Fulminant Peritonitis Following Second Trimester Spontaneous Abortion; Case Report, 2023
Okbu Frezgi1*, Berhe Tesfai1, Mhamoud Mohmed1 and Khalid Hussein2
1Department of Obstetrics and Gynecology, Orotta College of Medicine and Health Science, Eritrea
2Orotta College of Medicine and Health Science, Eritrea
Submission: February 09, 2023; Published:February 24, 2023
*Corresponding author: Okbu Frezgi, Department of Obstetrics and Gynecology, Orotta College of Medicine and Health Science, Ministry of Health, Asmara, Eritrea
How to cite this article: Okbu Frezgi*, Berhe Tesfai, Mhamoud Mohmed and Khalid Hussein. Fulminant Peritonitis Following Second Trimester Spontaneous Abortion; Case Report, 2023. Glob J Reprod Med. 2023; 9(4): 555768. DOI: 10.19080/GJORM.2023.09.555768.
Abstract
Background: Sepsis Following Abortion Is Usually a Feature of Induced Abortion, Especially When It Is Performed Under Unhygienic Conditions And By Untrained Person. Although Extremely Rare, Spontaneous Abortions Can Result Into Severe Sepsis And Endanger Life of the Pregnant Woman.
Case Report: A 30 year old multiparous mother was admitted with history of spontaneous abortion at 18 weeks gestation at nearby hospital in teseney, eritrea on 21/03/2022. It was planned pregnancy that ended up in inevitable abortion which was attended by general practitioners and midwives in the hospital and discharged after 48 hours. A week later, on 28/03/2022, she was re-admitted again with a complaint of diffuse abdominal pain, distention and shortness of breath. Despite a week course of broad spectrum antibiotics in the hospital, abdomen was progressively distended, and she was referred to orotta national maternity referral hospital. explorative laparotomy was done and about three liters of serous fluid with foul smelling debris was evacuated from the abdomen. Extensive bowel adhesion was found and gentle adhesion lysis was done. parietal peritoneum was red to black in color and uterus and ovaries were found healthy. on postoperative third day, she developed pulmonary embolism and transferred to intensive care unit. after a month of medical and surgical management, she was discharged home with full improvement.
Conclusion: The case is presented because of its rarity in regards to primary etiology and severity of sepsis. The onset was acute that may end in death if urgent interventions were not done. Clinicians should high index of suspicion for these rare associations in which the pathogenesis is not yet known.
Keywords: Fulminant; Abortion; Peritonitis; Maternal mortality; Eritrea
Introduction
Abortion associated with clinical evidence of infection of uterus and its content is usually considered as septic abortion [1]. Clinical features of the condition include pyrexia, offensive or purulent vaginal discharge, and other evidence of pelvic infection [1]. Severe degree of sepsis following spontaneous abortion is rare [2]. Incomplete evacuation of uterus and trauma to the uterus are predisposing factors for post-abortal sepsis [3]. Complications of unsafe abortion are particularly unsavory because majority of these females come from a place of shame and ostracization to have these clandestine procedures done by unskilled workers. These unskilled personnel use unsanitary sharp instruments, exposing patients to the highest form of injury and trauma. There is no consensus on the particular procedure to be done in the setting of bowel injury following unsafe abortion [4].
Uterine infection can spread to the pelvis or outside the pelvis. Spread of infection depends on severity of infection, virulence of organisms and immune response of the patient. Complications like peritonitis, endo-septic shock, renal failure and disseminated intravascular coagulation may endanger life following severe post-abortal sepsis [3]. Perforation of the uterus and entry into the peritoneal cavity with these heavily contaminated devices/agents kickstarts a long and turbulent septic illness which may require the intervention of the general surgeon [4]. A rare fatal combination of disseminated tuberculosis peritonitis and ARDS following spontaneous abortion was reported [5].
Case Report
This 30 years old gravidity 4 parity 3, married, housewife mother with 18 weeks of gestation by lMP was admitted in nearby community hospital, referred from a health station in her rural area with the impression of first trimester bleeding due inevitable abortion. The patient experienced abdominal cramps with scanty vaginal bleeding and admitted on 21/03/2022 and expelled non-alive fetus. Since there was no remnant tissue and expulsion of the fetus and placenta was complete, evacuation and curettage was not done for her in the hospital. After staying two days in the hospital, she was discharged home with doxycycline 100mg bid for 10 days, iron for three months and oral contraceptive pills for three cycles. A week after her discharge, she developed high grade fever, abdominal pain, vomiting and generalized body weakness. But, she denies any history of vaginal bleeding, foul smelling vaginal discharge and other obstetric or gynecologic problems. She is housewife and, as she and her family reported that the pregnancy was planned and wanted. She was re-admitted again in the hospital with a working diagnosis of post abortion sepsis and intravenous ceftriaxone 1g IV BIB, metronidazole 500mg IV TID and gentamicin 80mg iv TID was given for a week. Despite these broad spectrum antibiotics, her condition deteriorates and she was referred to orotta national maternity referral hospital for further management on 06/04/2022.
During her arrival to orotta national maternity referral hospital, she was toxic and was in mild respiratory distress with vital signs of blood pressure 100/50mmhg on right arm semisitting position, pulse rate 90 beats/minute, temperature 37.5oc and respiratory rate 22 breaths/minute. She had grossly distended abdomen, generalized tenderness and rebound tenderness with decreased bowel sounds. On per-vaginal examination, there was no discharge but she had adnexal fullness and cervical motion tenderness. Patient was admitted as a case of diffuse post abortion peritonitis and, the antibiotics were continued. She was investigated with CBC several times and maximum WBC count being 14,000 with neutrophil shift of 80%, and hemoglobin of 12.4g/dl. Trans-abdominal ultrasonography of abdomen and pelvis showed empty uterus with massive fluid in all abdominal quadrants. Peritoneal fluid analysis showed no organism, and gram stain was negative for AFB and increased cell count of 85% neutrophils with 15% lymphocytes. Cytology of the peritoneal fluid indicated peritoneal hemorrhagic background with many neutrophils but no malignant cells with overall features suggested suppurative inflammation.
Next day of her admission in the ward, her condition deteriorates, and her vital signs started to be deranged significantly. Surgical and gynecological departments decide for explorative laparotomy. Under general anesthesia aseptic technique, with midline infraumblical abdominal incision, around 3000l of serous anginous fluid was sacked. Parietal peritoneum was found rough, red to black in color (Figure 1 & 2).
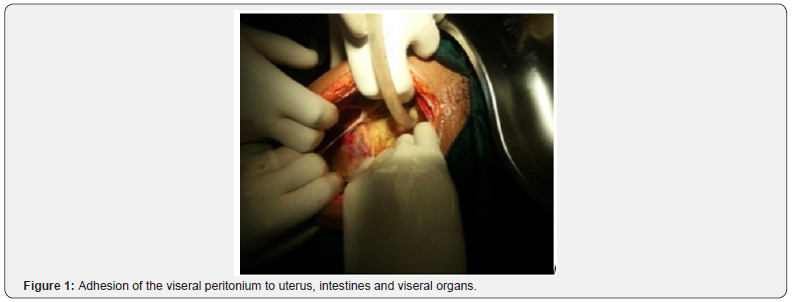
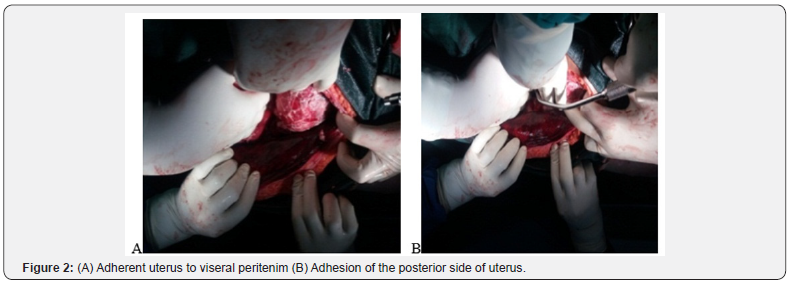
There was also multiple tissue debris in the right lower quadrant with diffuse adhesion of the intestines. Gentile adhesion lysis starting from stomach up to distal colon was done and an adhered retrocecal non-perforated, non-inflamed appendix was removed. Later, uterus and fallopian tubes were explored and the external surface of the uterus was found thread like whitish materials (Figure 2). No signs of perforated cystic materials and found normal without signs of uterine perforations. After full instrument and gauze count, drainage and nasogastric tube was secured intra-operatively and abdomen was closed in layers.
Postoperatively, she was on triple iv antibiotics, dressing and other supportive management. Her condition was improving gradually and she was also put under prophylactic dose of unfractionated heparin. Unfortunately, at her postoperative third day, she experienced sudden onset of dyspnea and restlessness. Pulmonary embolism was entertained and the patient was transferred to intensive care unit for better management and possible mechanical ventilation.
In the intensive care unit, patient was treated for pulmonary embolism and sepsis with heparin, cloxacilline, and clindamycin iv antibiotics, continuous oxygen supplement. She showed improvement and was discharged following full recovery after about one month stay in the hospital. On subsequent followups she was doing her regular daily activities and advised on her condition.
Discussion
Fulminant peritonitis following spontaneous abortion is a rare entity. In our case induced abortion (criminal) was suspected, but history was against it as she was married, housewife and pregnancy was planned. Perforation of the uterus and entry into the peritoneal cavity with heavily contaminated devices like curettage can lead to diffuse peritonitis. But as the patient and referral paper said in our case evacuation and curettage was not done which could predispose her to spontaneous peritonitis. This was similar to a previous case report [2]. Usually, spontaneous peritonitis follows induced abortions or spontaneous abortions complicated by evacuation and curettage.
The progressive abdominal distention was of short duration within 10 days, and the accompanying symptoms of fever and lower abdominal pain precede the distention. The possible pathogenetic processes was fast and not clear. Similar incidence was reported in a case report with diffuse abdominal pain of 2-week duration, massive ascites and prolonged intermittent fever suffered from a spontaneous abortion of 20-week gestation. [5] another study reported distension of abdomen, breathlessness and high grade fever following day of abortion. [2] this acute onset of spontaneous peritonitis would be fatal if urgent medical and surgical intervention was not done.
Since the inevitable abortion was uneventful or surgical management was not done and uterus was clearly empty by ultrasonography, explorative laparotomy was of dilemma and joint decision by gynecologist and general surgeon was done. Besides, the most potent available antibiotics were given for more than a week but the disease process was advancing and the patient was deteriorating, thus opening the abdomen becomes the option. Blood culture was not done because patient was on broad spectrum antibiotics. After laparotomy, around three liters of serous fluid with foul smelling debris was evacuated and parietal peritoneum was found rough, red to black in color with diffuse adhesion of the intestines. Rapidly, the serous fluid would convert to full blown intra-abdominal pus and the case would cost the patient’s life. Similarly, other cases reported white purulent, fecal smelling watery pus, approximately 4 liters in quantity and small intestines were adherent to the posterior wall of the uterus [2]. This massive intra-abdominal pus collection following spontaneous abortion was not accompanied by uterine perforation, which the association did not explain.
This case revealed severe peritonitis following spontaneous abortion. although extremely rare, spontaneous abortions can result into severe sepsis and endanger life of the pregnant woman [2]. A rare case of fatal disseminated tuberculosis peritonitis in a young woman with rapid progressive clinical course following spontaneous abortion of 20-week gestation was also reported [5]. Therefore, high index of suspicion is crucial in patients with spontaneous abortion with signs of peritonitis. in our case acid fast bacilli of the tapped peritoneal fluid was done which turns to be negative for tb peritonitis.
she was socioeconomically poor which could further predispose her to immune suppression and prone to fulminant peritonitis. It could also be a concomitant problem of spontaneous bacterial peritonitis associated with spontaneous abortion. other literatures also reported the significance of financial status for their predisposition to peritonitis [2]. Even though spontaneous abortion happened one week before the onset of peritonitis, partially treated septic abortion can lead to sepsis with peritonitis. but in this case, she was taking doxycycline and she had no signs of puerperal sepsis in her current presentation. so, the pathogens could be resistant to the treatment usually given as potent and broad spectrum or could be viral infection. blood culture was not done because she came to our hospital a week after taking triple antibiotics. Post operative and septic patients have high risk of clot formation and embolization. our patient was on prophylactic unfractionated heparin 5000iu on bid was give but she develops pulmonary embolism. as she had multiple risks, she developed pulmonary embolism and it better to consider as treatment instead of prophylacsis in such high-risk cases. This case had different clinical presentations as it followed spontaneous abortion with acute presentation and severity of peritonitis that leads to laparotomy. similarly, other studies reported the rarity of the case on following spontaneous abortion, severity of sepsis and short duration of symptoms [2]. Thus, urgent intervention is a clinical request to save this kind of fatal complications.
Conclusion
the case is presented because of its rarity in regards to primary etiology, severity of sepsis, acute clinical presentation. laparotomy, putting drainage tube and peritoneal lavage with warm saline could become lifesaving. the acute and diffuse peritonitis would end in death if urgent interventions were not done. This fulminant peritonitis was followed spontaneous abortion where perforation was not identified. clinicians should have high index of suspicion for these rare associations in which the pathogenesis is not yet known.
Acknowledgments
We acknowledge the surgical and gynecological department and all the hospital staff for their kind support, management, and care.
Declarations
8.1. Competing of Interest: Authors declare that they have no conflict of interest.
8.2. Consent to Participate: A written informed consent was obtained from the patient to be presented in the case report.
Funding
The case report has no source of funding.
References
- Samir Kumar Hazra, Prasanta Kumar Sarkar, Arunima Chaudhuri, Gadadhar Mitra, Debdut Banerjee, et al. (2013) Septic Abortion Managed in a Tertiary Hospital in West Bengal. Journal of basic and clinical science, (2).
- Bangal VB, Gupta Kanika, Fernandes Denita, Singh Pushpanjali, Gavhane S P, et al. (2014) Life threatening fulminant peritonitis following spontaneous midtrimester abortion. IJBR 05(09).
- Ibrahima KA, Papa Saloum Diop, Amadou Bocar Niang, Alioucoly Faye (2016) Acute generalized peritonitis due to uterine perforation following abortion: case study observation. Pan African Medical Journal 27.
- Adedire Timilehin Adenuga, Oluwatosin Wuraola Akande (2020) Peritonitis following unsafe abortion: a retrospective study in a tertiary health facility in North Central Nigeria. Pan African Medical Journal 37: 354.
- Munire Erman Akar, Tayfun Toptas, Havva Sutcu, Haney Durmus, Murat Ozekinci, et al. (2014) Fatal Disseminated Tuberculous Peritonitis following Spontaneous Abortion: A Case Report. Case Reports in Obstetrics and Gynecology.






























