Scrotal Calculi A Rare Ultrasonography Finding
Youness jabbour1,2, Amine slaoui1,2 Tarik Karmouni1,2 Khalid El Khader1,2 Abdellatif Koutani1,2and Ahmed Iben Attya Andaloussi1,2
1Department of Urology B, Ibn Sina teaching hospital, Morocco
1Faculty of medicine and pharmacy, Mohammed V University, Morocco
Submission: June 08, 2018;Published: July 20, 2018
*Corresponding author: Youness Jabbour, Department of Urology, Ibn Sina teaching hospital, Rabat, Morocco Tel: 00212(0)660278360; Email: uro.jabbour@gmail.com
How to cite this article: Youness j, Hamza l. Scrotal Fistula A Suggestive Sign of Genital Tuberculosis. Glob J Reprod Med. 2018; 5(4): 555666. DOI:10.19080/GJORM.2018.05.555666.
Abstract
Tuberculosis is still a major health problem in many developing countries including Morocco. We report the case of a 61 years patient with a history of unbalanced diabetes coming to our department complaining about a scrotal with purulent discharge. He was diagnosed with isolated unilateral tuberculous epididymitis after ultrasonography, positive pus culture for mycobacterium tuberculosis and failure of urine and computed- tomography to find another tuberculosis focus. fistula
Keywords: Tuberculosis; scrotal fistula; Epididymitis; Genitourinary system
Case Report
Diagnosis of urogenital tuberculosis is often late and difficult given the lack of other evocative locations, a notion of contagion or a history of tuberculosis. Generally male genital tuberculosis occurs secondary to urinary involvement through a canalicular or lymphatic pathway with epididymis most frequently affected. Isolated tuberculous epididymitis is rare explained by hematogenous spread of tuberculosis to the epididymis.
Urogenital tuberculosis is the most common form of extra pulmonary tuberculosis following pleural and lymphatic involvement and accounts for 15 to 30% of all extra pulmonary forms of tuberculosis.
Diagnosis of urogenital tuberculosis is often late and difficult given the lack of other evocative locations, a notion of contagion or a history of tuberculosis.
Generally male genital tuberculosis occurs secondary to urinary involvement through a canalicular or lymphatic pathway with epididymis most frequently affected.
Isolated tuberculous epididymitis is rare explained by hematogenous spread of tuberculosis to the epididymis.
Clinically, patients present with hard, non-painful nodule mostly caudal, limited to the tail of the epididymis. It may also present with an association of head and tail nodule giving a bipolar involvement, pathognomonic for epididymal tuberculosis or realise the classic aspect of the epididymis in helmet crest. Rarely patient present with scrotal fistula a clinical sign suggestive of genital tuberculosis.
We report the case of a 61 years-old patient presenting with a chief complaint of non-painful purulent discharge through a scrotal fistula.
He had a history of poorly managed diabetes and is experiencing poor socioeconomic conditions.
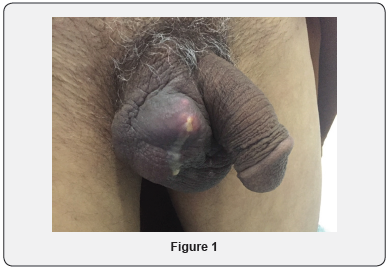
Clinical examination finds an induration of the scrotal skin nearby the fistula with emission of purulent content at its expression. Epididymis seems hard and attached to the scrotal skin. The contralateral testicle seems normal. (Figure 1).
Scrotal ultrasonography attested the normality of the contralateral testicle and showed hypoechoic and heterogeneous content of the right epididymal head.
Bacteriological study of the product of the fistula revealed mycobacterium tuberculosis.
Sputum and urine tests for tuberculosis and thoraco-abdominopelvic CT showed no other locations of tuberculosis.
The patient was put under anti-tuberculous treatment with good evolution.
Confirmation of isolated tuberculous epididymitis is challenging. Renal focus of tuberculosis may be microscopic and, therefore, undetectable to imaging procedures. Negative urine cultures are not sufficient to exclude associated urinary involvement due to its low sensitivity.
Conclusion
Isolated tuberculous epididymitis must be considered by health professionals in at-risk populations as patient coming from or living in endemic area, those with less effective immune systems and those with initial treatment failure to prevent any further the functioning of the genitourinary system.






























