Ectopic Pregnancy After Hysterectomy: A Case Report and Review of the Literature
Sarah Shehzad, Ismini Panayotidis, Michael Magro, Rekha Wuntakala and Kunal Rathod*
Barking, Havering and Redbridge University Hospitals NHS Trust, United Kingdom
Submission: April 27, 2023; Published:May 11, 2023
*Corresponding author: Kunal Rathod, Consultant Obstetrician and Gynaecologist, Barking, Havering and Redbridge University Hospitals, London, United Kingdom, Email: kunal.rathod1@nhs.net
How to cite this article: Sarah S, Ismini P, Michael M, Rekha W, Kunal R. Ectopic Pregnancy After Hysterectomy: A Case Report and Review of the Literature. Glob J Reprod Med. 2023; 10(1): 555778. DOI: 10.19080/GJORM.2023.10.555778.
Abstract
Ectopic pregnancy occurs in 1-2% of all pregnancies and involves an ovum implanting outside of the uterus. The most frequent site of ectopic pregnancy is the fallopian tubes, followed by the ovary, and occasionally can occur within the abdomen. Ectopic pregnancy after hysterectomy has been reported but is extremely rare, making it a diagnostic challenge and increasing the risk of morbidity and mortality. Herein we report the case of a 39-year-old woman who developed an ectopic pregnancy nine years after a sub-total hysterectomy. A literature review was also conducted to explore the available research on this extremely scarce event. The review suggests that the incidence of ectopic pregnancy after hysterectomy is extremely low, but it is a severe and life-threatening condition and requires a high index of suspicion to diagnose it. There is a need to share this case to alert medical practitioners of the potential for ectopic pregnancy after hysterectomy to ensure it is considered when women of childbearing age present with abdominal pain.
Keywords: Caesarean hysterectomy; Ectopic pregnancy; Sub-total hysterectomy; Salpingectomy
Abbreviations: HCG: Human Chorionic Gonadotrophin; SVD: Spontaneous Vaginal Delivery; TVUS: Transvaginal Ultrasound
Introduction
Ectopic pregnancy, which affects 1-2% of all pregnancies, is a well-known pregnancy problem [1]. Ectopic pregnancy is when an ovum that has been fertilized implants somewhere other than the uterus, most frequently in the fallopian tubes. The cervix, ovaries, and abdominal cavity are less typical sites for implantation. Ectopic pregnancies have the potential to be fatal since they might result in bleeding and rupture [2,3].
Ectopic pregnancies following hysterectomy, which involves removal of the uterus, have been seldomly reported and present a particular diagnostic challenge for clinicians. A hysterectomy is often recommended for the treatment of a number of gynaecological disorders such fibroids, irregular uterine bleeding, cancer and fatal bleeding during pregnancy and delivery. Women who have had hysterectomy are no longer able to carry a baby to term; as a result, any pregnancies they do have are typically ectopic [4-6]. Nevertheless, since the uterus, as well as frequently the fallopian tubes and the ovaries, have been removed, an ectopic pregnancy following hysterectomy is uncommon.
This case report examines an ectopic pregnancy that occurred in a woman nine years after a sub-total hysterectomy and evaluates the literature on this unusual occurrence.
Case Report
A 39-year-old female presented to hospital with lower abdominal pain. She initially presented to accident and emergency department, and on finding a positive urinary HCG, she was referred to the gynaecology team. She was P2 with 2 previous SVDs (spontaneous vaginal deliveries). At her most recent delivery, 9 years previously, she suffered a major post-partum haemorrhage of 4 litres due to uterine atony and was taken to the operating theatre. She subsequently underwent a subtotal hysterectomy with conservation of her fallopian tubes and ovaries. She had been amenorrhoeic for the last 9 years following this.
Her abdominal pain had been ongoing for 2 weeks in total. It was crampy in nature and worsening over the last day, with radiation to right upper quadrant of the abdomen and her right shoulder. She had a recent urine infection treated by her GP with 7 days of antibiotics. She denied vaginal bleeding, nausea/ vomiting, and had last opened her bowels the day before. She had no background of ectopic pregnancies, or previous sexually transmitted infections. She was not on any contraception and continued to have smear tests which were normal.
Her past medical history included immune thrombocytopenia purpura and a small simple ovarian cyst seen on TVUS a year before. She was not on any regular medication, had no medication allergies and was a non- smoker. Clinically, she was haemodynamically stable. Examination elicited tenderness over the suprapubic region and right iliac fossa. Speculum examination and bimanual vaginal examination were unremarkable. Her Haemoglobin was 12.1mg/dl, with a normal white cell count, and mildly raised CRP of 18. A serum Beta-HCG was performed and found to be 2638. Her urine dipstick showed Nitrites, blood (2+) and ketones (2+). Her lactate was 0.5 microgm/dl.
She underwent a TVUS which found a mass in the right adnexa measuring 27 x 27 x 25mm. A cervical stump was noted, and there was an absence of uterus. No free fluid was found in the pelvis. The team requested tumour markers and serum progesterone given the patient’s history. An MRI was requested to rule out possible differential diagnoses, including ovarian tumour. The tumour markers returned as normal.
Throughout her inpatient episode, the patient remained stable and free of pain. A repeat scan was ordered the next day for second opinion which demonstrated an ectopic pregnancy in the right adnexa (Figure 1) of 32x30mm with the gestation sac and yolk sac visible. There was free fluid in the pelvis, largest pool measuring 52 x 26mm. Number of ectopic pregnancy post hysterectomy reported in the past 50 years [7] (Figure 2).
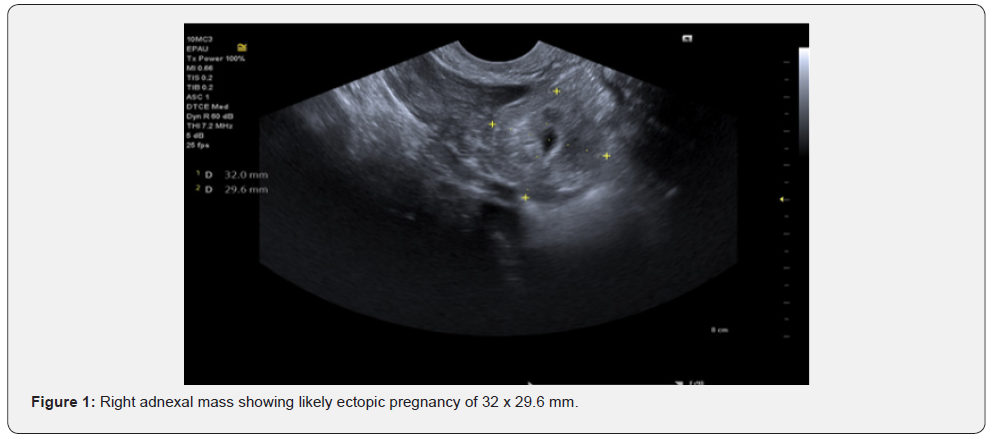
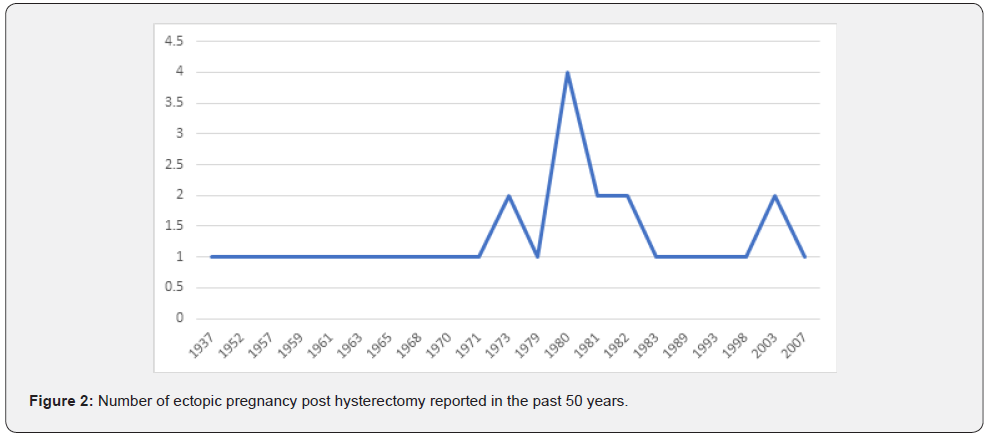
Repeat blood tests showed a rising Beta-HCG of 3925Miu/ml and a progesterone level of 21ng/mL. The patient was clinically stable, and her pain had settled with analgesia, so the team awaited the MRI report. MRI findings include hematosalpinx, a hemorrhagic or heterogeneous mass in the right adnexa, bloody ascites, and tubal dilatation and wall enhancement. The team discussed conservative vs medical vs surgical management with the patient, and a decision was made to take the patient to theatre. She was appropriately consented for a laparoscopic removal of an ectopic pregnancy +/- salpingectomy +/- oophorectomy. Palmer’s point entry was used and a right tubal ectopic of 60 x 40 mm was found (Figure 3 & 4). Appendix was noted to be normal.
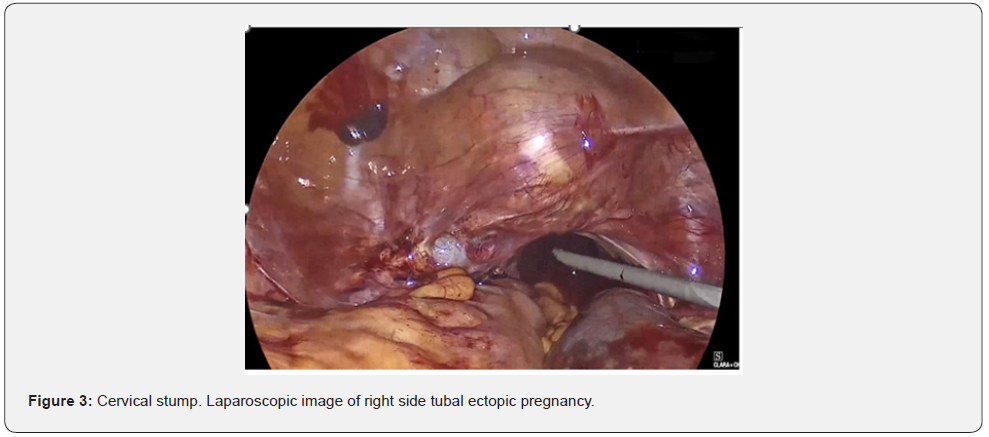
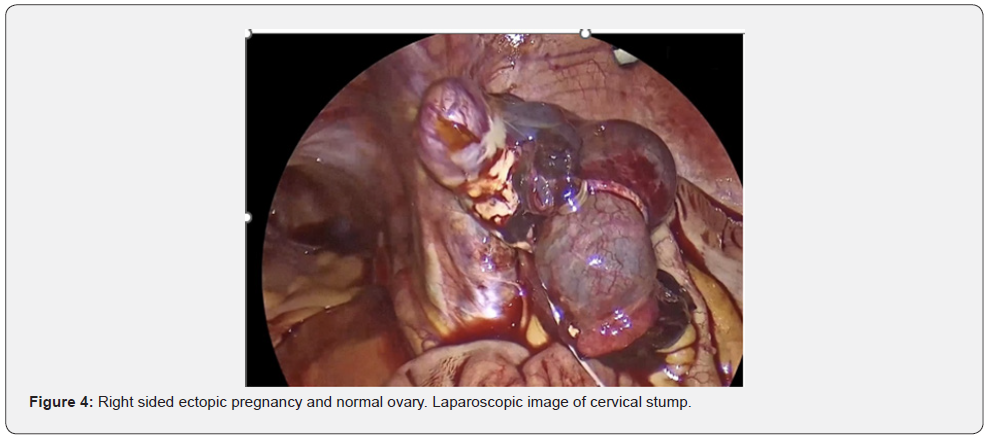
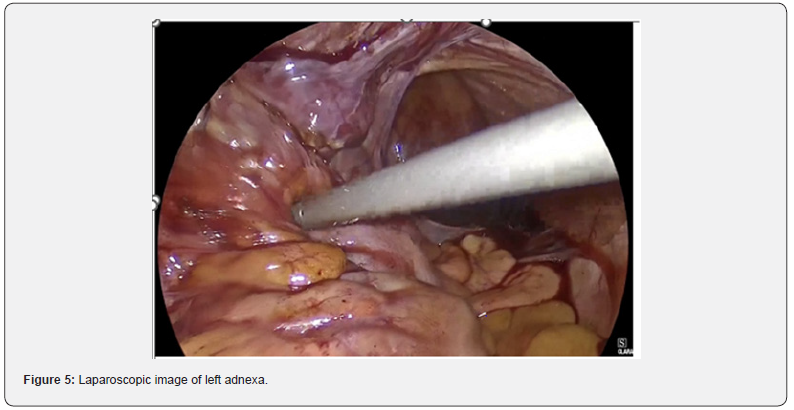
She underwent omental adhesiolysis, right pelvic side wall and ovarian adhesiolysis and a right complete salpingectomy, plus minimal left sigmoid adhesiolysis and suction of 300ml of haemoperitoneum. The left fallopian tube and ovary (Figure 5) were buried under the bowel due to adhesions and were therefore left in situ. A drain was inserted. Her total blood loss was 300ml from the haemoperitoneum with minimal blood loss from the surgery.
She was clinically well the next day, with stable observations. Her drain had minimal output and was removed on day 2. Her post op Hb was 10.4mg/dl. Her histology showed cells of endometrium associated with ectopy: any type of endometrium without trophoblasts may be associated with ectopic pregnancy. Beta HCG 2 weeks post op was 20 mIU/ml. She was discharged on day 2 post op.
Results
A literature review was conducted to identify the available reported research on post-hysterectomy ectopic pregnancy using the search terms “ectopic pregnancy”, “ectopic pregnancy after hysterectomy”, “early presentation”, “late presentation”.
The databases searched were PubMed, Google Scholar and ResearchGate and PMC looking for literature published between January 2000 to March 2023. Only English language papers were reviewed. Case reports, case series and other research papers were included, which identified a total of 57 reported cases of post-hysterectomy ectopic pregnancy worldwide.
Discussion
The implantation of a fertilized egg outside the uterus is referred to as an ectopic pregnancy. Although it is uncommon after a hysterectomy, this is a medical emergency since it can have significant consequences. There is a dearth of research on the prevalence, diagnosis, and treatment of ectopic pregnancy following hysterectomy.
An ectopic pregnancy after hysterectomy happens when a sperm fertilizes an ovum produced from either ovary and implants on the extraperitoneal or peritoneal surface of the abdominal cavity, according to a case report written by Onwugbenu et al. [7, 8]. The authors emphasized the significance of detailed analysis and the identification of a high-risk group for ectopic pregnancies following hysterectomy.
A research by Bansal et al. [5] also sought to determine the prevalence of an ectopic pregnancy following hysterectomy. Between 2005 and 2019, the researchers reviewed all ectopic pregnancies in women who had previously undergone hysterectomies. Six individuals out of a total of 35 had embryos implanted in the distal fallopian tube. The scientists came to the conclusion that although ectopic pregnancy following hysterectomy is uncommon, it can happen in women who still have fallopian tube tissue.
Shao et al. [9] conducted a systematic review which involved 57 individuals in all, with abdominal discomfort being the most common complaint. The majority of patients had surgical management, and implantation in a surviving fallopian tube was typical. Regardless of whether a woman has had a hysterectomy, a high index of suspicion and a low threshold for a -hCG pregnancy test should be advised in all cases when a woman presents with clinical indications of an ectopic pregnancy. Earlier diagnosis and less problems may result from this.
Ectopic pregnancies following hysterectomy may have a greater risk of rupture, haemorrhage, and mortality, according to Cohen’s et al. [10] research. Transvaginal ultrasonography is thought to be the first imaging method for ectopic pregnancy identification, with a diagnostic accuracy rate of 90.9%. A alternative imaging method that might be used, MRI, has a 96% accuracy rate for making diagnoses. Both imaging techniques were applied in this case report for surgical planning and diagnostic needs, both of which were essential in constructing the overall clinical picture. In circumstances of exceptional or unusual pregnancies, the development of such diagnostic procedures early in the gestation has enabled treatment to transition predominantly from dramatic surgical therapy to more conservative, less invasive approaches [11].
The fundamental reasons appear to be linked to three different processes. One technique involves fistulous passages between the vaginal dome and the peritoneum or the Fallopian tube. Hematomas or pelvic infections close to the vaginal dome may thus promote this fistulisation. A second mechanism that can promote ectopic pregnancy is the extension of the Fallopian tube into the vagina, which results in a link between the vagina and the tubum. Vaginal hysterectomies, when adnexal localization is not specifically regulated, may have a greater prevalence of this prolapse than other types of hysterectomies. It’s also possible that sperm to enter the uterus more easily because cervical permeabilization still can persists after supracervical hysterectomies [6].
In this case, although the diagnosis is clear retrospectively, the confusion surrounding a positive BHCG result in a woman with a hysterectomy caused a delay in definitive treatment and a search for other possible causes. The need for clinicians to be made aware of this potential diagnosis in women of a childbearing age is essential if earlier diagnosis and treatment is to occur.
In conclusion, it is uncommon for an ectopic pregnancy to be originally considered as the cause of a woman’s abdominal pain following a hysterectomy, although it can occasionally be identified in the operating room or during the final pathologic analysis of a surgical material. Although doctors must maintain a high threshold of suspicion, any woman who complains of stomach pain and has intact ovaries should be tested for pregnancy. Effective contraception and avoiding surgery during the periovulatory or luteal phases of the menstrual cycle, which is likely influenced by the type of the treatment and the existence of a remnant, can prevent early-presenting ectopic pregnancies.
References
- Fylstra DL (2015). Ectopic pregnancy after hysterectomy may not be so uncommon: A case report and review of the literature. Case reports in women’s health 7: 8-11.
- Ahmed DM, Fetene AA, Asres EM, Mekonnen AW, Mamuye HG (2019) Cervical stump pregnancy 6 years after subtotal hysterectomy: a case report. Journal of Medical Case Reports 13(1):135.
- Villegas E, González-Mesa E, Benítez MJ, Luna S, Gómez C, Marsac A, et al. (2014) Tubal ectopic pregnancy two years after laparoscopic supracervical hysterectomy. BMC Women’s Health 14(1): 69.
- Anis M, Irshad A, Ackerman S (2013) Late Occurring Ectopic Pregnancy in a Posthysterectomy Patient. Case Reports in Obstetrics and Gynecology 2013: 975196.
- Bansal S, Saini M, Harsh M, Kaur A, Chaturvedi J (2010) Is ectopic pregnancy possible after hysterectomy? Fertility and Sterility 94(1): 350.e5-350.e7.
- Vagg D, Arsala L, Kathurusinghe S, Ang WC (2018) Intramural Ectopic Pregnancy Following Myomectomy. J Investig Med High Impact Case Rep 6: 2324709618790605.
- Fylstra DL (2010) Ectopic pregnancy after hysterectomy: a review and insight into etiology and prevention. Fertility and Sterility 94(2): 431-435.
- Onwugbenu NMA (2020) Ectopic Pregnancy after Hysterectomy: A Case Report of Ectopic Pregnancy 7 Years after Postpartum Hysterectomy. R I Med J 103(8): 50-52.
- Shao EX, Hopper K, McKnoulty M, Kothari A (2018) A systematic review of ectopic pregnancy after hysterectomy. Int J Gynaecol Obstet 141(2): 159-165.
- Cohen A, Shi D, Keraney E, Stankard B, Nelson M (2022) Ultrasound in the Emergency Department Identifies Ectopic Pregnancy Post Hysterectomy: A Case Report. Clin Pract Cases Emerg Med 6(2): 129-132.
- Barhate KP, Domkundwar S, Patil N, Pai B (2009) Sonographic diagnosis of ectopic pregnancy 2 years after total hysterectomy. Journal of Clinical Ultrasound 37(6): 347-349.






























