An Unusual Case of Fish Bone Migration-A Case Report
Aynesha L1*, Lina L2, Pathma L2 and Philip R2
1ORL Department of University Malaya, Kuala Lumpur, Malaysia
2ORL Department of Hospital Raja Permaisuri Bainun, Ipoh, Perak, Malaysia
Submission: March 27, 2018; Published: April 03, 2018
*Corresponding author: Aynesha Letchmikanthan, 67, Jalan 5/69, Taman Gasing Indah, Petaling Jaya, 46000, Selangor, Malaysia, Aynesha@hotmail. com,+60 163317538, Email: Aynesha@hotmail.com
How to cite this article: Aynesha L, Lina L, Pathma L, Philip R. An Unusual Case of Fish Bone Migration-A Case Report. Glob J Oto 2018; 14(2): 555885. DOI: 10.19080/GJO.2018.14.555885
Abstract
Objective: To emphasize the importance of early identification and management of fish bone ingestion in order to prevent the migration phenomenon of an ingested foreign body.
Methods: This is a case report of a patient who had a migratory fish bone.
Results: A 4-centimeter fish bone was extracted from the right side of the patient's neck via an external incision.
Conclusion: Migration of ingested foreign bodies is a known phenomenon and one that causes substantial complications. With early and timely interventions, such complications can be avoided, as was in this particular patient.
Keywords: Fish bone; Migratory foreign body; Tongue; Neck
Abbreviations: FB: Foreign body; NG: Nasogastric Tube
Introduction
Fish bone ingestion is one of the commonest reasons for a foreign body (FB) in the Asian adult population as compared to meat in the Western or coins in the paediatric population [1]. As such, while it is well documented that such foreign bodies do migrate, in doing so, they may pass through the gastrointestinal tract uneventfully, or may end up causing bleeding, viscous perforation or even abscess collection [2,3].
Case Presentation
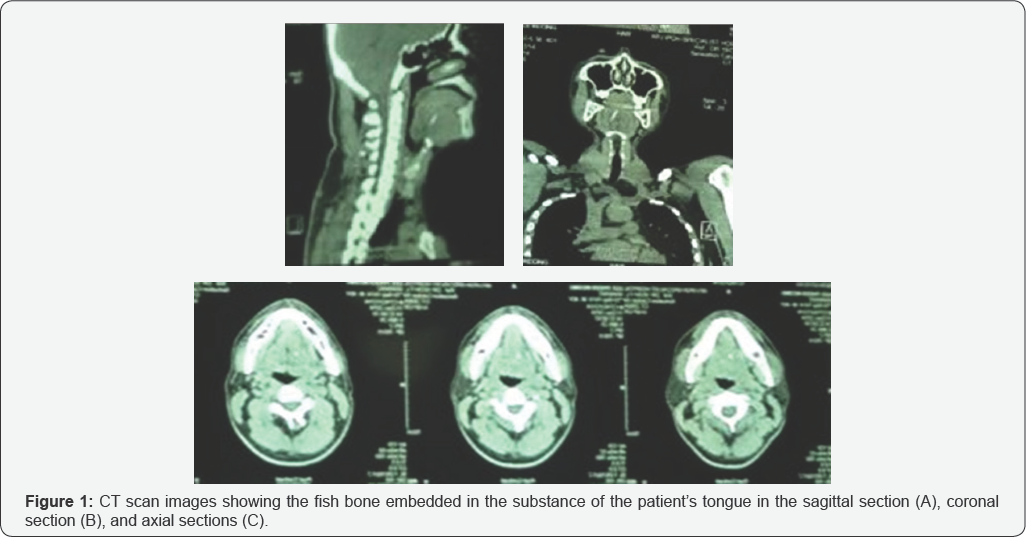
A 40-year-old man, with no co-morbidities, initially presented to a private ORL specialist complaining of dysphagia and odynophagia for 2 days duration. The patient gave a history of having eaten some fish the day before and had since been having pricking pain in his tongue. On further enquiry, he was unable to specify the type of fish he had ingested, but knew that the bone was a long one. Additionally, he denied any difficulty in moving his tongue or speaking Figure 1. On examination, there was no obvious foreign body in the oral cavity. A CT scan was done, which confirmed the diagnosis, as the fish bone was seen penetrating the entire thickness of the tongue. He was subsequently referred to our centre for removal.
Results and Discussion
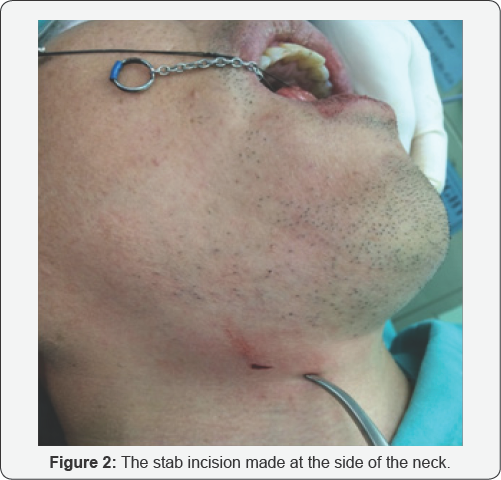
The patient underwent a direct laryngoscopy the same day, however intraoperatively, no foreign body was visualized nor was there any slough or indication of penetration of the tongue. Surprisingly, on palpation of the base of tongue, a sharp protrusion was seen coming from the right side of the neck and on making a small incision, a 4cm fish bone was extracted (Figures 2 & 3). Post operatively, the patient was kept nil by mouth for 2 days, during which he was fed via a nasogastric (NG) tube and covered with intravenous antibiotics, Cefuroxime and Metronidazole. He was also prescribed Benzydamine gargle and Paracetamol as analgesia. In the ward, he recovered well and was discharged with oral antibiotics after 2 days with a clinic appointment 1 week later. On review in the clinic, the incision site had healed well and the patient reported no pain, fever, difficulty in talking or eating since the surgery. He has since been discharged from our care.

Ingested FBs are a common cause of concern for patients and is a situation faced by most, if not all, emergency and ORL practitioners. As such, an estimated 69% of foreign bodies can be found within the oral cavity [4]. The most common sites to be involved for FB lodging include the tonsils, valleculae, tongue base and pyriform fossae, of which the tonsils are the most frequent [5]. While 90% of ingested fish bones tend to pass through the aero digestive tract uneventfully, about 20% of cases would require minimally invasive intervention [6]. About 1% of ingested fish bones go on to cause bleeding, viscous perforation, intestinal obstruction and abscesses [7].
While accidental ingestion of FB is frequent in paediatric patients, there are several predisposing factors that increase the possibility of ingestion in adults. Factors such as advanced age, dentures, psychiatric illnesses, mental retardation, alcoholism, eating rapidly and talking while eating tend to increase the likelihood of an ingested FB [7,8].
This case was interesting in the fact that, despite glaring CT scan evidence of a FB, intraoperatively, no entry wound could be identified on the tongue and it was not palpable. Nevertheless, we managed to remove the foreign body when it emerged from the right side of the neck. This particular instance illustrates that while CT scans can demonstrate the area of involvement in patients with a history of foreign body ingestion, it is also important to understand that migration can take place and as such, a more cautious interpretation of the imaging studies is needed. A high index of suspicion and clinical acumen are required for early and timely intervention so as to avoid potentially devastating complications [9-11].
Acknowledgement
I would like to take this opportunity to thank my colleagues Dr. Siri Kavitha Nalatamby and Dr. Dinesh Raj for assisting me in obtaining the CT scan films for me to use in this article.
References
- Guitron A, Adalid R, Huerta F, Macias M, Sanchez-Navarrete M, et al. (1996) Extraction of foreign bodies in the esophagus. Experience in 215 cases. Rev Gastroenterol Mex 61(1): 19-26.
- Sierra-Solis A (2013) Bowel perforations due to fish bones: rare and curious. Semergen 39(2): 117-118.
- Joglekar S, Rajput I, Kamat S, Downey S (2009) Sigmoid perforation caused by an ingested chicken bone presenting as right iliac fossa pain mimicking appendicitis: a case report. J Med Case Rep 3: 7385.
- Kim JP, Kwon OJ, Shim HS, Kim RB, Kim JH et al. (2015) Analysis of clinical feature and management of fish bone ingestion of upper gastrointestinal tract. Clin Exp Otorhinolaryngol. 8(3): 261-267.
- Kim HU (2016) Oroesophageal fish bone foreign body. Clin Endosc 49 (4): 318-326.
- Henderson CT, Engel J, Schlesinger P (1987) Foreign body ingestion: review and suggested guidelines for management. Endoscopy, 19(2): 68-71.
- Venkatesh SH, Karaddi NKV (2016) CT findings of accidental fish bone ingestion and its complications. Diagn Interv Radiol 22(2): 156-160.
- Wu C-X, Wu B-Q, Duan Y-F, Sun D-L, Jiang Y (2014) Rare case of omentum-wrapped abscess caused by a fish bone penetrating the terminal ileum. World J of Gastroenterol, 20(32): 11456-11459.
- Kim HU, Song HJ (2012) Clinical characteristics of an esophageal fish bone foreign body from Chromis notata. J Korean Med Sci 27(10): 1208-1214.
- Tan S, Tan S, Peng M, Yu F (2015) Management of an ingested fish bone in the lung using video-assist thoracic surgery: a case report. Medicine (Baltimore), 94(22): e943.
- Masoodi I, Alsayari K, Al Mohaimeed K, et al. (2012) Fish bone migration: an unusual cause of liver abscess. BMJ Case Reports.





























