The harm of Cigarettes and E-cigarettes on respiratory human airway smooth muscles (HASMC), normal human bronchial epithelial cells (NHBE) & whether it can lead to the development of Chronic Obstructive Pulmonary Disease (COPD).
Wael Alshehri1, Dr. Mohammed E Alarifi2, Mohammed Alasmary3 and Mohammed Al- alhuwayshil4
King Saud University, Saudi Arabia
Submission: May 26, 2022; Published:July 17, 2022
*Corresponding author:Wael Alshehri, King Saud University, Saudi Arabia
How to cite this article:Mr Wael Alshehri. The harm of Cigarettes and E-cigarettes on respiratory human airway smooth muscles (HASMC), normal human bronchial epithelial cells (NHBE) & whether it can lead to the development of Chronic Obstructive Pulmonary Disease (COPD). Int J Cell Sci & Mol Biol. 2022; 7(2): 555709. DOI: 10.19080/IJCSMB.2022.07.555709
Abstract
Chronic obstructive pulmonary disease (COPD) is a disease that characterized by the inflammatory response to inhaled particles like cigarette smoke. It is known that cigarette smoke stimulates the production of the inflammatory cytokines and chemokines from respiratory system. It has been linked that the overproduction of the mucus with COPD patients to cigarette smoke. On the other hand, the e-cigarettes made to aid smoking cessation, but it has presented with a pro-inflammatory effect. However, the production of cytokines and chemokines due to the use of e-cigarette is under investigation in order to present the haram. It is widely known that cigarette smoke induced airway inflammation. We aim to compare both cigarette and e-cigarette on the production of the inflammatory cytokines and chemokines from human airway smooth muscles (HASMC), normal bronchial epithelial cells (NHBE) and whether it can lead to the development of (COPD).
Hypothesis: The claim is that cigarette smoke effect similarly like e-cigarette vape on airways smooth muscles and bronchial epithelial cells that may lead to the production of the cytokines and chemokines. Both cigarette smoke and E-cigarette contribute to the development of Chronic Obstructive Pulmonary Disease (COPD).
Method: A systemic literature review was conducted using PubMed and European respiratory journal to determine the prevalence of cigarette and e-cigarette on airways. The study compared the effect of cigarette and e-cigarette with and without nicotine between different studies. The assessment of the harm of both cigarette and e-cigarette on airways smooth muscles and bronchial epithelial cells.
Result: Among 108 studies, we found that 10 studies with relevant content to the search. E-cigarette can be harmful to airway and unsafe as it showed an effect on both HASMC& NHBE. E-cigarette has smiler effect to cigarette smoke that identified on search.
Conclusion: Cigarette smoke like e-cigarette share a similarity on the production of cytokines and chemokines from airway and lung & may contribute to the development of Chronic Obstructive Pulmonary Disease (COPD).
Keywords: Chronic obstructive pulmonary disease; Cigarette smoke; bronchial epithelial cells; Airway smooth muscles; inflammation
Abbreviations: COPD: Chronic Obstructive Pulmonary Disease; ROS: Reactive Oxygen Species; CS: Cigarette smoke; FDA: Food and Drug Administration; BALF: Bronchoalveolar Lavage Fluid VEGF: Vascular Endothelial Growth Factor
Introduction
Chronic obstructive pulmonary disease (COPD) is a ‘’preventable and treatable disease that is characterized by persistent respiratory symptoms and airflow limitation that is due to airway and/or alveolar abnormalities usually caused by significant exposure to noxious particles or gases’’ [1]. It is known as severe chronic lung disease that is presented in later life, mainly caused by cigarette smoking, that recognized by symptoms such as a chronic cough, shortness of breath (dyspnea), frequent respiratory infections, cyanosis, fatigue, production of large amounts of phlegm, sputum and wheezing [2,3]. With the disease progression, there is a decrease in the lung compliance (elasticity) which is resulting in increased effort to exhale the air and a reduction of the expiratory air volume (FEV1) [1].
The observational cost with higher number of people being diagnosed with COPD, the cost of healthcare associated with the management, hospitalizations and maintenance is constantly increasing. The additional cost associated with the treatment of moderate to severe exacerbation attacks also imposes a financial burden on the countries. On the burden of COPD, there were 3.17 million COPD-related deaths worldwide in 2015, representing 5% of all deaths globally [4]. It has been determined that the rising costs are primarily due to the increasing number of people who are diagnosed with COPD. The United States alone were $32.1 billion in 2010 with a projected to $49.0 billion by 2020 [5]. On the other hand, England estimated that cost of COPD which projected to increase from £1.50 billion in 2011 to about £2.32 billion by 2030 and from £159 million in 2011 to £207 million in Scotland by 2030 [6].
Pathogenesis of COPD
Chronic inflammation has been shown to play a very important role in the pathogenesis of COPD. The disease causes airflow limitation and results in loss of lung elastic recoil which limits the flow to airways, obstruction of the lumen that leads to increase resistance in the airway and increase secretions [7]. COPD is involving in inflammatory cells such as neutrophils, macrophages and lymphocytes. Various studies have identified neutrophil infiltration as one of the most common findings in the pulmonary tissue of COPD patients. A cohort study demonstrated an increased localization of neutrophils within the bronchial glands and epithelium of COPD patients as opposed to the bronchial samples collected from non-COPD patients [8]. Extent of neutrophil infiltration has been associated with the severity of pulmonary dysfunction in COPD patients. The Hallmark features of disease is (airway obstruction and chronic expectoration) and reduction in the FEV1 levels with direct proportional to the number of neutrophils within the sputum of COPD patients.
In addition, neutrophilic inflammation of the lung plays a critical role in the pathogenesis of COPD [9,10]. Furthermore, there are some of the clinical manifestations of COPD. Chronic bronchitis that is known as a condition of large airways inflammation, and emphysema, a disease of distal airways and parenchyma that results in 16 destruction of the airway wall and reduces the maximal expiratory airflow by reducing the elastic recoil force [6]. Also, chronic bronchitis involves the rate of coughing and production of sputum. It is characterized by the decline in lung function, development of airway obstruction and frequency of exacerbation, wheezing, cough and dyspnea [11]. Hypersecretion of mucus and cough resulted of mucus gland enlargement [12]. The changes of airway structural with chronic bronchitis involve atrophy, focal squamous metaplasia, abnormalities of epithelial cilia, bronchial wall thickening goblet cell metaplasia and smooth muscle hyperplasia [12].
This chronic condition is presented by the reduction in the FEV1 [10]. Various studies showed that skin natural change to aging features with COPD patients [13,14]. Pulmonary emphysema has a significant difference in skin elasticity which presented with lower skin elasticity compared to others without emphysema [15]. It is known to present with airway wall distraction or constriction which causes the distal airspaces to grow in size in a disproportional and potentially damaging way [16]. The other secondary effect lead to COPD is the oxidative stress and reactive oxygen species (ROS) that play a role in lung inflammation and increase the alveolar destruction involved in the inflammatory process in the lungs [17]. The oxidants in cigarette smoke lead to the increase inflammation in the lung [18]. The oxidative stress activated neutrophils, macrophages and epithelial due cigarette smoke [18].
Cigarette Smoke and Airway Inflammation
Cigarette smoke (CS) has a link of association with chronic airway inflammation, which may eventually lead to COPD development [1]. CS is composed of multiple type of dangerous chemicals that are considered to be harmful to the lung such as acrolein, nicotine, carbon monoxide, ROS, acetaldehyde, ammonia and other dangerous chemicals [19]. The multiple chemicals in cigarette smoke associated directly or indirectly to the addiction of cigarette smoke [19]. In addition to that, the overproduction of the mucus with COPD patients is linked to cigarette smoke [20]. The mechanism of Losing cough up to phlegm in the airway and lung is due to damage to cilia with chronic inflammation which leads to the accumulation of the excessive volume of secretions [20]. An in vitro study on the effect of cigarette smoke on airway inflammation presented that T cells, macrophages, neutrophils and mast cells are elevated with patients whether they are current smokers or ex-smokers [21].
Cigarette smoke increased chemotaxis of neutrophils in response to IL-8 in smokers with and without COPD. That is an evidence of cigarette smoke linked to the association with systemic activation of neutrophils irrespective of the degree of COPD pathology [22]. Smoking cessation serve as the ultimate solution to slow down the progression of COPD disease. It has been demonstrated that lung function in smokers showed significant improvement within 1 year of smoking cessation. The FEV1 improved and observed reduction in the expectorant coughing in people after a year of smoking cessation [23]. However, these studies present cigarette smoke haram and implement role in airway inflammation by inducing inflammatory gene expression from different cells.
E-cigarette vapor and inflammation
E-cigarettes are battery-powered devices that work by heating liquid and vaporizing it by inhalation [24]. The components of E-liquid used in the-cigarettes are a mixture of propylene glycol, glycerin, nicotine and flavors. Currently the e-cigarettes are classified with disposable or reusable as per the manufacture. The disposable devises are not rechargeable and not refillable, whereas the reusable one is rechargeable and can be refillable with e-liquid. As an advantage some of the users with e-cigarettes can control and adjust the voltage supplied to heating coil, temperature, and air flow rate of puffing [25]. E-liquid with / without nicotine may contain with flavoring substance that made the reason for the e-cigarettes being popular for the users.
Food and Drug Administration (FDA) deemed those components of E-liquid as a toxic for lungs similar to tobacco cigarettes [26]. Exposure of e-cigarette vapor contains propylene glycol (PG) which may cause irritation to the upper airway with non-smoker [26]. When particles of (PG) and vegetable glycerin (VG) heated it can be converted to acrolein, formaldehyde and acetaldehyde, which are known as strong irritants and stimulate inflammation in the lung [27]. Wu Q, and his group provided evidence that concluded e-cigarette vapour exposure without nicotine induced the release of IL-6 on the healthy human airway epithelial cells of non-smokers [26]. On the other hand, the exposure of e-cigarette fluid with nicotine to mice for 4 months period had a significant increase in the levels of MCP-1, CXCL- 10, IL-6 and CXCL-2 found in the Bronchoalveolar lavage fluid (BALF) [28]. The flavor of cinnamon on electronic cigarette refill fluids presented the most cytotoxic effect compared to other 36 flavours tested on human embryonic stem cells and human adult pulmonary fibroblasts [29]. Therefore, electronic cigarettes are harmful to the lungs by producing the inflammatory mediators from different cells.
Method
Given the importance awareness of the effect of cigarette and e-cigarette, the research conducted a systematic literature review to determine the prevalence of the harm in cigarette and e-cigarette that can lead to the development of COPD. The literature search used PubMed and European respiratory journal for the manuscripts published from 2000 up to date. Among the search, a scan of 108 articles were done and 50 of it was excluded (n=50). This number of 50 records were excluded because it was either before the year of 2000 or not relevant to the subject (n=50). Before the screening is processed, we removed 20 of the duplicate’s records (n=20). However, among these reports we assessed 20 studies that is eligible to our topic (n=20). We have then excluded the studies that has no relevant and association with airway inflammation or may the inflammation has occurred with other cells (n = 10) (Figure 1).
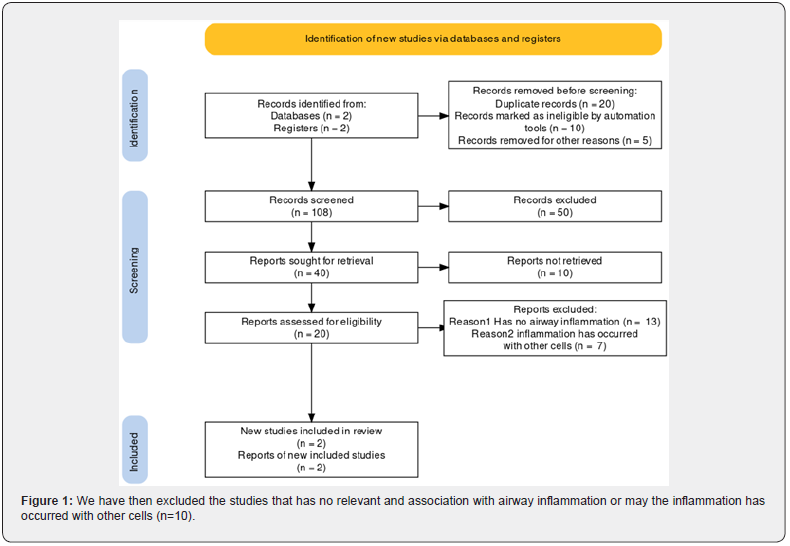
The abstracts were scanned for the relevant search method (effect of cigarette and e-cigarette on airway smooth muscle and normal bronchial epithelial cells. Containing data from a clinical trial on the prevalence effect of cigarette and e-cigarette on airway smooth muscles and bronchial epithelial cells. In the search scan the points were focusing on effect of Cigarette and e-cigarette on airway smooth muscles, bronchial epithelial cell and lung Cytokine chemokine predication. Also, assess E-cigarette liquid if it can increase airway inflammation like cigarette smoke which lead to the development of COPD. Moreover, in this method, the focus of the harm e-cigarette effect of secondhand vapor and compare it to cigarette smoke. Most importantly, in this literature search is to find out the side effect and harm of e-cigarette with/without (flavor- nicotine) on the human airways. It has been noticing that multiple types of the flavor of E-cigarette that can be vaping and need to find out if it safe on the respiratory airway smooth muscles, bronchial epithelial cells. The study compared the side effect of these harm by categorizing the inclusion and exclusion criteria for the effect of Cigarettes and E-cigarettes side effect on respiratory airway smooth muscles, bronchial epithelial cells that illustrate as the following (Table 1).
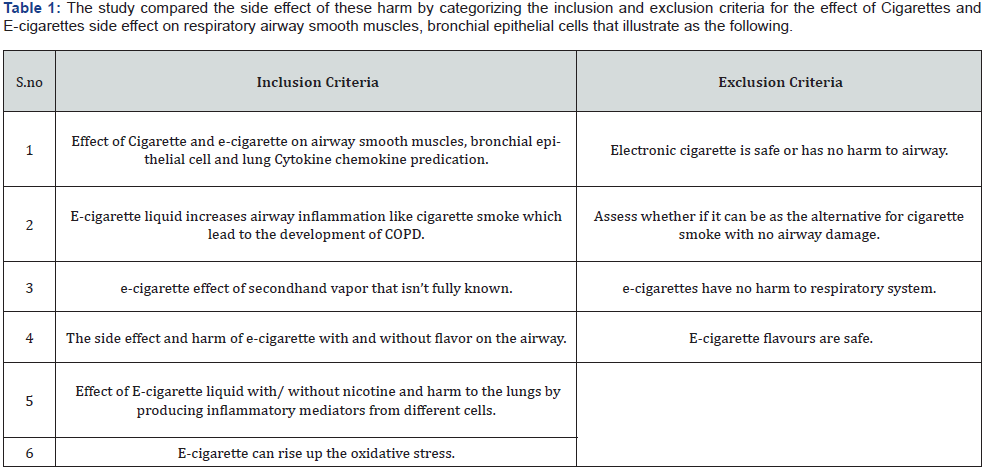
Results
To assess the effect of cigarette and e-cigarette on airway, studies in the search were identified form PubMed. Of 108 articles identified 10 studies that have relevant content to the search. The prevalence of cigarette and e-cigarette in the individual studies is summarized in the table below. The comparison of the studies on the search was assessing the impact haram of cigarette smoke and e-cigarette liquid exposure to HASM, HBEC & whether e-cigarette can cause the same effect as it has been showing on cigarette smoke. Among these studies were using the type of e-cigarettes that include both PG:VG (50%/50%), whereas cigarette smoke used some commercial type and others used research-grade cigarettes depend on the study protocol. Some studies on the search pointed out the cytotoxic effect of the cells due to either vape or smoke exposure. Also, it has been found that e-liquid without nicotine caused toxicity attributed with flavoring type of e-liquid on the cells. Interestingly there was direct effect of e-cigarette smiler to cigarette smoke that identified on some of the studies.
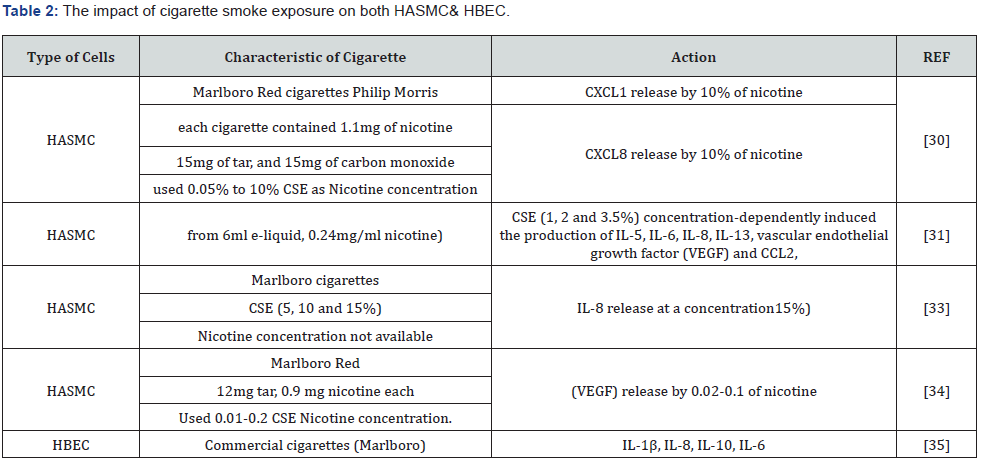
The cigarette smoke CSE increased the release of CXCL8 and CXCL1 from human airway smooth macules cells, and cells from smokers with COPD produced more CSE-induced CXCL1 [30]. Others demonstrated the effect of cigarette smoke on airway smooth muscles cells. CSE (1,2 and 3.5%) induced the production of IL-5, IL-6, IL-8, IL-13, vascular endothelial growth factor (VEGF) and CCL2, but not CXCL-10 and RANTES [31]. Unlike the e-cigarette without nicotine (from 6ml e-liquid, 0.24mg/ml nicotine) was using the e-liquid on the HASMC as the following percentage (1, 2.5 and 5%) which only significantly induced the production of IL-13 from HASMC [31]. Whereas the impact of exposure to e-cigarette vapor Nicotine: 24 mg/mL on NHBE cells induced cell viability and rise up the oxidative stress [32]. Therefore, e-cigarette showed toxicity to the cells and cannot be a good method of smoking cessation as it contributes to the rising up of oxidative stress (Table 2 & 3) [33-39].
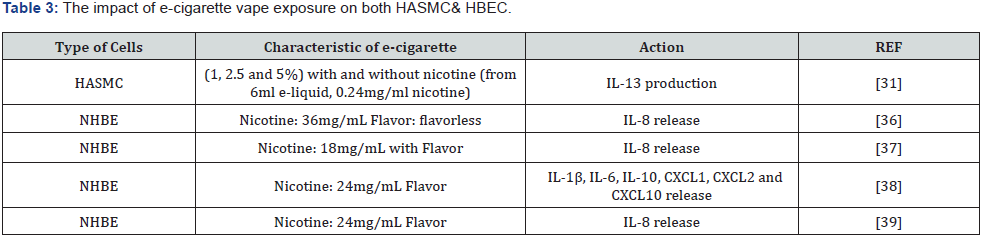
There was a strong association between cigarette and the development of COPD disease. Hermanowicz-Salamon showed that IL-6 and IL-13 induced sputum of COPD [40]. In addition, there was a link between the elevation of IL-13 and COPD [41]. Also, the chemokines GROalpha and MCP-1 levels Increased in sputum samples from patients with COPD [42]. That’s all can present clear evidence that cigarette smoke lead to the development of COPD & proved by the effect of the release of cytokines and chemokines. On the other hand, E-cigarette is harmful with/without nicotine on the lung. Their release of cytokine IL-13 from HASMC [31]is one of the evidences that clearly has an effect of the respiratory side. Moreover, flavor e-cigarette with different nicotine concertation exposure to NHBE release IL-8, IL-1β, IL-6, IL-10, CXCL1, CXCL2 and CXCL10 [43-46]. Vaping aerosol contains several dangerous chemicals components that may increase the risk of inflammation like formaldehyde and other airway irritants. In addition to that, vaping could be harmful especially to infants and children as second hand vape. Unfortunately, the harm of long-term effect of e-cigarette on others as second hand still unknown. Therefore, E-cigarette can be harmful and unsafe as it showed with the production of cytokines and chemokines from both HASMC& NHBE.
Discussion
Cigarette smoke caused a huge burden on public health costly on the treatment and care. On the other hand, E-cigarettes vaping has a direct cause on respiratory ways and may trigger lung disease. COPD in the United State is the 4th leading cause of death whereas cigarette smoke is the main leading cause [47]. The CDS showed that COPD are affecting 15 million people at USA, whereas 150000 Americans die of COPD each year. The second most common lung disease in the UK is COPD which conduct 2% of whole population,4.5% of all people aged over 40 live with COPD [48]. However, in Europe, the estimate case with COPD are 36,580,965 Europeans and might project to be 49,453,852 people will have COPD [49]. In addition to that the e-cigarette that has substance like flavor are harmful and irritating the airways [50]. There is huge debate on the safety of e-cigarette and can be used as an alternative method of smoking cessation.
However, these studies that include in our search about e-cigarette with or without nicotine, flavor or flavorless products pointed out that it can trigger inflammation in the lung tissue and cause the lung damage. Furthermore, E-cigarette share similarity of the same inflammatory marker that produce by the effect of cigarette smoke which make it relevant to COPD development that associated with these effects. In vivo, cigarette smoke condensation in mouse induced the proinflammatory cytokines IL-5, IL-6, VEGF and chemokines IP-10and MCP-1 but not IL-13 [ 51 ] . Compere to that Constantinos Glynos and his group, found that e-cigarette vapor exposure triggers the inflammatory responses that affected adversely the respiratory system mechanics in mice [ 52 ]. Also, with long term exposure of e-cigarette to mice, it has stimulated the production of IL-4, IL-5 and IL-13 in BALF [ 53 ]. However, it has been identified that cigarette and e-cigarette likely to have an effect on the development of respiratory disease [51]. Divyal Joshi and his group, the e-cigarette has an association with obstructive lung function impartment and may consider to be adding to the burden of respiratory and other chronic disease [52]. Moreover, Taeyun Kim and Jihun Kang on the association between dual use of e-cigarette and cigarette has pointed a link to the increased risk of COPD [53].
Furthermore, E cigarettes could be unsafe method to be used for nicotine replacement. It may lead to COPD and other respiratory disease due to the toxic mitral that need to be heating its solution to produce the vape. Many cases around the world have register the incidents of explosion and fire due to use of e-cigarette. It is not guaranteed that it is safe as a case of 40- years old female has developed pneumonia with a significant pulmonary toxicity secondary to e-cigarette [54]. However, it is widely known that smoking aid to the developing high risk of lung cancer, while there is more to find out about the vaping risks. It might be possible that lung cancer be one of the serious effects that caused by the use of vaping. The vaping liquid contains nicotine, toxic chemicals material such as the flavoring that require to find out whether it may involve in the risk of devolving lung Collectively, further studies need to be done to find more of the harm and side effect of e-cigarette as well as increase the awareness of its danger [55-58].
Conclusion
It has been demonstrated that cigarette and e-cigarette are both harmful to lung due to the toxic chemical’s components. However, e-cigarette vape effect similarly like cigarette smoke on airways smooth muscles and bronchial epithelial cells that may lead to the production of the cytokines and chemokines. In contrast cigarette smoke and E-cigarette may contribute to the development of Chronic Obstructive Pulmonary Disease (COPD).
References
1. Taeyun K, Jihun K (2021) Association between dual use of e-cigarette and cigarette and chronic obstructive pulmonary disease: an analysis of a nationwide representative sample.
- Mohammad S, Amos L, Jamal A, Faisal K, Zubair K, et al. (2018) Organizing pneumonia related to electronic cigarette use: A case report and review of literature. The clinical respiratory journal 12(3): 1295-1299.
- Global Initiative for Chronic Obstructive Lung Disease-. Global Strategy for Prevention, diagnosis, and management of COPD 2018 [01-01-2022]; Available from: https://goldcopd.org/archived-reports/
- Barnes PJ (2016) Inflammatory mechanisms in patients with chronic obstructive pulmonary disease. J Allergy Clin Immunol 138(1): 16-27.
- Qureshi H, Sharafkhaneh A, Hanania NA (2014) Chronic obstructive pulmonary disease exacerbations: latest evidence and clinical implications. Ther Adv Chronic Dis 5(5): 212-227.
- Mathers CD, Loncar D (2006) Projections of global mortality and burden of disease from 2002 to 2030. PLoS medicine3(11): e442-e442.
- “COPD Costs USA.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 21 Feb. 2018, https://www.cdc.gov/copd/infographics/copd-costs.html.
- Lean MC, Talitha LF, Sarah W, Rudolf TH, Martin H (2016) Projecting the COPD Population and Costs in England and Scotland: 2011 to 2030. Nature 1(6):31893.
- Papandrinopoulou, D, Tzouda V, Tsoukalas G (2012) Lung compliance and chronic obstructive pulmonary disease. Pulm Med 2012: 542769.
- Marina S, Turato G, Facchini FM, Corbino L, Lucchini RE, et al. (1997) Inflammatory Cells in the Bronchial Glands of Smokers with Chronic Bronchitis. Am J Respir Crit Care Med 156(5): 1633-1639.
- Donnell RO, Peebles C, Ward JA, Daraker A, Broberg P, et al (2004) Relationship between peripheral airway dysfunction, airway obstruction, and neutrophilic inflammation in COPD. Thorax 59(10): 837-842.
- Stanescu D, Sanna A, Veriter, C (1996) Airways obstruction, chronic expectoration, and rapid decline of FEV1 in smokers are associated with increased levels of sputum neutrophils. Thorax 51(3): 267-271.
- Kim V, Criner GJ (2013) Chronic Bronchitis and Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med 187(3): 228-237.
- Sturm R (2013) Theoretical models for the simulation of particle deposition and tracheobronchial clearance in lungs of patients with chronic bronchitis. Ann Transl Med 1(1): 3.
- Patel BD, Loo WJ, Tasker AD, Screaton NJ, Burrows NP, Silverman EK, et al. (2006) Smoking related COPD and facial wrinkling: is there a common susceptibility? Thorax 61(7):568–571.
- Kennedy C, Bastiaens MT, Bajdik CD, Willemze R, Westendorp RG, Bouwes JN, et al. (2003) Effect of smoking and sun on the aging skin. J Invest Dermatol 120(4):548–554.
- Michael BO, Divay C (2019) Loss of skin elasticity is associated with pulmonary emphysema, biomarkers of inflammation, and matrix metalloproteinase activity in smokers. Respiratory research 20(1): 128.
- David WK, Kenneth RL (2011) Emergent behavior of regional heterogeneity in the lung and its effects on respiratory impedance. Journal of applied physiology (Bethesda, Md: 1985) 110(5): 1473-1481.
- Eeden SF, Don DS (2013) Oxidative stress in chronic obstructive pulmonary disease: a lung and systemic process. Can Respir J 20(1): 27-29.
- Barnes PJ (2020) Oxidative Stress-Based Therapeutics in COPD. Redox Biology, Elsevier.
- Lee J, Taneja V, Vassallo R (2012) Cigarette smoking and inflammation: cellular and molecular mechanisms. J Dent Res 91(2): 142-149.
- Osadnik CR, CF McDonald, AE Holland (2014) Clinical issues of mucus accumulation in COPD. Int J Chron Obstruct Pulmon Dis 9: 301-302.
- Tamimi A, Serdarevic D, Hanania NA (2012) The effects of cigarette smoke on airway inflammation in asthma and COPD: therapeutic implications Respir Med 106(3): 319-328.
- Blidberg, K, Palmberg L, Larsson K (2012) Increased neutrophil migration in smokers with or without chronic obstructive pulmonary disease. Respirology 17(5): 854-860.
- Scanlon PD, Connect JE, Tashkin DP (2000) Smoking Cessation and Lung Function in Mild-to-Moderate Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med 161(2): 381-390.
- Zhang G, Zhangli W, Enqi L, Zhang K (2018) Safety Assessment of Electronic Cigarettes and Their Relationship with Cardiovascular Disease. Int J Environ Res Public Health 15(1):75.
- Brown CJ, Cheng JM (2014) Electronic cigarettes: product characterisation and design considerations. Tobacco Control 23 Suppl 2(Suppl 2): ii4-ii10.
- Wu Q, Jiang D, Chu HW (2014) Electronic cigarette liquid increases inflammation and virus infection in primary human airway epithelial cells. PLoS One 9(9): e108342.
- Shields PG, Berman M, Wewers MD, Joseph PM, Mathe E, et al. (2017) A Review of Pulmonary Toxicity of Electronic Cigarettes in the Context of Smoking: A Focus on Inflammation. Cancer Epidemiol Biomarkers 26(8): 1175-1191.
- Garcia AI, Geraghty P, Foronjy R, Matthias S (2016) Chronic electronic cigarette exposure in mice induces features of COPD in a nicotine-dependent manner. Thorax 71(12): 1119-1129.
- Behar RZ, Davis B, Talbot P (2014) Identification of toxicants in cinnamon-flavored electronic cigarette refill fluids. Toxicol in Vitro 28(2): 198-208.
- Chen L, Ge Q, Qi Ge, Gavin Tjin, Hatem Alkhouri, et al. (2014) Effects of cigarette smoke extract on human airway smooth muscle cells in COPD. Eur Respir J 44(3): 634-646.
- Alshehri W, Tatler A, Alqarni A, Alahmari M, Alghamdi A et al. (2019) Effect of cigarette smoke extracts (CSE) and e-cigarette vapour extracts (ECVE) on the production of cytokines and chemokines in human airway smooth muscle cells (HASMCs). European Respiratory Journal 54(Suppl 63).
- Merecz-Sadowska A, Przemyslaw S, H Zielinska-Blizniewska, Katarzyna M, Karolina Z, et al. (2020) A Summary of In Vitro and In Vivo Studies Evaluating the Impact of E-Cigarette Exposure on Living Organisms and the Environment. Int J Mol Sci 21(2): 652.
- Oltmanns U, Kian FC, Matthew W, Matthias J, Jane AM (2005) Cigarette smoke induces IL-8 but inhibits eotaxin and RANTES release from airway smooth muscle. Respir Res 6(1): 74.
- Volpi G, Fabrizio F, Nadia M, Maurizio C, Riccardo P (2011) Cigarette smoke and α, β-unsaturated aldehydes elicit VEGF release through the p38 MAPK pathway in human airway smooth muscle cells and lung fibroblasts. Br J Pharmacol 163(3): 649-661.
- Pereira ABM, Jhony RO, Ana LJS, L Andrade-Silva, Marcos VS, et al. (2021) Effects of cigarette smoke extract on bronchial epithelial cells stimulated with Cryptococcus neoformans. Med Microbiol Immunol 210(4): 221-233.
- Garcia-Arcos I, Patrick G, Nathalie B, Michael C, Abdoulaye JD, et al. (2016) Chronic electronic cigarette exposure in mice induces features of COPD in a nicotine-dependent manner. Thorax 71(12): 1119-1129.
- Ween MP, Jonathan JW, Rhys H, Paul NR, Sandra JH (2017) Phagocytosis and Inflammation: Exploring the effects of the components of E-cigarette vapor on macrophages. Physiol Rep 5(16): e13370.
- Leigh NJ, Ralph IL, Pamela AH, Maciej LG (2016) Flavourings significantly affect inhalation toxicity of aerosol generated from electronic nicotine delivery systems (ENDS).” Tob Control 25(Suppl 2): ii81-ii87.
- Crotty ALE, Christopher AD, Mark H, Denzil M, Alex M, et al. (2018) Chronic inhalation of e-cigarette vapor containing nicotine disrupts airway barrier function and induces systemic inflammation and multiorgan fibrosis in mice. Am J Physiol Regul Integr Comp Physiol 314(6): R834-R847.
- Grubek-Jaworska H, Magdalena P, J Hermanowicz-Salamon, K Białek-Gosk, Marta D, et al. (2012) IL-6 and IL-13 in induced sputum of COPD and asthma patients: correlation with respiratory tests. Respiration 84(2): 101-107
- Ning L, Hua Z, Min-Li C, Zheng-Fu X (2017) Association of the IL-13 polymorphisms rs1800925 and rs20541 with chronic obstructive pulmonary disease risk: An updated meta-analysis. Medicine (Baltimore) 96(47): e8556.
- SL Traves, SV Culpitt, REK Russell, PJ Barnes, LE Donnelly (2002) Increased levels of the chemokines GROalpha and MCP-1 in sputum samples from patients with COPD. Thorax 57(7): 590-595.
- Garcia-Arcos I, Patrick G, Nathalie B, Michael C, Abdoulaye JD, et al. (2016) Chronic electronic cigarette exposure in mice induces features of COPD in a nicotine-dependent manner. Thorax 71(12): 1119-1129.
- Ween MP, Jonathan JW, Rhys H, Paul NR, Sandra JH (2017) Phagocytosis and Inflammation: Exploring the effects of the components of E-cigarette vapor on macrophages. Physiol Rep 5(16): e13370.
- Leigh NJ, Ralph IL, Pamela AH, Maciej LG (2016) Flavourings significantly affect inhalation toxicity of aerosol generated from electronic nicotine delivery systems (ENDS).” Tob Control 25(Suppl 2): ii81-ii87.
- Crotty ALE, Christopher AD, Mark H, Denzil M, Alex M, et al. (2018) Chronic inhalation of e-cigarette vapor containing nicotine disrupts airway barrier function and induces systemic inflammation and multiorgan fibrosis in mice. Am J Physiol Regul Integr Comp Physiol 314(6): R834-R847.
- “CDC - Data and Statistics - Chronic Obstructive Pulmonary Disease (COPD).” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 14 June 2021, https://www.cdc.gov/copd/data.html.
- Chronic obstructive pulmonary disease (COPD) statistics British Lung Foundation Statistics. 2011 [01-01-2019]; Available from: https://statistics.blf.org.uk/copd.
- Benjafield A, Daniela T, Meredith B, Rahul G, Carlos N, et al. (2021) An Estimate of the European Prevalence of COPD in 2050. European Respiratory Journal 58(Suppl 65).
- Leigh NJ, Ralph IL, Pamela AH, Maciej LG (2016) Flavourings significantly affect inhalation toxicity of aerosol generated from electronic nicotine delivery systems (ENDS).” Tob Control 25(Suppl 2): ii81-ii87.
- Zhao J, Li Xiang, Fuwei X, Zhihua Y, Xiujie P, et al. (2017) Immunomodulatory effects of cigarette smoke condensate in mouse macrophage cell line. Int J Immunopathol Pharmacol 30(3): 315-321.
- Glynos, Constantinos, Sofia-Iris B, Paraskevi K, Athanasia P, Christina M, et al. (2018) Comparison of the effects of e-cigarette vapor with cigarette smoke on lung function and inflammation in mice.” Am J Physiol Lung Cell Mol Physiol 315(5): L662-L672.
- Lim HB, SH Kim (2014) Inhalation of e-Cigarette Cartridge Solution Aggravates Allergen induced Airway Inflammation and Hyper-responsiveness in Mice. Toxicol Res 30(1): 13-8.
- Bhatta ND, Glantz AS (2020) Association of E-Cigarette Use with Respiratory Disease Among Adults: A Longitudinal Analysis. Am J Prev Med 58(2): 182-190.
- Joshi D, Duong M, Kirkland S, Parminder R (2021) Impact of electronic cigarette ever use on lung function in adults aged 45-85: a cross-sectional analysis from the Canadian Longitudinal Study on Aging. BMJ Open 11(10): e051519.
- Kim T, Kang J (2021) Association between dual use of e-cigarette and cigarette and chronic obstructive pulmonary disease: an analysis of a nationwide representative sample from 2013 to 2018. BMC Pulm Med 21(1): 231.






























