- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Medico-Surgical Therapeutic Management of Benign Prostatic Hyperplasia
Oyovwi Mega Obukohwo*
Department of Human Physiology, Adeleke University, Nigeria
Submission: January 17, 2023; Published:February 21, 2023
*Corresponding author: Oyovwi Mega Obukohwo, Department of Physiology, Faculty of Basic Medical Sciences, Adeleke University, Nigeria
How to cite this article: Oyovwi Mega Obukohwo. Medico-Surgical Therapeutic Management of Benign Prostatic Hyperplasia. Glob J Reprod Med. 2023; 9(4): 555766. DOI: 10.19080/GJORM.2023.09.555766.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Abstract
Although benign prostatic hyperplasia (BPH), a condition that affects many elderly people, is frequent, surgical treatment for BPH has advanced significantly in comparison to medicinal care. Instead of addressing the disease itself, medical treatment just addresses the symptoms. Due to the fact that the majority of senior patients will have comorbid conditions like diabetes and hypertension, surgery may not be an option for everyone, making medical care more widely available. Notably, even while TURP, TUIP, TVP, TUMT, and TUNA continue to be the gold standards for treatment, medicinal therapy still offers hope for recovery and averting surgery. But one must be aware of the recently identified negative effects that these drugs can have in the elderly male, especially over a lengthy period of time. Though they are not appropriate for every patient, novel minimally invasive procedures have shown promise for the elderly male who has failed medicinal therapy but is not a surgical candidate or wishes to avoid surgery. Before choosing a course of treatment for your BPH patient, it’s crucial to talk with them about the risks, advantages, side effects, and alternatives.
Keywords: Medical therapy; Surgery; BPH; TURP
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Introduction
BPH, which is clinically recognized as the worsening of a man’s ability to pass pee, is a multibillion-dollar enterprise [1,2]. BPH incidence rises with aging, hence it will continue to rise sharply as the population ages. BPH is quite prevalent and can have serious consequences [2,3]. For centuries, men with prostate blockage have been able to receive treatment. But in 2023, what changes? What makes this subspecialty of medicine such a thrilling field to work in and conduct research in? It has a lot to do with the revolution in medical technology and the credo of personalized medicine. We will demonstrate how the approach to treating BPH is evolving using these two fundamental ideas.
Men’s urinating problems are frequently referred to as BPH in informal language. However, a variety of acronyms and phrases are employed in the literature to define the signs and situations connected to urinating problems [2,4]. BPH is a pathological alteration that causes the prostate to expand, strictly speaking. This growth may result in what is known as benign prostatic blockage (BPO). Although BPO can induce urinary symptoms in males, it’s important to keep in mind that many other medical disorders can also produce same symptoms. On these topics, the European Association of Urology and the American Urology Association both provide concise evidence-based recommendations [5,6]. In order to keep this seminar on topic, we will only discuss recent developments in the treatment of BPH and BPO. Reviewing the physio-anatomy of the prostate is crucial for a deeper understanding, though.
Anatomy of prostate
Embryology: The pelvic region of the urogenital sinus, which is weeks along in the gestation, is where the prostate gland develops [7-9]. After the growth of multiple endodermal buds, which at first proliferate along the full length of the primitive urethra, the prostate emerges. The adjacent urogenital sinus mesenchyme, where the connective tissue and muscular components of the definitive prostate are developed, is invaded next by the endodermal buds. By the end of the fourth month, the gland has developed fully. For the prostate to develop and grow, conversion to dihydrotestosterone is necessary [8].
Gross Anatomy: Between the bladder and the rectum, where it wraps around the urethra, is where the prostate gland [10]. It is crossed by the ejaculatory ducts and the prostatic portion of the urethra [10]. Its base is located close to the bladder neck, and its apex joins the membrane urethra before resting on the urogenital diaphragm [11]. Of the male reproductive system’s accessory glands, it is the largest [11]. Different cell types make up the majority of it:
a) Cells called glandulars secrete a milky fluid that causes semen to liquefy.
b) Smooth muscle and stromal cells, which during sex contract and squeeze the fluid from the glandular cells into the urethra, where it combines with sperm and other fluids to form semen.
The chemicals known as alpha adrenergic receptors excite the muscle cells. It has a transverse diameter of 4 cm, a length of 3 cm, and an anteroposterior diameter of 2 cm. It weighs about 40g [11]. Before 20 weeks of gestation, the five lobes of the prostate gland, which are separated into it, can be seen in the fetus [10]. Where the hypertrophy is disturbed, the median lobe is of major clinical significance. A fibrous sheath that is a component of the pelvic fascia surrounds the prostate and the fibrous capsule that encloses it [10]. The urethra extends vertically downward from the base to the two-thirds of the gland, just in front of the apex. The prostate utricle’s ejaculatory duct opens at the colliculus on either side of it as it passes posterolaterally by the median lobe [10]. The prostate utricle, which rises and recedes from the colliculus behind the median lobe, is a mucous sac about 6mm long.
Arterial supply: The internal pudendal arteries, middle rectal artery, and prostatic branch of the inferior vesical artery all supply the prostate [10].
Venous supply: Prostatic plexus of veins is responsible for venous drainage [10].
Nerve supply: The sympathetic nerves are carried by the inferior hypogastric plexus; the preganglionic fibers come from the L1 and L2 spinal cords. The parasympathetic fibers and pregangionic fibers are generated from the pelvic splanchic nerves, respectively [10].
Physiology
The male accessory sex gland is responsible for a sizeable portion of semen. Its milky, thin secretion also contains zinc, calcium citrate ion, prostaglandin, fibrinolysin, and acid phosphate ions [12]. Endocrine hormones regulate the prostate’s development and operation; androgens are necessary for the prostate to develop and maintain proper tissue bulk, composition, and secretary 6 function. During ejaculation, the somewhat alkaline prostatic fluid serves to balance the acidity of the other seminal fluids, improving sperm motility and ovum fertilization [12].
Changes during the Lifespan: Prostate size resembles that of a pea during birth. Up until adolescence, it just barely expands before expanding quickly until, by the time a man is in his early 30s, it has a normal adult size and shape, roughly the size of a walnut. Up until the mid-forties, the gland usually remains constant. At this point, most men see a regrowth of their prostate gland due to cell multiplication [13].
Histopathology
Two different sorts of alterations are present: an overgrowth of connective tissue elements and an overgrowth of glandular elements [14]. The consistency of the swollen gland depends on which of the components is more prominent. In contrast to an overgrowth of connective tissue parts, which results in a stiffer consistency, a glandular overgrowth has a softer consistency. All glandular regions, excluding the posterior and anterior lobes, may experience an expansion. Most typically, the median lobe, the two lateral lobes, and the brain stem are affected. Because of the development of the nodules, the gland has grown larger. Possible mass formation from the nodules fused together [10]. The gland’s inner submucous group experiences hyperplasia, which causes the rest of the gland to grow. The outside component of the gland, which is made of fibrous tissue with a tiny amount of muscle tissue and very few glands, is what makes up the artificial capsule that is later formed when the gland is compressed to such a degree. The surgical capsule and the nodular mass are divided along this line. Microscopic examination demonstrates a hyperplastic alteration in the gland’s glandular, fibrous, and muscular components [14]. Early on, there is hyperplasia of the stroma around the ducts, acini, and urethra. After that, ducts and acini proliferate greatly and begin to sprout, which causes the stroma and glands to hyperplasia, which ultimately results in the development of nodules.
Definition of BPH: The histological condition known as benign prostatic hyperplasia (BPH), commonly referred to as benign prostatic hypertrophy, is defined by the proliferation of the prostate’s cellular components, which causes the prostate gland to grow. Chronic bladder outlet obstruction (BOO) due to BPH can result in bladder calculi, recurrent UTIs, reduced kidney function, and gross hematuria.
Epidermiology and Prevalence of BPH: In elderly men, benign prostatic hyperplasia (BPH) is a prevalent issue that can significantly lower quality of life. BPH is a histologically confirmed condition that affects 8% of men between the ages of 41 and 50, 40% to 50% of men between the ages of 51 and 60, 70% of men between the ages of 61 and 70, and more than 80% of men over the age of 80. There are numerous known risk factors for developing BPH, however the disease’s etiology is still not fully understood. One’s race, family history of cancer, higher serum levels of testosterone and estrogen, drinking, prostatitis, and usage of nonsteroidal anti-inflammatory drugs are a few of these [15]. Having symptoms in the lower urinary tract is the standard clinical manifestation of BPH (LUTS). These signs and symptoms include frequent urination, nocturia, urgency, incontinence, a sluggish or intermittent stream of urine, straining, and terminal dribbling (Table 1). 25% of men in their fifties, 33% of men in their sixties, and around half of men in their eighties report having these symptoms in a moderate to severe way. As with any other condition, a comprehensive history and physical examination are the first steps in the clinical evaluation of a man with probable BPH. You can categorize the severity of LUTS in patients using the International Prostate Symptom Score (IPSS) index. There are seven questions in all, and they evaluate the severity and recurrence of various BPH symptoms. Additionally, they ask the patient to score how these symptoms have an impact on their quality of life [15].
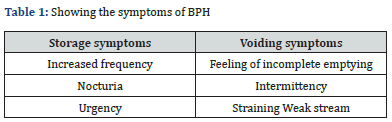
Until recently, autopsy investigations were the only way to estimate the prevalence of BPH. In the sixth decade of life, BPH was histologically present in around half of the men. By their ninth decade of life, about 90% of men had developed BPH. A review of the literature shows conclusively that histologic BPH prevalence is comparable over the world. It is unknown what specific elements start and encourage the proliferative process. Age and androgens are both necessary for the emergence of histologic BPH [10]. The particular androgen that controls the growth and development of the prostate is dihydrotestosterone (DHT). The 5-alpha reductase enzyme converts testosterone to DHT (5AR). 5AR has two subtypes: type 1 and type 2. Prostate Type 2 is the most prevalent subtype. Intraprostatic testosterone is not converted to DHT in males with the 5AR deficient condition [10]. It’s interesting to note that guys with this disease do not develop BPH and as adults have rudimentary prostates. Long-term usage of the 5-alpha reductase inhibitors (5ARIs) dutasteride [16], and finasteride [9], not only results in some prostate volume reduction, but also stops the prostate from growing any further. The main benefit of dutasteride is that it inhibits both type 1 and type 2 5-alphareductase subtypes, leading to a more thorough reduction of DHT synthesis. These observations collectively show that androgens play a crucial role in the formation of the prostate and BPH. The finding that DHT levels do not directly correspond with prostate growth shows that, although DHT promotes growth, other variables other than androgens also contribute to the final degree of prostatic enlargement [17].
Complications of BPH-associated bladder outlet obstruction
I. Renal insufficiency
II. Acute urinary retention
III. Urinary tract infection
IV. Bladder stones
V. Bladder decompensation
VI. Urinary incontinence
VII. Upper urinary tract deterioration and azotemia
VIII. Hematuria
History of BPH
John Hunter, one of the most important British surgeons of the eighteenth century, is credited with the idea that obstruction by an enlarged prostate causes LUTS. Hunter stated in 1786 that “...... swelling of the prostate is the most prevalent in the decline of life... when sick, it must hinder the passage of urine” [18]. He went on to say that in addition to the symptoms directly related to blockage, thickening of the bladder wall and irritation were also side effects of urethral obstruction (Figure 1).
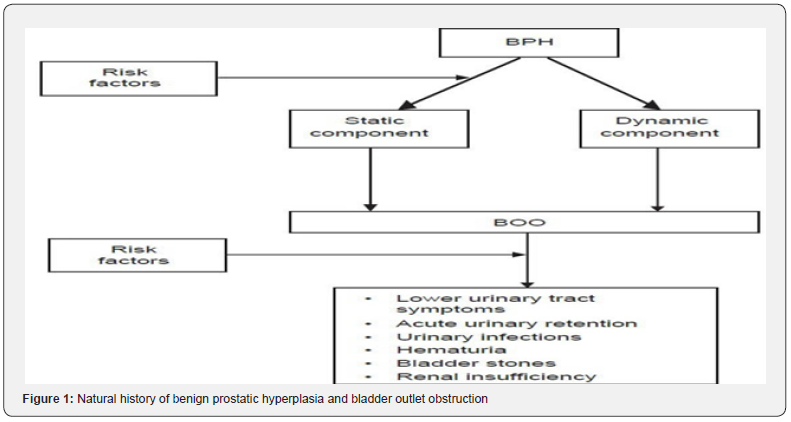
Causes of Benign Prostatic Hyperplasia
There are several theories put out to explain benign cell proliferation.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Hormonal Changes
Androgens, or male hormones, almost certainly contribute to the development of the prostate. Testosterone, which is created throughout a man’s lifespan, is the most significant androgen. Dihydrotestosterone, a more potent androgen, is produced by the prostate from testosterone. The main factor for the fast prostate enlargement that happens between adolescence and young adulthood is DHT, which encourages cell development in the tissue that lines the prostate gland (the glandular epithelium). In later adulthood, DHT is the main suspect in prostate hypertrophy.
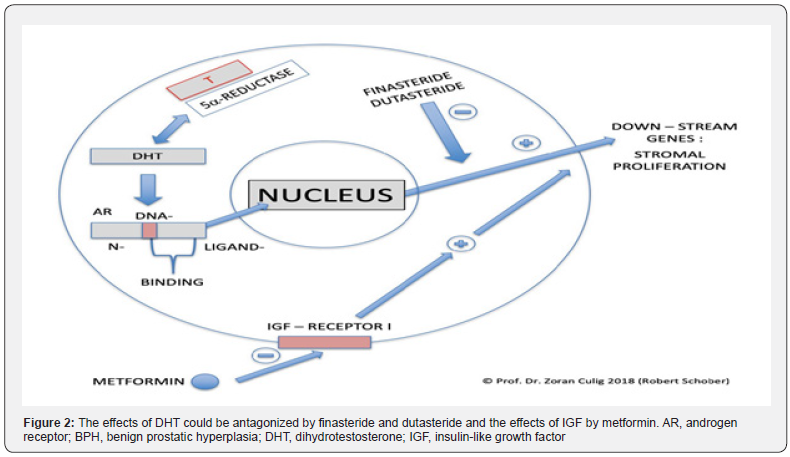
Estrogens: Some experts think that the female hormone estrogen, which is always present in men, may also contribute to BPH. As men become older, their estrogen levels rise and their testosterone levels fall, which could lead to prostate enlargement. The presence of androgen and oestrogen receptors is necessary for the hormonal modulation of BPH. The 5-reductase enzyme’s activity also contributes significantly to the development of BPH. BPH is controlled by hormones. The powerful androgen DHT is created from testosterone, and 5’-reductase regulates the process. In conjunction with the insulin-like growth factor (IGF) pathway, DHT controls the expression of genes that are favorable to differentiation and growth in benign prostate cancer. Finasteride and dutasteride may counteract the effects of DHT, while metformin may counteract the effects of IGF (Figure 2).
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Age-Related factor
Two recognized risk factors for the emergence of BPH/BPE include aging and androgens [20]. Additionally, as demonstrated in a review by Untergasser et al., local para- and luminocrine pleiotrope mechanisms/factors are related to the remodelling of the prostatic tissue [21]. Hypertrophic basal cells, altered luminal cell secretions that cause calcification, blocked ducts, and inflammation, lymphocytic infiltration that produces proinflammatory cytokines, increased production of reactive oxygen species that damages epithelial and stromal cells, increased production of basic fibroblasts and TGF- that promotes stromal proliferation, transdifferentiation, and remodeling, and hypertrophic basal cells are the characteristics of prostate tissue remodelling in the transition zone [21].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Inflammation
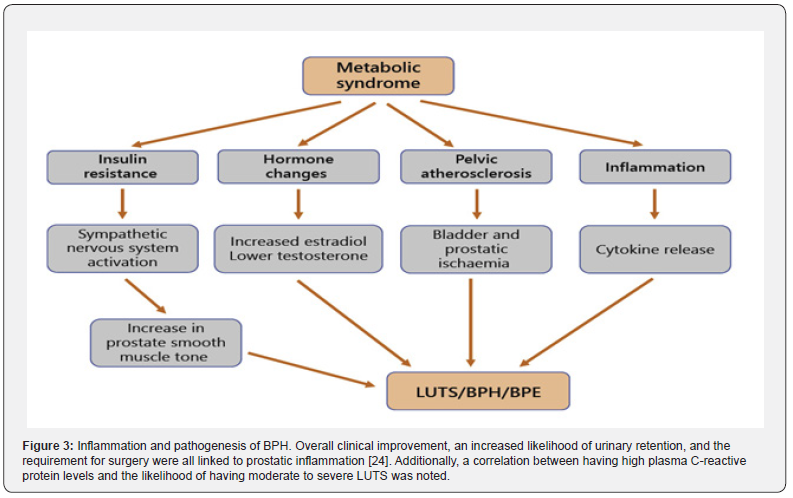
The presence of chronic inflammation alongside BPH histologic alterations in pathologic specimens raised the possibility that inflammation contributes to the emergence of BPH/BPH as well as LUTS (Figure 3). A bacterial or viral infection may cause local inflammation, which would cause the release of cytokines, chemokines, and growth factors involved in the inflammatory response, leading to the proliferation of epithelial and stromal prostatic cells [22]. Inflammatory responses are thought to be sustained by the production of prostatic self-antigens after tissue injury, which would sensitize the immune system and initiate autoimmune responses (Figure 3) [22]. Prostatic stromal cells, which stimulate CD4+ lymphocytes and proinflammatory cytokines and chemokines, like stromal-derived interleukin-8, are significant players in this process (Figure 3) [23].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Metabolic Factors
The findings of numerous pre-clinical and clinical investigations suggest that a number of age-related metabolic abnormalities (metabolic syndrome, obesity, dyslipidaemia, and diabetes) are significant factors in both the onset and progression of BPH/LUTS (Figure 3). [25]. BPH/LUTS onset and progression have been linked to metabolic syndrome and its associated comorbidities, including changes in sex hormones and lowgrade inflammation (Figure 3). Body mass index (BMI) increases of 1 kg/m2 are associated with 0.4-mL increases in prostate volume in the Baltimore Longitudinal Study of Aging cohort. In comparison to non-obese (BMI 25 kg/m2) participants, obese (BMI > 35 kg/m2) participants exhibited a 3.5-fold higher risk of prostate enlargement [26]. The metabolic syndrome’s most welldocumented features are related to BPH/BPE. A higher rate of annual BPE growth, more sympathetic activity, and LUTS are all indicators of metabolic syndrome [22].
The underlying pathophysiologic mechanisms behind the link between metabolic variables and BPH/BPE/LUTS are not fully understood, however systemic inflammation, pelvic ischaemia, and elevated sympathetic activity may be relevant (Figure 2) [22].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Family History
The likelihood of acquiring BPH seems to rise if there is a family history of the condition [27], additional elements, including smoking, diet, race, sexual activity, socioeconomic position, and diet [27].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Clinical Evaluation of BPH
The inability to start urinating and the sensation of incomplete urination are among the early signs of benign prostatic hyperplasia. The urethra narrows as the prostate gland gets bigger and presses against it. As a result, urine cannot flow. The bladder’s muscles enlarge and become more sensitive as it starts to exert more pressure to pass the urine. As a result, there is a constant feeling of urinal urgency and the bladder never feels completely emptied. Other signs include the need to urinate more frequently at night and a weak urine stream that drips after urinating [28]. Incontinence or urine leakage could result from an overfilled bladder in the patient. In addition to kidney stones, some men will get recurrent UTI (urinary tract infections). Infections of the urinary tract can result in fever and burning or pain during urinating. If he squishes to urinate, small veins in the urethra and bladder may burst, which could result in blood showing up in the urine. Empirically, irritable and obstructive symptoms are distinguished from one another [29]. Urge incontinence, nocturnal urgency, and increased frequency are irritable symptoms. Hesitation, decreased urine flow, straining, a sense that the bladder isn’t completely emptied, incontinence, and urinary retention are the obstructive symptoms [29].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Diagnostic Test
International Prostatic Symptom Score
A committee of the American Urological Association created this questionnaire, known as the International Prostate Symptom Score [30]. Key lower urinary tract symptoms can be assessed using a technique called the International Prostate Symptoms Score (IPSS). This grading method measures the patient’s subjective experience as opposed to laboratory tests or other neutral assessments. The more serious the condition, the higher the score. There are numerous uses for it. The patient’s performance on this exam provides a very accurate evaluation of the impact of lower urinary tract problems on a man’s quality of life [31].
Other Indexing Systems
In addition to the IPSS, other indexing systems that measure various quality-of-life and disease-related issues are used to help evaluate the patient. These indexing systems include the Boyarsky guidelines, the Madsen-Iverson point system, the Symptom Problem Index (SPI), and the BPH Impact Index (BII) [31].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Physical Examination
Digital Rectal Examination
An enlarged prostate can be found via the digital rectal examination (DRE). To gauge the prostate’s size and feel for nodules or pain, the doctor slips a gloved, lubricated finger into the patient’s rectum. Although short and painless, some people find the examination embarrassing. Prostate size is typically underestimated by the test, which nevertheless aids in ruling out prostate cancer. It is ineffective for determining the presence of prostatic hyperplasia and is never used as the main diagnostic method for BPH or cancer.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Others
In order to rule out potential neurological reasons of bladder dysfunction, some tests that assess reflexes, sensations, and motor response may be conducted in the lower extremities. These procedures also involve palpating the abdomen to look for kidney or bladder abnormalities.
Uro-flowmetry
Uroflowmetry, a technique that measures the rate of urine flow, can identify whether the bladder is obstructed [31]. The patient is told to wait several hours before urinating and to drink plenty of fluids so that his bladder is full and he feels a strong urge to urinate. An uroflowmeter-equipped special toilet is used for this test, which requires the patient to urinate into it. It is crucial that the patient urinates regularly, without straining to empty his bladder or making an effort to slow down the flow of urine, while also remaining motionless to help assure accuracy. The test should be repeated at least twice because a variety of circumstances, including straining or self-consciousness, might impact urine flow. The usual range is defined as voiding volumes of 150 ml or more and values more than 15 ml per second [31]. Qmax: The amount of urine that is passed per second (ml/s) is used to measure the flow rate of urine. The flow rate measurement is noted and referred to as the Qmax at its highest point. The better the patient flow rate, the greater the Qmax.
Urine Analysis
To identify bleeding or infection symptoms, a urine analysis may be carried out. During a urinalysis, urine is physically and chemically analyzed. Microscopically, urine is analyzed. Younger men rarely get urinary infections, while older men, especially those with BPH, tend to get them more frequently. Additionally, a urinalysis aids in excluding bladder cancer.
Serum Creatinine
Serum creatinine, a kidney function test marker, is measured in blood tests for males who have symptoms [27]. The majority of BPH patients experience renal issues.
Prostate Specific Antigen (PSA)
During a PSA test, the amount of prostate-specific antigen (PSA) in the patient’s blood is determined. The usual prostate cancer screening test is it [27]. Every year, it’s advised that men over 50 and those over 40 who are at high risk for prostate cancer get their PSAs. The PSA test has typically been optional for men with suspected BPH despite the fact that BPH itself can increase PSA levels. A drop in PSA levels is correlated with a reduction in prostate size. There is a 10% reduction in prostate volume for every 19% drop in PSA values [32]. Finasteride, a medication used to treat BPH, and TURP, a surgical procedure that removes the prostate through the transurethral route, can both lower PSA levels and perhaps conceal the presence of prostate cancer. Less than 4 nanograms per milliliter should be the norm. A more recent test finds “free PSA,” which is present at lower levels in prostate cancer and at higher levels in benign prostate hyperplasia. Whether a man is on finasteride or not, this might be more accurate than total PSA.
Postvoid Residual Urine
The amount of urine remaining after urinating, or postvoid residual urine volume (PVR), is one of the crucial tests for urinary incontinence. Urine should only be left in roughly 50 mL or less in a typical situation; anything over 200 mL is definitely odd. Transabdominal ultrasound is the most popular way to measure PVR. A soft tube called a catheter, which is placed into the urethra shortly after urinating, can also be used to measure PVR [33].
Ultrasound
An accurate view of the prostate gland’s size and form can be obtained using ultrasound without the need of a catheter. When choosing treatments and deciding how effective they will be, ultrasound is a highly useful tool. In addition to these uses, ultrasound may be used to find malignancies, bladder stones, and kidney injury. Because it is less intrusive, it can provide an accurate measurement of postvoid residual pee [34]. Using a rectal probe, transrectal ultrasonography (TRUS), another ultrasound test for the prostate, analyzes the prostate. The measurement of prostate volume using TRUS is substantially more precise. In some cases, it can identify cancer.
Filling Cystometry
When a patient is unable to urinate and there is a suspicion of nerve damage or bladder injury, filling cystometry, also known as cystometrography, is typically employed [34]. Uninhibited detrusor contractions (UDC), which frequently happen in men with symptoms of the storage urinary tract, are detected with the test. The collection of muscle fibers known as the detrusor lines the exterior of the bladder. The test is not frequently applied.
Urethrocystoscopy
When men with BPH are given the diagnosis, a urethrocystoscopy, also known as a cystourethroscopy, may be carried out, especially if they are candidates for surgery or if other urinary tract issues are detected. Infection, interstitial cystitis, bladder cancer, previous surgery, or an injury are examples of such issues. Blood in the urine is another. The urologist can identify a range of structural issues, such as enlarged prostate, obstruction of the urethra or bladder neck, anatomical anomalies, or the presence of stones. The lower urinary system can be seen during this technique by inserting an endoscope, a flexible or rigid fiber optic tube, into the urethra. The procedure is not without risks. Complications are uncommon but can include allergic response to the anaesthetic, urinary tract infection, bleeding, and urine retention [34].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Management of BPH
Men typically have the option of either treating BPH or choosing cautious waiting because it rarely results in major consequences. Treatment Alternatives: Enhancing urine flow and minimizing symptoms are the main targets of BPH treatment. There are lots of choices. They include prescription medications, minimally invasive techniques, and major surgery.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Watchful Waiting
Studies have indicated that in patients with low IPSS symptom scores (zero to seven), drugs are not significantly more helpful than placebo. Therefore, in these individuals, watchful waiting is advised [35]. Sepsis, upper tract dilatation with or without renal insufficiency, and acute urine retention can all develop, even in the absence of treatment, making follow-up monitoring crucial. It is important to tell patients with higher IPSS symptom scores about available treatments.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Complementary Medicine
Following epidemiologic research that revealed Asians to have lower rates of BPH and prostate cancer than people from Western countries, interest in complementary treatments for BPH rose [10]. The more soy that is typically consumed in Asian diets is one theory for this. In histoculture, it has been discovered that the main isoflavone in tofu, genistein, inhibits the formation of hyperplastic prostate tissue [36]. It may be attempted a standardized isoflavone product containing genistein instead of natural soy food products because they are not widely accessible or acceptable. Early trials on short time periods revealed that BPH symptoms were quickly relieved. Long-term and independent studies, on the other hand, are not accessible. Saw palmetto (Serena repens) is a popular BPH supplement [37,38]. Although it has been found to inhibit the enzyme 5-alpha reductase, clinical evidence has yet to be obtained. Saw palmetto has been demonstrated to be as beneficial as finasteride in patients with BPH, but not as effective as other pharmacological treatments like alpha blockers. saw palmetto had less adverse effects than standard drugs in a study of 18 research, and repeated ultrasound exams revealed that therapy with this medicinal herb decreased prostate size without increasing serum PSA levels. Saw palmetto is typically taken in doses of 160 mg twice daily. Mild headaches or digestive problems are typically the most common side effects (incidence: less than 3%). Other herbal or supplementary treatments are utilized to treat BPH all over the world [37,38]. However, a lot of these medications lack standardization or have undergone inadequate efficacy research. Agents including African plum, South African star grass, stinging nettle, and rye pollen are frequently employed [10].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Medical Treatments
Nonselective Alpha-1 Blockers
The prostatic smooth muscle tone is decreased by doxazosin, prazosin, and terazosin, which has an immediate impact on urine flow [39]. The International Prostate Symptom Scores improve more slowly with these drugs than they do with surgery, despite the fact that BPH symptoms are immediately alleviated. There are negative consequences include asthenia, retrograde ejaculation, asthenia, postural hypotension, and dizziness. When used at night and with a moderate dosage titration, side effects can be reduced. When necessary, alpha blockers may be used with other treatments. Since there are generic versions of prazosin, they are more affordable.
Selective Alpha-1 Blocker
A highly selective alpha-1 adrenergic antagonist called tamsulosin was created to counteract the negative effects of nonselective drugs. Tamsulosin may be effective for some people who do not react to non-selective alpha blockers and may have less side effects, such as hypotension, due to its selectivity. Tamsulosin is started at a dosage of 0.4 mg once daily and increased to a daily maximum of 0.8 mg [40]. Tamsulosin is more expensive than non-selective alpha blockers but has no effect in lowering blood pressure.
5-Alpha Reductase Inhibitors
The amount of serum dihydrotestosterone is gradually reduced by 50% as a result of finasteride [41]. Over the course of three to six months of treatment, the prostatic volume consequently reduces by roughly 19%. Significant improvements in urinary symptoms and flow rates were seen after finasteride therapy. However, in the Prospect investigation, the benefits of finasteride were noticeably inferior to those of any alpha blocker or surgical procedure [42].
Studies indicate that alpha blockers are beneficial across the spectrum of prostate diameters, however finasteride may be most effective in males with a large gland. Finasteride side effects are less common than placebo in terms of frequency (4 to 5 percent). Impotence, an abnormal ejaculatory pattern, and a lowered libido are negative effects. PSA readings drop by 40–50% when taking finasteride. The PSA values should be doubled and then compared to age related norms in a patient who is on finasteride and has undergone a PSA screening. The sensitivity and specificity for the prostate cancer diagnosis remain unchanged. Recently, the US Food and Drug Administration approved dutasteride in 0.5 mg capsule form for the treatment of BPH (labeling for the treatment of male-pattern baldness is still pending) [10]. The fact that this medication inhibits both types 1 and 2 of 5alpha reductase gives it a unique mode of action. Finasteride has similar sexual side effects.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Hormonal Treatment
Gonadotropin-Releasing Hormone Agonists
The anterior lobe of the pituitary gland is triggered to release luteinizing hormone when GnRH is released pulsatilely from the brain. When exogenous GnRH is injected, endogenous GnRH production falls, the pulsatile signal to the anterior pituitary lobe is disrupted, and luteinizing hormone release is inhibited. Without luteinizing hormone, the testicular Leydig’s cells are unable to make testosterone. Gabrilove et al. reported the best outcomes from the GnRH treatment for BPH [43]. Leuprolide, a GnRH agonist, was administered subcutaneously daily to study participants for six months. Patients had improvement in urine flow and, to a lesser extent, nocturia and frequency [44]. An average 45% reduction in prostate size was observed [44].
Androgen Receptor Blockers
When it comes to androgen receptor sites, flutamide, a nonsteroidal anti-androgen, faces off against dihydrotestosterone [45]. Apoptosis, cell shrinkage, and reduced protein synthesis occur in the absence of androgenic stimulation (cell death). In a prospective, placebo-controlled experiment, individuals receiving 750 mg/day of flutamide experienced a 41% mean reduction in prostatic size and a 35% mean increase in urine flow. The flutamide and placebo groups experienced similar levels of symptom relief. The side effects of flutamide treatment include gynecomastia in some patients, diarrhea and an increase in liver transaminase in others [46]. However, the serum levels of luteinizing hormone and testosterone actually rise, preventing some of the side effects of testosterone inhibition (impotence), as well as gynecomastia [10]. These males have increased amounts of estradiol because estrogens are produced from androgens. As a result, dose limiting side effects such as breast discomfort and gynecomastia may arise. About one-third of instances with BPH will significantly improve with anti-androgen and GnRH agonist treatments. Antiandrogen and GnRH agonist medications are pricey on a yearly basis. These drugs have not been widely used as medical therapies for symptomatic BPH due to their unfavorable side effects and exorbitant pricing.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Surgical Treatments
When medicinal treatment is unsuccessful, a patient has refractory urine retention, is unable to have a catheter removed, has recurrent urinary tract infections, chronic hematuria, bladder stones, or renal insufficiency, surgery should be considered [10]. Patients with high IPSS symptom ratings who are strong candidates for surgery and who want surgical treatment may also receive surgery as their initial treatment [47,48].
Open Prostatectomy
The oldest and best method of treating BPH symptoms and maximizing urine flow is surgical excision of the core section of the prostate utilizing a suprapubic or retropubic approach [10]. Only 2% of individuals who receive this surgery experience treatment, although 98 percent of them report relief in their symptoms. But open prostatectomy, the most intrusive treatment for BPH, is also the one that carries the greatest risk of side effects [49]. Because of this, this treatment is often only performed on patients who have a very big prostate gland or structural issues, such as a large median lobe that protrudes into the bladder, a large bladder calculus, or a large urethral diverticulum.
Transurethral Resection of the Prostate (TURP)
TURP, the most popular surgical treatment for BPH, helps 88% of patients with their symptoms.
Inability to empty, clot retention, and secondary infection are the most common side effects of the surgery [10]. Only 1% of people get bleeding, the most severe consequence. Impotence, retrograde ejaculation, partial incontinence, and complete incontinence are examples of long-term consequences [50]. (Xu et al., 2018) [50]. In the first five years, 10% of patients need a retreatment [50].
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Recent advance Procedures
The risk of sexual dysfunction associated with TURP is unacceptable to many younger patients, and many elderly BPH patients are poor surgical candidates [10]. In an effort to achieve TURP-like outcomes with “minimally invasive” surgical methods that are less expensive and morbidity-prone [51,52]. The use and accessibility of these more recent techniques varies by area. Abranches-Monteiro et al. (2020) [53], describe the endoscopic operation known as transurethral incision of the prostate (TUIP), which reduces urethral constriction without removing any prostate tissue. An outpatient treatment called TUIP is possible. Younger patients who have serious fertility and antegrade ejaculation problems are typically offered it as a therapy option. While the operation is less time-consuming and less bloody than TURP, the results are comparable. It has not been sufficiently examined how long-term satisfaction and retreatment rates work. An aurethral catheter is inserted with a microwave antenna as part of transurethral microwave thermotherapy (TUMT), a single session, minimally invasive outpatient procedure [54]. While a cooling system pumps water to protect nearby tissue from deep, rapid tissue heating caused by the microwave radiation [54]. It takes roughly an hour and neither general anesthesia nor spinal anesthesia is required. There has been a 45 percent improvement in objective flow rates and a 65 percent drop in subjective urinary symptoms, according to a few small trials. 7.3% of patients required retreatment two years after TUMT [55]. In patients receiving TUMT, there have been no serious side effects—including incontinence and sexual dysfunction—reported. Prostate ablation with a laser or electrode is another minimally invasive technique. Due to the fact that all necrotic tissue was not removed, some early investigations found a link between this technique and an increase in methicillin-21 resistant Staphylococcus aureus infections [56]. The likelihood of this problem has decreased as a result of advancements in electrodes, lasers, and training. To eliminate prostatic tissue with minimal coagulation, transurethral vaporization of the prostate (TUVP) or transurethral electro vaporization of the prostate (TVP) is currently carried out using endoscopic electrosurgical equipment [57]. The surgery reduces urinary symptoms in a way that is comparable to TURP, but with less postoperative discomfort, urine retention, blood loss, and risk of hyponatremia. In the same way as with TUMT, no tissue is collected, making it impossible to evaluate patients for concomitant prostatic cancer [10]. Prostate radiofrequency needles are inserted during transurethral needle ablation (TUNA) [10]. Local anesthesia can be used to carry out the procedure, which is secure. The bladder neck and median prostate lobe cannot be treated, hence the effectiveness may be constrained. According to studies, patients who received TUNA also had significantly lower IPSS symptom levels and higher maximum urine flow rates [58-60]. In the past, transurethral balloon dilation of the prostate was utilized as a secure, less invasive treatment for BPH. The rate of retreat, though, was substantial. Urethral stents can be inserted to increase the success of the dilatation, although they are prone to infection, encrustation, and reblockage. Stent implantation is often reserved for usage in patients who are highrisk surgical candidates with a limited life expectancy due to the high complication rate.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Conclusion
Despite the fact that benign prostatic hyperplasia (BPH) is one of the most frequent illnesses among the elderly, surgical treatment has expanded dramatically in comparison to medicinal treatment. The medical treatment simply gives symptomatic alleviation and does not cure the condition. Because the majority of the older population has allied comorbidities such as diabetes or hypertension, not everyone is able to undertake surgical operations, medical treatment becomes more accessible. Notably, despite the fact that TURP, TUIP, TVP, TUMT, and TUNA continue to be the gold standard for treatment, drug therapy continues to offer hope for both treatment and avoiding surgery. However, it’s important to be aware of the recently discovered side effects that these medications, especially when taken for a long time, can have on senior men. The older male who has failed medical therapy and is neither a surgical candidate nor does he want to undergo surgery has showed promise in receiving novel minimally invasive therapies, though not for every patient. As with any disease, it is crucial to discuss the risks, advantages, side effects, and options with your patient before deciding on a treatment plan for a BPH patient.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Ethics Statement
Approval of an ethics committee was not required as this was a review of other published works.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
Human and Animal Rights
This article does not contain any studies with human or animal subjects performed by any of the authors.
- Review Article
- Abstract
- Introduction
- Hormonal Changes
- Age-Related factor
- Inflammation
- Metabolic Factors
- Family History
- Clinical Evaluation of BPH
- Diagnostic Test
- Physical Examination
- Others
- Management of BPH
- Watchful Waiting
- Complementary Medicine
- Medical Treatments
- Hormonal Treatment
- Surgical Treatments
- Recent advance Procedures
- Conclusion
- Funding
- Ethics Statement
- Human and Animal Rights
- References
References
- Saigal CS, Gore J, Polich S, Litwin MS (2005) 487: Trends in Reconstruction after Radical Cystectomy in the Medicare Population. The Journal of Urology 173(4S): 133-134.
- Van Rij S, Gilling P (2015) Recent advances in treatment for Benign Prostatic Hyperplasia. F1000Research 4:1482.
- Parsons JK (2010) Benign prostatic hyperplasia and male lower urinary tract symptoms: epidemiology and risk factors. Curr Bladder Dysfunct Rep 5(4): 212-218.
- Abrams P, Cardozo L, Fall M, Griffi ths D, Rosier P, Ulmsten U, et al. (2002) Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn 21(2): 167-178.
- McVary KT, Roehrborn CG, Avins AL, Barry MJ, Bruskewitz RC, et al. (2010) American urological association guideline: management of benign prostatic hyperplasia (BPH). American Urological Association Education and Research Inc 17-22.
- Gratzke C, Bachmann A, Descazeaud A, Drake MJ, Madersbacher S, et al. (2015) EAU guidelines on the assessment of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. European urology 67(6) 1099-1109.
- Larsen WJ (2001) Development of the urogenital system. Human embryology. 2nd edn. Churchill living stone 261-309.
- Minn RM (1997) Male internal genital organs. Last’s anatomy regional and applied. 9th edn. Churchill living stone 384-86.
- McConnell JD, Bruskewitz R, Walsh P, Andriole G, Lieber M (1998) The effect of finasteride on the risk of acute urinary retention and the need forsurgical treatment among men with benign prostatic hyperplasia. N Engl J Med 338: 557-63.
- Praveen R (2013) Benign prostatic hyperplasia: Updated review. Int Res J Pharm 4(8): 45-51.
- Glass J, Mundy A (2005) The perineum and pelvis. The anatomical basis ofclinical practice. 13th ed. Elsevier Churchill livingstone 893-841.
- Guyton AC, Hall JE (2012) Reproduction and hormonal functions of the male (and function of the pineal gland) In: Guyton AC Hall JE edit.
- Keeth DW, Andriole GL (2002) Medical therapy for benign proststic hyperplasia. J Advances in clinical medicine 164: 11-15.
- Harsh Mohan (2005) The male reproductive system and prostate. In: Harsh Mohan editor. Text book of pathology. 5th edn. Jaypee brothers 728-747.
- Nimeh T, Magnan B, Almallah YZ (2016) Benign prostatic hyperplasia: review of modern minimally invasive surgical treatments. Semin Intervent Radiol 33(3): 244-250.
- Roehrborn CG, Marks LS, Fenter T, Freedman S, Tuttle J, et al. (2004) Efficacy and safety of dutasteride in the four-year treatment of men with benign prostatic hyperplasia. Urology 63(4): 709-715.
- Walsh PC, Hutchins GM, Ewing LL (1983) Tissue content of dihydrotestosterone in human prostatic hyperplasis is not supranormal. The Journal of clinical investigation 72(5): 1772-1777.
- Hunter J (1976) A treatise on the veneral disease. J Clin Invest 45: 56-62.
- Patel ND, Parsons JK (2014) Epidemiology and etiology of benign prostatic hyperplasia and bladder outlet obstruction. Indian J Urol 30(2): 170-176.
- Madersbacher S, Sampson N, Culig Z (2019) Pathophysiology of benign prostatic hyperplasia and benign prostatic enlargement: a mini-review. Gerontology 65(5): 458-464.
- Untergasser G, Madersbacher S, Berger P (2005) Benign prostatic hyperplasia: age-related tissue-remodeling. Experimental gerontology 40(3): 121-128.
- Soler R, Andersson KE, Chancellor MB, Chapple CR, de Groat WC, et al. (2013) Future direction in pharmacotherapy for non-neurogenic male lower urinary tract symptoms. Eur Urol 64(4): 610-621.
- Chughtai B, Lee R, Te A, Kaplan S (2011) Role of inflammation in benign prostatic hyperplasia. Rev Urol 13(3) 147-150.
- Nickel JC, Freedland SJ, Castro-Santamaria R, Moreira DM (2017) Chronic prostate inflammation predicts symptom progression in patients with chronic prostatitis/chronic pelvic pain. The Journal of urology 198(1): 122-128.
- Sebastianelli A, Gacci M (2018) Current status of the relationship between metabolic syndrome and lower urinary tract symptoms. Eur Urol Focus 4(1): 25-27
- Parsons JK, Carter HB, Partin AW, Windham BG, Metter EJ, et al. (2006) Metabolic factors associated with benign prostatic hyperplasia. J Clin Endocrinol Metab 91(7): 2562–2568.
- Lam JS, Cooper KL, Kaplan SA (2004) Changing aspects in the evaluation and treatment of patients with benign prostatic hyperplasia. Med Clin North Am 88(2): 281-308.
- Pamela D, Reagan RW, Bahnson RR (2002) Managing benign prostate hyperplasia. J American family physician 66: 77-84.
- Thorpe A, Neal D (2003) Benign prostatic hyperplasia. J Lancet 361: 1359-67.
- Barry MJ, Fowler Jr FJ, O’Leary MP, Bruskewitz RC, Holtgrewe HL, et al. (1992) The American Urological Association symptom index for benign prostatic hyperplasia. J Urol148(5) 1549-1557.
- Joseph O (2007) BPH medical and minimally invasive treatment. NEJM 332: 115-19.
- Girman CJ (1998) Population-based studies of the epidemiology of benign prostatic hyperplasia. Br J Urol 82(1): 34-43.
- McNeill SA, Hargreave TB, Ricouard CG, Santoni JP, Roehborn CG (2001) Postvoid residual urine in patients with lower urinary tract symptoms suggestive of benign prostatic hyperplasia: pooled analysis of eleven controlled studies with alfuzosin. J Adult urol 57: 459-65.
- McConnell JD (1999) Benign prostatic hyperplasia: diagnosis and treatment. Benign Prostatic Hyperplasia Guidelines J BMJ 55: 223-229.
- Roehrborn CG, Oyarzabal Perez I, Roos EP, Calomfirescu N, Brotherton B, et al. (2015) Efficacy and safety of a fixed‐dose combination of dutasteride and tamsulosin treatment (Duodart®) compared with watchful waiting with initiation of tamsulosin therapy if symptoms do not improve both provided with lifestyle advice in the management of treatment‐naïve men with moderately symptomatic benign prostatic hyperplasia: 2‐year CONDUCT study results. BJU Int: 116(3) 450-459.
- Andres S, Abraham K, Appel KE, Lampen A (2011) Risks and benefits of dietary isoflavones for cancer. Critical reviews in toxicology 41(6): 463-506.
- Grammatikopoulou MG, Gkiouras K, Papageorgiou SΤ, Myrogiannis I, Mykoniatis I, et al. (2020) Dietary Factors and Supplements Influencing Prostate-Specific Antigen (PSA) Concentrations in Men with Prostate Cancer and Increased Cancer Risk: An Evidence Analysis Review Based on Randomized Controlled Trials. Nutrients 12(10) 2985.
- Villa G, Boarin M, Rosa D, Togni S, Manara DF, et al. (2022) Phytotherapy in urological benign disease: A systematic review. International Journal of Urological Nursing 16(3): 174-195
- Kaplan SA (2005) alpha-Blocker Therapy: current update. Rev Urol 7(8): S34-42.
- Yanardag H, Goktas S, Kibar Y, Kilic S, Erduran D (2005) Intermittent tamsulosin therapy in men with lower urinary tract symptoms. J Urol 173(1): 155-157.
- Caserini M, Radicioni M, Leuratti C, Terragni E, Iorizzo M, et al. (2016) Effects of a novel finasteride 0.25% topical solution on scalp and serum dihydrotestosterone in healthy men with androgenetic alopecia. Int J Clin Pharmacol Ther 54(1): 19-27.
- Gupta N, Rogers T, Holland B, Helo S, Dynda D, et al. (2018) Three-year treatment outcomes of water vapor thermal therapy compared to doxazosin finasteride and combination drug therapy in men with benign prostatic hyperplasia: cohort data from the MTOPS trial. J Urol 200(2): 405-413.
- Gabrilove JL, Levine AC, Kirschenbaum A, Droller M (1987) Effect of a GnRH analogue (leuprolide) on benign prostatic hypertrophy. J Clin Endocrinol Metab 64(6): 1331-1333.
- Levine AC, Kirschenbaum A, Kaplan P, Droller MA, Gabrilove JL (1989) Serum prostate-antigen levels in patients with benign prosttic hypertrophy treated with leuprolide. Urology 34(1): 10-13.
- Nejishima H, Yamamoto N, Suzuki M, Furuya K, Nagata N, et al. (2012) Anti‐androgenic effects of S‐40542 a novel non‐steroidal selective androgen receptor modulator (SARM) for the treatment of benign prostatic hyperplasia. Prostate 72(14): 1580-1587.
- O'Bryant CL, Flaig TW, Utz KJ (2008) Bicalutamide‐Associated Fulminant Hepatotoxicity. Pharmacotherapy 28(8): 1071-1075.
- Sievert KD, Schonthaler M, Berges R, Toomey P, Drager D, et al. (2019) Minimally invasive prostatic urethral lift (PUL) efficacious in TURP candidates: a multicenter German evaluation after 2 years. World J Urol 37(7): 1353-1360.
- Arezki A, Sadri I, Couture F, Schwartz R, Nguyen DD, et al. (2021) Reasons to go for Rezūm steam therapy: an effective and durable outpatient minimally invasive procedure. World journal of urology 39(7): 2307-2313.
- Eredics K, Wachabauer D, Röthlin F, Madersbacher S, Schauer I (2018) Reoperation rates and mortality after transurethral and open prostatectomy in a long-term nationwide analysis: have we improved over a decade?. Urology 118: 152-157.
- Xu P, Xu A, Chen B, Zheng S, Xu Y, et al. (2018) Bipolar transurethral enucleation and resection of the prostate: Whether it is ready to supersede TURP?. Asian journal of urology 5(1) 48-54.
- Patel HD, Ball MW, Cohen JE, Kates M, Pierorazio PM, et al. (2015) Morbidity of urologic surgical procedures: an analysis of rates risk factors and outcomes. Urology 85(3): 552-560.
- Sivarajan G, Borofsky MS, Shah O, Lingeman JE, Lepor H (2015) The role of minimally invasive surgical techniques in the management of large-gland benign prostatic hypertrophy. Rev Urol 17(3): 140-149.
- Abranches‐Monteiro L, Hamid R, D'Ancona C, Alhasso A, Dmochowski R, (2020) The International Continence Society (ICS) report on the terminology for male lower urinary tract surgery. Neurourology and urodynamics 39(8): 2072-2088.
- Aleksic I, Mouraviev V, Albala DM (2014) Transurethral Microwave Therapy 16. Treatment of Benign Prostatic Hyperplasia: Modern Alternative to Transurethral Resection of the Prostate 121.
- Hoffman RM, Monga M, Elliott SP, MacDonald R, Langsjoen J, et al. (2012) Microwave thermotherapy for benign prostatic hyperplasia. Cochrane Database Syst Rev 9.
- Chen Q (2019) Identification of Synergistic Drug Combinations Against Cystic Fibrosis Pathogens Doctoral dissertation.
- Issa MM (2008) Technological advances in transurethral resection of the prostate: bipolar versus monopolar TURP. J Endourol 22(8):1587-1596.
- Bhatia S, Sinha VK, Harward S, Gomez C, Kava BR, et al. (2018) Prostate artery embolization in patients with prostate volumes of 80 mL or more: a single-institution retrospective experience of 93 patients. J Vasc Interv Radiol 29(10): 1392-1398.
- Haroun H, Eltatawy H, Soliman MG, Tawfik A, Ragab MM, et al. (2019) Evaluation of outcome of transurethral needle ablation for treating symptomatic benign prostatic hyperplasia: A 10-year experience. Urology Annals 11(2): 198-203.
- McVary KT, Gittelman MC, Goldberg KA, Patel K, Shore ND, et al. (2021) Final 5-year outcomes of the multicenter randomized sham-controlled trial of a water vapor thermal therapy for treatment of moderate to severe lower urinary tract symptoms secondary to benign prostatic hyperplasia. J Urol 206(3): 715-724.






























