CT scan versus Surgery: How Necessary is the Mastoidectomy in Patients with Chronic Otitis Media?
Ergun Sevil1*, Sami Bercin2, Togay Muderris3, Fatih Gul4, Huseyin Cetin5 and Muzaffer Kiris6
1Department of Otorhinolaryngology, Head and Neck Surgery, Karaman State Hospital, Turkey
2Faculty of Medicine Department of Otorhinolaryngology, Head and Neck Surgery, Yildirim Beyazit University, Turkey
3Department of Otorhinolaryngology, Head and Neck Surgery, Bozyaka Training and Research Hospital, Turkey
4Department of Otorhinolaryngology, Head and Neck Surgery, Tatvan State Hospital, Turkey
5Faculty of Medicine Department of Radiology, Yildirim Beyazit University, Turkey
6Department of Otorhinolaryngology, Head and Neck Surgery, Gulhane Training and Research Hospital, Turkey
Submission: March 17, 2018; Published: April 03, 2018
*Corresponding author: Ergun Sevil, Karaman State Hospital, Department of Otorhinolaryngology Head and Neck Surgery, 70000, Karaman, Turkey, Tel:905363104655; Fax:903382263309; Email:drergunsevil@yahoo.com
How to cite this article: Ergun S, Sami B, Togay M, Fatih G, Huseyin C, et al. CT scan versus Surgery: How Necessary is the Mastoidectomy in Patients with Chronic Otitis Media?. Glob J Oto 2018; 14(1): 555880. DOI: 10.19080/GJO.2018.14.555880
Abstract
Objective: To compare the computed tomography (CT) results with the surgical findings of patients experiencing mastoidectomy for chronic otitis media (COM), and to determine whether or not mastoidectomy is necessary.
Materials and methods: A retrospective analysis was made of a series of 130 patients with COM between May 2011- April 2014. Each patient underwent a surgical procedure for treatment of COM. The results of CT scanning and the intraoperative findings were compared. The evaluation of the mastoid CT scan was based on the preoperative reports. The parameters of comparison were the presence of cholesteatoma, fluid, cholesterol granuloma, granulation tissue or mucosal thickening. The operation notes were recorded and data were collected to obtain the mastoid findings.
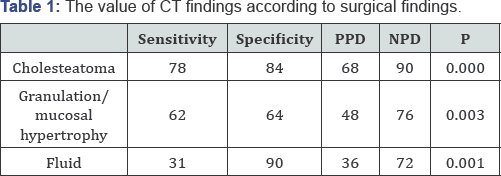
Results: Cholesteatoma was present in 38 of 130 patients (29.2%). In 44/130 (33.8%) cases, the CT scan showed cholesteatoma and surgical findings revealed cholesteatoma in 30/44 (68.1%) of these cases. According to the data, the sensitivity of the scan in determining cholesteatoma was 78%, specificity was 84%, positive predictive value was 68%, and negative predictive value was 90% (p: 0.000). Diagnostic value was evaluated by the area under the receiver-operating characteristics (ROC) curve analyses which were 0.81 for cholesteatoma, 0.63 for mucosal hypertrophy/granulation tissue and 0.61 for fluid.
Conclusion: The evaluation of preoperative computed tomography is adequately helpful particularly in cases of cholesteatoma. Based on these findings, mastoidectomy is performed only if necessary.
Keywords: Chronic Otitis Media; Cholesteatoma; Mastoidectomy; Computed tomography
Abbreviations: COM: Chronic Otitis Media; SPSS: Statistical Package for the Social Sciences; ROC: Receiver-Operating Characteristics; AUC: Area Under the Curve
Introduction
Otolaryngologists routinely refer to computerized tomography (CT) of the temporal bones before mastoidectomy for chronic suppurative middle ear disease [1]. CT scanning has made significant contributions to the ability to diagnose and evaluate temporal bone diseases. Especially, it could be used to prove the place and comprehension of the disease and also asymptomatic complications, secondary to bony destruction [2]. In preoperative temporal bone CT, soft tissue lesion associated with bony erosion is considered as cholesteatoma [3,4]. The definition of cholesteatoma is important before surgery because it allows us to estimate the method of operation and the extend of disease. There are doubts that CT cannot confidently differentiate fluid from mucosal disease and soft tissue and that it lacks a guaranteed sensitivity for erosive complications such as cholesteatoma. However, the extent of soft tissue involvement of the mastoid antrum, especially the epitympanum, may help the surgeon in deciding between mastoidectomy or not and in order to avoid complications. The aim of this study was to compare preoperative mastoid CT findings with operative findings for chronic otitis media (COM).
Materials and Methods
A retrospective study was carried out with 130 patients who underwent mastoidectomy between May 2011-April 2014 for chronic otitis media and were determined by CT scan preoperatively. Informed consent was obtained from all the patients. Approval for the study was granted by the local ethic committee (Ethics Committee Decision no: 2015/498). The study group included 62 male and 68 female patients ranging in age from 14 years to 65 years. The patients with a diagnosis of COM were selected for surgical procedure. The patients included in this retrospective study suffered from chronic tympanic membrane perforation, conductive or mixed type hearing loss and intermittent or refractory otorrhoea. CT scan was obtained when the examination of the ear was dry. However, patients with refractory otorrhoea were performed CT scan after oral and topical therapy.
The results of CT scanning and the intraoperative findings were compared. The evaluation of the mastoid CT scan was based on the preoperative reports. The parameters of comparison were the presence of cholesteatoma, fluid, cholesterol granuloma, granulation tissue or mucosal thickening. Both coronal and axial images were performed. Using Siemens Sensatron 40 equipment (Somatom X; Siemens, Erlangen, Germany), CT scans were performed using 1.5mm contiguous sections through the temporal bone CT was reviewed by only one experienced radiologist in the preoperative evaluation of COM. A comparison was then drawn between the radiological and intraoperative appearance of each patient's mastoid.
Statistical Analysis
Statistical analyses were performed using statistical package for the social sciences (SPSS) software version 22 for Macintosh. Descriptive analyses were presented using mean and standard deviation for the normally distributed variables. The Kolmogorov-Smirnov test was used to evaluate the distribution of variables, the Student's t test was used for continuous variables for those with normal distribution and the Chi-square test was used for categorical variables. The receiver-operating characteristics (ROC) curve was used to show the sensitivity, specificity and area under the curve (AUC) of the parameters. The statistical significance was set at p<0.05.
Results
Generalradiologicalmastoidfindingwashypopneumatization, which was present in all of the patients. The next most common mastoid abnormalities were involvement of the air cells by soft tissue. The values of the CT findings compared to the surgical findings are shown in Table 1. Intraoperatively, cholesteatoma was found in 38 out of 130 patients (29.2%). In 44/130 (33.8%) subjects, the CT scan revealed cholesteatoma. Surgical results demonstrated cholesteatoma in 30/44 (68.1%) of these cases. In 8 patients (21%) it was excluded by CT scan but was present at surgery. From the above data, the sensitivity of the scan in detecting cholesteatoma was determined as 78%, specificity as 84%, positive predictive value as 68%, and negative predictive value as 90% (p: 0.000) (Tables 1 & 2; Figure 1). Granulation tissue was noticed in 45/130 (%34.6) cases intraoperatively.
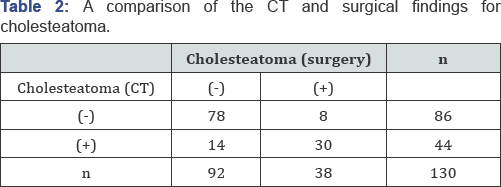
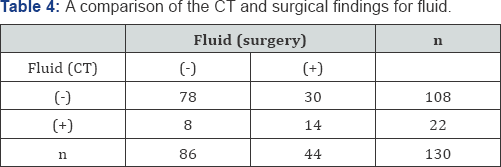
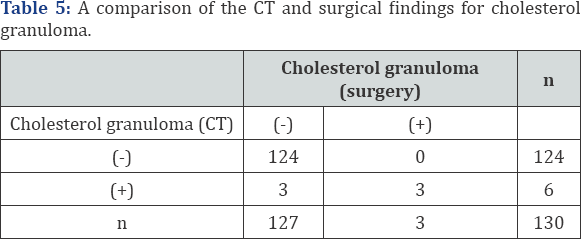
In 58/130 (44.6%) cases, the CT scan showed granulation tissue. In 28 patients (21.5%), granulation tissue was predicted correctly by the CT scan. In 17 patients, it was excluded by CT scan but was present at surgery. According to the above data, the sensitivity of the scan in determining granulation tissue was detected as 62%, specificity as 64%, positive predictive value as 48%, and negative predictive value as 76% (p: 0.003) (Table 1 & 3; Figure 1). In 64/130 (49.2%) cases, bone erosion was not seen despite abnormal soft tissue density on CT. In 8 (12.5%) of these 64 cases, cholesteatoma was controlled during operation. The rest of the patients were associated to granulation tissue, cholesterol granuloma and fluid (Table 4 & 5; Figure 1). Cholesteatoma was detected in 30/44 (68.1%) cases where CT showed soft tissue density and ossicular chain erosion being together. Despite the diagnosis of cholesteatoma in 6 cases intraoperatively, preoperative CT results were reported as granulation tissue.

In 44 /130 (33.8%) cases, surgical exploration did not show any proof regarding with soft tissue collection. None of these mastoid bones had cholesteatoma, cholesterol granuloma, mucosal thickening and granulation tissue. Therefore, it was thought to be related to fluid. It is difficult to show this situation clearly, which hinders the differentiation of fluid from the water which is used while drilling the mastoid.
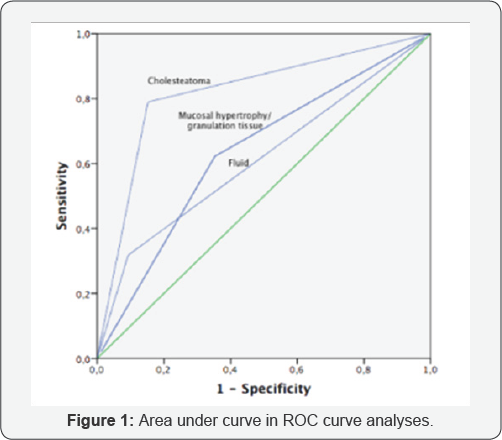
Diagnostic value was evaluated by the AUC ROC curve analyses, and the values obtained were 0.81 for cholesteatoma, 0.63 for mucosal hypertrophy/granulation tissue and 0.61 for fluid (Figure 1). The ROC curve analyses indicated that the cholesteatoma could not be significantly differentiated from non-cholesteatoma patients. However, cholesteatoma had higher sensitivity and specificity values when compared to other mastoid diseases in CT
Discussion
The role of CT in the preoperative evaluation of COM patients is not clear, although the accepted imaging modality in imaging temporal bone pathologies is CT [5]. However, using CT of the temporal bone before mastoid surgery is becoming routine practice for most otolaryngologists, provides data about the surgical anatomy and extension of the pathology, and is also important for medicolegal reasons as it gives preoperative documentation of the disease. As has been previously reported, the diagnostic value of CT making different cholesteatoma, granulation tissue, and fluid has been debated in the preoperative evaluation of COM patients [4,6,7]. It is difficult to claim that a soft tissue appearance without destruction on CT is a cholesteatoma in the mastoid. Tatlipinar et al. argued that CT scans of chronically draining ears demonstrated abnormal soft tissue densities in the middle ear or mastoid in 80% (40/50) of cases, and surgical findings revealed that 57.5% (23/40) of those were cholesteatoma [8].
In the current study, CT scan demonstrated abnormal soft tissue in 83% (108/130) of cases, and surgical findings showed that 35.1% (38/108) were cholesteatoma. Furthermore, although CT scan reported soft tissue density in the attic region in certain cases, surgical exploration revealed only mucosal edema intraoperatively. Obstruction was not observed because of soft tissue during mastoidectomy. It was thought that the view on CT might be by the reason of inflammation caused by chronic otorrhea. Using ROC curve analyses, the accuracy of the cholesteatoma (AUC=0.81, Figure 1) in tomography was comparable to recent publications, thus demonstrating that cholesteatoma has higher sensitivity and specificity values when compared to other mastoid diseases in CT. Baylan et al. demonstrated that cholesteatoma was present in 19 of 56 patients (33.9%).
In 18 patients (94.7%), the cholesteatoma was predicted correctly by the CT scan, and in 34 patients (91.9%), it was put out of accurately. The sensitivity of the scan in detecting cholesteatoma was 91.9%, specificity was 94.7%, positive predictive value was 97.1%, and negative predictive value was 85.7% [9]. Chatterjee et al. showed that the important role of high resolution CT lies on the early detection of cholesteatoma, and more conservative surgical procedures can be used to eradicate the disease [10]. Thukral et al. claimed that the surgical and radiological findings showed a high level of sensitivity (89.29%) in the identification of cholesteatoma [11]. The results of the cholesteatoma in the current study were comparable to the findings of these reports that used CT and obtained good prediction with high sensitivity and specificity.
In the current study, cholesteatoma could be properly viewed by computed tomography. If there are bone erosion and smooth expansion with soft tissue mass, which are the hallmarks of cholesteatoma, mastoidectomy should be applied. On the other hand, if the soft tissue mass is not associated with bone erosion, it is difficult to determine cholesteatoma on CT as it could be associated with mucosal thickening, granulation tissue and fluid. Belal et al. reported on functional middle ear and mastoid surgery, stating that the surgeon needs to clear the middle ear first because cholesteatoma almost always starts in the middle ear [12]. When the scan is reported with mastoid diseases except cholesteatoma, the middle ear approach can be recommended first to remove the pathology, and the decision of mastoidectomy should be taken at the time of surgery because conclusive diagnosis of cholesteatoma is comprehensible at the time of middle ear exploration. Thus, the surgeon can avoid unnecessary intervention to preserve mastoid mucous membrane and surface area.
If there is no suspicion of cholesteatoma, no discharge from the ear on examination and there is little air-bone gap on the audiogram, the mastoid hypopneumatization reported on the temporal CT should suggest mucosal thickening, granulation tissue or fluid associated with the previous infection. In this situation, mastoidectomy should not be routinely applied because it does not contribute to the treatment. However, if there are suspicions of cholesteatoma, the surgical approach should go through the middle ear first, because cholesteatoma usually starts from the middle ear and extends to the mastoid [12]. In conclusion, in spite of the benefits, there are some disadvantages of CT including the insufficiency of scanning to distinguish cholesteatomas from granulations, mucosal edema and fluid. This information may help the autologous in the choice of surgery to be performed as tympanoplasty with or without mastoidectomy.
References
- Arellano B, Gonzalez FM, Pinilla MT, Ramirez-Camacho RA, Vergara J (1996) Effectiveness of imaging diagnosis in chronic otitis media. Acta Otolaryngologica Espanola 47 (6): 435-437.
- Yates PD, Flood LM, Banerjee A, Clifford K (2002) CT scanning middle ear cholesteatoma: what does the surgeon want to know? BR J Radiol 75(898): 847-852.
- Tierney PA, Pracy P, Blaney SP, Bowdler DA (1999) An assessment of the value of the preoperative computed tomography scans prior to otoendoscopic 'second look' in intact canal wall mastoid surgery. Clin Otolarngol Allied Sci 24(4): 274-276.
- Phelps PD, Wright A (1990) Imaging cholesteatoma. Clin Radiol 41(3): 156-162.
- Walshe P, McConn Walsh R, Brennan P, Walsh M (2002) The role of computerized tomography in the preoperative assessment of chronic suppurative otitis media. Clin Otolaryngol Allied Sci 27(2): 95-97.
- OReilly BJ, Chevretton EB, Wylie I (1991) The value of CT scanning in chronic suppurative otitis media. J Laryngol Otol 105(12): 990-994.
- Jackler RK, Dillon WP, Schindler RA (1984) Computed tomography in suppurative ear disease: a correlation of surgical and radiographic findings. Laryngoscope 94(6): 746-752.
- Tatlipinar A, Tuncel A, Ogredik AE, Gokceer T, Uslu C (2012) The role of computed tomography scanning in chronic otitis media. Eur Arch Otorhinolaryngol 269(1): 33-38.
- Baylan MY, Ozmen CA, Gun R, Yorgancilar E, Akkus Z, et al. (2012) An evaluation of preoperative computed tomography on patients with chronic otitis media. Indian J Otolaryngol Head Neck Surg 64(1): 6770.
- Chatterjee P, Khanna S, Talukdar R (2015) Role of High Resolution Computed Tomography of Mastoids in Planning Surgery for Chronic Suppurative Otitis Media. Indian J Otolaryngol Head and Neck Surg 67(3): 275-280.
- Thukral CL, Singh A, Singh S, Sood AS, Singh K (2015) Role of High Resolution Computed Tomography in Evaluation of Pathologies of Temporal Bone. J Clin Diagn Res 9(9): 07-10.
- Belal A, Reda M, Mehana A, Belal Y (2013) Functional middle ear and mastoid surgery (FMMS). Int Adv Otol 9(1): 21-29.





























