Assessment of Dispensing Practices and Quality of Pharmaceutical Services Given at Shenen Gibe Hospital and Mendera Kochi Health Center in Jimma Town South West Ethiopia
Etsegenet Yoseph and Anbessa Bekele*
Pharmacy School, Health Institute, Jimma University, Ethiopia
Submission: January 25, 2018; Published: April 26, 2018
*Corresponding author: Anbessa Bekele, Pharmacy School, Health Institute, Jimma University, Ethiopia, Tel:251-910-817853 ; Email: anbebake@gmail.com
How to cite this article: Etsegenet Y, Anbessa B. Assessment of Dispensing Practices and Quality of Pharmaceutical Services Given at Shenen Gibe Hospital and Mendera Kochi Health Center in Jimma Town South West Ethiopia. Glob J Pharmaceu Sci. 2018; 5(4): 555667. DOI: 10.19080/GJPPS.2018.05.555667
Abstract
Background: Dispensing practices refers to the delivery of the correct drug and medical supply to the right patients, in the required dosage, quantities and clear drug information. The contributing of pharmacy professional in this regard has a role towards that goal.
Objective: To assess knowledge of the dispensers and quality in dispensing practices given at shenen gibe hospital and mendera Kochi health center in Jimma town.
Methods: The study was conducted at Shenen Gibe hospital and Mendera Kochi health center in Jimma town. A cross sectional study was conducted by using self administered questionnaire including with all dispensers at working area during study period.
Result: The result of this study was analyzed using tables and graphs.
Conclusion: Irrational dispensing practice like dispensing of poorly labelled drugs, lack of patient counselling and dispensing error were frequently occurred. In addition, only few of the dispensers updated themselves timely. Therefore, dispensers should be well trained on good dispensing practice to decrease dispensing errors.
Keywords: Dispensing; Practices; Knowledge; Quality of pharmaceutical services Shenen Gibe hospital and Mendera Kochi health center
Introduction
Background
Dispensing refers to the process of preparing drugs and distributing them to their users with provision of appropriate information [1]. It may be based on a prescription or an oral request of users (patients or care providers) depending on the type of drugs to be dispensed. The dispensing process involves the correct interpretation of the prescription or oral request, accurate preparation and labelling of drugs with provision of appropriate information. The drug should be dispensed in a safe and hygienic manner, making sure that the patient or care provider understands and appreciates the value of taking specific drugs for specific indications [2]. Rational drug use is a tool through which safe, effective and economic medication is provided. It is promoted by the collaborated efforts of prescribers, dispensers and drug consumers. Rational prescribing ensures adherence to treatment and protects drug consumers from unnecessary drug adverse reactions. Rational dispensing on the other hand, promotes the safe, effective and economic use of drugs [3].
Traditionally, pharmacist's primary responsibility has been the correct dispensing of drugs and the pharmaceutical quality of the drugs dispensed. Now a day, their role has increased to involve advising the physician and other health professionals about drug therapy, counselling patients about drugs and monitoring drug use. They bridge the gap between the physician and the patient and serve as the gatekeepers of the drug supply system [1] . Globally, more than 50% of all medicines are prescribed, dispensed or sold inappropriately while, 50% of patients fail to take the prescribed drugs correctly. Moreover, about one-third of the world populations lack access to essential medicines [4]. In Ethiopia, poor understanding about medications leading to non-adherence is a common phenomenon indicated by different studies [3]. Irrational dispensing practice like dispensing of prescription only drugs at partial dose and even without a prescription, poor labelling of the dispensed drugs, lack of patient counselling, incomplete compiling and recording of prescriptions and charging patients unreasonably high price for dispensed items are common in developing countries [5]. The aim of the study was to ensure the availability of facilities including equipments and materials in the dispensary room, the drug information updating sources for pharmacists and to identify the main problems encountered during dispensing practices. Moreover, the current study evaluated the quality of pharmaceutical services provided.
Statement of the Problem
Dispensing is one of the vital elements of rational drug use. All the resources involved in patient care up to the point of dispensing may be wasted if dispensing does not result in the named patient receiving on effective from of the correct drug, in appropriate packaging and with the correct dose and advice [2] . Dispensing is critical part of the drug use process so that, inappropriate dispensing practices can adversely affect the benefits of the health care delivery system. Patient's compliance to medication instruction is often influenced by the information given during dispensing. In most developing countries drug dispensing is usually done by untrained staff [2]. Studies show that, more than 50% of all medicines worldwide are prescribed, dispensed in appropriately, while another 50% of patients fail to take them accordingly [3].
Irrational dispensing practices like any other developing country are not uncommon in Ethiopia. The dispensing of prescription- only drugs at partial doses and even without prescription, poor labelling of the dispensed items, lack of patient counselling, incomplete compiling and recording of prescriptions, and charging patients unreasonably high prices are among the irrational dispensing practices [2]. Crosscontamination is one of the problems encountered while sing dispensing equipments for measuring liquids or counting tables or capsules. In appropriate labelling of stock container is liable to unsafe selection of the correct preparation and increase the risk of error selecting a stock container during dispensing process according to colors or location of the container, without consciously reading the label has dangerous consequence on the patients.
During dispensing the need for confidentiality and privacy when explaining the use of some types of medicine must be recognized and every patient must be treated with respect [2]. The dispenser plays a crucial role in the therapeutics process. The quality of dispenser may be affected by the training and supervision the dispenser has received and the drug information available of dispenser. The low status of dispensers can also affect the quality of dispensing [2]. The pharmacist has ultimate professional responsibility to decide whether or not to dispense the prescription [4].
According to Hong Kong medical association; there are lots of factors contributing to dispensing errors. These are in adequate knowledge or skills, fail to comply with polices or procedures, failure in communication or miss interpretation of prescription order, stress, similar drug name, stock management, wrong dose mislabelling, illegible hand writing, unclear prescription, product labelling, drug storage problem etc [5]. The lack of necessary materials or medicines in hospitals and low purchasing power of the population have sometimes led to use of available and affordable medication that is not necessary represent the most appropriate treatment. Extremely low and irregularly paid salaries have lowered the motivation of health professional and worsened that quality of care. Availability of new medicines at the market and the poor access to the information their knowledge [6].
Significance of the study
The in effectiveness of dispensing practice was affected by the way the drugs are dispensed and the types of information given to the patients during dispensing. Therefore, the study finding will help us to identify the main problems encountered during dispensing practice, will contribute knowledge for pharmacists to identify major causes for dispensing error. It Will also helps to determine the cost effective intervention to improve dispensing practice at different health facilities. Moreover, it will provide a base line data for further study because there is no study done at Jimma town regarding good dispensing practice.
Literature review
A study on dispensing practice showed that due to poor hand writing prescription, wrong drug was dispensed. The dispensing drug name is similar to the actually prescribed drug but completely different .A drug an antacid diouol was prescribed but anti diabetic drug daonil was actually dispensed and the patients died of hypoglycemia [2]. A study done in the Mambere- kadei health district of the central Africa Republic in April 2008, (21.5%) of dispensed drugs were in adequately labelled. patients under stood the modalities of use for 69.6% of prescribed drugs. The average dispensing time was five minutes .Excessive use of antibiotics and injection and blunder buss therapy was observed. Other problems observed from the survey made was poor information on drug use, in adequate labelling of dispensed drugs and lack of access to standard drugs tools such as locally adopted essential drug list, formularies and standard treatment guide line [7].
In the united states, a July 2006 report from the national Academic of science institute of medicine (IOM), medical practitioners sloppy hand writing kills more than 7000 peoples annually .According to an Irish study, prescription hand writing is notorious for being often illegible which constituted 5%.some jurisdictions, example Florida, have made legible prescription, all together and computer printed prescription are becoming increasingly common in some place [8,9]. A study done in North West Ethiopia shows that 3.8% of the patients were non compliant with the drug regimens due to miss understanding of instruction [10].
A similar study done in Gander showed that 13.5% of patients were no complaints with therapeutics regimens due to miss understand or lack of instruction about dosing schedule of prescribed drugs [11]. In February 2001, a study in the Lao people's Democratic showed that , poor dispensing practice were manifested by lack of information about drugs dispensed in 59% of case, drug not being labelled in 47% and different drugs being in the same package in 26% of case [12]. Dispensing and storage based on ministry of institution in south Africa practiced by dispensing doctors are 52% of medicine are dispensed by in appropriately trained person, 33% of dispensing doctor counted tablets by hand, 61% of dispensing Doctor had unsuitable container: labelling of dispensed drugs was unsatisfactory in 27% of the dispensing doctor practice: storage conditions were in appropriate in 46% of the dispensing doctors practices, with un satisfactory cool storage facilities in 39% no expiry monitoring system in 70% and medications not clearly labelled in 20% [13].
In Ghana, study done in 2008 indicated that, in most developing country drug dispensing is usually done by untrained staff. Only 8.3% dispensing staff actually interacting with patients had received formal training as dispensers. The rest were mainly dispensing assistants, medical assistant and nurses [14]. A study done in America at 2002 show that 47% of antibacterial drugs, 25% of injections were sold from pharmacies without prescription of a doctor. It was confirmed that pharmacist carry out not only generic, but also therapeutic substitution and sometimes advising wrong medicines. In addition there was no regulation on labelling and patient leaflets for many pharmaceuticals at market do not comply with WHO recommendations and EU guidelines in this care. Neglecting education also causes the irrational consumption of medicines in Armenia [3,11].
Shortage of essential drugs and availability of non essential drugs; lack of sound objectives on drug information; and the considerable influence of drug promotion; on both prescriber and consumer. Therefore, dispensing must be performed accurately and should be done in an orderly manner with disciplined use of effective procedure. Care should be taken to read labels accurately. The dispenser must count with equipment and avoid handling of medicines. Pre-packaging medicines can improve efficiency in dispensing. Labels should contain information about the medicines and its correct use. The style and language of labelling should be appropriate to the needs of the patients. Ensuring patients understanding of how to take their medicines is a primary responsibility of dispensers. Good records are essential part of dispensing and they facilitate good management and monitoring of services provided [1].
Objectives
General objectives
To assess knowledge and quality of dispensing practices of pharmaceutical products at Shenen gibe hospital and Mendera Kochi health center in Jimma town.
Specific objectives
a. To assess practice of prescription processing and labelling of the drugs
b. To assess drugs or pharmaceutical arrangements in dispensing room
c. To determine common errors occurred during dispensing
d. To identify the cause of dispensing errors
e. To determine the drug information source (like text books, standard treatment Guide line leaflets etc)
Method and Materials
Study area and period
The study was conducted at Shenen Gibe Hospital and Mendera Kochi Health Center found in Jimma town Feb8/2017- Feb26/2017.
Study design
A cross- sectional study was carried out by using open ended and closed ended questioner through face to face interview.
Population
Source of population
All dispensers working in Hospital and health centers in Jimma town 2016/17.
Study population
All dispensers working at Shenen Gibe Hospitals and Mendera Kochi Health Centers, in Jimma during the study period.
Sample size and sampling technique
Since study populations were small that was total pharmacist and druggist the study area population were 46 who were include in the study exclusively. Therefore, no sample size determination and sampling technique was employed in this study. All 46 (pharmacist and druggist) dispensers who were available at Shenen Gibe Hospitals and Mendera kochi Health Center were included in the interview.
Study variables
Independent variable:
a. Age
b. Sex
c. Religion
d. Ethnicity
Dependent variables:
a. Status of dispensers
b. Types and natural of dispensing errors
c. Stage at which an error will occur
d. Possible cause for dispensing error
e. Access to drug information
f. Knowledge and practice regarding dispensing of drugs to patients
g. Dispensing time
Data collection instrument & data collector
Semi-structured questionnaire was used to collect the necessary information. Accessories materials like, pencil, chalk, binder, eraser and sharpener were used. The data was collected by investigator.
Data collection methods: Data was collected by interviewing the dispensers through structured questionnaires and with incursion of observation.
Data processing and analysis: The collected data was processed by using scientific calculator and Microsoft excel. Then the results were presented using tables and figures.
Quality assurance: Before the respondent asked the question, information was given to them about how they understand the words written and the idea about what the questionnaire says. They will also be informed about the objective of the study, so that every respondent will understand the question well and give an attention (with responsibility).
Ethical consideration: Before data collection started to conduct this study ethical approval was obtained from Jimma University School of pharmacy, facility of health sciences, institute of health research team leader. Ethical approval was obtained from Jimma University Ethical review board. Informed consent was obtained from each study participant. First official letter of permission from Jimma University student research program to School of pharmacy was given. After giving brief explanation about the objective of the study for the study subjects' informed consent was obtained before data collection. Confidentiality of the information they gave was be assured for each study subjects.
Results
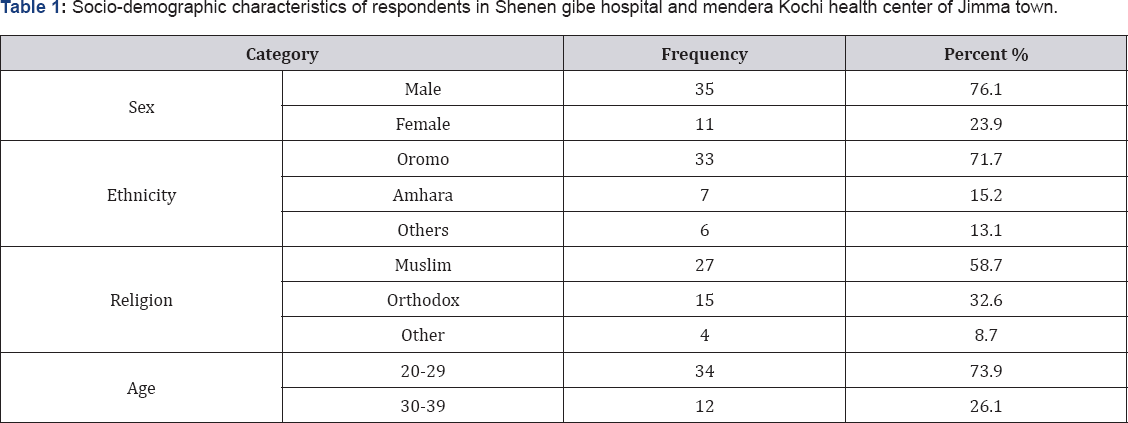
(Table 1) Socio-demographic characteristics of respondents in Shenen gibe hospital and mendera Kochi health center of Jimma town. A total of 46 dispensers selected from Shenen Gibe Hospital and Mendera Kochi Health Center institution included in the study. Among the 46 study subjects, 35 were male. The remaining 11 were female and their respective ethnicity was Oromo (33), Amhara (7) and others (6). The majority of practitioners are found in the age rang 22-29 years.
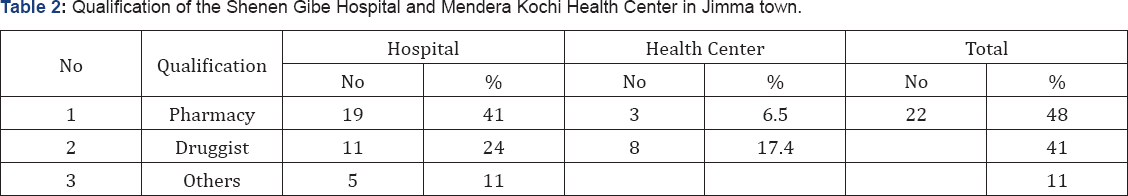
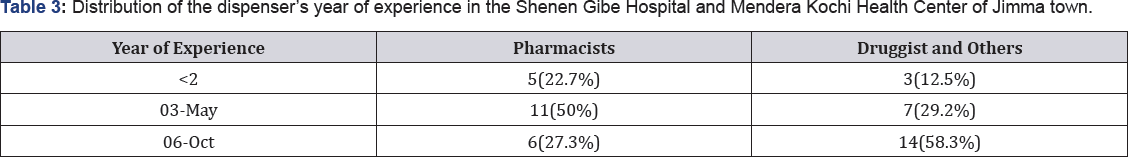
In this study, majority of pharmacists (41.3%) are working in hospital and the remaining (6.5%) are working in the health center. Most of the pharmacists are working in the hospital (41.3%) than health center (6.5%) (Table 2). Based on this study 3-5 year 11(50%) majority of the pharmacist year of experience and from druggist most of them work 6-10 year 14(58.3%) (Table 3).
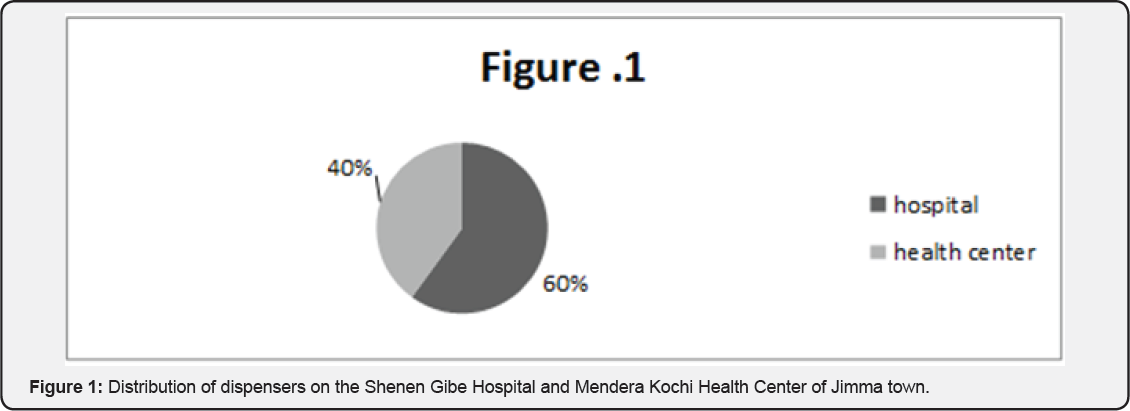
From the above figure 60% of the pharmacy professionals included in the study was working in Shenen Gibe Hospital and the remaining 40% of dispensers were working in the Mendera Kochi Health Center (Figure 1).
Availability of drug information center in Shenen Gibe Hospital and Mendera Kochi Health Center of Jimma town. From Shenen Gibe Hospital and Mendera Kochi Health Centers .1 of Shenen Gibe Hospital and no drug information centers In Mendera Kochi Health Center. Availability of equipment and material during the study at Shenen Gibe Hospital and Mendera Kochi Health Centers in Jimma town. In this study the Shenen Gibe Hospital and Mendera Kochi Health Centers have refrigerator, telephone service and portable water but only Hospital have national drug list.
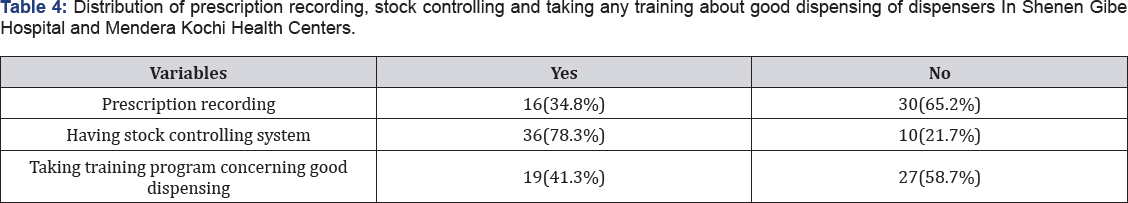
On the prescription recording habit the participant, 16(34.8%) were recording dispensed prescription dispensed prescription and 30(65.2%) of the dispenser reported that they do not record. 36(78.3%) of the respondent were using stock controlling system and the remaining 10(21.7%) were not using. Majority of the dispensers had not taken any concerning good dispensing practice (Table 4).
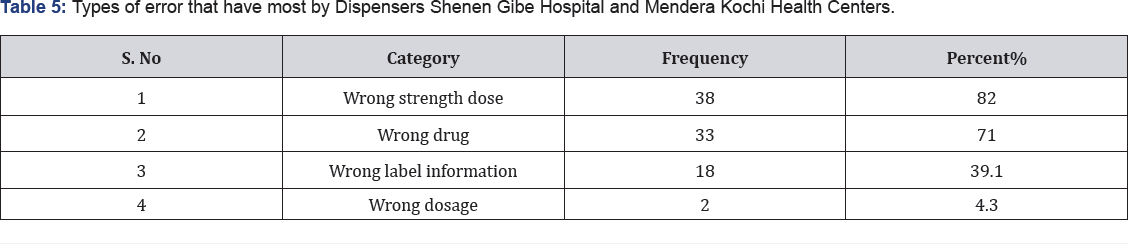
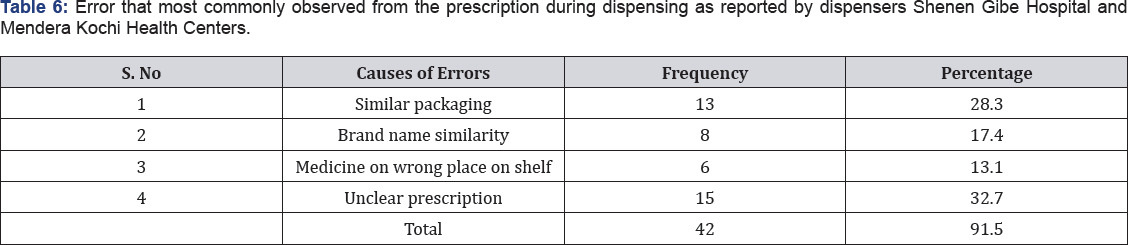
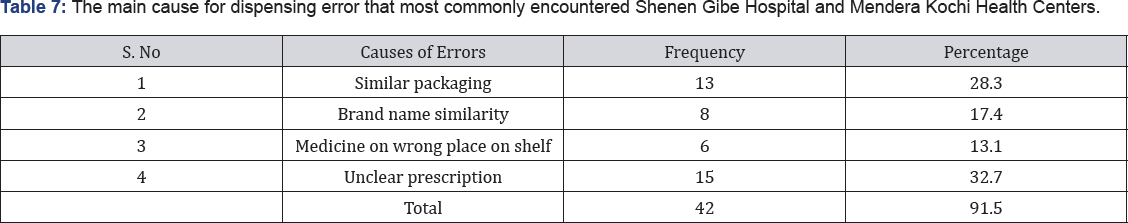
From the Table 5, 38 (82%) of the dispensers respond that wrong strength or dose was dispensed, 33(71%) said that wrong drug was dispensed and 18(39.1%) wrong label information from the Table 6. 33(71.7%) of the respondents said that error that commonly observed was illegible hand writing while 31(67.4%) said that it was due to drug-drug interaction and the rest was wrong contents 9(19.6%). From the Table 7, in this study the most common frequency of error was: unclear prescription 15(32.7%), similar packaging 13(28.3%), brand name similarity 8(17.4%).
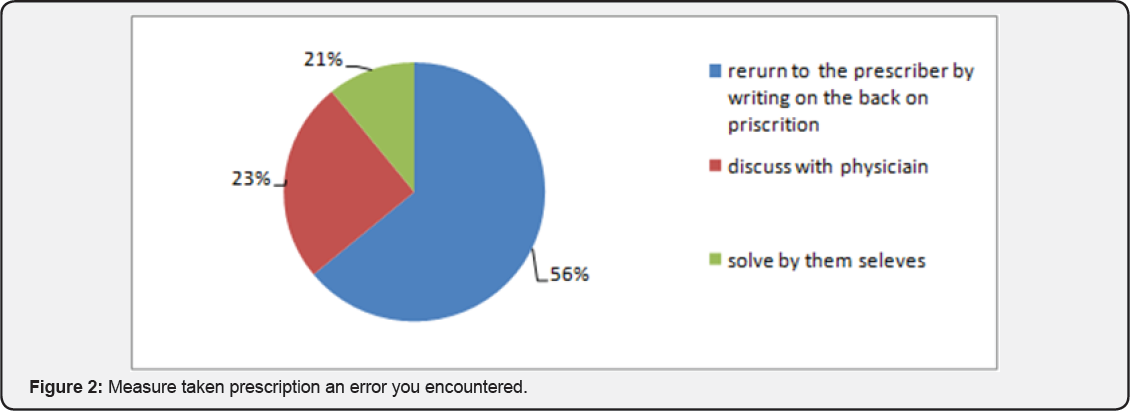
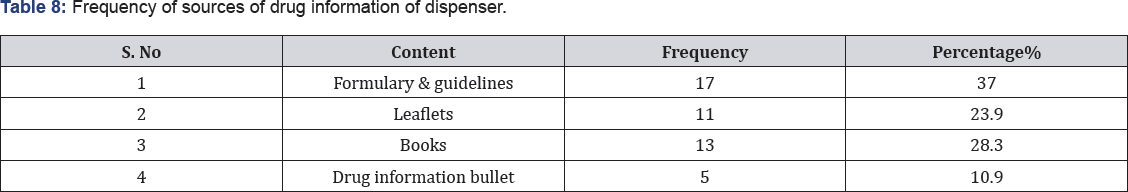
From the above figure (56%) of the dispenser said that they return incorrect prescription to the prescriber, 23% of the dispensers said they discuss with the prescriber and 21% said that they correct by themselves (Figure 2). The most common source of drug information for those who reported to update themselves was formulary and guidelines 17(37%), and leaflets 11(23.9%). In addition, materials like books and bullet were also used, but in less extent (Table 8).
Discussion
In this study 46 practioners were participated 0.35(76.1%) were male and the rest 11(23.9%) were female, 34(73.9%) were 20-29 years, 12(26.1%) were 31-39 year old. In hale the study which was done in Turkey 44.5% were have primary degree (pharmacists) but in this study 47.8% were have primary degree and the remaining participant in hale the study were have not primarily degree, in this study the remaining study participants were have diploma (druggist) and others. Study done in Ghana, 2008 indicated that in most developing country the drug dispensing was done by untrained staff. Only 8.3% of the dispensers had received formal training but in this study most of the dispensers had a formal training (professional qualification). The greater number of dispenser works in hospital and the remaining 40% work in health center.
In this study 37%of the respondent use formularies and guidelines and other leaflets, books and bullet. 100% have drug information center and Medera Kochi Health Center has not drug information center .41.3% respondent had taken good dispensing training and the remaining respondent 58.7% had not taken any training. In Hale Z study which was done in Turkey 12.7% had a post graduate education and 41.8% had on other professional experience in hospital pharmacy [15]. On the prescription recording habit of the dispensers 34.8% record dispensed prescription and 65.2% of the dispensers do not record. Regarding the use of stock control system, 78.2% of the respondents were using the controlling system and the remaining 21.7% were not using.
Dispensing of drug need up to data knowledge about the drugs. It was somehow good to get up data information but they were think about more education or other training to take. In this study 67.4% of the participants responded that error was due to miss reading, 71.7% due to illegible prescription and 19.6%was due to wrong content of prescription .A study done in the member kadei health district of the central Africa 21.5% of dispensed drugs were in adequately labelled and according to Irish study, when prescription hand writing is notorious for being often illegible which constituted 5%, so when it was compared , dispensing error was the most problem pointed from the study.
In correction of prescription or managing the prescription error, 56% of the dispensers return incorrect prescriptions to the prescriber 23% of the dispensers were discussing with the prescriber and 21% were correcting by themselves. As of in accordance to Hale of pharmacists reported that in the case of a prescription problem their approach was to call the doctor (95.5%) ask a colleague (43.71%) use their own knowledge/ judgment (93.0% check a reference book or drug index etc. (21.1%) [16]. As compared to Hale's study which was done in Turkey 93.1% of the dispensers judge by themselves but in this study 21% judge by themselves and also 95.8% of the dispenser call to the doctor in according to the study of hales study but in this study only 23% of the dispenser discuss with prescriber. Study done in Turkey by Hale the pharmacists give information about the medication drug interactions, possible side effects, contraindication and storage instructions was not given at all. The other information given was the name of the drug (20%) diagnosis/purpose of the drug (8.9%), Pharmaceutical dosage form of the prescribed drug of (6.3%) 1.3% of the simulated patients were misinformed about the dosing schedule [16].
But in this study all of the participants give information regarding direction for use, method of handling, (63.3%) side effect of the drug and (36.4%) were not giving information of side effect of the drug to the patients, none of them gives about expiry date of the drugs. From this study, the most commonly information given to the patient was direction for use and method of handling. Writing expiry date of the drug is not common from the study. This study revealed that unclear prescription was the main cause for dispensing error which accounts (32.7%) and the remaining possible causes were similar packaging (28.3%), brand name similarity (17.4%). According to Hong kong medical association, the main cause, that associated with dispensing errors were inadequate knowledge or skills, faller in communication, product labeling, unclear prescription, drug storage problem. So this study is similar with the present study, regarding unclear prescription as the cause of the dispensing error.
Conclusion
Form the finding of the study it is possible to conclude that irrational dispensing practice like dispensing of poorly labelled drugs and lack of patient counselling were occurred. In addition, illegible prescription was the most commonly encountered practice on prescription during dispensing. The main causes of dispensing error were illegible prescription and brand name similarity. Dispensers should council the patients, practice labelling during dispensing and not dispense illegible prescriptions to ensure that an effective form of the correct drug is given to the right patient in the prescribed dosage and quantity with clear instructions. Dispensers should also be trained about good dispensing practice to decrease dispensing errors.
Recommendation
Based on the finding of this study, the following recommendations are forwarded to the concerned body.
To make dispensing rational:
a. The dispensers should give the drug with the write indication, dose, strength and
b. Instruction because he|she is the last person in the health care services to those patient contacts.
c. The dispensers should have relevant and up to date information about drug
d. The control authority should make the regulation in appropriate way and with in short period .The entire dispenser should give relevant and good in to the patient.
e. Pharmacies should have enough staff and stock in the dispenser.
f. The dispenser should have quick reference in dispensing area and there should be drug information centers in the health facilities.
g. Dispensing should be carried out only by pharmacy professional.
h. It is essential that under graduate and postgraduate education of pharmacists and other health care professional aim to improve the quality of dispensing.
i. The prescriber should prescribe the drug clearly and legible.
Study limitations
• Some of the responses provided by the respondents may not reflect their actual practice.
• Lack of cooperation from some respondent those who are concerned giving information.
Acknowledgement
The authors' heartfelt thanks go to Jimma University, Institute of Health Sciences for facilitating this research. We would also like to acknowledge all Shenen Gibe Hospital and Mendera Kochi Health Center staffs for helping us in data collection.
References
- WHO (2001) How to develop and implement a national Drug policy (2nd edn). World health organization, Geneva, Switzerland.
- HKMA (2002) Good Dispensing manual (2nd edn): Hong Kong medical associations.
- HAI AP press release (2008) Rational use of Medicines, Health Action international Asia pacific.
- Collette M, Aulton E (1991) Pharmaceutical practice. ELBS edition. Sngapore: Longman Singapore publishers; Singapore, p. 71.
- Yerevan (2001) The TRIPS Agreement and Access to essential medicines.
- (2001) Progress in implementation of national drug policy in Armenia during 1994-2004, Report on working meeting, agency on drug and medical technology Yerevan.
- Moula C, Abeye J, somes P, Maritoux J, Goumba A (2008) Prescribing and dispensing generic drugs in the Membere-Kadeihealth district of the central Africa Republic. Med Trop mars 68(2): 149-154.
- Kennedy AG, Littenberg B (2004) A modified out Patient Prescription form to Reduce Prescriptions errors. Joint commission Journal of quality and safety 30(9): 480-487.
- Zwarenstien MF, Dainty KN, Quan S, Kiss A, adhikari NK (2007) a cluster randomized trial evaluating electronic Prescribing in ambulatoty care setting” biomrd central trials. 8: 28.
- Teferra A, Alemayehu W (2001) Patient non-compliance with drug regimens for chronic disease in North -west Ethiopia. Ethiopia journal of health development 159(3): 185-192.
- Teferra A, Alemayehu W (2000) patient noncompliance with therapeutic regiments and the factor of noncompliance in Gonder. Ethiopia journal of health development (1491): 1-6
- Stenson B, Syhakhang L, Eriksson B, Tohomson G (2001) Real world pharmacy: assessing the quality of private pharmacy practice in the Lao peoples Democratic republic. soc Sci Med 52(93): 393-404.
- Trap B (2008) Zimbabwe essential Drugs action program, ministry of Health and child welfare. International conferences on improving use of medicines (icium): practice of dispensing doctor's drug use and health economics.
- Ameyaw A, Margaret M, Ofori A, David G (2007) International conferences on improving use of medicines (ICIUM): The impact of three forms of educational interventions on dispensing practices.
- Hale ZT, Ahmet A, Sule O, Sanda C, Sena F (2010) SEzen, Meral Keyer- Uysal The pharmacy prommunity pharmacacists in Turkey.
- Francisco C (2005) Manual Tome-Otero/Bahi Takkouche, Juan Jesus Gestal-Otero,influence of pharmacists opinions on their dispensing Medicines without requirement of a doctor's prescription. Gaceta Sanitaria Barcelona Gac sanit 19(1): 2005.






























