Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis Testis
Xiaowen Guo, Zhengyang Han, Huimin Zhu and Zhengguang Chen*
Department of Ultrasound, the First Affiliated Hospital of Zhengzhou University, Zhengzhou University, China
Submission: June 26, 2023; Published:July 14, 2023
*Corresponding author: Zhengguang Chen, Department of Ultrasound, the First Affiliated Hospital of Zhengzhou University, Zhengzhou, China, Email: czg916@163.com
How to cite this article: Xiaowen G, Zhengyang H, Huimin Z, Zhengguang C. Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis Testis. Glob J Reprod Med. 2023; 10(2):8055779. DOI: 10.19080/GJORM.2023.10.555785.
Abstract
Well-differentiated papillary mesothelioma (WDPM) is an uncommon mesothelial tumor rarely from the tunica vaginalis of testes. Hereinafter, we report a 38-year-old male with ultrasound findings of several lumps located within the testicular sheath and testicular hydrocele. The patient underwent surgery to remove the mass, and the histological characteristics suggested WDPM.
Keywords: Well-differentiated papillary mesothelioma; Tunica vaginalis testis; Ultrasound
Abbreviations: WDPM: well-differentiated papillary mesothelioma
Case Presentation
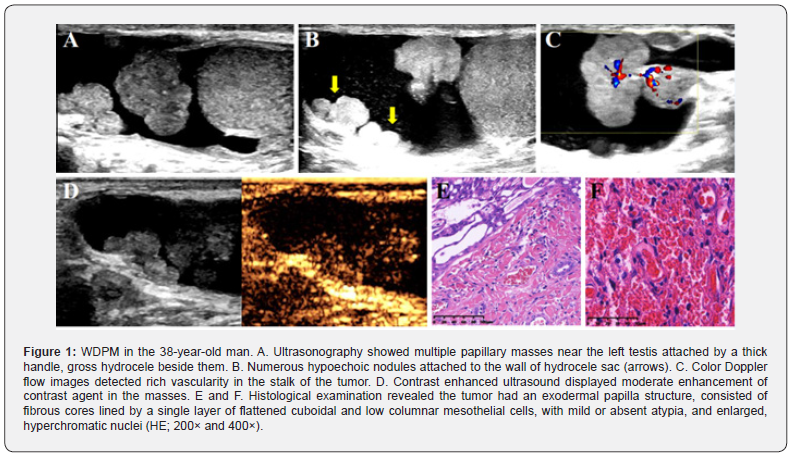
A 38-year-old man presented with a history of chronic painless enlargement of the left hemiscrotum for 2 months. He denied any trauma, urethral discharge, sexual or asbestos exposure, and there was no previous smoking or alcohol use. Physical examination revealed a grossly enlarged left hemiscrotum with fluctuance and both testes were palpable and appeared normal size. The laboratory examination were all within normal limits. Ultrasonography demonstrated fluid accumulation in the left tunica vaginalis and multiple polypoid masses, 14 mm×13 mm maximum size, located on the tunica vaginalis testis (Panel A and B). Color Doppler flow images detected vascularity within both the stalks and the masses (Panel C). Contrast enhanced ultrasound displayed moderate enhancement of contrast agent in the masses (Panel D). The above lesions were confirmed by pelvic magnetic resonance imaging, which showed no evidence of metastatic disease. Initially, a paratesticular neoplasm was suspected. A left hydrocelectomy and excisional biopsy of the tunica vaginalis masses were performed. Pathological examination revealed multiple soft papillary lesions ranging from 1 mm to 14 mm in diameter on the tunica vaginalis testis, which showed pale yellow surfaces with firm and smooth palpation. Microscopically, the masses were composed of multiple branching, papillary structures with a fibrovascular core, the former lined with a single layer of bland cuboidal cells. The matrix was edemaous and mucoid, and no necrosis, hemorrhage or atypical mitosis were observed (Panel E and F). Given the lack of evidence for significant stromal invasion, a diagnosis of WDPM was made. The recovery from surgery was uneventful and the patient was discharged a week later from our hospital. At his 3-month follow-up visits, he remained asymptomatic without any adverse events.
Mesothelioma is a tumor derived from mesothelial cells covering the visceral surface, which usually develops in the peritoneum and pleura [1]. Paratesticular mesothelioma accounts for less than 1% of all mesothelioma cases, which could be further subdivided into malignant mesotheliomas, mesothelial hyperplasia, and WDPM [2,3]. WDPM rarely involves the tunica vaginalis, and approximately one-third of cases have a history of asbestos exposure [4]. Most WDPM patients suffer from scrotal pain or swelling, while the most common presenting symptom is hydrocele. Typically, the lesion is characterized as a firm, painless testicular mass from a few millimeters to 3 cm size, often occurring in conjunction with recurrent hydrocele, mostly unilateral [5]. Microscopically, it shows dendritic papillary structure with a single layer of flat epithelial cells. Immunohistochemistry is positive for cytokeratin and epithelial membrane antigens [6,7]. A small percentage of patients present with metastatic disease, most commonly involving the retroperitoneal, inguinal, and iliac nodes [8]. For WDPM, ultrasound is the preferred screening method because of its simple and economical advantages. On the ultrasound imaging, WDPM generally appears massively enlarged scrotum with thickening of overlying skin, irregular edge effusion in the scrotum, and multiple soft-tissue lesions of mixed echo attached to the scrotal wall and extended to the tunica vaginalis. A small amount of blood flow signals can be seen in the lesions on color Doppler flow images [9].
WDPM is considered as a lesion of low malignant potential, and radical orchiectomy is the preferred treatment, which can achieve good survival results. Given the chance of progression to a truly malignant lesion, radical orchiectomy is the preferred treatment [10]. WDPM is easily differentiated from mesothelial hyperplasia, which usually has no fibrovascular core and lacks papillary structures. Malignant mesotheliomas is highly aggressive and likely to appear local invasion to other scrota structures and distant metastases, which is the reliable feature for malignant mesotheliomas. And only WDPM can display papillary or tubular papillary structures, bland nuclear cytology, infrequent mitoticactivity, single cuboidal epithelium and absence of stromal invasion [11].
As a rare testicular tumor, WDPM usually appears not aggressive and accompanied by an indolent clinical behavior, for which ultrasound is a convenient, fast and efficient diagnostic method. And timely evaluation should be considered in patients with a paratesticular mass with associated hydrocele (Figure 1).
Funding
This work was supported by the Key R&D and Promotion Special Project of Henan Provincial Science and Technology Department (No. 232102311154).
Ethics Approval and Consent to Participate
The hospital ethics committee approval was granted of this case report.
Consent for Publication
Written informed consent of clinical data and image publication was obtained from the patient.
Availability of Data and Materials
Please contact the corresponding author for data on reasonable request.
References
- Fields JM, Russell SA, AndrewSM (1992) Case report: ultrasound appearances of a malignant mesothelioma of the tunica vaginalis testis. Clin Radiol 46(2): 128-130.
- Tolhurst SR, Lotan T, Rapp DE, Lyon MB, Orvieto MA, et al. (2006) Well-differentiated papillary mesothelioma occurring in the tunica vaginalis of the testis with contralateral atypical mesothelial hyperplasia. Urol Oncol 24(1): 36-39.
- Fukunaga M (2010) Well-differentiated papillary mesothelioma of the tunica vaginalis: a case report with aspirate cytologic, immunohistochemical, and ultrastructural studies. Pathol Res Pract 206(2): 105-109.
- Plas E, Riedl CR, Pfluger H (1998) Malignant mesothelioma of the tunica vaginalis testis: Review of the literature and assessment of prognostic parameters. Cancer 83(12): 2437-2446.
- Parcesepe P, Sina S, Zanella C, Pancione M, Giuliani J, et al. (2016) Case Report of a Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis in an Undescended Testis With Review of Literature. Int J Surg Pathol 24(5): 443-447.
- Erdogan S, Acikalin A, Zeren H, Gonlusen G, Zorludemir S, et al. (2014) Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis: A Case Study and Review of the Literature. Korean J Pathol 48(3): 225-228.
- Gan AML, Plantinga P, Punjani N, Hussey A, Power N (2018) Images - Well-differentiated papillary mesothelioma of the tunica vaginalis. Can Urol Assoc J 12(9): E425-E427.
- Ko KWS, Tse KS, Shek KW, Hau MN , Ting SH (2018) Well-differentiated papillary mesothelioma of tunica vaginalis testis of unknown malignant potential: Sonographic appearance. J Clin Ultrasound 46(5): 364-367.
- Mathew BS, Jyothirmayi R, Nair MK (1996) Case report: malignant mesothelioma of tunica vaginalis testis presenting with spinal metastasis--report of two cases. Br J Radiol 69(827): 1067-1068.
- Trpkov K, Barr R, Kulaga A, Yilmaz A (2011) Mesothelioma of tunica vaginalis of "uncertain malignant potential" - an evolving concept: case report and review of the literature. Diagn Pathol 2011; 6:78.
- Chys B, De Graeve N, Merckx L (2022) Well differentiated papillary mesothelioma of the tunica vaginalis: case report. Acta Chir Belg 1-4.






























