we have ever eaten and their magnificent company. The children were an absolute joy and they could not believe that a father and daughter doctor team actually existed. I don’t think we cooked a single meal in any of the towns we stopped in due to the wonderful generosity of the Nepalese People. We then trekked another two days to Dingboche at 4,260 meters (13,976 ft.) before resting for another day for further acclimatization. Another two days took us to Everest Base CampSouth (5364 meters = 17,598 feet) via Gorakshep, the flat field below Kala Patthar, 5,545 meters (18,192 ft) and Mt. Pumori. The reason we relate our personal trek into veryhigh altitudes is because neither one of us suffered from any kind of AMS, one of us is past 40 and the other is in her 20’s! If you just fly in, you miss the beauty of the countryside, the incredible people of Nepal, their hospitality and their incredible love of life and nature and you are at a very high risk of AMS!!
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Introduction And Facts Regarding HAPE
HAPE stands for High Altitude Pulmonary Edema and this termsimply means “excess fluid accumulation in the lungs”. Everyone who travels to high altitude should know about this triad (AMS, HAPE, HACE) and the fact that death can result rapidly from these disorders, do not ignore the symptoms!
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
High Altitude Pulmonary Edema (HAPE)
HAPE is a dangerous build-up of fluid in the lungs that prevents the alveoli from opening up and filling with fresh air with each breath. When this happens, the patient becomes progressively more and more short of oxygen, which in turn worsens the build-up of fluid in the lungs. In this way, HAPE can be fatal within hours.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What are the Symptoms?
HAPE usually develops after 2 or 3 days at altitudes above 2500 meters (8,202 feet). Typically the sufferer will be more breathless compared to those around them, especially on exertion. Most patients will have symptoms of acute mountain sickness. Often, they will have a cough and this may produce a white or pink frothy sputum. The breathlessness will progress and soon they will be breathless even at rest. Heart rate may exhibit tachypnea, the lips may be cyanotic and the body temperature may be elevated. It is easy to confuse symptoms of HAPE with a chest infection, but at altitude HAPE must be suspected as your primary differential and the affected individual must be evacuated to a lower altitude immediately, preferably accompanied by the highest ranking medical person by education(in order of preference: physician, nurse or paramedic) on the mountain.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Who gets HAPE?
Unfortunately, it is currently impossible to predict who will get HAPE. People who have had HAPE before are much more likely to get it again. Therefore, there must be some factor that puts certain individuals at high risk of the condition. However, just like acute mountain sickness, there are some known risk factors. A fast rate of ascent and the altitude attained will make HAPE more likely. Vigorous exercise is also thought to make HAPE more likely and anecdotal evidence suggests that people with chest infections, symptoms of a common cold before ascent or smokers [1] may be at higher risk. One very good axiom to follow is to “climb high, sleep low” (Obrowski, M.H. – Denali – 1986 – unpublished). What this basically means that if you are attempting to climb a high mountain in stages (such as Denali, formerly known as Mt .McKinley – (5,190 meters or 20,310 feet), climb as high as you can on whatever number day you are on, establish a camp and then go down AT LEAST 150 to 200 meters (492 to 656 feet) to sleep – you will sleep better and exponentially reduce your chances of trying to sleep through a miserable night. You will also feel much better in the morning. In addition, while climbing, all experienced backpackers know they should hike/climb for 45 minutes of every hour and take a break for 15 minutes – giving the body a rest break helps with acclimatization. Whenever you take a break and feel the slightest symptoms of AMS, HAPE or HACE, come down immediately at least 150 meters (482 feet). As Mountaineering Physicians who run a non-profit wilderness organization (www. wildernessphysicians.org) for the past twenty years, we have recovered many dead “macho men” off of a mountain or simply had to leave them there as eternal popsicles to remind other climbers of what not to do!! No organization, including ours, will EVER risk the lives of their Rescue Physicians, Rescue Teamsor Search and Rescue Dogs to drag a corpse off a mountain – this is the brutal reality of High Altitude Mountaineering!!
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What Causes HAPE?
Despite years of careful research the exact causes of HAPE remain poorly understood. Fluid has been shown to fill up the alveoli in the lungs preventing oxygen getting into the blood and causing the vicious circle of events that can kill people with HAPE. As with many biological processes, many factors play a role in this condition and there is good evidence to support a number of theories about how this fluid accumulates in the lungs.
Normally, oxygen gets into your blood and is supplied to the body from your lungs. Each time you take a breath in, air rushes into the tiny alveoli at the end of all the bronchioles in your lungs. At the same time, blood from your heart is brought close to these thin-walled alveoli so that oxygen can move into your blood while waste products move out. Oxygen-rich blood then returns to the heart and is distributed to the body. If, by accident, a person inhaled a small object into their lungs, it would become stuck in one of the airways branches. Little oxygen would get to the downstream alveoli. To prevent this area of lung supplying blood starved of oxygen back to the heart (and therefore the rest of body), blood vessels in this area will constrict, self-protecting the body.
At high altitudes however, this same process occurs and is a cause of the disorder HAPE. The entire lung is starved of oxygen and therefore the entire lung reacts in the same way – blood vessels start constricting everywhere within the lung and not just in small areas. The blood in these vessels is constricted and the pressure goes up, the permeability of the vascular endothelium increases and fluid is forced out of the blood and into the alveoli. Reactive Oxygen Species (ROS) are formed in your blood when a patient is starved of oxygen. Some of these highly damaging molecules are produced as follows: The reduction of molecular oxygen (O2) produces Superoxide (•O2−); Dismutation of Superoxide produces Hydrogen Peroxide (H2O2); H2O2 in turn may be partially reduced to a hydroxyl radical (•OH) or fully reduced to water (H2O), which fills the alveoli. The hydroxyl radical is so extremely reactive that it immediately removes electrons from any molecule nearby, turning that molecule into a free radical and so propagating a chain reaction.These highly reactive molecules can directly damage the alveolar membranes between the air and blood in the lungs, causing further fluid leakage into the alveoli and worsening HAPE.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
How is HAPE Treated??
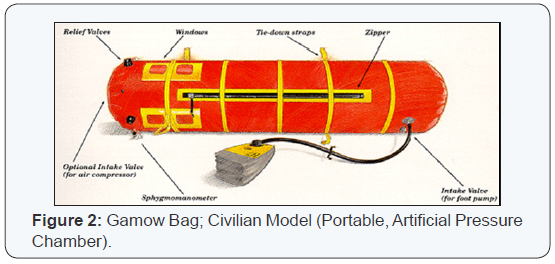
The most important treatment for HAPE is descent. Providing extra oxygen and/or raising the air pressure around a victim with a Gamow Bag (Figure 2) can partially reverse the underlying process, lack of oxygen, but these measures are not a permanent substitute for rapid descent down the mountain. The patient is placed in a sleeping bag and then inside the Gamow Bag. The foot pump is used to increase the internal pressure of the bag and this in effect lowers the “altitude” that the patient is experiencing. There is also a port that allows oxygen to be connected and insufflated, helping increase the patient’s pO2. Again, the patient still has to be rapidly moved down the mountain as there is no way for a physician to physically touch the patient and treat him/her. The Gamow Bag is a temporary, although extremely effective adjunct.
The primary author of this paper has personally seen the Gamow Bag actually save the life of a patient on top of California’s highest peak, Mount Whitney (14,505 ft. or 4,395 meters). This author climbed Mt. Whitney with his Rottweiler in about 8 hours and when he got to the top, there was a massive commotion going on. A patient had literally dropped unconscious at the summit, but unfortunately he was the group’s paramedic and was totally unresponsive. The author took over and by the basic history he could gather from the hysterical group, the patient had either HAPE or HACE, although the author suspected HACE, due to the rapid deterioration and unconsciousness. The author found that they actually had a packaged, brand new Gamow Bag in their medical supplies, but no one even knew what it was. We placed the paramedic-victim in a sleeping bag, then into the Gamow Bag; pressurized the Gamow Bagand hooked up the Rottweiler by her harness to the bag. The dog dragged the patient all the way down to a road that went about ⅓ of the way up the mountain, for people that didn’t want to climb the mountain from the base. (This was the problem, a relatively small climb on a high mountain with absolutely no acclimatization). These people had all their vehicles there but were from a different state, so we took one of the trucks with the patient, the author and the Rottweiler in the back and we took the patient to the nearest hospital, about a two hour drive at 100 mph (161 kph). In the meantime, the author had opened the Gamow Bag, started an I.V. TKO and eventually the patient made a full recovery. No drugs were available as this was the paramedics’ personal medical kit and paramedics in California are not allowed to possess or give any drugs without a direct order from a physician. The Gamow Bag saved his life for sure and is one of the best investments a mountaineering group can make. Current 2016 pricing: $2,110; €1,942; £1,465.
Some drugs can be helpful, but should only be used by trained doctors, there for no dosing will be provided here as this article can be read by anyone. Nifedipine is a drug that helps to open up the blood vessels in the lungs. By doing so, it reduces the high pressure in those vessels that is forcing fluid out into the lungs. Following recent research, physicians may also give the steroid, dexamethasone. Drug treatment should only ever be used as a temporary measure; the best treatment is descent.
HAPE also causes breathlessness due the increased fluid in the lungs. It is never normal to feel breathless when you are resting - even on the summit of Everest. This should be taken as a sign that the patient has HAPE and may die soon. HAPE can also cause a fever and coughing up frothy, bloody sputum. HAPE remains the major cause of death related to highaltitude exposure with a high mortality in absence of adequate emergency treatment.
Physiological and symptomatic changes often vary according to the altitude involved. The Lake Louise Consensus Definition for High Altitude Pulmonary Edema [4] has set widely-used criteria for defining HAPE symptoms.
- The patient should have at least two symptoms [5]:
- Dyspnea at rest
- Cough
- Weakness or decreased exercise performance
- Chest Congestion
- The patient should have at least two signs [5]:
- Crackles or wheezing in at least one lung field
- Central Cyanosis
- Tachypnea
- d.Tachycardia
- Intermediate Altitudes (1,500 – 2,500 meters or 4,950 – 8,250 feet)
- Clinical symptoms are unlikely
- Blood oxygen levels remain >90%
- Clinical symptoms are common
- May develop after 2 to 3 days
- Blood oxygen levels may drop below 90% or lower during exercise
- Prior acclimatization will decrease the severity of the symptoms.
- Extreme Altitude (>5800 meters or 19140 feet)
- Blood oxygen levels are <90%, even at rest
- Progressive deterioration may occur despite acclimatization
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Introduction and Facts Regarding HACE
If a travelling companion has symptoms of acute mountain sickness and becomes confused or unsteady or develops an extremely severe headache or vomiting, they may have the life-threatening condition called High Altitude Cerebral Edema (HACE).
There are many remedies touted as treatments or “cures” for altitude sickness, but there is no evidence to support any of them. The only chance the patient has is IMMEDIATE evacuation to as low an altitude as possible. Put the patient in a Gamow Bag if one is available.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
General Facts Regarding HACE
HACE is high altitude cerebral edema and is a build-up of fluid on the brain. HACE is extremely life-threatening and requires urgent action.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What are the Symptoms?
HACE is the most severe form of acute mountain sickness [6]. A severe headache, vomiting and lethargy will progress to unsteadiness, confusion, drowsiness and ultimately a coma. Drowsiness and loss of consciousness occur shortly before death. HACE can kill in only a few hours, so the treating person must act immediately. If you wait a “few hours” until it is light enough to see, the patient will either die waiting to be evacuated or shortly thereafter. A person with HACE will find it difficult to walk heelto- toe in a straight line (ataxia) – this is a useful test to perform on someone with severe symptoms of acute mountain sickness. HACE should also be suspected if a companion starts to behave irrationally or bizarrely. Protect the patient from hurting him or herself by removing or hiding anything sharp or dangerous objects (such as climbing axes) or weapons.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Who gets HACE?
About 1% of people who ascend to over 3,000meters (9,900 ft.) get HACE. The lowest altitude at which a case of HACE has been reported was 2,100meters (6,930 ft.). HACE can also occur in people with HAPE and vice versa. Factors that increase the risk of HACE are similar to those for acute mountain sickness and HAPE. The faster the rate of ascent and the higher the altitude, the more likely it is that HACE will develop. HACE is thought to occur mainly in trekkers or climbers who have ignored symptoms of acute mountain sickness and continued climbing higher rather than staying at the same altitude or descending.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
What causes HACE?
The cause of HACE, like HAPE, remains unknown. Several factors may play a role including increased blood flow to the brain. An increase in blood flow is a normal response to low oxygen levels in the brain as the body needs to maintain a constant supply of oxygen to the brain. However, if the blood vessels in the brain are damaged, fluid may leak out of the vessels [7] and cause HACE. The skull is an immobile encasement designed to protect the brain, but any additional fluid will increase intracranial pressure, contributing to HACE and in the extreme, causing an Uncal Herniation (a subtype of transtentorial downward brain herniation) and instant death.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
How is HACE Treated?
As mentioned before, HAPE and HACE often occur together, so as the treating physician, do not waste time trying to ascertain which one the patient has, just get the patient evacuated to a lower altitude as soon as possible.
Again, as with HAPE, rapid descent is the most effective treatment of HACE and should not be delayed if HACE is suspected. A Gamow Bag (Portable Pressure Chamber - Figure 2), can be used as a temporary measure and, if available, oxygen and a drug called dexamethasone should be given, but only by a physician [8].
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Quick Summary and Conclusion
Altitude sickness occurs when an individual who is accustomed to low altitudes rapidly climbs to a high altitude [8]. Altitude sickness is a potentially lethal complication of climbing to altitudes above 8,000 feet (2,425 meters) [9-11]. Three main syndromes of altitude illness may affect travelers: Acute Mountain Sickness (AMS), High Altitude Pulmonary Edema (HAPE) and High Altitude Cerebral Edema (HACE). The risk of dying from altitude related illnesses is low, at least for tourists. For trekkers to Nepal the death rate from all causes was 0.014% and from altitude illness 0.0036%, soldiers posted to altitude had an altitude related death rate of 0.16%.
Treatment of altitude related illness is to stop further ascent and if symptoms are severe or getting worse, to descend immediately! DO NOT DELAY!! Oxygen, drugs, Gamow Bags and other treatments for altitude illness should be viewed as adjuncts to aid descent, NOT AS PRIMARY TREATMENTS!
The Death Zone is the name used by mountain climbers for high altitude where there is not enough oxygen for humans to breathe. This is usually above 8,000 meters (26,400 feet). Most of the 200+ climbers who have died on Mount Everest have died in the death zone.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
Quick Summary and Conclusion
No human patients were used in the development and writeup of this paper.
- Research Articlet
- Abstract
- Introduction and Facts Regarding AMS
- What are Other Names for AMS?
- How are the Symptoms of AMS Recognized?
- Who gets AMS?
- What Causes Altitude Sickness?
- Where the Constant Parameters are as Described Below
- What are the treatments for AMS?
- The Golden Rules of AMS to tell Patients
- What causes altitude sickness?
- Altitude Sickness Prevention
- Introduction And Facts Regarding HAPE
- High Altitude Pulmonary Edema (HAPE)
- What are the Symptoms?
- Who gets HAPE?
- What Causes HAPE?
- How is HAPE Treated?
- Introduction and Facts Regarding HACE
- General Facts Regarding HACE
- What are the Symptoms?
- Who gets HACE?
- What causes HACE?
- How is HACE Treated?
- Quick Summary and Conclusion
- Human Studies
- References
References
- Machowicz R, Ciechanska J, Zycinska K, Mahboobi N, Wnekowicz E, et al. (2013) Medical Students Attitude Toward Smoking in Warsaw, Strasbourg, and Teheran. Adv Exp Med Biol 755: 195-202..
- Tadeusz Z, Michael O, Bychawsk M, Bialas B, Zycinska K, et al. (2013) The Influence of Sera from Interstitial Lung Disease Patients on Human Mononuclear Cell Production of VEGF and bFGF. Adv Exp Med Biol 756: 139-145.
- A quick derivation relating altitude to air pressure. Portland State Aerospace Society (2004) accessed 05-03-2015.
- http://www.high-altitude-medicine.com/AMS-LakeLouise.html
- Zielonka TM, Demkow U, Radzikowska E, Bialas B, Filewska M, et al. (2010) Angiogenic Activity of Sera from Interstitial Lung Disease Patients in Relation to Pulmonary Function. Eur J Med Res 15 (Suppl 2): 229-234.
- Baillie JK, Thompson AA, Irving JB, Bates MG, Sutherland AI, et al. (2009) Oral antioxidant supplementation does not prevent acute mountain sickness: double blind, randomized placebo-controlled trial. QJM 102(5): 341-348.
- Zielonka TM, Zycinska K, Chorostowska-Wynimko J, Filewska M, Bialas B, et al. (2013) Angiogenic Activity of Sera from Interstitial Lung Disease Patients in Relation to Angiotensin-Converting Enzyme Activity. Published in the book: Respiratory Regulation: The Molecular Approach. Chapter 27, 756: 213-221. Dordrecht [u.a.]: Springer.
- Hackett P, Roach RC (2004) High altitude cerebral edema. HAMB 5(2): 136-146.
- Barry PW, Pollard AJ (2003) Altitude Illness. BMJ 326(7395): 915-919.
- Zielonka TM, Demkow U, Michalowska-Mitczuk D, Filewska M, Bialas B, et al. (2011) Angiogenic Activity of Sera from Pulmonary Tuberculosis Patients in Relation to IL-12p40 and TNFα Serum Levels. Lung 189(4): 351-357.
- Reynolds K (2006) Everest - A Trekker’s Guide. Cicerone Press Limited. 230-231.






























