Modified Chondrocutaneous Helical Rim AdvancementFlap: Reconstruction of Marginal Pinna Defects
Salil Sood*, Eugene Omakobia, Graham Banfield and Patrick Donnelly
FRCS (ORL-HNS), Alder Hey Children's Hospital, Liverpool, UK
Submission: March 26, 2018; Published: April 26, 2018
*Corresponding author: Salil Sood, FRCS (ORL-HNS), Alder Hey Children's Hospital, Liverpool, UK, Email: salilsood@hotmail.co.uk
How to cite this article: Salil S, Eugene O, Graham B, Patrick D. Modified Chondrocutaneous Helical Rim Advancement Flap: Reconstruction of Marginal Pinna Defects. Glob J Oto, 2018; 15(3): 555911. DOI: 10.19080/GJO.2018.15.555911
Abstract
Due to its unique structure, repair of marginal pinna defects requires special considerations. Various repair techniques have been documented in the literature for decades but many of these techniques result in deformity of the pinna and some can be unnecessarily complicated. Here we report a novel technique for repairing such defects, which is actually a modification of an older method. We have shown that a natural auricle shape is achieved with minimal disruption of the anatomical landmarks.
Introduction
Anatomy and Embroyology of Pinna
The Pinna (Latin for feather) is the visible external part of the ear. It is first noticeable around the sixth week of gestation, developing from six rounded protuberances known as the hillocks of Hiss. These develop into the folds of the pinna and gradually shift upwards and backwards to their final position on the head. The first three hillocks are derived from the 1st branchial arch and form the tragus, crus of the helix, and helix, respectively. The final three hillocks are derived from the 2nd branchial arch and form the antihelix, antitragus, and lobule, respectively (Figure 1).
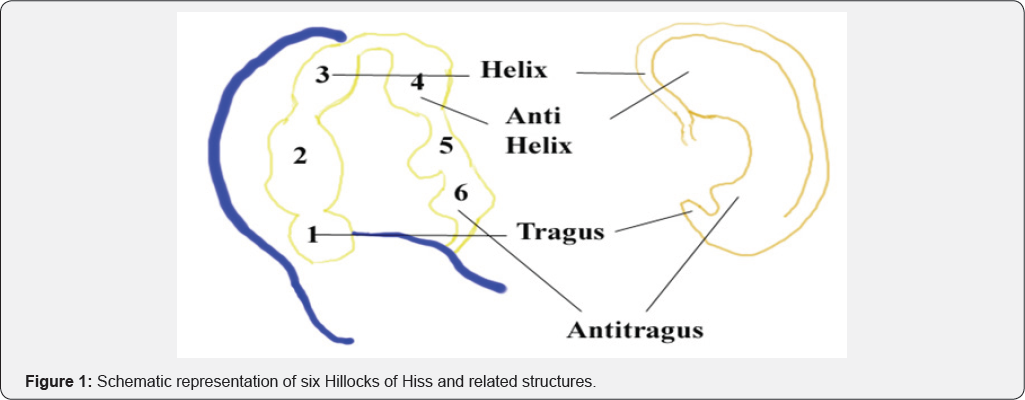
Background & Study
Defects of the helical rim may occur as a result of trauma, burns or cancers. The helical rim of the ear is involved in 45-55% of cancers of the ear [1]. The helical rim is a common site for basal cell and squamous cell carcinoma as this is a sun-exposed area. It is also an area which can be susceptible to trauma resulting in marginal loss. Reconstruction of auricular defects with 'like for like' (ideally pinna) tissue offers the best aesthetic option. There is, however, a paucity of redundant local ear tissue, owing to well-defined landmarks of the semi rigid cartilage and tight adherence of the overlying skin. A total of one hundred patients underwent repair of a pinna defect between 2004 and 2008 at our institution. The inclusion and exclusion criteria are listed below
a) Inclusion criteria:
i. All helical rim procedures undertaken by a single named surgeon.
ii. Primary lesions of the helix, antihelix and scapha.
b) Exclusion criteria:
i. Post radiotherapy lesions
ii. Revision surgery
iii. Conchal lesions
iv. Patients with concomitant otitis externa
Technique
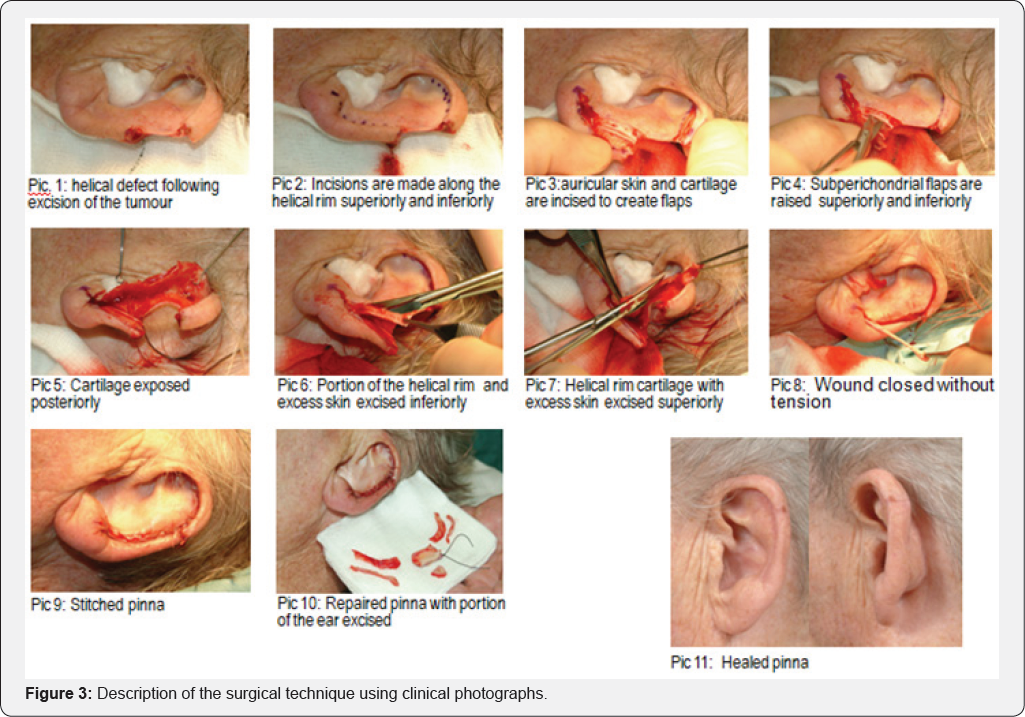
The surgical technique is described below and also displayed schematically in Figure 2 and using clinical photographs (pictures 1-11) in (Figure 3).
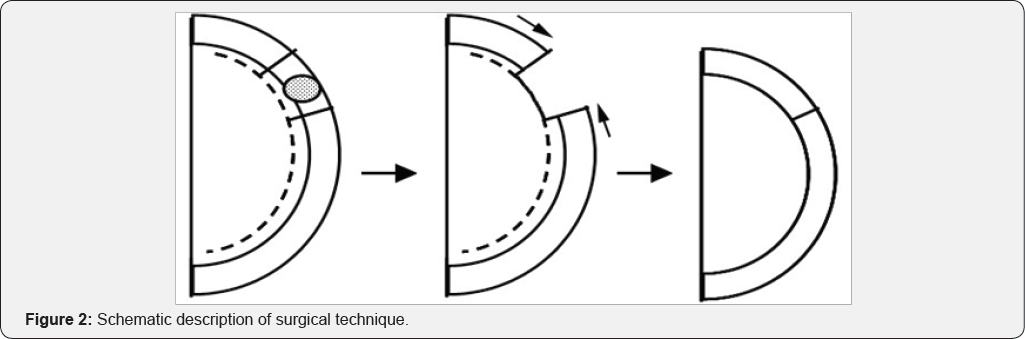
a) The skin lesion is marked and the excision margin measured and delineated.
b) The lesion is then excised as rectangular section of helical rim (Picture 1).
c) The skin and cartilage are incised along the lateral surface of the ear superiorly towards the scaphoid fossa and inferiorly to the lobule (Picture 3).
d) The post-auricular skin is elevated off the conchal cartilage both above and below the excised lesion and the skin raised off the anterior aspect of the cartilage for 2-3mm (Picture 4-5).
e) The cartilage rim is then trimmed so that the skin edges can meet without undue tension and accurate apposition of skin and cartilage (Picture 6-8).
f) Stitched pinna with tissue excised to include lesion and additional tissue excised to attain closure of the defect (Picture 9 & 10).
g) Well healed pinna at 3 months (Picture 11).
Discussion
The original technique described by Antia and Buch in 1967 used chondrocutanous advancement flaps with wide posteromedial auricular skin pedicle and V-Y helical root advancement [2]. The senior author in the current study has modified this technique by using residual auricle tissue to repair the helical rim defect. The edges are brought together by reduction of the size of the scapha and part of the conchal cartilage, which mobilises the superior and inferior helical flaps to achieve good apposition. This allows repair of defects arising after the excision of lesions extending to the antihelix and scapha. This creates a normal looking ear, though smaller from superior to inferior. Other surgical techniques include the frequently described wedge excision [3], which allows single stage repair of defects. However this results in a pointed auricular shape and protrusion of the upper pole. Wedge resection with approximation of the edges by removing two burrows triangle over the concha has also been described in the past [4]. Additionally, composite auricular grafts [5], post auricular flaps [6] and tissue expanders with cartilage grafts [7] have been discussed in the literature. Many of these techniques are complicated procedures and may require general anaesthesia. Reduction of the opposite ear has also been documented to correct the asymmetrical size of the ears [8].
Conclusion
We achieved a natural auricle shape with minimal disruption of the anatomical landmarks. No mobilisation of the helical root as described by the original authors [2] was performed which improved the cosmetic results. Thus a major limitation of the original technique, in that it was best for repairing only peripheral helical defects, has been improved by our technique. Furthermore, our modified technique avoided unnecessary dissection on the post auricular area to create a wide based post auricular advancement flap as described by the original authors.
References
- Leferink VJ, Nicolai JP (1988) Malignant tumours of the external ear. Ann Plast Surg 21(6): 550-554.
- Antia NH, Buch VI (1967) Chondrocutanous advancement flap for the marginal defect of the ear. Plast Reconstr Surg 39(5): 472-477.
- Adam Bialostocki, Swee T Tan (1999) Modified Antia-Buch repair for full thickness upper pole auricular defects Plast Reconstr Surg 103(5): 1476-1497.
- Joseph J Fata (1997) Composite chondrocutaneous advancement flap. Plast Reconstr Surg 99(4): 1172-1175.
- Menick FJ (1990) Reconstruction of the ear after tumour excision. ClinPlastSurg 17(2): 405-415.
- Cronin TD (1952) One stage reconstruction of the helix. Plastic and Reconstructive Surgery 9(6): 547-546.
- Sasaki GH (1990) Tissue expansion in reconstruction of acquired auricular defects. Clin Plast Surg, 17(2): 327-338.
- Gault DT, Grippaudo FR and Tyer M (1995) Ear reduction. Br J Plast Surg 48(1): 30-34.





























