Facility Readiness Assessment for Implementationof Adolescent and Youth Health Care Service in Central Zone, Southern Ethiopia
Achamyelesh Gebretsadik1* Nebiyu Melaku2 and Yemisrach Shiferaw1
1Hawassa University college of Medicine and Health Science, School of public and Environmental Health Science, Ethopia
2Southern Nation Nationalities People Regional Health Bureau Maternal and child health Core process
Submission: January 02, 2019; Published: March 26, 2019
*Corresponding author: Achamyelesh Gebretsadik, Hawassa University, Hawassa, Ethiopia
How to cite this article: Achamyelesh G, Nebiyu M, Yemisrach S. Facility Readiness Assessment for Implementationof Adolescent and Youth Health Care Service in Central Zone, Southern Ethiopia. Glob J Reprod Med. 2019; 6(4): 555693. DOI:10.19080/GJORM.2019.06.555693.
Abstract
Background: In 2016, a new strategic plan is developed nationally to address the adolescent and youth health issues holistically. For its implementation, it is important to assess the available resources at health facilities. The aim of this study was to assess the readiness of the health facilities for the implementation of comprehensive adolescent and youth health care.
Methods: A cross-sectional study was conducted among the youth-friendly service delivering and not delivering health facilities with 1:1 ratio in the central zones of Southern Nations Nationalities People Region from May 14-26, 2017. A total of 14 health centers was selected using lottery methods. The data were collected through interview and observation. Interviews were done among 14 health facility managers 14 health care providers and 5 district health office heads. Data were entered into Microsoft Excel 2010 software and descriptive analysis was made.
Result: Totally, 14 health facilities were observed. Of all 42.8% of health facilities have at least six health officers, 78.5% have more than ten diploma nurses, 85.7% have diploma midwifery at least one, 70% have no displayed information items such as the rights of adolescent to information, only 50% of them have a waiting room. 75% were working in a room with no curtains in windows and doors, no screen separating the consultation area from the examination area to maintain privacy during the consultation. All health facility managers and heads of the district health office mentioned that shortage of trained manpower as a result of frequent turnover, budget, vehicle, and room were critically hampered the implementation of the services as required.
Conclusion: It is possible to begin the comprehensive adolescent and youth health care service with the existing manpower health professionals and rooms. However, the training of health care providers and fulfilling the necessary medical supplies and materials are important. So, service quality will be improved based on the standards in collaboration with different stakeholders and partners.
Keywords: Facility readiness; Adolescent youth; Southern ethiopia
Abbrevations: AYHS: Adolescent and Youth Health Service; SNNPR: Southern Nation Nationalities People Region; HMIS: Health Management Information Systems; AYFS: Adolescent and Youth Friendly Services
Background
Adolescents and youth comprise one-third of the world’s population [1], whom 90% live in developing countries [1]. Overall the proportion of adolescent and youth expected to rise from 20% to 50% within the coming thirty years [2]. Ethiopia is a young country with 71 % of the populations are under the age of thirty and 10-24 years were 33.8 % [3,4]. Investing in young people (ages 10 to 29) now will lay the groundwork for future. Adolescent and youth is a critical age for risk taking and critical period for professional intervention [5,6]. Intervention in this time help adolescent and youth to make appropriate decision for the future live and can prevent risk behaviors which can also affect their adulthood health. Adolescent and youth need different approach than adult in service provision. Currently adolescent and youth are not getting the expected services worldwide [6,7].
Mortality rate of adolescent and youth are rising due to several health problems. Especially road traffic accident is the first contributor for mortality. Non communicable diseases and mental illness also another contributor for morbidity and mortality of adolescent and youth [7]. Globally a number of initiatives have been taken place over the last decades to provide adolescent and youth responsive health care [8,9]. However, most of the initiatives were focusing only on sexual and reproductive health issues [10-12].
Similarly, in Ethiopia though it was not in an integrated and comprehensive manner there were a lot of straggles to address adolescent and youth health since 2000 [13-16]. However, with all the efforts made the intended improvement not achieved in the health of adolescents and youth due to health system was not responsive and young people not utilized the service. Therefore, federal ministry of health revised the previous strategy and launched a new strategy that comprise comprehensive adolescent and youth health care and to make the health system responsive for that comprehensive approach [17]. Therefore, the aim of this study was to assess facility readiness for the implementation of comprehensive adolescent and youth health care.
Methods
Study settings
The Southern Nations Nationalities and Peoples’ Regional State is the third largest administrative region of Ethiopia and represents about 20% of the country’s population with close to 20 million people. The central zones of Wolita and Hadiya zones and Halaba special district contributes more than 20% of the regions population. Wolaita zone has five hospitals, 69 health centers, 372 health posts and 98 private clinics. Hadiya zone has one general hospital, 4 primary hospitals 61 health centers and 305 health posts. In Halaba there are 7 health centers and 50 health posts.
Study area and period: This readiness assessment was conducted in 14 health centers of the central zones of Southern Nation Nationalities People Region health facilities from May 14- 26, 2017.
Study design: A cross-sectional study was conducted in two central zones namely Wolaita and Hadiya and one special district (Halaba).
Sampling criteria: The zones and special district were selected purposively. Since these two zones and districts have high population density and their proximity to the head quarter of the region might be a true representative of the general health facility of the region. From Wolaita zone, six health centers were selected from five districts (namely, Offa, Damot Pulasa, Damot Gale, Bodity and Sodo). And from Hadiya zone, three districts and six health facilities and from Halaba special district one from started and one from not started were selected based on their youth friendly service delivery status among started and non-started 1:1 ratio. The health centers were selected using lottery methods (Table 1).
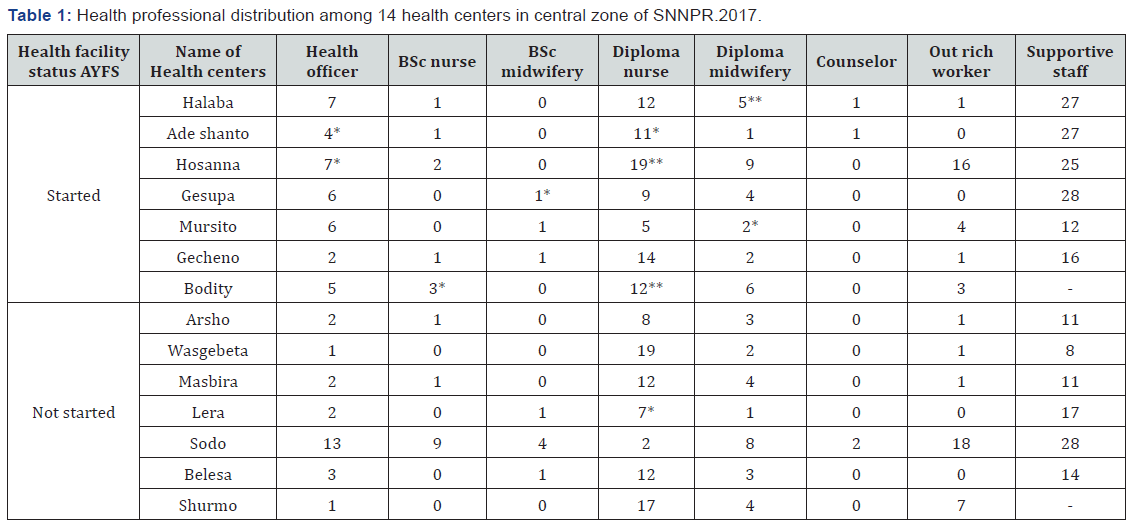
Study population: Health care providers (nurse and health officers), health center managers and district health office heads of the selected health facility.
Data collection and sources: Data were collected from 7-19 May 2017. Five reproductive health professional data collectors/ technical assistant were hired and trained to collect the data. Data were collected through interview and observation using questionnaires and observation check list prepared to assess national adolescent and youth health service quality by Federal Ministry of Health (FMOH). Interview were done among health providers (nurse and health officers) those working in youth friendly service room from started health centers and maternal and child health nurses from non-started health centers and health center managers and district health office heads. The collected data were entered in to Microsoft Excel 2010 software and descriptive analysis was made using percentage.
Classification criteria: Readiness of the facility was assessed based on the standard set by World Health Organization for adolescent and youth health [18]. When the facilities fulfilled>=75% of the standards we considered ready for that element i.e. staff, basic amenities etc. Support letter was also taken from RHB maternal and child health and nutrition core process office to the two zones and Halaba special district and district health office heads also communicated officially to get consent from each health centers.
Result
Staffing
During the survey, 14 health facilities, their managers, one health care provider from each and 5 district health office heads were interviewed. Of all 6 (42.8%) of health facilities have at least five health officers, 9 (64.2%) have more than ten diploma nurses, 7 (50%) have diploma midwifery at least four and 6 (42.8%) have no bachelor nurse and midwifery (Table 1). Staff numbers and their orientation to the right and confidential delivery of service is important for provision of quality adolescent and youth friendly services. In this survey 12 (86%) of the health facility managers have no training for quality improvement in adolescent and youth health care and supportive supervision. All youth friendly service started health facilities have 2-3 trained health persons. Among non YFS started health facilities only one had training. During the survey time except one health center with YFS, they were closed due to community mobilization for community based health insurance, while other units are operating their routine activities. In all YFS available health centers service for adolescent and youth were in working hours.
Basic amenities
All started health centers have clearly visible signboard that mentions operating hours of the facility. Among all 13(92.8%) have functional toilet but, only 1/14(7.1%) have functioning hand washing facilities after toilet, 3/14(21.4%) of toilets were clean, 4/14(28.5%) had disposal bin in the toilet. About 11/14(80%) of health facilities do not have adequate and comfortable seating in their waiting area. Almost all health facilities are clean and well coming however; only 2/7(28.5%) health facilities have a clean and well coming separate waiting room and 5/7(75%) were working in a room where windows and doors have no curtains. 3/7(42.8%) have no screen to separate consultation area from the examination to maintain privacy during consultation. There is pipe water in the entire health centers compound but no drinking water facilities in waiting area. Nine out of fourteen (64.2%) has permanent electric supply during working hours. All the facilities have general waste disposal system in the health center. Communication equipment (phone or shortwave radio) found in 5/14 (35.7% %) of the health facilities.
Adequacy of furniture
Seven out of fourteen (50 %) of the health centers have adequate, whereas 5/14 (36%) need repair of their furniture and 2/14 (14 %) of the health facilities do not have furniture while having separate room prepared for YSFs (Figure 1). Computer is available in7/14 (50%) of health facilities and no internet access was observed in all health facilities.
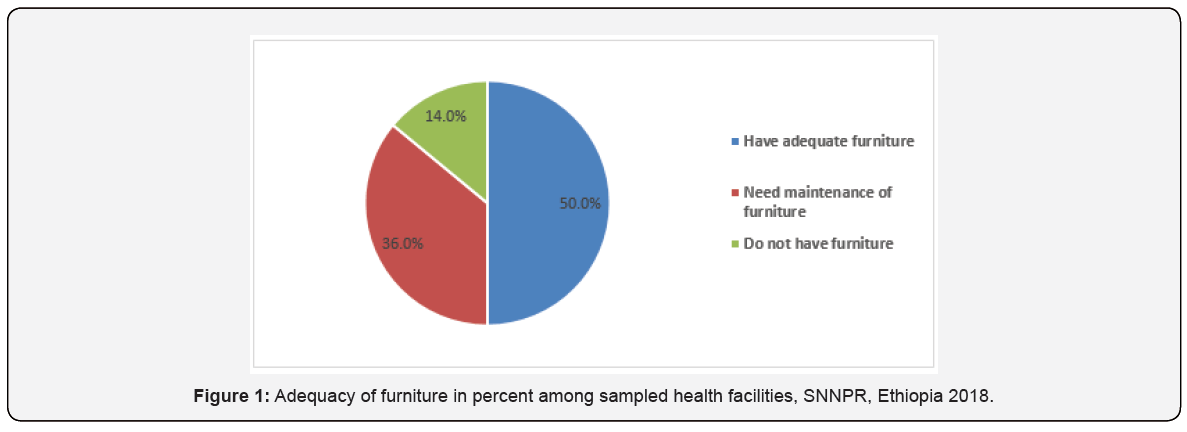
Equipment supply
Equipment/material/supplies are available in all health facilities: Blood pressure measurement machine, binaural adult stethoscope, monaural fetal stethoscope, clinical thermometer, an adult weighing scales, latex gloves, single-use standard disposable or auto-disposable syringes, pregnancy test strips and haemoglobinometer. Materials inadequately supplied /found in surveyed health facilities: Measuring tape, Light source, for example a torch, height meter, soap or alcohol-based hand rubs for hand hygiene body mass index growth charts for adolescents, test strips for urine with 10 parameters, ophthalmoscope set and otoscope set were not found in any of the health centers.
Essential medicine supplies
Condoms, oral contraceptive pills, emergency contraceptive pills, injectable contraceptives, contraceptive implants, intravenous fluids, paracetamol, amoxicillin, Ceftriaxone, ciprofloxacin, cotrimoxazole suspension, diclofenac, omeprazole, diazepam and vaccines found in all health centers uniformly. Only 8/14 (59%) of health centers have magnesium sulfate. Atenolol, Salbutamol, Glibenclamide not available in all health centers, which are important for the treatment of diabetes mellitus, hypertension and asthma respectively.
Infection prevention
All health facilities have sharps/box/container and a general waste disposal incinerator in the compound. Nine out of fourteen (64.3%) have safe storage and disposal of clinical waste and potentially infectious waste that requires special disposal i.e. disposal of equipment that may have in contact with body fluids and safe storage and disposal of sharps. However, 5 (35.7%) have adequate hand hygiene facilities that are located in or adjacent to the office/examination room.
Adolescent participation
In health facilities where services are started 4/7 (57%) health care providers involved the adolescents in the planning, monitoring, evaluation and in any aspects of health service provision for adolescents. But the vulnerable groups of adolescents are not participating.
Overall facilities readiness
All health facilities were fulfilled criterion for the essential medical supply,11 for laboratory services ,9 for infection prevention ,5 for basic equipment’s and 6 for basic amenities (Table 2).

Discussion
Readiness assessment survey was conducted for the implementation of the national adolescent and youth friendly health care strategies in SNNPR. Out of nine standards, four of them were seen in this survey, which are important for the readiness assessment, this includes: facility characteristics, data and quality improvement, adolescents’ participation and intersect oral collaboration. This study showed majorities (86%) of manager lack to get training of adolescent and youth friendly services (AYFS). According to current Ethiopia AYHS, advocate for district managers to guarantee their ownership and support for implementation the designed strategy [17]. The health workers in YFS not started health facilities were deficient in training which is one of the tools for readiness assessment. This finding is in line with study in Uganda in which all staff including the managers lack training. For the implementation of comprehensive AYH all type of health worker received the basic knowledge and skill in preservice training, but at least one person needs to have a training on AYH and can provide orientation for others to overcome the staff shortage and turnover.
Facility characteristics: this is the third standard as this is a readiness assessment study it focusses on the input aspect of the standard: among the elements of the standard availability of essential medicines were acceptable >= 75% in all surveyed facilities. This finding is in line with study conducted in Sudan [19], and higher than Northern Rwanda in which up to 73% of health facilities faced a challenge of medium to high levels of stock outs and slightly higher than study done in South west Ethiopia, which one third of the health facilities are below the standard [20,21]. This variation may be explained that the drugs were used to assess the readiness in this study may varies in types.
To provide quality and standard health care it is important to fulfill the necessary equipment and availability of basic equipment. Only 35.7% fulfilled the standard equipment needed for AYHS. Among the listed infection prevention precautions 64.9% and 78.5% of HFs fulfilled laboratory service required for AYFHS respectively [22]. This also in line with study done in 10 developing countries [23]. One of the significances of health information management system is to make evidence-based decision at all level. We could not find age and sex disaggregated data in all non-started health facilities. This might be due to the national HMIS format not captured age and sex of adolescent and youth. In the revised HIMS format the above problem might be solved. Adolescent participation in planning, monitoring and evaluation of health services and in decisions regarding their own care, as well as in certain appropriate aspects of service provision is considered as very crucial according to the current AYHS [17]. However, in this study only 4/7 health facilities delivering youth friendly service were participated adolescent and youth in planning, monitoring, evaluation and in any aspects of health services provision. This is low according to the standard and study done in Uganda. Possible explanation for this low result may be currently the program was not running very well [22,24].
On the other hand, they were not participated in decision making none of them are member of facility governing board. Possible explanation for this might be the program is not implemented properly as the standard. This may be improved when the program is implemented throughout the health facilities in the region. In assigning health workers less priority was given for AYH rooms. In addition, the working hours were not convenient for adolescents most adolescents prefer out of working hours for YFS.
Conclusion
With available resources it is possible to implement AYHS in central zones of SNNPR. Lack of training for facility managers and health care providers, Essential medicines supply were in satisfactory manner. There were shortages of essential equipment, no intersectoral collaboration and also non-governmental partners working to support this program. Less attention was given for noncommunicable disease for adolescent and youth. Job description for each profession were not including about adolescent and youth health. Therefore, training of trainers at zone level, training of managers, providers at zone and district level is very important. Health facilities should include adolescents in facility governing board. Facility-level registers and health management information systems (HMIS) need to include client information about age, sex, presenting problem, diagnosis and services provided for adolescent and youth. Communication and collaboration with the community, different governmental and non-governmental organizations are very mandatory.
Declarations
Funding
The study not supported by any funding organization.
Availability of data and materials
The datasets generated and/or analyzed during the current study available from the corresponding author on reasonable request.
Authors’ contributions
AG: Supervised the data collection, coded the data, carried out the analysis, and wrote the of the article. NM &YS: Contributed design of the study and analysis, comments throughout the entire process. All authors approved the final version of the manuscript prior to submission
Ethics approval and consent to participate
The study was approved by the Southern Nation Nationalities People Regional health bureau Ethics Committee, and verbal consent was also taken from each respondent for participation.
Disclosure of interests
I declare that we have no competing interests.
Acknowledgements
We greatly acknowledge Southern Nation Nationalities People Regional Health Bureau of Medicine and Health Sciences support letter and financial support for this research. I would like to thank study participants and data collectors as well.
References
- http://www.prb.org/Publications/Datasheets/2017/2017-world-population-data-sheet.aspx.
- Population facts (2015) Youth population trends and sustainable development 2015(1).
- (2014) Population Reference Bureau Ethiopia’s Key: Young People and the Demographic Dividend Fact Sheet.
- Central Statistical Agency [Ethiopia] (2014). Ethiopia Mini-Demographic and Health Survey 2014. Addis Ababa, Ethiopia: Central Statistical Agency.
- http://www.who.int/maternal_child_adolescent/topics/adolescence/development/en/.
- World Health Organization (2015) Core competencies in adolescent health and development for primary care providers: including a tool to assess the adolescent health and development component in pre-service education of health-care providers. WHO, Geneva, Switzerland.
- World Health Organization (2014) Health for the World’s Adolescents A second chance in the second decade. WHO, Geneva, Switzerland.
- (2010) UN Secretary-General. The Global Strategy for Women’s, Children’s and Adolescents’ Health (2016-2030).
- WHO (2017) Introduction to Global Accelerated Action for the Health of Adolescents (AA-HA!): Guidance to Support Country Implementation.
- Global Accelerated Action for the Health of Adolescents (AA-HA!): guidance to support country implementation. Summary. Geneva: World Health Organization; 2017 (WHO/FWC/MCA/17.05). Licence: CC BY-NC-SA 3.0 IGO.
- Pan American Health Organization (2010) Adolescent and Youth Regional Strategy and Plan of Action 2010-2018.
- World Health Oraganization (2016) Global Health Sector Strategy on Sexually Transmitted Infections. Geneva, Switzerland, 2016-2021. 2016.
- (2015) Federal Democratic Republic of Ethiopia (FDRE) National Adolescent and Youth Reproductive Health Strategy2007 - 2015 Addis Ababa, Ethiopia.
- (2000) Federal Negarit Gazetta of the Federal Democratic Republic of Ethiopia.
- Federal Democratic Republic of Ethiopia (FDRE) (2004) The Criminal Code of the Federal Democratic Republic of Ethiopia. Addis Ababa, Ethiopia.
- FDREMOH (2014) Federal Democratic Republic of Ethiopia Ministry of Health Sector Development Plan-IV (HSDP-IV) Addis Ababa, Ethiopia.
- (2016) Federal Democratic Republic of Ethiopia Ministry of Health National Adolescent and Youth Reproductive Health Strategy 2016 - 2020 Addis Ababa, Ethiopia
- WHO (2015) Global standards for quality health-care services for adolescents: a guide to implement a standards-driven approach to improve the quality of health care services for adolescents. Standards and criteria 1:1.
- Edmund Mohammed Nyanwura RKE (2013) Essential medicines availability and affordability: a case study of the top ten registered diseases in builsa district of Ghana. International journal of scientific & technology research 2: 8
- Louis Nditunze, Solomon Makuza, Cheryl LA, Jackline Odhiambo, Elisephan Ntakirutimana, et al. (2015) Assessment of Essential Medicines Stock-Outs at Health Centers in Burera District in Northern Rwanda. Rwanda Journal Series F: Medicine and Health Sciences 2(1): 85-88.
- Abazinab S, Woldie M, Alaro T (2016) Readiness of Health Centers and Primary Hospitals for the Implementation of Proposed Health Insurance Schemes in Southwest Ethiopia. Ethiop J Health Sci 26(5): 449-456.
- (2017) Federal Democratic Republic of Ethiopia Ministry of Health. Adolescent and Youth Health Standards, Implementation Guideline and Minimum Service Delivery Package with Quality and Coverage Measurement Tools.
- Moazzam A, Madeline F, Thandassery RD, Rachel F (2018) Assessment of Family Planning Service Availability and Readiness in 10 African Countries. Global Health: Science and Practice.
- Bukenya JN, Mulogo E, Kibira SPS, Muhumuza C, Atuyambe LM (2017) Health facilities’ readiness to provide friendly reproductive health services to young people aged 10-24 years in Wakiso district, Uganda. Glob J Reprod Med 2(3): 555588.






























