Leishmaniasis in Syria
Al-Nahhas S1 and Altawil A2
1Department of Animal Biology, Faculty of Science, Damascus University, Damascus, Syria
2National Leishmaniasis Control Program, Ministry of Health, Damascus, Syria
Submission: August 23, 2017; Published: September 22, 2017
*Corresponding author: Al-Nahhas S, Department of Animal Biology, Faculty of Science, Damascus University, Damascus, Syria, Email: samar.nahhas@yahoo.com
How to cite this article: Al-Nahhas S, Leishmaniasis in Syria. Int J cell Sci & mol biol. 2017; 3(2) : 555609. DOI: 10.19080/IJCSMB.2017.03.555609.
Opinion
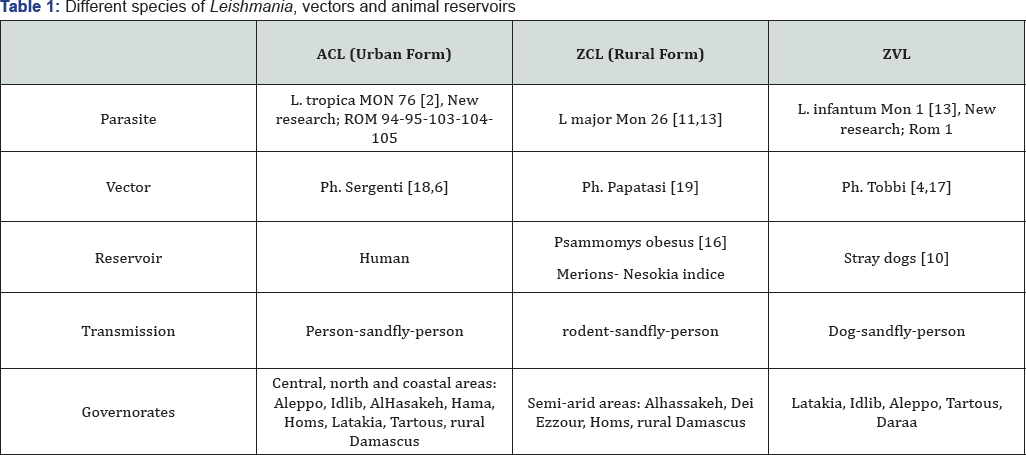
Leishmaniasis is still considered a main health problem in Syria. Three epidemiological forms are known in this country: ACL (L. tropica), ZCL (L. major) and VL (L. infantum) which spread according to the geographical nature of the place (the altitude); the species of the vectors (sandflies) [1], the animal reservoirs and many other environmental factors. Table 1 presents the parasite species, the vector species, the animal reservoirs and the transmission way. These make the control of this disease difficult and more complicated beside to many other problems related to different issues like: population growth and movement, the health system, intersect oral co operation, the weakness of national research institutions. etc. Most of the reported cases from rural areas around the capital Damascus, the costal western region (Latakia and Tartous), the middle region (Homs, Hama and Idlib) and the eastern region (Al , Hasakeh and DeirEz-Zour) of the country, are cutaneous (ACL and ZCL). However, in the eastern and southern regions dozens of visceral cases are reported every year.
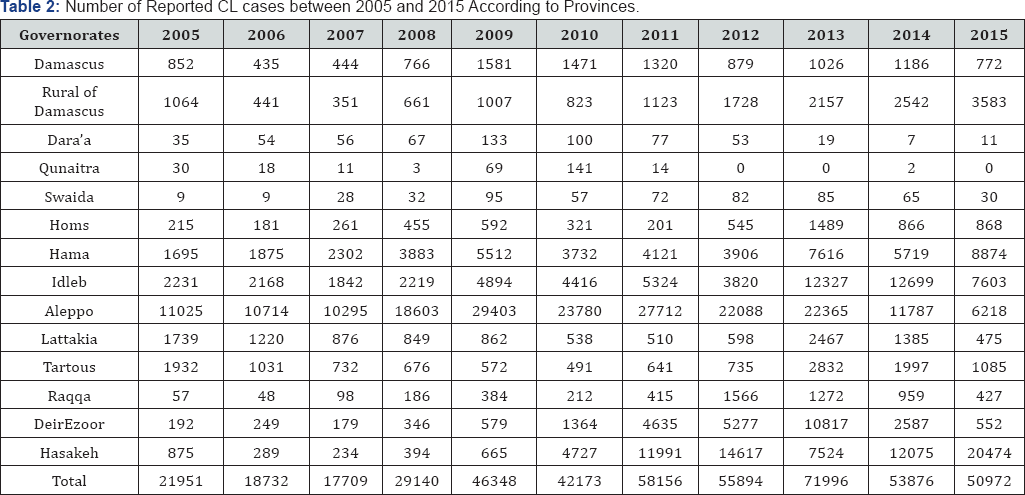
During the 10 year period (2005-2015), the number of cutanoeus leishmaniasis cases reported by the Department of disease control (Table 2), while the number of visceral leishmaniasis was 211 cases between 2006 and 2016. People with cutaneous leishmaniasis have one or several long-lasting lesions on the skin, usually without fever or general symptoms. Cutaneous leishmaniasis caused by L. major (known as rural zoonotic cutaneous leishmaniasis). The lesions are often severely inflamed and ulcerated and heal within 2-8 months. The incubation period is often less than 4 months. While, Cutaneous leishmaniasis caused by L. tropica (known urban anthroponotic cutaneous leishmaniasis) produces painless, frequently multiple, dry ulcers of the skin, which usually heal spontaneously within about one year. The incubation period is usually 2-8 months.
In light of the crisis our country faces, there is a big demographic change due to:
i. The migration of people from their permanent residency areas and staying in evacuation shelters, poor housing.
ii. The introduction of non-immune people into areas with existing endemic or enzootic transmission cycles.
iii. The large number of people found into a small space may attract sand flies
iv. The deficient medical facilities
v. The high density of rodents in some areas.
vi. The per-domestic sanitary conditions (e.g. lack of waste management, open sewerage).
vii. The climate changes (rainfall, atmospheric temperature and humidity)
All of these changes increase the incidence of the leishmaniasis, or affect the transmission of the disease.
Depending on the Ministry of Health reports, a high number of ACL cases, was recorded in safe governorates (Latakia and Tartous). During the period (2011-2015), the number of cutanoeus leishmaniasis cases was:
1) Latakia: 510, 589, 2457,1385 and 475 respectively
2) Tartous: 641, 735, 2832, 1997 and 1085 respectively.
While the number of CL cases (mostly ZCL) at Alhasaka governorate Increased dramatically from 4727 cases in 2010 to 20474 cases in 2015.
The diagnosis and treatment centers were established in each province of Syria. The original techniques for demonstrating amastigotes in smears of bone marrow and skin lesions for diagnosis are still reference methods. Although, the detection of parasite DNA by PCR in blood or bone marrow aspirates is substantially more sensitive than microscopic examination [2-4].
Two serological tests, the direct agglutination test and the rK39 antigen-based immuno-chromatographic test were specifically developed for field use and have shown good diagnostic accuracy in most endemic areas [5-9]. The rK39- based test is easy to perform, fast, cheap and give reproducible results and can therefore be used for early diagnosis of visceral leishmaniasis (especially in hot spot areas). A standard treatment regimen was started for patients with parasitological proven either Local or systemic treatments (Antimonials) or physical treatment (Thermotherapy 50 °C, Cryotherapy -196 °C). The cost of treatment and implementation of prevention strategies needs a high financial and human resource investment [10-19].
The control activities are:
a) Early active and passive case detection
b) Laboratory Diagnosis & Treatment
c) Health education and community participation.
d) Establishment vector control activities (two insecticides spray campaigns), and animal reservoir control activities (in zoonotic foci).
e) Cooperation and coordination with other concerned sections and authorities.
f) Environmental corrections and managements.
References
- Ismail MT, Pesson B (1992) Contribution à l'étude des Phlebotomes de Syrie. Bull Soc Path Ex 85: 317-321.
- Al-Nahhas S (2005) Contribution study of visceral leishmaniasis in Syria. Saudi Med J 26(3): 490-492.
- Al-Nahhas S, Kaldas R (2013) Characterization of leishmania Species isolated from cutaneous human samples from centeral region of Syria by RFLP analysis. ISRN Parasitol 19: 308726.
- Haddad N, Saliba H, Altawil A, Villinsky J, Al-Nahhas S, et al. (2015) Cutaneous leishmaniasis in the central provinces of Hama and Edlib in Syria: Vector identification and parasite typing. Parasit Vectors 12(8): 524-532.
- Burns JM, Shreffler WG, Benson DR, Ghalib HW, Badaro R, et al. (1993) Molecular characterization of kinesin-related antigen of L. chagasi that detects specific antibody in African and American VL. Proceedings of the national academy of sciences of the United States of America 90(2): 775-779.
- Zijlstra EE, Nur Y, Desjeux P, Khalil EA, El-Hassan AM, et al. (2001) Diagnosing VL with the recombinant k39 test: experience from the Sudan. Trop Med Int Health 6(2): 108-113.
- Ryan JR, Smithyman AM, Rajasekariah GH, Hochberg L, Stiteler JM, et al. (2002) ELISA based on promastigote antigen detects IgM and IgG antibodies in sera from cases of VL and CL. J Clin Microbiol 40(3): 1037-1043.
- Al Nahhas S, Shabaan M, Hammoud L, Al Taweel A, Al Jorf S (2003) VL in the Syrian Arab Republic: early detection using rk39. Eastern Med. Health J 9(40): 865-862.
- Al-Nahhas SA, Al-Taweel AA, Al-Taweel MA (2008) Assessment of the direct agglutination test, fast agglutination screening test, and rK39 dipstick test for the sero-diagnosis of visceral leishmaniasis in Syria. Saudi Med J 29(9): 1250-1254.
- Dereure J, Rioux JA, Khiami A, Pratlong F, Périères J, et al. (1991) Ecoepidemiologie des leishmanioses en Syrie. 2-Presence chez le chien de Leishmania infantum Nicolle et Leishmania tropica (Wright) (Kinetoplastidae: Trypanosomatidae). Ann Parasitol Hum Comp 66(6): 252-255.
- Haddad N (1998) les phlébtomes du liban. Inrentaire et corollaire éco- épidémiologique. These d'universite, Reims pp.208-220.
- Killick-Kendrick R (1999) The biology and control of Phlebotomine sand flies. Clin Dermatol 17: 279-289.
- Khiami A, Dereure J, Pratlong F, Martini A, Rioux JA, et al. (1991) Human cutaneous leishmaniasis caused by Leishmaniamajor MON-26 in the region of Damascus (Syria). Bull Soc Pathol Exot 84(4): 340-344.
- Rioux JA, Lanotte G, Serres E, Pratlong F, Bastien P, Perieres J, et al. (1990) Taxonomy of Leishmania. Use of isoenzymes. Suggestions for a new classification. Ann Parasitol Hum Comp 65(3): 111-125.
- Rioux JA, Dereure J, Khiami A, Pratlong F, Sirdar K, et al. (1990) Ecoepidemiology of leishmaniasis in Syria. 1. Leishmaniamajor Yakimoff and Schokhor (Kinetoplastida-Trypanosomatidae) infestation of Psammomysobesus Cretzschmar (Rodentia-Gerbillidae). Ann Parasitol Hum Comp 65(5-6): 203-207.
- Rioux JA, Ashford RW, Khiami A, et al. (1992) Ecoepidemiology of leishmaniases in Syria. 3. Leishmaniamajor infection in Psammomysobesus provides clues to life history of the rodent and possible control measures. Ann Parasitol Hum Comp 67(6): 163-165.
- Rioux JA (1998) Infestation naturelle de Phlebotomus tobbi (Diptera - Psychodidae) par Leishmania donovani .s. st. (Kinetoplastidae- Trypanosomatidae) en Syrie. Parassitol 40: 148.
- Volf P (2002) Cutaneous leishmaniasis in Sanliurfa, Turkey: Phlebotomus sergenti remains abundant with the decline of recent epidemic. J Med Entomol 39: 12-15.
- Yaman M, Ozbel Y (2004) The sand flies (Diptera: Psychodidae) in the Turkey province of Hatay: some possible vectors of parasites causing human cutaneous leishmaniasis. Ann Trop Med Parasitol 98 (7): 741750.






























