Impact of Creating Awareness About Birth Preparedness and Complications Readiness Amongst Pregnant Women of Remote Communities with Extreme Poverty and Access Problems
Chhabra S*, Jatkala R and Bathla M
Department of Obstetrics Gynaecology, Mahatma Gandhi Institute of Medical Sciences, Sevagram, India
Submission: October 08, 2022; Published:November 14, 2022
*Corresponding author: Chhabra S, Department of Obstetrics Gynaecology, Mahatma Gandhi Institute of Medical Sciences, Sevagram, India
How to cite this article: Chhabra S, Jatkala R, Bathla M. Impact of Creating Awareness About Birth Preparedness and Complications Readiness Amongst Pregnant Women of Remote Communities with Extreme Poverty and Access Problems. Glob J Reprod Med. 2022; 9(2): 555758. DOI: 10.19080/GJORM.2022.09.555758.
Abstract
Background: Although antenatal care sets in road to safety of mother and baby, birth affects pregnancy outcome most. Birth preparedness, complications readiness (BPCR) during pregnancy become essential, especially for rural women who have scarce health services, resources and access problems.
Objectives: Community based study was carried out to know about impact of creating BPCR awareness to rural, tribal pregnant women.
Material and methods: Study was conducted in 100 villages, randomly divided into 50 studies and 50 controls. Minimum 10 from each village, 15 to 39 years old, 1040 pregnant women, became study subjects. BPCR awareness was tried with maximum 5 sessions. Some women had only one session, because of inclusion from mid pregnancy, research assistant’s fixed visits, women’s availability. Ten randomly included women from each village in control set of villages, with no BPCR sessions, 1000 became study subjects. Pregnancy outcome was collected in study, as well as control villages.
Results: Of 115 women who could have only one session, 45.2% found session useful, 16.5% of them had home births, 40.9% at Subcentre, 5.2% District hospital, 11.3% Referral hospital, 96.5% had live births, 3.5% stillbirths, 6.3% neonatal deaths occurred. Of 475 women who had 2-3 sessions, 77.1% found sessions useful, 3.6% had HBs, 42.3% at SC, 35.8% primary health centre, 30 (6.3%) DH, 12% RH, with 100% LBs, 1.1% NNDs. Of 450 women who had 4-5 sessions, 84.9% said sessions were very useful, 0.7% had HBs, 42.7% at SC, 38% PHC, 6.4% DH, 12.2% at RH, no SB, 1.6% NNDs. Of 1000 women who were not given BPCR awareness sessions, 40.4% had HB, 32.4% SC, 19.2% PHC, 2.8% DH, 5.2% RH, 92.7% had LBs, 7.3 SBs, 11.3% NNDs, no maternal death.
Conclusion: BPCR awareness helped increase facility births, improved neonatal outcome, especially with more sessions.
Background
Maternal foetal, neonatal mortality and morbidity continue to be high in developing countries, because of many reasons, including lack of awareness, resources, health facilities and quality care during pregnancy and birth. Antenatal care sets in the maternal, newborn, and child health (MNCH) continuum [1], but critical time, ‘birth’ affects the pregnancy outcome, the most. Tura et al. [2], reported that skilled care during birth and immediately after birth were the key strategies for reducing maternal deaths. Women, families, communities and health providers need to be aware of issues which need to be addressed to achieve safe outcome, for mother and the baby. Birth preparedness and complications readiness (BPCR) are being implemented as comprehensive strategies to fill the gap from antenatal care to birth and postbirth, for improving pregnancy outcome, especially for women with low resources and those for whom emergency care difficult. It is essential to know the impact of BPCR awareness created during pregnancy.
Objective
Community based study was carried out to know the impact of BPCR awareness created during pregnancy in rural, tribal, pregnant women.
Material and Methods
After institute’s ethics committee’s approval, the study was carried out in the tribal communities of 100 villages around the village with the health facility. Villages were randomly divided in 50 study villages and 50 control. Randomly included, minimum 10 from each village, over a year 1040 pregnant women of 15 to 39 years, in whom knowing outcome was possibly became the study subjects in study villages, where BPCR sessions were conducted from mid pregnancy onwards. In control villages, 1000 women with same criteria became controls. No BPCR awareness was created. The numbers are not equal as villages and duration of study were equalized and not numbers of pregnant women. Difference was awareness sessions with pregnant women in study villages. Plan was to include women of 15 to 45 yrs, but eldest was 39 yrs. After taking consent, women from mid pregnancy had BPCR sessions individually. Some women could have only one session, some more, maximum 5, because of inclusion from mid pregnancy and availability of women during fixed village visits of research assistant. Women were included from mid pregnancy as in the area most women did not talk about pregnancy till mid pregnancy as well as resources for rural visits. Sonography is not done by many and if done is only in late pregnancy in camps. Women continued to get whatever services, from wherever they were getting in study as well as control villages. Pregnancy outcome was collected post birth in all the women included in study as well as control villages. Information regarding impact of awareness created about BPCR sessions was collected post birth.
Results
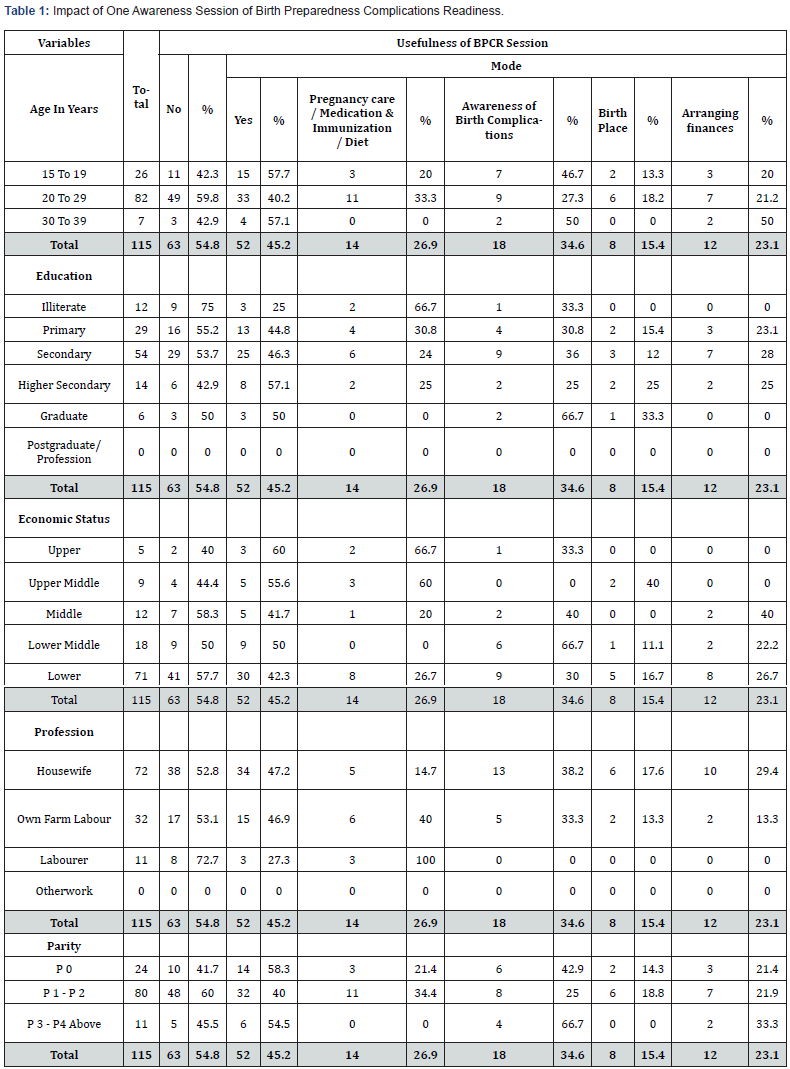
Over all 115 women could have only one session of BPCR. Of them 82 women were 20-29 years old, 33 (40.2%) of them found session useful, (9 (27.3%) in awareness of birth complications (BC), 6 (18.2%) in deciding the birth place, 7 (21.2%) in arranging finances and others for other reasons). Of 26 women who were 15-19 years old, 15 (57.7%) found session useful, (7 (46.7%) in creating awareness of BC, 2 (13.3%) in deciding the birth place, and 3 (20%) in arranging finances). Of the 29 women with primary school education, 13 (44.8%) found session useful, (9 (30.8%) in awareness of BC, 2 (15.4%) in deciding the birth place and 3 (23.1%) in arranging finances). Of 54 women who were secondary school educated, 25 (46.3%) found session useful, (9 (36%) in creating awareness of BC, 3 (12%) in deciding the birth place and 7 (28%) in arranging finances). Of 9 women from upper middle economic class, 3 (55.6%) found session useful, (no one said for awareness of BC, or in arranging finances. Of 71 women from lower economic class, 30 (42.3%) women found session useful, (9 (30%) in awareness of BC, 5 (16.7%) in deciding the birth place and 8 (26.7%) in arranging finances). Of the 72 housewives, 34 (42.7%) found session useful, (13 (38.2%) in awareness of BC, 6 (17.6%) in deciding the birth place, and 10 (29.4%) in arranging finances). Of 11 labourers, 3 (27.3%) found session useful, but no one said for BPCR or place of birth. Of the 24 women with no birth, 14 (58.3%) found session useful, (6 (42%) in awareness of BC, 2 (14.3%) in deciding the birth place, and 3 (21.4%) in arranging finances). Of the 80 women with more births, 32 (40%) found session useful, (8 (25%) in awareness of BC, 6 (18.8%) in deciding the birth place and 7 (21.9%) in arranging finances) (Table 1).
Of the 82 women of 20-29 years out of the 115 women who had one session, 10 (12.2%) had Home Births (HBs), 36 (43.9%) at Subcentre (SC), 21 (25.6%) at Primary Health Centre (PHC), 5 (6.1%) at District Hospital (DH) and 10 (12.2%) at Referral Hospital (RH). Total 80 (97.6%) women had live births (LBs), 2 (2.4%) still births (SBs), and 3 (3.8%) neonatal deaths (NNDs) occurred. Of 26 women of 15-19 years, 5 (19.2%) had HBs, 9 (34.6%) at SCs, 8 (30.8%) at PHCs, 1 (3.8%) DHs and 3 (11.8%) at RHs. Total 24 (92.3%) had LBs, 2 (7.7%) SBs, with 3 (12.5%) NNDs. Of 29 primary school educated women, 7 (24.1%) had HBs, 12 (41.4%) at SCs, 8 (27.6%) at PHCs, 1 (3.4%) at DH and 1 (3.4%) at RH. All 29 (100%) women had LBs, but 1 (3.4%) NND occurred. Of 54 secondary school educated, 7 (13%) had HBs, 25 (46.3%) at SCs, 14 (25.9%) at PHCs, 3 (5.6%) at DHs, and 5 (9.3%) at RHs. Total 53 (98.1%) women had LBs, 1 (1.9%) SB and 2 (3.8%) NNDs occurred. Of 9 women from upper middle economic class, 1 (11.1%) delivered at SC, 1 (11.1%) at PHC, 2 (22.2%) at DHs and 5 (55.6%) at RHs. All 9 (100%) women had LBs, but 1 (11.1%) NND occurred. Of 71 from lower economic class, 11 (15.5%) had HBs, 38 (53.5%) at SCs, and 22 (31%) at PHCs. Total 70 (98.6%) women had LBs, 1 (1.4%) SB and 2 (2.9%) NNDs occurred. Of 72 housewives, 4 (5.6%) had HBs, 33 (45.8%) at SCs, 18 (25%) at PHCs, 6 (8.3%) at DHs, and 11 (15.3%) at RHs. Total 70 (97.2%) women had LBs, with 2 (2.8%) SBs and 2 (2.9%) NNDs occurred. Of 11 women who were labourer, 6 (54.4%) had HBs, 4 (36.4%) at SCs and 1 (9.1%) at PHC. Total 10 (90.9%) had LBs, 1 (9.1%) SB and 3 (30%) NNDs occurred. Of 12 women with previous no birth, 5 (41.7%) had HBs, 8 (66.7%) at SCs, 7 (58.3%) at PHCs, 1 (8.3%) at DH, and 3 (25%) at RHs. Total 11 (91.7%) women had LBs, with 1 (8.3%) SB and 1 (9.1%) NND occurred. Of 71 women with many births, 10 (14.1%) had HBs, 34 (47.9%) at SCs, 21 (29.6%) at PHCs, 6 (7%) at DHs, and 10 (14.1%) at RHs. Of them 70 (98.6%) women had LB, with 1 (1.4%) SB and 2 (2.9%) NNDs occurred (Table 2).
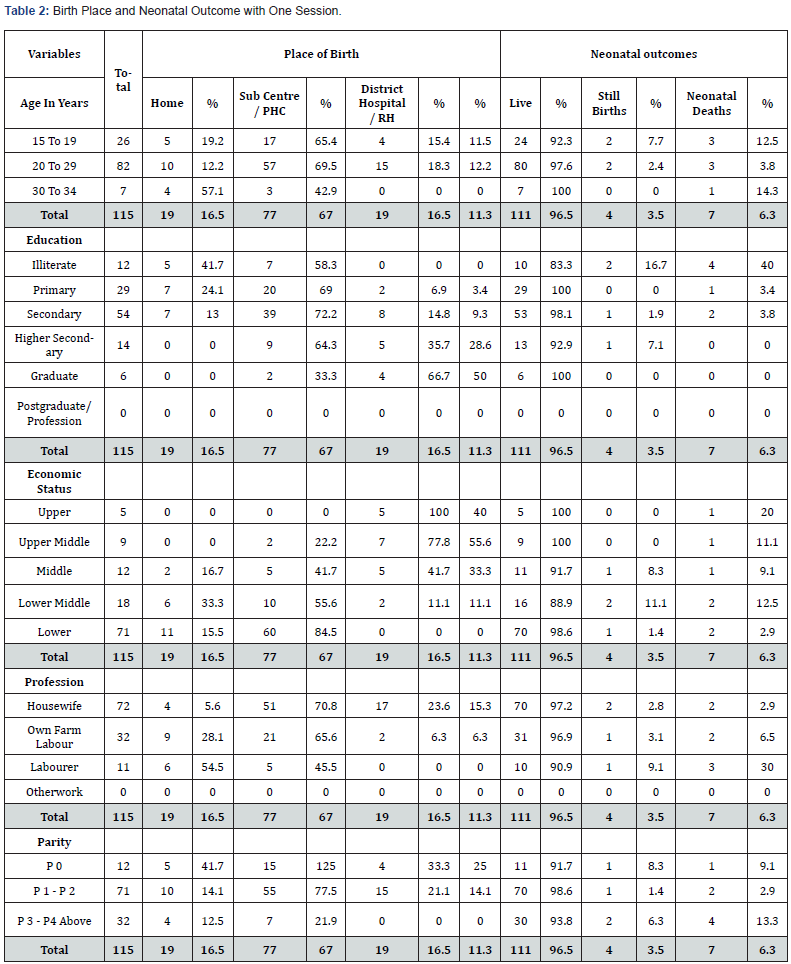
PHC – Primary Health Centre RH - Referred Hospital
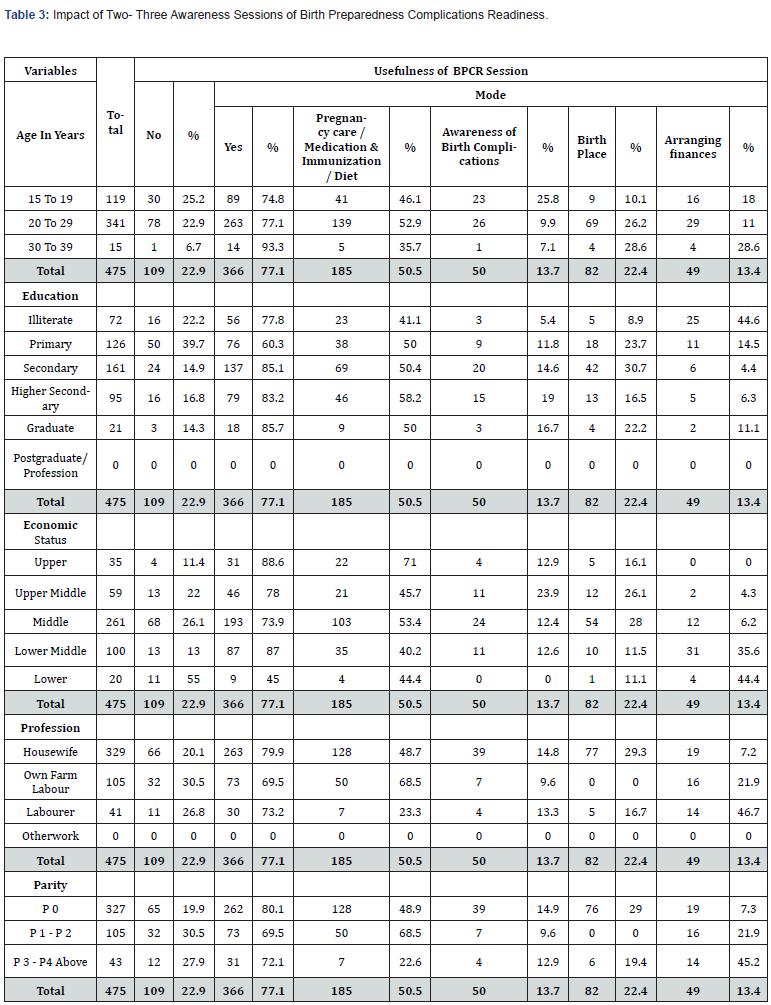
Out of 475 women who had 2-3 sessions of BPCR, 341 were 20-29 years old, and 263 (77.1%) women found sessions useful, (26 (9.9%) in creating awareness of BC, 69 (26.2%) in deciding the birth place and 29 (11%) in arranging finances). Of 119 women who were 15-19 years old, 89 (74.8%) found sessions useful, (23 (25.8%) in awareness of BC, 9 (10.0%) in deciding the birth place, and 16 (18%) in arranging finances). Of the 126 women who had primary school education, 76 (60.3%) found sessions useful, [9 (11.8%) in awareness of BC, 18 (23.7%) in deciding the birthplace and 11 (14.5%) in arranging finances]. Of the 161 secondary school educated women, 137 (85.1%) found sessions useful, (20 (14.6%) in creating awareness of BC, 42 (30.7%) in deciding the birth place and 6 (4.4%) in arranging finances). Of the 59 women from upper middle economic class, 46 (78%) found sessions useful, (11 (23.9%) said awareness of BC, 12 (26.1%) in deciding the birth place, and 2 (4.3%) in arranging finances). Of the 20 women from lower economic class, 9 (45%) found sessions useful, (1 (11.1%) in deciding the birth place and 4 (44.4%) in arranging finances). Of the 329 housewives, 263 (79.9%) women found sessions useful, (39 (14.8%) in awareness of complications during birth, 77 (29.3%) in deciding the birth place, and 19 (7.2%) in arranging finances). Of 41 labourer, 30 (73.2%) women found sessions useful, (4 (13.3%) in creating awareness of BC, 5 (16.7%) in deciding the birth place, and 14 (46.7%) in arranging finances). Of the 327 women who had no birth earlier, 262 (80.1%) found sessions useful, (39 (14.9%) in awareness of complications during birth, 76 (29%) in deciding the birth place, and 19 (7.3%) in arranging finances). Of the 105 women with many births, 73 (69.5%) found sessions useful, (7 (9.6%) in awareness of complications during birth, and 16 (21.9%) in arranging finances) (Table 3).
Of the 341 women of 20-29 years out of 475 women who had 2-3 sessions, 17 (5%) had HBs, 138 (40.5%) at SCs, 124 (36.4%) at PHCs, 23 (6.7%) at DHs and 39 (11.4%) at RHs. All women had LBs but 2 (0.6%) NNDs occurred. Of 119 women of 15-19 years, no one had HB, 54 (45.4%) at SCs, 42 (35.3%) at PHCs, 5 (4.2%) at DHs and 18 (15.1%) at RHs. All 119 (100%) women had LBs and 2 (1.7%) NNDs occurred. Of 126 primary school educated, 13 (10.3%) had HBs, 37 (29.4%) at SCs, 69 (54.8%) at PHCs, 7 (5.6%) at RHs and no one at DH. All 126 (100%) women had LBs but 1 (0.8%) NND occurred. Of 161 secondary school educated women, 2 (1.2%) had HBs, 107 (66.5%) at SCs, 41 (25.5%) at PHCs, 1 (0.6%) at DH, and 10 (6.2%) at RHs. All 161 (100%) women had LBs but 1 (0.6%) NND occurred. Of the 59 women from upper middle economic class, 2 (3.4%) delivered at SCs, 22 (37.3%) at PHCs, 10 (16.9%) at DHs and 16 (27.1%) at RHs. All 59 (100%) women had LBs but 1 (1.7%) NND occurred. Of 20 women from lower economic class, 3 (15%) had HBs, 10 (50%) at SCs, 5 (25%) at PHCs, and 2 (10%) at RHs. All 20 (100%) women had LBs, with no SB or NND. Of 329 housewives, 2 (0.6%) had HBs, 139 (42.2%) at SCs, 133 (40.4%) at PHCs, 24 (7.3%) at DHs, and 31 (9.4%) at RHs. All 329 (100%) had LBs but 2 (0.6%) NNDs occurred. Of 41 labourer, 3 (7.3%) had HBs, 23 (56.1%) at SCs, 6 (14.6%) at PHCs, and 9 (22%) at RHs. All 41 (100%) women had LBs, but 1 (2.4%) NND occurred. Of 43 women who had no birth earlier, 3 (7%) had HBs, 24 (55.8%) at SCs, 7 (16.3%) at PHCs and 9 (20.9%) at RHs. All 43 (100%) women had LBs, but 1 (2.3%) NND occurred. Of 327 women with many births, 2 (0.6%) had HBs, 138 (42.2%) at SCs, 132 (40.4%) at PHCs, 24 (7.3%) DHs, and 31 (9.5%) at RHs. All 327 (100%) women had LBs, but 2 (0.6%) NNDs occurred (Table 4).
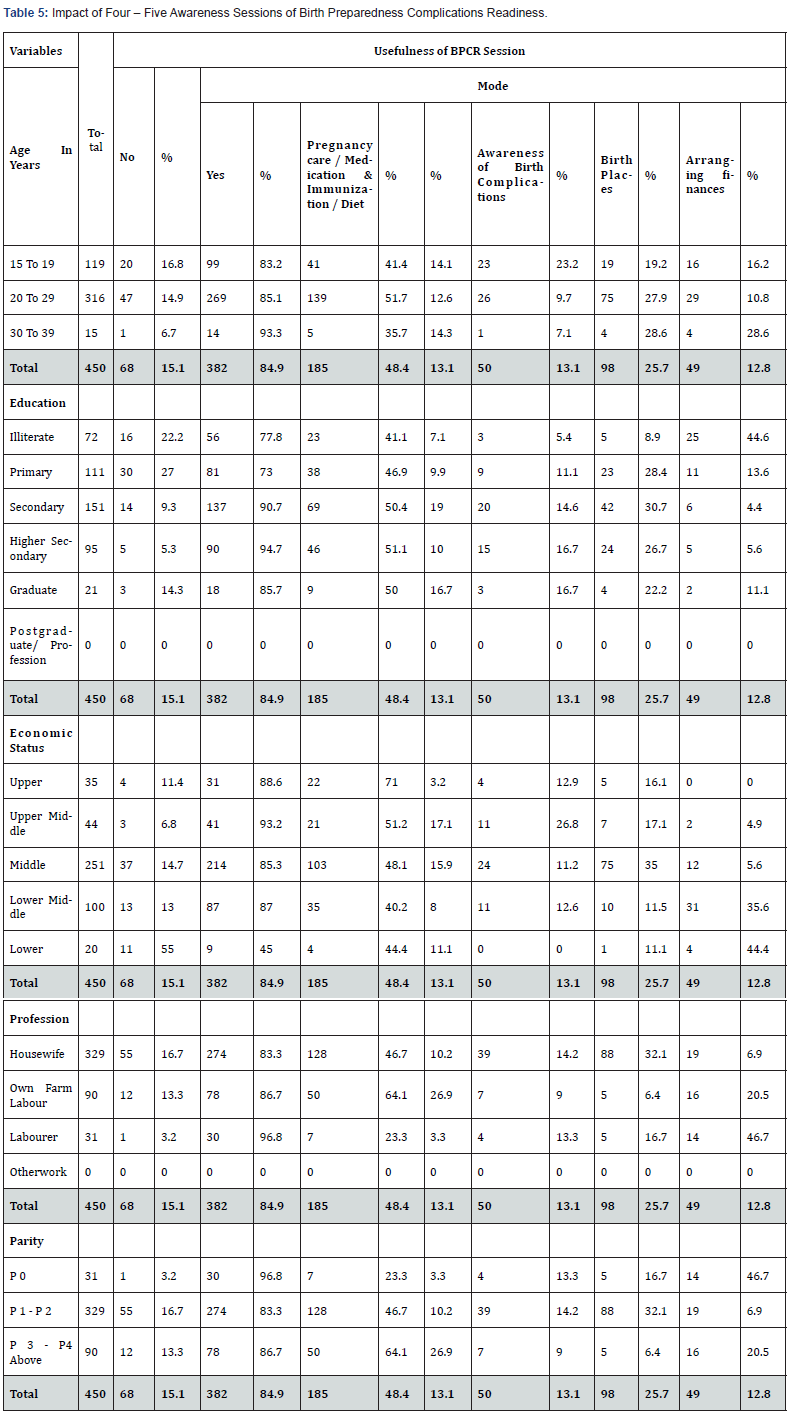
Total 450 women with had 4-5 sessions of BPCR, of 316 women were of 20-29 years, 269 (85.1%) found sessions useful, (26 (9.7%) in having awareness of complications during birth, 75 (27.9%) in deciding the birth place and 29 (10.8%) in planning arrangement of finances]. Of the 119 women who were 15-19 years old, 99 (83.2%) found sessions useful, (23 (23.2%) in having awareness of complications during birth, 19 (19.2%) in deciding the birth place, and 16 (16.2%) in arranging finances]. Of the 111 women who were primary school educated, 81 (73%) found sessions useful, (9 (11.1%) in being aware of BC, 23 (28.4%) in deciding the birth place and 11 (13.6%) in arranging finances). Of 151 secondary school educated women, 137 (90.7%) found sessions useful, (20 (14.6%) in creating awareness of BC, 42 (30.7%) in deciding the birth place and 6 (4.4%) in arranging finances). Of the 44 women from upper middle economic class, 41 (93.2%) found sessions useful, (11 (26.8%) in awareness of BC, 7 (17.1%) in deciding the birth place and 2 (4.9%) in arranging finances). Of 31 women from lower economic class, 30 (96.8%) found sessions useful, (4 (13.3%) in awareness of BC, 5 (16.7%) in deciding the birth place and 14 (46.7%) in arranging finances). Of the 329 housewives, 274 (83.3%) found sessions useful, [39 (14.2%) for awareness of complications during birth, 88 (32.1%) in deciding the birth place and 19 (6.9%) in arranging finances). Of 31 labourer, 30 (96.8%) found sessions useful, (4 (13.3%) in awareness of complications during birth, 5 (16.7%) in deciding the birth place and 14 (46.7%) in arranging finances]. Of the 31 women with no births, 30 (96.8%) found sessions useful, (4 (13.3%) in awareness of BC, 5 (16.7%) in deciding the birth place, and 14 (46.7%) in arranging finances). Of the 329 women with many births, 274 (83.3%) found sessions useful, (39 (14.2%) in awareness of BC, 88 (32.1%) in deciding the birth place and 19 (6.9%) in arranging finances) (Table 5).
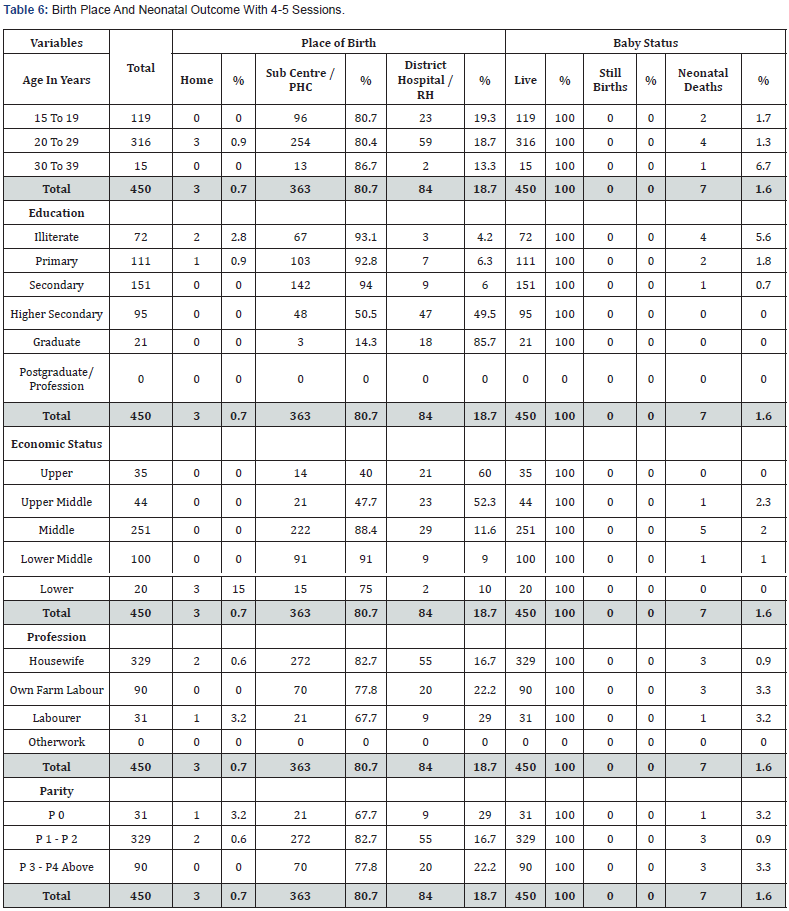
Out of 450 women with 4-5 sessions, of 316 women of 20-29 years, 3 (0.9%) had HBs, 129 (40.8%) at SCs, 125 (39.6%) at PHCs, 22 (7%) at DHs and 37 (11.7%) at RHs. All 316 (100%) women had LBs, but 4 (1.3%) NNDs occurred. Of 119 women who were 15-19 years old, no one had HB, 54 (45.4%) at SCs, 42 (35.3%) at PHCs, 5 (4.2%) at DHs and 18 (15.1%) at RHs. All 119 (100%) women had LBs and 2 (1.7%) NNDs occurred. Of 111 primary school educated women, 1 (0.9%) had HB, 33 (29.7%) at SCs, 70 (63.1%) at PHCs, and 7 (6.3%) at RHs. All 111 (100%) women had LBs but 2 (1.8%) NNDs occurred. Of 151 secondary school educated, 101 (66.9%) delivered at SCs, 41 (27.2%) at PHCs, 1 (0.7%) at DH, and 8 (5.3%) at RHs and no one had HB. All 151 (100%) had LBs with 1 (0.7%) NND. Of 44 women from upper middle economic class, 12 (27.3%) delivered at SCs, 9 (20.5%) at PHCs, 9 (20.5%) at DHs and 14 (31.8%) at RHs and no one had HB. All 44 (100%) had LBs and 1 (2.3%) NND occurred. Of 20 women from lower economic class, 3 (15%) women had HBs, 10 (50%) at SCs, 5 (25%) at PHCs and 2 (10%) at RHs. All 20 (100%) women had LBs, and no NND. Of 329 housewives, 2 (0.6%) had HBs, 139 (42.2%) at SCs, 133 (40.4%) at PHCs, 24 (7.3%) at DHs, and 31 (9.4%) at RHs. All 329 (100%) had LBs, but 3 (0.9%) NNDs occurred. Of 31 labourer women, 1 (3.2%) had HB, 15 (48.4%) at SCs, 6 (19.4%) at PHCs, and 9 (29%) at RHs.
All 31 (100%) women had LBs, but 1 (3.2%) NND occurred. Of 31 women who had no birth earlier, 1 (3.2%) had HB, 15 (48.4%) at SCs, 6 (19.4%) at PHCs, and 9 (29%) at RHs. All 31 (100%) had LBs, but 1 (3.2%) NND occurred. Of 329 with many births, 2 (0.6%) had HBs, 139 (42.2%) at SCs, 133 (40.4%) at PHCs, 24 (7.3%) at DHs, and 31 (9.4%) at RHs. All 329 (100%) women had LBs, but 3 (0.9%) NNDs occurred. There was no maternal death (Table 6).
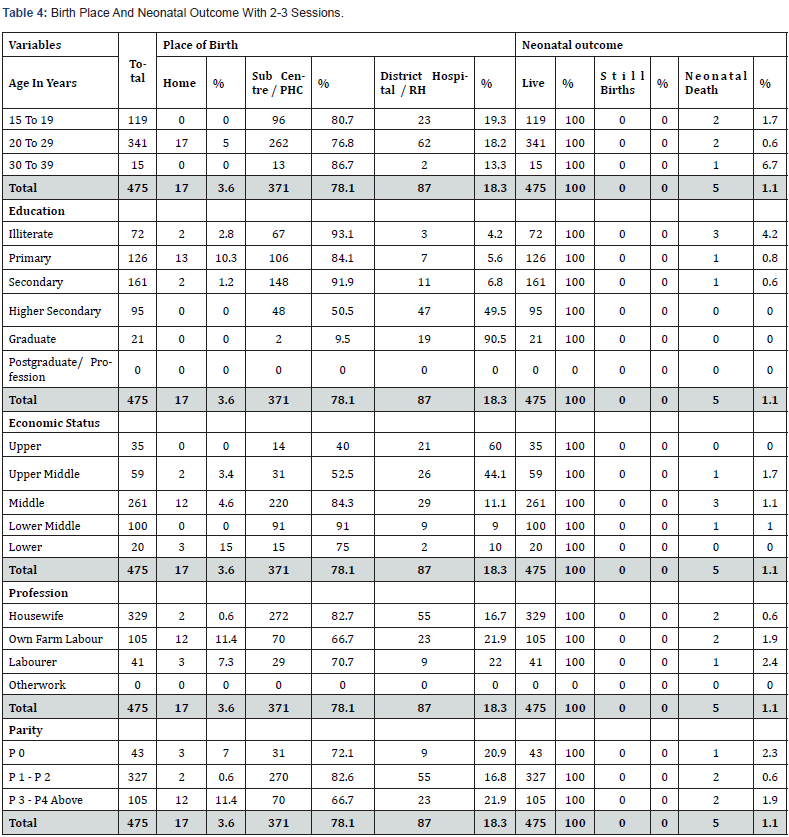
PHC – Primary Health Centre RH - Referred Hospital
PHC – Primary Health Centre RH - Referred Hospital
PHC – Primary Health Centre RH - Referred Hospital
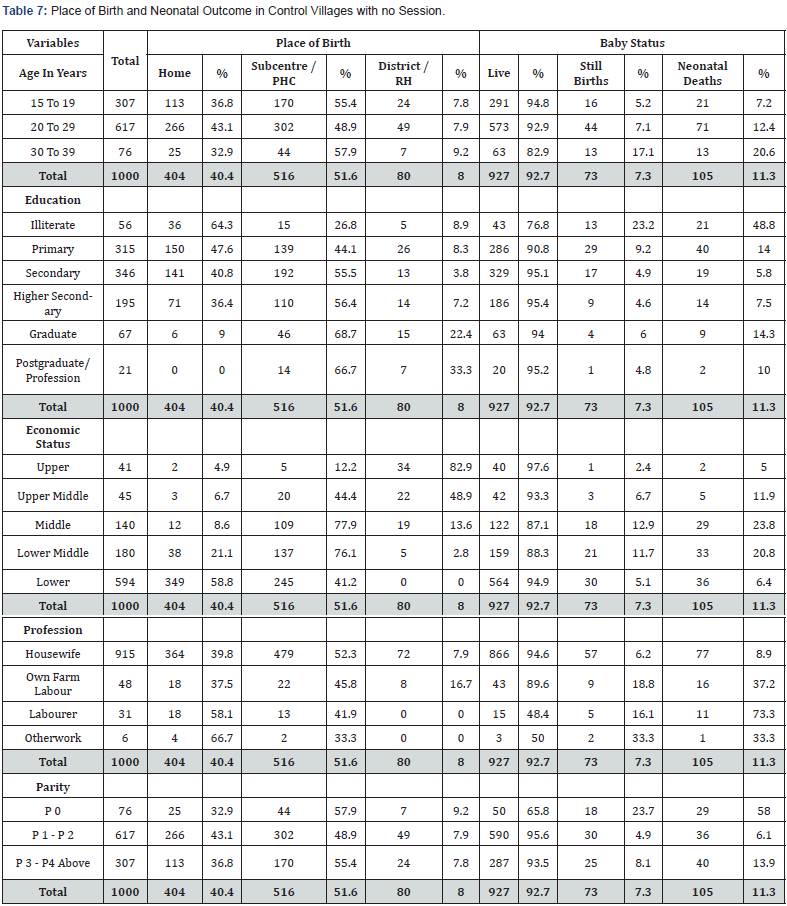
Of the 1000 women who did not have any BPCR awareness session, 617 were 20-29 years old, 266 (43.1%) had HBs, 191 (31%) at SCs, 111 (18%) at PHCs, 17 (2.8%) at DHs and 32 (5.2%) at RHs. Of total 307 of 15-19 year old, 113 (36.8%) had HBs, 100 (32.6%) at SCs, 70 (22.8%) at PHCs, 9 (2.9%) at DHs and 15 (4.9%) at RHs. Of 315 primary school educated, 150 (47.6%) had HBs, 82 (26%) at SCs, 57 (18.1%) at PHCs, 11 (3.5%) at DHs and 15 (4.8%) at RHs. Of 346 were secondary school educated, 141 (40.8%) had HBs, 111 (32.1%) at SCs, 81 (23.4%) at PHCs, 4 (1.2%) at DHs and 9 (2.6%) at RHs. Of 45 women from upper middle economic class, 3 (6.7%) had HBs, 6 (13.3%) at SCs, 14 (31.1%) at PHCs, 7 (15.6%) at DHs and 15 (33.3%) at RHs. Of 594 from lower economic class, 349 (58.8%) had HBs, 172 (29%) at SCs, 73 (12.3%) at PHCs, and no one at DH. There was significant difference with no session, one, 2-3, 4-5 sessions with economic classes (p value is 0.001). Of 76 women who had no birth earlier, 25 (32.9%) had HBs, 33 (43.3%) at SC, 11 (14.5%) at PHC, 2 (2.6%) at DH and 5 (6.6%) at RH. Of 617 women with many births, 266 (43.1%) had HBs, 191 (31%) at SCs, 111 (18%) at PHCs, 17 (2.8%) at DHs and 32 (5.2%) at RHs (Table 7).
Of 617 women of 20-29 years out of 1000 women in control villages, 573 (92.9%) had LBs, 44 (7.1%) SBs and 71 (12.4%) had NNDs. Of 307 women of 15-19 yrs, 291 (94.8%) had LBs, 16 (5.2%) SBs and 21 (7.2%) NNDs occurred. There was significant difference even in 15-19 years age group with no session, one, 2-3, and 4-5 sessions of BPCR (p value is <.0001). Of 315 primary school educated women, 286 (90.8%) had LBs, 29 (9.2%) had SBs and 40 (14%) NNDs occurred. Of 346 secondary school educated women, 329 (95.1%) had LBs, 17 (4.9%) SBs and 19 (5.8%) NNDs occurred. There was significant difference with better education with no session, one, 2-3, and 4-5 sessions (p value is <.01). Of the 45 women from upper middle economic class, 42 (93.3%) had LBs, 3 (6.7%) had SBs and 5 (11.9%) NNDs occurred. Of the 594 women from lower economic class, 564 (94.9%) had LBs, 30 (5.1%) had SBs and 36 (6.4%) NNDs occurred. There was significant difference, inrespective of economic status with no session, one, 2-3, and 4-5 sessions in neonatal outcome (p value is <.00001). Of the 915 housewives, 781 (85.4%) had LBs, 57 (6.2%) had SBs and 77 (9.9%) NNDs occurred. Of the 31 labourer, 25 (80.6%) had LBs, 5 (16.1%) SBs and 1 (3.2%) NND occurred. There was significant difference in profession with no session, one, 2-3, and 4-5 sessions (p value is <.00001). Of the 594 women who had many births, 528 (88.9%) had LBs, 30 (5.1%) had SBs and 36 (6.8%) NNDs occurred. There was significant difference with parity with no session, one, 2-3, and 4-5 sessions (p value <.001). There was no maternal death.
Discussion
The concept of BP CR emerged almost two decades back and has been included by the World Health Organization (WHO) as an essential part of the antenatal care [3,4]. BP means prebirth awareness about needs during birth, and after birth, with mission of improving pregnancy outcome. Johnson [5], opined that ‘BPCR were set of interventions that aimed to identify and modify biomedical, behavioural, and social risks to a woman’s health or pregnancy outcome through timely prevention and therapy’. The aim of BPCR is to improve pregnancy outcome for mothers and newborns, by optimizing health before labour by preventive, curative or promotive interventions, safe birth place, and timely appropriate actions if complications occur. Mbonu et al. [6], with their study in Nigeria, reported that few pregnant women had made adequate arrangements in anticipation of safe birth. Ketema et al. [7], from Ethiopia reported that the proportion of women with BPCR remained low. Maternal education had a positive effect on the level of BPCR. Hudson et al. [8], did a study in Kenya and reported that those mothers who had BP sessions 3 times, were more likely to experience favourable birth outcome than those who did not. In the present study also 2-3 BPCR sessions significantly changed pregnancy outcome. It was found that 40.4% delivered at home amongst those who had no session, 16.5% after one session, with 2-3 sessions PHC births increased to 42.3% and HBs reduced to 3.6% and women who had 4-5 sessions, the HBs were only 0.7% and PHCs births increased to 38%, result is significant (p-value <.016673) in birth place with no session, one, 2-3 and 4-5 session. The NNDs reduced from 11.3% in women with no session, 6.3% in women who had one session to 3.1% with 2-3 times sessions to a significantly low number of 1.6% in women who had 4-5 sessions. There was significant difference (p-value <0.0001). Soubeiga et al (2013) did a study, in Canada to search for a link between the characteristics of the center delivering the health care and the probability of being exposed to information and advice about BP. Women reported receiving advice about institutional delivery (72%), danger signs (55%), cost of institutional delivery (38%) and advice on transportation in the event of emergency (12%). Number of antenatal visits was one independent factor associated with getting BP advice. In the present study also with 4-5 sessions birth places and baby outcome changed significantly. Tura et al2 did a study to know the effects of BPCR on utility of skilled care in Southwest Ethiopia. The status of skilled care at birth was 17.5%. Planning to use skilled care during pregnancy was found to increase significantly. Yohai et al. [9], did a study in Israel and reported that the knowledge acquired had positive effects on the course of labor and delivery outcomes. Shukla et al. [10], did a study in Uttarpradesh of India and reported that focused BPCR counseling could play an important role in increasing the awareness of pregnant women regarding BC. BPCR aims to reduce delays in seeking care, promote skilled birth attendance, and facility deliveries, deciding to seek care (delay one), reaching maternal health care facility in time (delay two), and receiving adequate care (delay 3) [11]. These three delays have multiple prongs which affect outcome. Goodburn [12] and Graham [13] opined that little was known about BP practices among populations living in hard-to-reach areas. So we did the study and did find some impact. Despite poor functioning health systems in low-and middle income countries, increased BPCR should allow women and their families to anticipate potential delays and ensure timely use of skilled care for birth and arrival at the appropriate facility for any complications. A recent systematic review of randomized controlled trials also revealed that BPCR strategies could reduce maternal and neonatal mortality [14]. Seven out of the twelve included studies implemented BPCR through action-learning cycles with women’s groups, a specific intervention and methodology which reported improvements in maternal and newborn health outcomes [15,16]. Miltenburg et al. [17], did a systematic review and found that BPCR interventions increased knowledge of BPCR, desired place of birth; preferred birth attendant, location of the closest facility for birth and its complications, funds, supplies and materials to bring to the facility; an identified labour and birth companion, an identified support person to look after other children at home, identified transport and identification of compatible blood donors. In a low resource rural, hilly forestry region of Central India, present study aimed to know the impact of BPCR awareness sessions. Of the 1000 women who had no session, 404 (40.4%) women had HBs, and 927 (92.7%) had LBs, 73 (7.3%) SBs, and 105 (11.3%) NNDs occurred. Of the 115 women who could have only one session, 52 (45.2%) women found session useful, 10 (16.5%) women had HBs, and 111 (96.5%) had LBs, 4 (3.5%) SBs, and 7 (6.3%) NNDs occured. Of the 475 women who could have 2-3 sessions of BPCR, 366 (71.1%) women found sessions useful, only 17 (3.6%) had HBs, 475 (100%) had LBs, and 5 (1.1%) NNDs occurred. Of the 450 women who could have 4-5 session of BPCR, 382 (84.9%) women found sessions useful, only 3 (0.7%) had HBs, 450 (100%) had LBs, and 7 (1.6%) NNDs. Very very significant change occurred, as the awareness sessions increased, but even one session midpregnancy helped. Moinuddin et al. [18], after doing a sectional survey reported that greater emphasis on BPCR interventions tailored for hard-to-reach areas were needed to improve skilled birth attendance, care seeking for complications and essential newborn care. Since BP is a new concept, hence currently fragmented, though there is potential to positively impact pregnancy outcome. Taking care of the health status before labour is not familiar to those who would benefit most from it. Kinney [19], suggested that while the primary objective of BP/CR was to increase care seeking, mortality reduction, benefits also depended on accessibility and availability of services being provided and this made the contributing effectes of the BP/CR interventions on mortality less clear. Maharashtra is one of the largest states of India with better economic status as well as health indicators, but in the same province in the Melghat region, situation is different. The region where the study was done has more problems because of forests, hills with a tiger reserve with the inherent restrictions about roads, transport, and difficulties of communication. Some villages get completely disconnected during rain. So BPCR becomes imperative. As such in spite of the best of the community care, some women need treatment at health facility for survival because it is very well known that around 10-15% pregnant women do develop complications and need special care not possible at home [19]. In India BP has been there with various celebrations in last few weeks of pregnancy and preparations for newborn’s welcome. Some rituals have scientific linkages too. For example women ware a lot of bangles around their wrists and forearms during the ‘Baby Shower’ ceremony, which can help as an early warning sign for HDsP. Miltenburg [17], reported that BPCR interventions can increase knowledge of BPCR, but did not always correspond to an increase in the use of a skilled attendant at birth. In the present study there was real impact on place of birth and baby outcome. Saaka et al. [20], did a study to assess BPCR and associated factors among mothers who had given birth over a year prior to the study and reported that BPCR practices were low. Study by Debelie et al [21], to know about of BPCR practice and associated factors among pregnant women in Ethiopia, revealed that BPCR practice was higher than previous studies conducted in the country, however BPCR practices were found to be lower than the standard that every woman should practice. Ely et al. [22], did a study about informed consent and BPCR and reported that 55% of participants suggested policy change in favour of increased BPCR. WHO [23], reported the risks of BP like intruding on the privacy for women, diluting effects of certain interventions if stretched too far and neglecting existing maternal, neonatal and child health interventions that work, medicalizing issues that were better dealt with by experts or stakeholders in other domains (e.g. sociocultural, religious). Risks of care also included blaming women (stigmatization, undermining women’s autonomy). Present study envisioned reduction in maternal, perinatal mortality, maternal neonatal severe, morbidity and there was impact even in women with extreme poverty. There was difference in place of baby with no session, one, 2-3 and 4-5 sessions even adolescents (p-value <0.0001). Of the 115 women who could have only one session, 26 women were 15-19 year, 15 (57.7%) women found session useful, 5 (19.2%) women had HBs, and 24 (92.3%) had LBs, 2 (7.7%) SBs, and 3 (12.5%) NNDs onwards. Of the 475 women who could have 2-3 sessions, 119 women were 15-19 year old, 89 (74.8%) women found sessions useful, no woman had HBs, and 119 (100%) had LBs, and 2 (1.7%) NNDs occurred. Of the 450 women who could have 4-5 sessions, 119 women were 15-19 year, 99 (83.2%) women found sessions useful, no woman had HBs, and 119 (100%) had LBs, and 2 (1.7%) NNDs onwards. Of the 307 women of 15-19 years out of 1000 women who had no sessions, 113 (36.8%) had HBs, 100 (32.6%) at SC, 70 (22.8%) at PHC, 9 (2.9%) at DH and 15 (4.9%) at RH, 291 (94.8%) had LBs, 16 (5.2%) SBs and 21 (7.2%) NNDs occurred. Of the 115 women who could have only one session, 12 women were illiterate, 3 (25%) found session useful, 5 (41.7%) had HBs, and 10 (83.3%) had LBs, 2 (16.7%) SBs, and 4 (40%) NNDs occurred. Of the 475 women who could have 2-3 session, 72 women were illiterate, 56 (77.8%) women found sessions useful, 2 (2.8%) had HBs, and 72 (100%) had LBs, and 3 (4.2%) NNDs occurred. Of the 450 women who could have 4-5 sessions, 72 women were illiterate, 56 (77.8%) women found sessions useful, 2 (2.8%) women had HBs, and 72 (100%) had LBs, and 4 (5.6%) NNDs onwards. So sessions 1 and 2-3 and 4-5 made a significant different even in illiterate but 2-3 or 4-5 had no difference (p-value <0.0001). Total 56 women were illiterate out of 1000 women who had no sessions, 36 (64.3%) had HBs, 13 (23.2%) at SCs, 2 (3.6%) at PHCs, 2 (3.6%) at DHs and 3 (5.4%) at RHs, 43 (76.8%) had LBs, 13 (23.2%) SBs and 21 (48.8%) NNDs occurred. There was difference (p-value <0.0001) in place of baby even in illiterate. Of the 594 women of lower economic out of 1000 women who had no session, 349 (58.8%) had HBs, 172 (29%) at SCs, 73 (12.3%) at PHCs, no one DH and RH, 564 (94.9%) had LBs, 30 (5.1%) SBs and 36 (6.4%) NNDs occurred. Of 71 women of lower economic class, out of the 115 women who could have only one session, 30 (42.3%) women found session useful, 11 (15.5%) women had HBs, and 70 (98.6%) LBs, 1 (1.4%) SB, and 2 (2.9%) NNDs occurred. Of the 475 women who could have 2-3 sessions, 20 women were of lower economic class, 9 (45%) found sessions useful, 3 (15%) had HBs, and 20 (100%) had LBs, and no NND occurred. Of the 450 women who could have 4-5 sessions, 20 women were illiterate, 9 (45%) found sessions useful, 3 (15%) women had HBs, and 20 (100%) had LBs, and 4 (5.6%) NNDs occurred. There was no maternal death. Limitations of study were only clearly known information was analyzed. Maternal sicknesses could not be analyzed because information on papers was not complete, and women could not provide clearly.
Conclusion
BPCR awareness helped increase facility births, improved neonatal outcome, especially with 2-3 and 4-5 sessions, though one session also affected, and this was inrespective of age, literacy, social class. It has been observed that BPCR awareness helped increase facility births, improved neonatal outcome. Improvement was directly proportional to the no of sessions and less dependent on other variables like age, literacy, economic status and occupation.
Conflict of Interest
Nil
Funding and Acknowledgement
We are grateful to The Foundation for Collaborative Medicine and Research, USA for the support for doing the study. We thank the rural tribal communities for the cooperation in conducting the study and all those who have helped in the study.
References
- World Health Organization (2010) Packages of interventions for family planning, safe abortion care, maternal, newborn and child health.
- Tura G, Afework MF, Yalew AW (2014) The effect of birth preparedness and complication readiness on skilled care use: a prospective follow-up study in Southwest Ethiopia. Reproductive health 11(1): 1.
- Carroli G, Villar J, Piaggio G, Khan-Neelofur D, Gülmezoglu M, et al. (2001) WHO systematic review of randomised controlled trials of routine antenatal care. Lancet 357(9268): 1565-1570.
- Dean SV, Imam AM, Lassi ZS, Bhutta ZA (2013) Systematic review of preconception risks and interventions. Pakistan: Division of Women and Child Health, Aga Khan University.
- Johnson K, Posner SF, Biermann J, Cordero JF, Atrash HK, et al. (2006) Recommendations to improve preconception health and Health Care—United States: report of the CDC/ATSDR preconception care work group and the select panel on preconception care. Morbidity and Mortality Weekly Report: Recommendations and Reports 55(6):1-CE.
- Mbonu EO (2018) Knowledge, Attitude and practice of birth preparedness and complication readiness amongst pregnant women in Eti-OsaLga, Lagos. Universal Journal of Public Health 6(4): 220-230.
- Ketema DB, Leshargie CT, Kibret GD, Assemie MA, Petrucka P, et al. (2020) Effects of maternal education on birth preparedness and complication readiness among Ethiopian pregnant women: a systematic review and meta-analysis. BMC pregnancy and childbirth. 20(1): 149.
- Hudson I, Gatongi PM, Nyongesa P, Makwali J, Mudany M (2016) The impact of birth preparedness on pregnancy outcome: findings from Lurambi Sub county, Kakamegacounty, Kenya. J Pregnancy Child Health 3:269.
- Yohai D, Alharar D, Cohen R, Kaltian Z, Aricha-Tamir B, et al. (2018) The effect of attending a prenatal childbirth preparedness course on labor duration and outcomes. J Perinat Med 46(1): 47-52.
- Shukla M, Khan NZ, Agarwal A, Dwivedi AD, Singh JV, et al. (2019) Effect of focused birth preparedness and complication readiness counseling on pregnancy outcome among females attending tertiary care hospital in Barabanki district, Uttar Pradesh, India. Journal of education and health promotion 8.
- Thaddeus S, Maine D (1994) Too far to walk: maternal mortality in context. Soci Sci Med 38 (8): 1091–1110.
- Goodburn E, Campbell O (2001) Reducing maternal mortality in the developing world: sector-wide approaches may be the key. BMJ 322(7291): 917-920.
- Graham WJ (2002) Now or never: the case for measuring maternal mortality. Lancet 359(9307): 701-704.
- Soubeiga D, GauvinL, Hatem MA, Johri M (2014) Birth Preparedness and Complication Readiness (BPCR) interventions to reduce maternal and neonatal mortality in developing countries: systematic review and meta-analysis. BMC Pregnancy and Childbirth 14:129.
- Prost A, Colbourn T, Seward N, Azad K, Coomarasamy A, et al. (2013) Women’s groups practising participatory learning and action to improve maternal and newborn health in low-resource settings: a systematic review and meta-analysis. 38 (9879): 1736-1746.
- World Health Organization (2014) WHO recommendation on community mobilization through facilitated participatory learning and action cycles with women’s groups for maternal and newborn health.
- Solnes Miltenburg A, Roggeveen Y, Van Elteren M, Shields L, Bunders J, et al. (2013) A protocol for a systematic review of birth preparedness and complication readiness programs. Systematic Reviews 2(1): 11.
- Moinuddin M, Christou A, Hoque DE, Tahsina T, Salam S, et al. (2017) Birth preparedness and complication readiness (BPCR) among pregnant women in hard-to-reach areas in Bangladesh. PLoS One 12(12): e0189365.
- Kinney MV, Boldosser-Boesch M, McCallon B (2016) Quality, equity, and dignity for women and babies. Lancet 388(10056): 2066-2068.
- Saaka M, Alhassan L (2021) Prevalence and predictors of birth preparedness and complication readiness in the Kassena-Nankana district of Ghana: an analytical cross-sectional study. BMJ open 11(3): e042906.
- Debelie TZ, Abdo AA, Anteneh KT, Limenih MA, Asaye MM, et al. (2021) Birth preparedness and complication readiness practice and associated factors among pregnant women in Northwest Ethiopia: 2018. Plos one 16(4): e0249083.
- Ely S, Langer S, Dietz HP (2022) Informed consent and birth preparedness/complication readiness: A qualitative study at two tertiary maternity units. Aust N Z J Obstet Gynaecol 62(1): 47-54.
- World Health Organization (2013) Preconception care to reduce maternal and childhood mortality and morbidity: policy brief.






























