Stress Level and Length of Use Contraception to Premenstrual Syndrome (PMS) Type in Childbearing Age Women
Bambang Hariyadi, Colti Sistiarani*, Eri Wahyuningsih and Siti Nurhayati
Department of Public Health, Jenderal Soedirman University, Indonesia
Submission: April 14, 2023; Published:May 12, 2023
*Corresponding author: Colti Sistiarani, Department of Public Health, Jenderal Soedirman University, Indonesia, Email: coltisistiarani@yahoo.co.id
How to cite this article: Bambang Hariyadi, Colti Sistiarani, Eri Wahyuningsih, Siti Nurhayati. Stress Level and Length of Use Contraception to Premenstrual Syndrome (PMS) Type in Childbearing Age Women. Glob J Reprod Med. 2023; 10(1): 555779. DOI: 10.19080/GJORM.2023.10.555779.
Abstract
The identification of factors related to PMS is still general in nature and has not focused on identifying risk factor related the type of PMS. PMS itself is more experienced by women of childbearing age. The prevalence of PMS types in women of childbearing age is done to be able to map the types of PMS so that their magnitude can be found in the population. This research is a descriptive analytic study with a cross sectional approach. The population in this study were women of childbearing age (15-49 years) who were in the west Purwokerto subdistrict and Sumbang subdistrict. The number of samples in this study were 101 respondents. The sampling technique was purposive sampling. Collect data using interviews with respondents. Data analysis used binomial test and multinomial regression. The results of the study can be explained that there are differences in the proportion of PMS A, H and D types in the population. There is a difference in the proportion between Type H, PMS C, Type A and Type D depending on the length of time using contraceptive and stress level.
Keywords: Premenstrual syndrome; Childbearing age women; Contraception
Introduction
Premenstrual syndrome (PMS) is a condition felt by women before experiencing menstruation, which is characterized by physical changes in the body and emotions that can interfere with daily activities, but will disappear along with the completion of the menstrual phase. The cause of the syndrome can be caused by the role of the hormonal system, nutrition, and environment. PMS generally occurs in women of reproductive age between 20-40 years. The incidence is more in women with higher education because there is a link between stress factors and environmental pressures. Psychological factors, the amount of nutritional intake, and hormonal cycles can affect the incidence of Premenstrual syndrome (PMS) which can cause behavioral, psychological and physical changes in an individual [1].
The causes of PMS are genetic factors, psychological factors and psychological factors such as stress, and lifestyle factors such as diet. PMS symptoms include physical symptoms, emotional symptoms. The types of PMS according to Dr. Guy E. Abraham, obstetrician and gynecologist and UCLA school of medicine, USA, divides PMS according to its symptoms, namely premenstrual syndrome. types A, H, C and D. 80% of premenstrual syndrome disorders including type A. Patients with type H about 60%, premenstrual syndrome C 40% and premenstrual syndrome D 20%. A woman is said to have this type if she experiences more than 1 symptom. Premenstrual syndrome type A (anxiety) is characterized by symptoms such as anxiety, sensitivity, nervous tension, and feelings of instability. Premenstrual syndrome type H (hyperhydration) has symptoms of edema, flatulence, chest pain, swelling of the hands and feet, weight gain before menstruation. Premenstrual syndrome type C (craving) is characterized by a hunger to eat sweet foods (usually chocolate) and simple carbohydrates (usually sugar). Type D premenstrual syndrome (depression) is characterized by symptoms of depression, wanting to cry, weakness, sleep disturbances, forgetfulness, confusion, difficulty in pronouncing words (verbalization), and sometimes even feeling suicidal or trying to commit suicide.
The most studies related to PMS in syndrome were type A category, which was 70 respondents (63.1%), while the least was type D category, which was 10 respondents (9.0%). Severe anxiety was experienced by 59 respondents (53.2%) and the least was mild anxiety, as many as 19 (17.1%) respondents. The results showed that there was a relationship between anxiety levels and PMS syndrome [2]. Previous studies have shown that the global prevalence of PMS is high and about half of women of childbearing age experience this symptom. Given that different tools have been used in the studies and many studies have been designed based on limited samples, therefore, future research needs to consider the prevalence of STDs in different countries of the world [3].
Another study stated that 85.6% of subjects showed PMS symptoms with the severity of PMS in 14% of subjects was high. The most common mood (emotional) and somatic (physical) symptoms were fatigue and lethargy and abdominal pain (72.6% and 62.7%). PMS was significantly associated with dysmenorrhea and the severity of menstrual pain. The high prevalence of this syndrome has an effect on various aspects of life [4]. Premenstrual symptoms occur in 95% of women of childbearing age. Severe and debilitating symptoms such as PMDD occur in about 5% of women. Implants and oral contraceptive pills with estrogen can improve premenstrual symptoms in women, but this evidence is considered insufficient [5].
The results showed that 4.1% of women had severe PMS (six symptoms) and 8.1% were in the moderate PMS category (one to five symptoms). From these results 12.2% of women who reported PMS symptoms could affect their daily lives [6]. Respondents of 23.8% were categorized as having moderate to severe PMS (PMS score 30), and 76.2% had PMS scores <30. Age and genetic factors were found to be associated with PMS severity. Other factors (marital status, economic status, number of parity, history of depressive episodes, history of child abuse, and stress) did not have a correlation with the severity of PMS [7].
One of the significant differences between PMS and premenstrual dysphoric disorder (PMDD) is the severity of the signs and symptoms that occur. Although both can show physical and emotional signs and symptoms, PMDD can be characterized by drastic mood swings, which can interfere with work and relationships with others. PMDD is a category of severe PMS, which can make a woman feel very sad or nervous, have impaired social relationships with family members and friends, and have difficulty concentrating on work or education.
According to research, there is an interaction between premenstrual syndrome, psychological complaints, types of premenstrual syndrome and the use of leave on the productivity of the female workforce. PMS syndrome types can be divided into single and combination. Research has found that low productivity is more common in female workers who have a single PMS syndrome than in combination PMS [8]. The results of the study of respondents who experienced PMS were mostly combined types as many as 76 female students (50%). The results of this study indicate that most of the PMS experienced by female students are combined types, although in theory women generally feel type A [9].
This study aims to determine the proportion of the incidence of PMS type A, PMS type D, PMS type C, and PMS type H in the population of women of childbearing age. This study also wanted to examine factors related to the types of PMS such as the length of use of family planning, types of contraception, stress levels.
Method
This research is a quantitative study using a cross sectional approach with an analytical type of research, namely by identifying the proportions of each type of PMS, namely PMS type A, PMS type D, PMS type C and PMS type H. This research was conducted in Banyumas Regency. The time of the study was carried out in July-September 2020. The study population included women of childbearing age who were in the working area of the Sumbang Health Center and the West Purwokerto Health Center, namely 11,843.
The minimum sample calculation uses the formula, which is 101 WUS. The sample is women of childbearing age who were selected based on inclusion and exclusion criteria.The inclusion criteria are Married woman, women have physical and psychological symptoms related to PMS. The exclusion criteria are women not having normal menstruation, women not using contraception, women not permanently domiciled in the Subdistricts of Sumbang and West Purwokerto The type of PMS is seen from the complaints or physical symptoms experienced by women who appear in the range of 6-10 days before menstruation seen by the type of PMS type Anxiety (A), PMS type Hyperhydration (H), PMS type Depression (D), PMS type Craving ( C) or a combination of AD-type PMS and CH-type combination PMS.
Stress level is seen from the efforts made by WUS in dealing with situations that cause pressure, change and emotional tension. The type of use of hormonal contraceptives is seen from the use of contraceptives which can be seen from the contraceptives used, namely hormonal and non-hormonal contraceptives. The duration of use is seen from the duration/span of women of childbearing age using hormonal contraception in the span of less than 2 years and more than 2 years.
Research ethics has been submitted and received approval from the Ethics Committee of the Faculty of Health Sciences, Jenderal Soedirman University. research ethics has been issued on August 10, 2021 no 525/EC/KEPK/VIII/2021. This study used an instrument in the form of a closed questionnaire, a checklist of PMS type symptoms. Sources of data in this study using primary data and secondary data. Primary data obtained from interviews with respondents using questionnaires and checklists. Secondary data are health profiles of Banyumas Regency, profiles of Puskesmas Purwokerto Barat and Sumbang as well as medical record data for women who use contraception accessed through primary health center.
Univariate analysis was conducted to describe the type of PMS and related factors based on the type of PMS. Bivariate analysis to analyze risk factors for BMI level, daily consumption, daily activities, and contraceptive use seen from the type of contraception and duration of use. The proportion to find out the factors related to the type of PMS is done by using multinomial regression test.
Result and Discussion
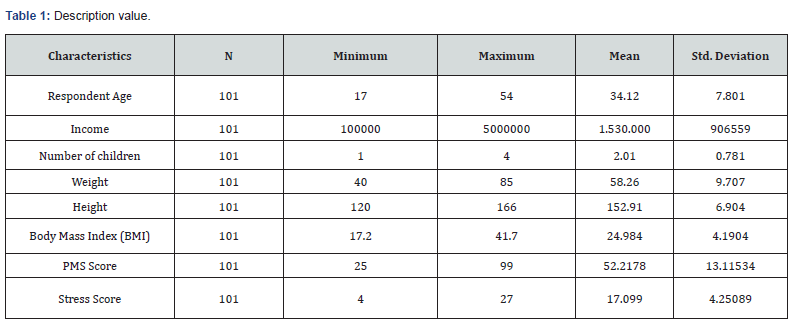
From the table 1, it can be seen that the average age of respondents is 34 years and has an average number of children 2. Most of the respondents have a normal BMI. Respondents have an average PMS score of 52 while the average stress score is 17.
Based on table 2, it can be explained that the proportion of PMS types compared to previous research studies has differences in the types of PMS type A, PMS type D, PMS type H in the population used in this study. The same proportion was found in type C PMS. The proportion value of type A PMS was 0.3, type D PMS was 0.7, type C PMS was 0.6, while type H was 0.6.
Based on table 3, it can be concluded that there is a difference in the proportion of PMS types between Types A and H depending on the duration of family planning use. This can be seen from the p value of 0.000. There is a difference in the proportion of PMS types between types A and H depending on the level of stress. This can be seen from the p value obtained of 0.048. There is a difference in the proportion of PMS types between type D and type H depending on the level of stress. This result can be seen from the p value of 0.049. This result is significant seen from the p value <= 0.05.


Note: Category Reference using PMS Type H.
According to Guy Abraham, the proportions of PMS type A from the research have different proportions, according to Guy Abraham, PMS type A, PMS D type, and PMS type H. PMS type C has the same proportion according to Guy Abraham. According to Guy Abraham 80% of premenstrual syndrome disorders include type A. Patients with type H about 60%, premenstrual syndrome C 40% and premenstrual syndrome D 20%.
The results of the study [2], showed that the proportion value of PMS type A was 63.1%, PMS type D was 9%, PMS type C was 12.6%, PMS type H was 15.3%. The value of this proportion is much different, respondents have PMS type A because more respondents experience severe anxiety levels. The proportions in this study are also different from other studies. The incidence of PMS is mostly a combination of several types of PMS as much as 85.2%. PMS type A (anxiety) as much as 7.7%. PMS type C (craving) was 3.5%, type D (depression) experienced these symptoms as much as 2.1% then the least type was type H (hyperhydration) as much as 1.4%. Respondents whose age is more than 25, namely 100.0% have Premenstrual Syndrome. Married respondents who experienced PMS were 100.0%. All respondents who had given birth experienced Premenstrual Syndrome, which was 100.0%. Psychological stress levels and neuroticism are associated with PMS. PMS cases had earlier menarche and lower body mass index than the control group. PMS occur in a higher proportion of nulliparous women or women who have never given birth. The causative process is reversed, where the presence of premenstrual symptoms results in stress and inadequate coping strategies [10].
PMS can develop into symptoms PMDD. Premenstrual Dysphoric Disorder (PMDD) is a severe form of premenstrual syndrome (PMS) which affects up to 7% of women aged reproduction. So that women with PMDD who are of reproductive age, advised to use contraception and PMDD treatment. PMDD characterized by the occurrence of a cycle of psychological, behavioural and physical premenstrual symptoms lost in the first week of menstruation. Symptoms can start up to 14 days before menstruation, at the time of ovulation or at any time during the luteal phase. The main psychological (mood) symptom of PMDD is characterized by lability or sensitivity of a rejection, increased irritability, irritability, presence of interpersonal conflict, depression, hopelessness or feelings of worthlessness, anxiety, tension, feeling restless [11].
Changes in symptoms that occur in the menstrual cycle are more experienced by the nonhormonal contraceptive group compared to the hormonal contraceptive group. Significant symptom changes in the nonhormonal group are common for individuals who are depressed, irritable or irritability, and fissile symptoms [12,13]. Common symptoms of PMS are breast pain with a percentage of 55.7%, acne with a percentage of 39.2%, and abdominal pain with a percentage of 31.1%. Other reported symptoms of 1.7% include feelings of hopelessness, headaches, insomnia, food cravings, and nausea. Meanwhile, the rarest symptoms are diarrhoea and depression. In users of hormonal contraceptives or oral contraceptives found a higher prevalence of STDs than those who do not use these contraceptives. The prevalence of STDs is significantly higher in contraceptive pill users compared to those who do not use the contraceptive pill.
Conclusion
From this study, it can be concluded that there are differences in the proportion of PMS type A, type H and type D in the population. There is a difference in the proportion between PMS Type H, PMS Type C, PMS Type A and PMS Type D depending on the length of time using contraception and stress levels in women of childbearing age who use contraception.
The importance of women of childbearing age to identify the type of PMS and focus attention to the duration of contraceptive use and stress because these factors are related to the type of PMS they have. With regard to policies and services on contraceptive use, it is necessary to attention to the duration of hormonal contraceptive use related to the incidence of PMS types in family planning acceptors because there is a relationship with PMS types.
Acknowledgments
We thank LPPM Jenderal Soedirman University for financing this research with BLU funds in 2021.
References
- Rodiani, Annisa Rusfiana (2016) Hubungan Premenstrual Syndrome (PMS) Terhadap Faktor Psikologis Pada Remaja. Medical Journal of Lampung University 15 (1): 18-22.
- Siyamti S, Pertiwi HW (2011) Hubungan Antara Tingkat Kecemasan Dengan Sindrom Premenstruasi Pada Mahasiswi Tingkat II Akademi Kebidanan Estu Utomo Boyolali. Jurnal Kebidanan 3(1): 29-36.
- Moghadam AD, Sayehmiri K, Delpisheh A, Kaikhavandi S (2014) Epidemiology of Premenstrual Syndrome (PMS)-A Systematic Review and Meta-Analysis Study. J Clin Diagn Res 8(2): 106-109.
- Naeimi N (2015) The Prevalence and Symptoms of Premenstrual Syndrome under Examination. Journal of Biosciences and Medicines 3: 1-8.
- Kwan I, Onwude JL (2015) Premenstrual Syndrom. BMJ Clin Evid 2015: 0806.
- Potter J, Bouyer J, Trussell J, Moreau C (2009) Premenstrual Syndrome Prevalence and Fluctuation over Time: Results from a French Population-Based Survey. Journal Women Health 18(1): 31-39.
- Anggrajani F, Muhdi N. Korelasi Faktor Risiko dengan Derajat Keparahan Premenstrual Syndrome pada Dokter Perempuan.
- Sulistiyani F, Seweng A, Tahir AM (2019) The Effect of Premenstrual Syndrome On Female Workers’ Productivity In PT. Bogatama Marinusa, Makassar City. Hasanuddin International Journal of Health Research Sciences 1(1): 29-35.
- Nisa F (2018) Tipe Gabungan Mendominasi Jenis Pre Menstrual Syndrome (Pms) Pada Mahasiswi Tingkat I Dan II Prodi DIII Kebidananunusa. Jurnal Ilmiah Kesehatan 11(1): 33-37.
- María Del Mar Fernández, Carlos Regueira-Méndez, Takkouche B (2019) Psychological factors and premenstrual syndrome: A Spanish case-control study. PLoS ONE 14(3): e0212557.
- Rapkin AJ, Korotkaya Y, Taylor KC (2019) Contraception counseling for women with premenstrual dysphoric disorder (PMDD): current perspectives. Open Access Journal of Contraception 10: 27-
- Mufida E (2015) Faktor yang Meningkatkan Risiko Premenstrual Syndrome pada Mahasiswi. Jurnal Biometrika dan Kependudukan 4(1): 7-13.
- Saryono, Sejati W (2009) Sindrom Premenstruasi, Nuha Medika, Yogjakarta.






























