Melatonin as Potent Therapeutic Drug in Vesicular Delivery Application in Combating Diseases
Ardhendu Kumar Mandal*
Central Instrumentation Division, CSIR-Indian Institute of Chemical Biology, India
Submission:August 12, 2021; Published:September 07, 2021
*Corresponding author: Ardhendu Kumar Mandal, Central Instrumentation Division, CSIR-Indian Institute of Chemical Biology 4, Raja S.C. Mullick Road, Jadavpur, Kolkata – 700032, India
How to cite this article: Ardhendu Kumar Mandal. Melatonin as Potent Therapeutic Drug in Vesicular Delivery Application in Combating Diseases.Glob J Nano. 2021; 5(4): 555669. DOI: 10.19080/GJN.2021.05.555669
Abstract
Diminishing amounts in endogenous melatonin synthesis in the body with increased aging enhance/ induce susceptibility to oxidative damages, infectious diseases, cancer, neurodegenerative diseases, inflammation, obesity, immune-deficiencies, and cardiovascular diseases in the biological systems. Exogenous administration of melatonin hormone in the body may inhibit the diseased state as it acts as antioxidant, anti-inflammatory, neuro-protective, immune-regulatory, and anti-carcinogenic molecule. As conventional drug therapy has limitations in therapeutic biological efficacies, melatonin may be utilized in vesicular delivery system to get maximum targeted therapeutic efficiencies against diseased cells. This review illustrates mainly the inhibitory therapeutic effects of melatonin with or without its vesicular forms against various diseases as potent molecule regarding remedy.
Keywords: Diseases; Melatonin; Vesicular melatonin; Biological efficiencies; Inhibitory therapeutic effects
Introduction
Diseases may be inducted primarily due to oxidative attack into the body cells for the exposures of toxic and infective agents following development of progressive diseased states when they dominates over defense systems such as antioxidant and immune defense mechanisms [1]. Owing to aging factor, many people suffer from deficiency in endogenous synthesis of antioxidants for scavenging reactive oxygen and nitrogen species (ROS and RNS) to neutralize toxic substances and to protect body-immunity against invading virulent micro-organisms for inhibiting disease progress [2]. ROS such as superoxide anion radical (O2.-) derived in mitochondria, cytosol and endoplasmic reticulum, hydrogen peroxide (H2O2) generated in peroxysomes to form highly reactive singlet oxygen (1O2) and hydroxyl radical (. OH) may be involved in cellular transformation, regulation, and degradation [3]. RNS e.g., nitric oxide (.NO) derived by the NO-synthases may react with O2.- for forming peroxynitrite (ONOO-) to damage cell [4]. An oxidative and nitrative stress status may result in cellular damage leading to a loss of cellular functions and integrities involving pathological conditions such as cardiovascular diseases, neurological disorders, cancer, infectious diseases, and aging process [5,6]. ROS produced from metabolic process may play a pivotal role in aging, while mitochondria may be intricated in these process-oriented related diseases [7]. Oxidative stress may regulate neural microglia and astrocytes for excitotoxicity and apoptosis in neuronal death [8]. Mitochondrial dysfunctions such as cell-energy impairments, ROS-overproduction, and apoptosis may involve the pathogenic mechanisms in aging and neurodegenerative diseases such as amyotrophic lateral sclerosis, Parkinson, and Alzheimer diseases [9].
On the other hand, the .NO productions from neuronal NO synthase (nNOS), inducible NO synthase (iNOS) by triggered macrophages / microglia, and endothelial NO synthase (eNOS) involved in further formation of reactive peroxynitrite may produce nitrosative stress to damage cells [10]. To overcome the oxidative stress, exogenous potent antioxidant molecules should be administered to scavenge free radicals. However, simple conventional therapy is not the proper approach to attenuate cell damage as it becomes diluted into the systemic circulation with its insolubility and poor bioavailability barriers after entry into the body. Therefore, it is necessary to develop a device which could deliver drug to the targeted site/s with reduced drug toxicity against oxidative attack. The vesicular systems, such as liposome and nanocapsule, the drug delivery vehicles by virtue of their nontoxic, non-immunogenic, biodegradable, biocompatible and sustained drug releasing ability in the living system, have attracted attention as effective therapeutic device in combating oxidative damage [11]. Melatonin (N-acetyl-5- methoxytryptamine) is a steroid hormone secreted mainly by the pineal gland of mammals involved in the regulation of sleep and circadian rhythm and in the neuroimmuno modulation [12]. Melatonin is also synthesized in many mammalian tissues and organs such as respiratory, gastrointestinal, immune, and genitourinary systems, and skin [13]. Melatonin is derived by the conversions from the amino acid tryptophan into 5- hydroxy tryptophan (5-HTP) and serotonin by tryptophan-5-hydroxylase and 5-HTP decarboxylase respectively, and then acetylation to N-acetyl serotonin by arylalkalamine N- acetyl transferase, and finally by hydroxyl-indole-O-methyltransferase [13]. It shows the functional versatilities as anti-aging, antioxidant, anti-microbial, immunomodulatory and oncostatic activities [13,14]. In general, it acts as free radical scavenger, a reducer of electron discharge from the electron transport chain, an activator of endogenous antioxidant enzymes, and an enhancer of the efficacy of other antioxidants against cellular oxidative damage [11]. As melatonin having lipophilic characteristics, its encapsulation in the vesicular system may provide maximum targeting efficiency to specific sites of interest with longer bioavailability from the metabolic degradation, the reduced toxicity, and the higher cellular permeability [11]. This review demonstrates mainly the biological efficiencies of melatonin and vesicular melatonin for the treatment of various diseases to consider it as potent vectoring drug.
Preparation of vesicular melatonin
Few drug-loaded vesicular systems are depicted below:
Liposomal melatonin
Multi-lamellar liposomes are prepared with phosphatidyl ethanolamine (PE), cholesterol, stearyl amine / dicetyl phosphate (DCP), and melatonin in the 7:1:1:1 molar ratio respectively [11]. In brief, the above-mentioned ingredients are dissolved in methanol and chloroform mixture (1:2 v/v) in a round-bottomed flask. The formation of a thin dry coating is occurred in the inner side flask by the evaporation of organic solvents following flaskdesiccation overnight. After that, the dried layer is swollen in salinated phosphate buffer (PBS; pH 7.2) for 1h and sonicated for 30 s with a probed sonicator. Then the suspension is centrifuged at 105,000xg for 1h following pellet-washing twice with PBS and storing at -20◦C.
Nano encapsulated melatonin
Following the modified emulsion-diffusion-evaporation method [11], in brief, melatonin and poly (D, L-lactide-co-glycolide) (PLGA) are dissolved in ethyl acetate at room temperature, mixed and emulsified by drop by drop -addition to aqueous dido decyl dimethyl ammonium bromide solution. The emulsion is stirred for 3h at room temperature following homogenization at 15,000 rpm for 5 min and stirring in a water bath at 40◦C for 2h. The suspension is centrifuged at 105,000xg for 1h. The deposited nano capsule is washed twice with Milli-Q water, then re- suspended or lyophilized with 20% sucrose for cryoprotection and stored at -20◦C.
Determination of drug loading and encapsulation efficiency
The drug loading and encapsulation efficiency of vesicular formulations may be assayed spectrophotometrically or using high-performance liquid chromatography (HPLC). The lyophilized vesicular melatonin is dissolved in methanol for 24 h at 4◦C. The percentage drug loading and encapsulation efficiency of vesicular melatonin are detected following the formulas:
Drug loading (%) = [(Total amount of formulated drug – Amount of supernatant drug) / Vesicular mass] x 100
Encapsulation efficiency (%) = [(Total amount of formulated drug – Amount of supernatant drug) / Total amount of formulated drug] x 100
Characterizations
The morphology of the vesicular melatonin may be studied by transmission electron microscope, scanning electron microscope and atomic force microscope. The distribution- analyses and the particle size may be determined by the dynamic light scattering utilizing backscatter detection at 173◦C and the volume-weighted mean diameter by laser diffractometry at 25◦C. The zeta potential may be determined by electrophoretic light scattering.
Functions of melatonin
Melatonin chiefly acts on circadian rhythm regulation and shows its roles as antioxidant, anti- inflammatory and antiapoptotic activities. Melatonin exerts attenuation of circadian disruption based on light-induced inhibition or dark-induced stimulation of melatonin synthesis and secretion via the regulation of in vivo clock genes [15,16]. Melatonin enhances cryptochrome-2 (CRY-2), brain muscle ARNT-like1 (BMAL1) and period circadian protein homologue1 (PER1) -expressionsassociated neurodegeneration. Melatonin as a free radical scavenger and an antioxidant can protect epilepsy, cancer, and neurodegeneration by blocking in vitro and in vivo oxidative stress and enhancing superoxide dismutase (SOD), glutathione peroxidase (GPx) and catalase (CAT) enzymatic expressions and activities [17-20]. Melatonin reacts with ROS and RNS and is oxidatively converted to an antioxidant named N1-acetyl-N2- formyl-5- methoxy kynuramine (AFMK) [21]. Melatonin can attenuate pathogenic inflammation as anti- inflammatory agent through regulations different pathways via decreasing secretions of cytokines (interleukin-1 (IL-1), IL-2, tumor necrosis factor-alpha (TNF-α), and interferon- gamma (IFN-γ)) and enhancing productions of cytokines (IL-27, IL-10, and IL-4). Melatonin can alleviate the secretion of pro-inflammatory cytokines through inhibition of nuclear factor kappa B (NF-kB) and the expression of pro-inflammatory factor cyclooxygenase-2 (COX-2) in neurodegenerative diseases [22,23]. Additionally, melatonin can suppress apoptosis by controlling Bcl-2 / Bax and diminishing the activity and expression of caspase-3 in the protection against neurodegeneration and cancer [24-26].
Mechanisms of actions of melatonin
Melatonin may apply its effects through coupling to particular receptor or direct attachment with its substrate. Melatonin functions via membrane receptors, located chiefly in the central nervous system, named melatonin receptors- type 1a (MT1), type 1b (MT2) and type 1c (MT3) [27,28]. The activations of G-protein coupled receptors members MT1 and MT2, lead to the physiopathological effects of melatonin in anxiety, pain, depression, sleep disorders and neurodegenerative diseases mediating adenylyl cyclase inhibition, phospholipase Cβ activation and soluble guanylyl cyclase inhibition, whereas MT3, the quinine reductase-2 enzyme, has little known effects on melatonin mediated activity on disorders [29-31]. Generally, melatonin enters the nucleus and interacts with the transcription retinoid-related orphan receptoralpha (RZR/ROR) factor following immune modulation and antioxidant enzyme regulation via RORα [32,33]. Furthermore, melatonin may bind intracellular tubulin, calreticulin and calmodulin (CaM) proteins, while melatonin may bind directly to CaM with strong affinity and antagonize intracellular secondary messenger Ca2+ binding to CaM relating to the regulation of CaMkinase- II, cAMP phosphodiesterase and nitric oxide synthase enzymes [27,34-39].
Effects and molecular mechanisms of melatonin in diseases
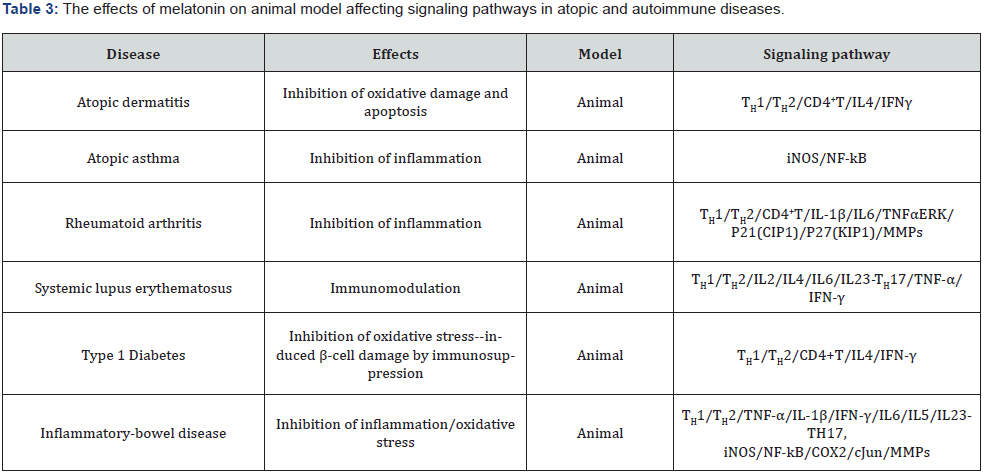
Various evidence have indicated that melatonin has therapeutic and preventive effects on many pathophysiological disorders, while reduced melatonin-level specifically in aged individuals can commit to the development of different diseases emphasizing mainly on the effects of melatonin, cell / animal model and affected signaling pathways [13,40-48] (Tables 1-4).
Effects of melatonin against viral infections
Respiratory syncytial virus (RSV), the negative strand RNA virus belonging to Pneumoviridae family, may cause the lower respiratory tract -infection, while the immune-compromised and aged individuals become prone to drastic disease development with the inflammation and oxidative stress leading to asthma. The virus may activate v-rel reticuloendotheliosis viral oncogene homolog A (Rel A) through ROS generation and the enhancement of interferon regulatory factor 3 (IRF-3) signaling. Some researchers have revealed that melatonin can suppress RSV infection via modulating toll-like receptor 3 (TLR-3) signaling activated nuclear factor kB (NF-kB), IRF-3, the expressions of various inflammatory mediators and the pro- inflammatory cytokines production [40].
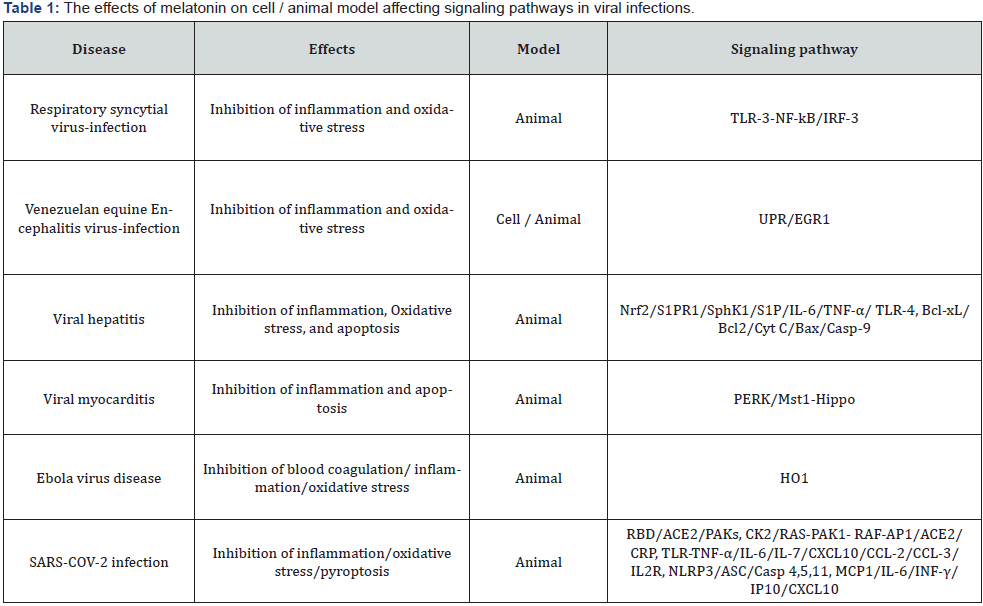
Venezuelan equine encephalomyelitis / encephalitis (VEE) virus, belonging to Togaviridae family, may cause flu-like symptoms e.g., nausea, pharyngitis, fever, fatigue and myalgia among people. After being infected, VEE virus replicates in the brain causing inflammation and injury of the blood brain barrier contributing increased permeability, neuro-invasion, neurological sequelae and pro-inflammatory factors release. VEE viral infection may initiate the unfolded protein response (UPR) signaling through triggering of early growth response protein 1 (EGR-1) leading to oxidative stress induced apoptosis and altered immune responses. Usages of melatonin may diminish enhanced apoptosis marker proteins, malondialdehyde and nitrite against VEE virus infection [40] (Table 1).
Viral hepatitis, caused by the infection with liver-tropic viruses, metabolic disorders, paracetamol toxicity and autoimmune diseases, generates acute liver failure characterized by severe disruption of liver functions resulting jaundice, impairment of coagulation, extensive liver necrosis and progression of encephalopathy. Rabbit hemorrhagic disease (RHD), caused by lethal viral infection, is featured by necrotizing hepatitis, and dispersed intravascular coagulation in the spleen, liver, and kidney. It has been observed that melatonin can protect partial hepatic failure by the triggering of nuclear factor erythroid 2-related factor 2 (Nrf 2) signaling to inhibit oxidative stress and elevate antioxidant enzymes activities. Melatonin can also suppress the apoptotic liver damage by inhibiting the endoplasmic reticulum (ER) stress with the modulation of UPR signaling [40].
The sphingosine kinase 1 (Sph K1) / sphingosine 1-phosphate (S1P) signaling activates RHD virus (RHDV) replication with inflammation during its infection, while melatonin reduces elevated S1PR1 receptor expression, S1P production, TNF-α, IL-6, TLR-4 expressions in RHDV-infection [40]. Moreover, melatonin can inhibit liver apoptosis induced by RHDV infection through the elevation of B-cell lymphoma 2 (Bcl-2) and B-cell lymphoma extra-large (Bcl-xL) expressions, and decrement of cytochrome c (Cyt c) release, Bcl-2 associated X (Bax) expression and caspase-9 activation [40]. Furthermore, melatonin administration can repress autophagic responses in rabbit hemorrhagic virus disease [40].
Myocarditis, characterized by the pathogen-infected inflammation of cardiac muscle tissue, is caused by the immunocompetent cells -infiltration leading to cardiac dysfunction, injuries, and subsequently dilated cardiomyopathy (DCM). Mainly, coxsackievirus B3 induces apoptosis in cardiomyocytes via ER-stress-induced protein kinase R-like ER kinase (PERK) or Mst-Hippo upregulated markers signaling, while melatonin can repress ER stress by reducing autophagy or apoptosis related upregulated markers signaling and inflammations to prevent viral myocarditis [40].
Hemorrhage shock, owing to endothelial injury of blood vessels infected by Ebolavirus, is characterized by increased blood coagulation, weaken immune system, significant inflammatory responses resulting oxidative stress-induced cell, tissue, or organ damages. It has been studied that melatonin can diminish the replication of Ebola virus by inducing heme oxygenase 1 (HO 1) expression, triggering the immune system, affecting thrombin formation, platelet physiology, and reducing vascular permeability [40].
Coronavirus disease 2019 (COVID-19), caused by dire acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is manifested by headache, fever, dry cough, sore throat, chest pain, myalgia, diarrhea, fatigue, decrement of total number of white blood cells, inflammation, pneumonia, and dyspnea leading to chiefly pulmonary injuries. The crown like surface S protein spikes of viruses intermediate the virus entry into the target cells, while the receptor-binding domain (RBD) of S1- subunit of the SARS-CoV-2 anchors to angiotensin-converting enzyme 2 (ACE 2) to initiate endocytosis into the host cells leading to acute respiratory distress syndrome with dysfunction of rennin-angiotensin system (RAS) and amplification of inflamed pulmonary tissue damage triggered by CK2/RAS-PAK1-RAF-AP1 or other signaling [40]. The role of melatonin against anti-viral immunity in bat is not yet thoroughly investigated. However, it is hypothesized that melatonin can act a significant role against SARS-CoV-2 virus infection in bats and other carriers.
The p-21-activated kinases (PAKs), a family of serine / threonine kinases for the effectors GTPases, are involved in the pathogenesis of SARS-CoV-2 viral infection, while p-21 is downregulated by PAK1 in Th1 cells. The phosphatase and tensin homolog (PTEN), a tumor- suppressing phosphatase, can inhibit the COVID-19-inducted angiotensin II-pathological vascular fibrosis via inhibition of PAK1 activity by melatonin [40]. In COVID-19 infection, toll- like receptors (TLRs) interact with SARSCoV- 2 pathogens to activate nicotinamide adenine dinucleotide phosphate (NADPH) oxidase in macrophages through TNF-α induction leading to ROS production for infected cells damages by oxidative bursts and increments of inflammatory markers e.g., c-reactive protein, monocyte chemoattractant protein 1 (MCP1), INF-γ, INF-γ-induced protein 10 (IP-10), ferritin, D-dimers, cytokines (TNF-α, IL-6 and IL-17), chemokines CXC-chemokine ligand 10 (CXCL 10), CC-chemokine ligands 2 and 3 (CCL-2 and CCL-3) and soluble IL-2 receptor associated with dysregulation of the mononuclear phagocyte system [40].
SARS-CoV-2 may also cause severe acute respiratory inflammatory programmed cell death triggering pyroptosis, while ORF8B viral protein anchors to nucleotide-binding domain leucine- rich repeat (NLR) protein and pyrin domain-containing receptor 3 named NLRP3 inflammasome to stimulate apoptosisassociated caspases 4, 5 and 11 and speck-like protein-containing CARD (ASC) for disrupting cell membrane with the liberation of inflammatory products to the extracellular space. Therefore,inhibition of NLRP3-induced pyroptotic cell death in lungs may be the other therapeutic approach for melatonin-utility [40].
Effects of melatonin against few diseases
In ischemic condition due to lack of oxygen supply and its subsequent reperfusion stage, melatonin treatment may restrict the mechanism for RipK3/PGAM5/CypD axis signaling and desensitize endothelial cells to necrosis activated by RipK3 induction, CypD phosphorylation and PGAM up-regulation. Melatonin may also inhibit mPTP opening and mitophagymediated cell death through the suppression of mitochondrial fission followed by ischemic reperfused injury to restore bound VDAC1-HK2 for arresting cardiac microvasculature cell death [41]. Several studies have indicated that melatonin can regulate the immune system activation by reducing acute and chronic inflammation, while melatonin can inhibit lipopolysaccharide induced NF-kB activated iNOS, NO, COX, NLRP3, ASC, caspase-1 and IL-1β expressions in different inflammed / pyrototic cells or tissues [41].
The state of chronic oxidative and endoplasmic reticulum (ER) stresses-induced signaling and subsequent inflammation, insulin and leptin peptide resistances, due to excessive oxidation of glucose and lipids and inefficient autophagy, may cause accumulation of unfolded damaged proteins and mitochondrial dysfunction to develop over-weighted obesity and its comorbodities including diabetes, metabolic syndrome, cardiovascular and neurodegenerative diseases and cancer. Various studies have implicated that melatonin administration can counteract all the damaging effects by improving antioxidant defenses, reducing ER-stress and misfolded proteins, leading to the reductions in neurodegenerative markers, proteasome and the modulation in autophagy, and the amelioration of mitochondrial dysfunction with increased ATP production [42].
Myocardial infarction, the leading cause of morbidity and mortality, may cause oxidative stress- induced inflammatory microenvironment in the infracted areas leading to the apoptotic cell death mediated by mitochondrial outer membrane permeabilization (MOMP), mPTP opening and Cyt c release through the activation of caspase-9 and Bax. Myocardial infarction may also cause necrotic cell death in the infracted areas through the upregulated p53-cyclophilinD (CypD) signaling. Several studies have implicated that melatonin administration may downregulate active pro-apoptotic proteins such as caspase-9 and Bax and upregulate anti-apoptotic Bcl-2 protein from apoptosis through inhibition of MOMP, while it may downregulate p53 expression by inhibiting its translocation to the mitochondria from the cytoplasm for inhibition of cellular necrosis [43].
Osteoporosis, the metabolic disease distinguished by the bone marrow loss with the bone microstructure destruction leads to the bone fragility with the enhanced bone fracture risk. It has been studied that osteoporosis can generate ROS with the oxidative stress leading to the apoptotic cell death, while the melatonin administration can reduce the Bax protein level with the enhanced Bcl-2/Bax ratio by inhibiting the mitochondrial oxidative stress through the SIRT3/SOD2 signaling [44] (Table 2).
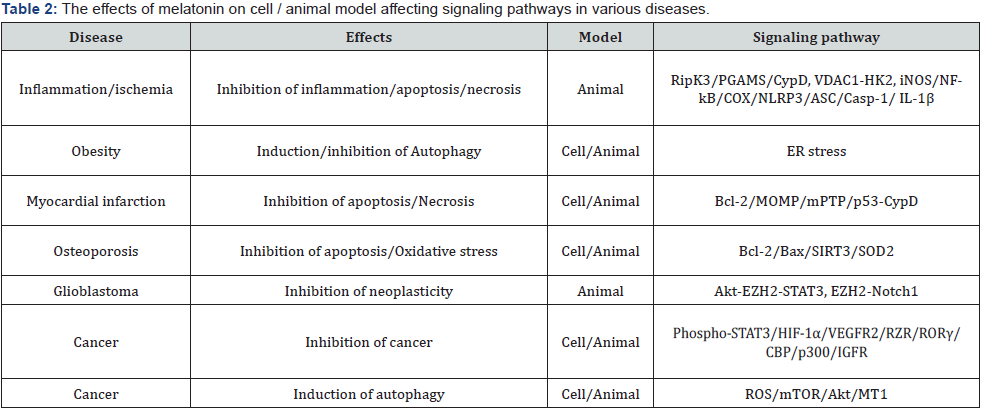
Glioblastoma (GBM), the aggressive common primary brain tumor, contains glioma stem-like cells (GSCs) grown as spheres to induce the enhancement in the tumor-propagation with the self- renewal. Several studies have indicated that for GSC growth, protein kinase B (Akt) phosphorylation can activate the enhancer of zeste 2 polycomb repressive complex 2 (EZH2) which in turn, may catalyze histone H3 methylation and induce the signal transducer and activator of transcription 3 (STAT3) to take part in the cell cycle, tyrosine and serine phosphorylation, and DNA binding. Moreover, EZH2 also can activate and upregulate Notch1.
Several investigators have shown that melatonin treatment can reduce the neoplasticity through the inhibition of Akt-EZH2- STAT3 and EZH2-Notch1 signaling [45].
It has been noted by several researchers that in carcinogenesis due to initiation of uncontrolled cell growth, several signaling and expression of marker proteins such as phospho-STAT3, HIF- 1α, VEGFR2, RZR/RORγ, CBP/p300, and IGFR have been evolved, while melatonin treatments have reduced and inhibited their over-expressions and signaling to protect the cells from cancer development [46]. Other studies have indicated that ROS-induced up-regulation of mTOR/Akt phosphorylation signaling may be operated in carcinogenesis, while the inhibition of the pathway (ROS/mTOR/Akt/MT1) may be exerted through the induction of autophagy by the treatment of melatonin through its MT1 receptor activity [42].
Effects of melatonin against atopic and autoimmune diseases
The hypersensitivity diseases such as allergic or atopic diseases are caused by the activation of TH2 cells and the generation of IgE antibody. The key events for the development of autoimmunity denote the breakdown or failure of different mechanisms to maintain self- tolerances in either T or B lymphocytes, or both. The recognition and the activation of the self- antigens by the auto-reactive lymphocytes are involved for the proliferation and differentiation into the effector cells or their products to cause tissue injury.
Atopic dermatitis named eczema or skin lesions, the chronic inflammatory skin disease, is caused by the TH1/TH2 biphasic inflammatory response to produce IL-4, IL-5, IL-13 and IFN-γ cytokines, possibly owing to the partial diminished activity of the sympathetic nervous system controlled by reduced melatonin secretion. Several investigators have suggested that melatonin treatment can suppress the hypersensitive dermatitis by reducing IgE, IL-4 and IFN-γ productions by activated CD4+ T cells or by both antioxidant and anti-apoptotic signaling [13].
Atopic asthma, the inflammatory lung disease characterized by broncho-constriction, cell migration and hyper-responsiveness, is developed and progressed through the interactions between environmental and genetic factors with the imbalances between oxidative stress and antioxidant defenses probably due to reduced melatonin secretion. Several researchers have investigated that melatonin treatment can inhibit ROS/RNS-induced NF-kBmediated matrix metalloproteinase-9 (MMP-9) and iNOS signaling activities to produce collagen, NO and mucus for reducing airway hyper-responsiveness, inflammation, and mucus production [13].
Autoimmune rheumatoid arthritis (RA), the chronic inflammation of the joints characterized by progressive bone and cartilage erosions associated pannus-proliferation, indicates hyperplasia, enhanced vascularity, and filtration of immune inflammatory cells to the synovial membrane of the joints. In this context, activated CD4+ T lymphocyte cells activate macrophages, monocytes, and synovial fibroblasts to generate various inflammatory IL-1β, IL-6 and TNF-α cytokines. CD4+ T lymphocyte cells also activate B lymphocytes to generate immunoglobulins. Several studies have indicated that melatonin treatment can inhibit the ROS-induced proliferation of RA fibroblast-like synoviocytes via activation of the ERK-mediated cyclin-dependent kinase P27 (KIP1) and P21 (CIP1) inhibitors, and inflammatory immune cells signaling expressions with MMPs-activated cartilage-degradation [13] (Table 3).
Functions of melatonin
Systemic lupus erythematosus (SLR), the multi-factorial autoimmune disease, is developed by immune complexes in blood and tissues to cause extensive tissue damage involving the activation of auto-reactive T lymphocyte cells to initiate B lymphocytes-hyperactivity leading to immune complexes -depositions and polyclonal hyper-gammaglobulinemia. In this context, the levels of TH1, TH2 and TH17 -mediated immune responsive cytokines e.g., IL-2 and IFN-γ, IL-4, and TNF-α and IL-6, respectively, are increased in the SLE disease. Researchers have studied that melatonin administration against SLE disease may reduce the serum auto-antibodies-levels and the generation of inflammatory cytokines through its antioxidant, immunomodulatory and anti-apoptotic effects [13].
Type 1 diabetes (T1D), the insulin-dependent diabetes mellitus, is a T-cell mediated autoimmune disease causing pancreatic β-cells destruction leading to insulin deficit. The imbalance between TH1 and TH2 responses causes the development of diabetes, while TH1- dominant phenotype causes CD4+ T cells-activated enhanced IFN-γ and reduced IL-4 productions. It has been investigated that melatonin treatment can protect the organism by immunesuppression and attenuation of the oxidative stress-induced pancreatic β-cells damages [13].
Autoimmune inflammatory bowel disease (IBD), the group of intestinal inflammatory ulcerative colitis and Crohn’s disease, is manifested by chronic, idiopathic, and relapsing inflammations with the accumulations of immune cells in the intestinal tissues. The infiltration and accumulation of neutrophils, dendritic cells, macrophages, and T and B lymphocytes into the intestinal lamina propia mucosa induct the inflammatory responses associated with TH1 and TH2 lymphocytes-involvements and the enhanced productions of TNF-α, IFN-γ, IL-1β and IL-6 in IBD. In Crohn’s disease, TH1-mediated T cells in lamina propia produce enhanced amounts of IFN-γ, whereas TH2-mediated T cells in ulcerative colitis produce enhanced amounts of IL-5. Furthermore, it has been investigated that the other IL-23-TH17 signaling pathway is involved in IBD. Several investigations have suggested that melatonin treatments can reduce visceral hyperalgia and diseaseseverity through its antioxidant mechanisms, reducing nitrosative stress and lipid peroxidation by scavenging free radicals. Melatonin treatment can also modulate immune attack by regulating the activities of macrophages, metalloproteinases, and by suppressing the activations of iNOS and COX-2, and the levels of pro-inflammatory cytokines by diminishing inflammations. Moreover, melatonin treatment also can modulate apoptosis in colitis by the inhibition of NF-kB and the activation of c-Jun suggesting its antioxidant, anti- inflammatory, and anti-apoptotic features [13].
Effects of melatonin against neurodegenerative diseases
Alzheimer’s disease (AD), manifested by progressive cognitive impairments in the elderly people, indicates the pathology of extracellular senile plaques (SPs) composed of accumulated β- amyloid (Aβ), and intracellular neurofibrillary tangles (NFTs) composed of aggregated, abnormal hyperphosphorylated tau. In addition, the combination of Aβ with apolipoprotein E4 (apo E4) may synergistically aggravate Aβ neurotoxicities. It has been reported that melatonin can inhibit the production and aggregation of Aβ and apo E4 against AD neurotoxicity. Melatonin treatment can also inhibit apoptosis by the decrement of caspase-3 activity and the elevation of Bcl-2 expression in the brain tissue. Furthermore, melatonin usages can diminish Aβ-accumulation through GSK-3β inhibition mediated by the upregulation of the PI3K/Akt signaling to rescue synaptic dysfunction and attenuate memory deficit in AD. Several studies have indicated that multiple protein kinases are involved to phosphorylate tau for its aggregation in neurofibrillary tangles, and protein phosphatases in the regulation of tau phosphorylation in AD. Usages of melatonin can attenuate tau hyperphosphorylation by the regulation of proline- directed GSK-3β kinase, non-proline-directed kinases such as PKA and PKC, cyclin-dependent kinase 5 (CDK5), deathassociated protein kinase 1 (DAPK1), and protein phosphatase- 2A (PP- 2A). Recent study has implicated that melatonin can bind to DAPK1 for promoting DAPK1 protein-degradation via the ubiquitin-mediated proteasome signaling leading to enhanced Pin 1 activity and reduced tau hyperphosphorylation against taurelated AD [47].
Parkinson’s disease (PD), the chronic neurodegenerative disease with bradykinesia, resting tremor, rigidity, postural imbalance, sleep disorder, dysosmia and cognitive impairment, is developed for dopamine (Dop) diminution due to the gradual loss of nigrostriatal dopaminergic neurons in the locus coeruleus (LC) and substantia nigra pars compacta (SNpc) and the existence of cytoplasmic Lewy bodies formed chiefly by fibrillar α-synuclein. Several α-synuclein (SNCA) mutations e.g. A30P are reported to be involved in contributing to PD. It has been reported that melatonin can inhibit oxidative stress and apoptosis by the enhancement of Dop-concentration to preserve SNCA mutated loss of dopaminergic neurons in PD. Furthermore, melatonin treatment can also inhibit α-synuclein aggregation and autophagy through inhibition of CDK5 or enhancement of the ubiquitination of α-synuclein against PDneurotoxicity [47].
Huntington’s disease (HD), the autosomal dominant neurodegenerative disease activated by the dilated cytosineadenine- guanine (CAG) triplet in the gene encoding the Huntingtin (HTT) protein affecting originally the cortex and striatum, is identified by the progressive motor decline, cognitive impairment, sleep and psychiatric disorders, dysphagia, and weight loss. The HD is characterized by the intra-nuclear inclusion of aggregated mutant HTT in neuronal cytoplasm, nucleus, axon terminal and dendrite inducing its apoptosis caused by mitochondrial dysfunction. Mitochondria-dependent cell death in HD, may also be occurred by the enhancement of the intracellular Ca2+ influx via the N-methyl-D-aspartate (NMDA) receptor channel and the induction of mitochondrial permeability transition pore (mPTP). Several studies have implicated that melatonin can diminish cell death by inducting Bcl-2 and reducing Bax expressions with mitochondrial translocation via the interactions with MT1/ MT2 receptors. Moreover, melatonin may exert anti-apoptotic activity through the interactions between Bcl-2 and Bax, and calmodulin with the mitochondrial binding to the MT1/MT2 receptors resulting in the decrement of NMDA receptor-induced enhancement of Ca2+ influx through mPTP activity [47] (Table 4).
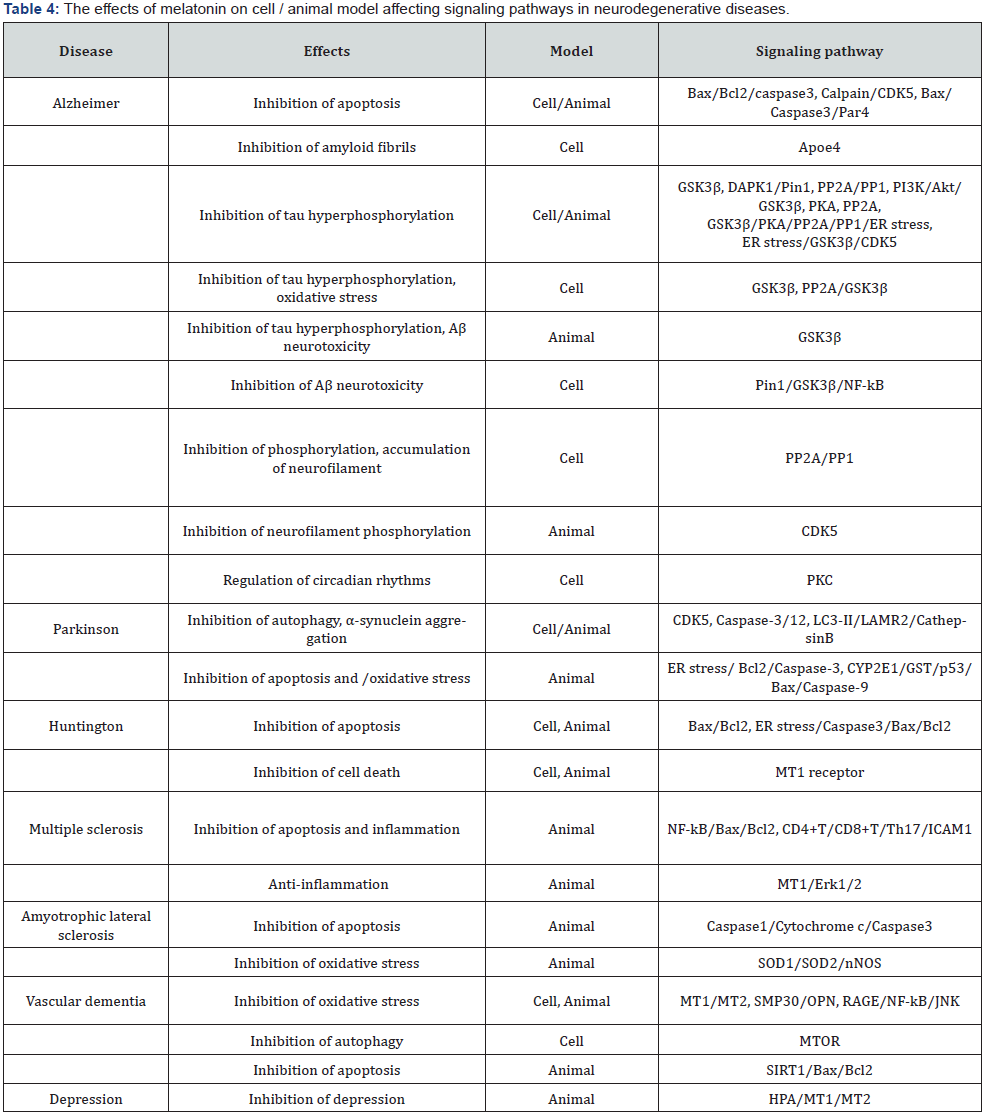
Multiple sclerosis, the progressive chronic inflammatory disease associated with genetic and environmental factors, and immune -mediated disorders resulting in neuro-inflammation, demyelination and axonal loss in the white and gray matters of the central nervous system (CNS), is identified symptomatically by the weakness, numbness or spastic paralysis in the limbs, pain, cognitive impairment, visual dysfunction, non-traumatic disability and psychiatric disorders, evidenced by the lower secretion of melatonin in the biological system [47]. Several researchers have studied that melatonin can exhibit anti-oxidative and antiinflammatory effects against demyelination through the reduction of apoptosis by enhancing Bcl-2 expression and reducing Bax and caspase-3 levels, and the antioxidant activity by triggering NFkB and diminishing heme oxygenase-1 expressions. Moreover, melatonin has been reported to exert the anti-inflammatory effect by diminishing pro-inflammatory IL-1β and TNF-α cytokines against demyelination. Furthermore, few investigators have disclosed that melatonin may reduce the levels of IL-17 produced by TH17 cells through MT1-dependent signaling against demyelination [47].
Amyotrophic lateral sclerosis (ALS), the developing and discriminating degenerations of motor neurons (MNs) in the hypoglossal motor neurons (HMNs), brain stem, spinal cord and the facial motor neurons (FMNs), and their subsequent accumulations as abnormal neurofilaments, is identified by the eventual progressive paralysis and death of the organism. Several investigators have studied that melatonin can significantly inhibit motor neuronal apoptotic death by suppressing the NO formation, the receptor interacting protein-2 (Rip-2)/caspase-1 and caspase-3 signaling and inhibiting mitochondrial Cyt c release through MT1-dependent pathway, and also by eliminating the neurofilaments-accumulation through the enhancement of SOD1 expression in ALS [47].
Vascular dementia (VD) is characterized by the chronic cerebral hypo-perfusion associated with oxidative stresses, neuroinflammations and central cholinergic dysfunctions leading to hippocampal neuronal injuries, deaths, and cognitive impairments. Several researchers have investigated that melatonin can produce antioxidant and anti-inflammatory effects by the modulations of NF-kB, JNK, hypoxia-inducible factor-1 alpha (HIF-1α) and nuclear factor erythroid 2-related factor-2 (Nrf-2) mediated signaling, the elevation of acetylcholine (Ach), nor- epinephrine (NE) and Dop in the hippocampus, the decrement of oxidative stress markers and the enhancement of anti-oxidative factors [47]. Few investigators have studied that melatonin can significantly increase the expressions of osteopontin (OPN) and senescence marker protein- 30 (SMP30), while OPN can inhibit apoptosis as neuroprotection through the downregulations of ROS, iNOS, cleaved caspase-3 and Bax, and the up-regulations of NF-kB, PI3K and Bcl-2, and SMP30 can suppress apoptosis via the modulations of Ca2+ pump activities in the neuronal cell membranes and inhibit the autophagy to restore its expressions [47]. Moreover, few other researchers have elucidated that melatonin can improve cognitive dysfunctions as neuro- protective effects along with the inhibition of oxidative stresses, neuro-inflammations, and central cholinergic dysfunctions through the elevation of brain-derived neuro-throphic factor (BDNF) levels [47].
Depression, the brain-dysfunction, is initiated due to hypothalamus-pituitary-adrenal (HPA) axis dysregulation, while the melatonin treatment can inhibit and modulate HPA axis dysfunction as well as symptomatic depressive-like behaviors through its MT1/MT2 receptor pathway [48].
Elimination of melatonin
Melatonin, secreted or synthesized in the biological system, usually is bound to albumin in blood, then metabolized to 6-hydroxymelatonin by cytochrome P-450 isoforms and conjugated in the liver for producing the main urinary 6-sulfatoxymelatonin metabolite, excreted via the kidney [41].
Conclusions and future perspectives
Several evidence have implicated that potent melatonin plays a pivotal role in the improvement of circadian rhythms, oxidative stress, inflammation, mitochondrial dysfunction, neuronal loss, immune dysfunction, infection, carcinogenesis and other diseases. The endogenous indole molecule of melatonin, responsible for the most potent antioxidant properties, is produced in small amounts, related to diminished synthesis with aging, may cause easily susceptible age-related diseases. It has been observed that most of the experiments have been performed with free melatonin and a few with vesicular melatonin against diseases.
Though melatonin, the small hydrophobic compound, can penetrate cell membrane and biological barriers smoothly, it is needed to encapsulate it into vesicular system with or without selective ligand for its lipophilic property and to reduce toxicity for delivering to specific target site/s to get maximum biological effectiveness with its sustained release and longer bioavailability [11]. In this context, there should be thorough systemic explorations regarding their biodistributions, pharmacokinetics, immune responses, toxicity, elimination, and therapeutic efficacies in different administrative routes especially for oral and intravenous in in vivo biological system to utilize them as proper future therapeutic nanomedicines before going to clinics.
Declaration of Conflicting Interest
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Acknowledgement
This study was supported by the Council of Scientific and Industrial Research (CSIR), Government of India.
Refrences
- Mandal AK (2021) Dendrimers in targeted drug delivery applications: A review of diseases and cancer. Int J Polym Mater Polym Biomater 70(4): 287-297.
- Tan BL, Norhaizan ME, Liew WPP, Rahman HS (2018) Antioxidant and oxidative stress: A mutual interplay in age-related diseases. Front Pharmacol 9: 1162.
- Snezhkina AV, Kudryavtseva AV, Kardyman OL, Savvateeva MV, Melnikova NV, et al. (2019) ROS generation and antioxidant defense systems in normal and malignant cells. Oxid Med Cell Longev 2019: 6175804.
- Ahmed R, Hussain A, Ahsan H (2019) Peroxynitrite: Cellular pathology and implications in autoimmunity. J Immunoass Immunochem 40(2): 123-138.
- Liguori I, Russo G, Curcio F, Bulli G, Aran L, et al. (2018) Oxidative stress, aging, and diseases. Clinic Intervent Aging 13: 757-772.
- Rahal A, Kumar A, Singh V, Yadav B, Tiwari R, et al. (2014) Oxidative stress, prooxidants, and antioxidants: The interplay. Biomed Res Int 2014: 761264.
- Giorgi C, Marchi S, Simoes ICM, Ren Z, Morciano G, et al. (2018) Mitochondria and reactive oxygen species in aging and age-related diseases. Int Review Cell Mol Biol 340: 209-344.
- Chen Y, Qin C, Huang J, Tang X, Liu C, et al. (2020) The role of astrocytes in oxidative stress of central nervous system: A mixed blessing. Cell Prolif 53: e12781.
- Wu Y, Chen M, Jiang J (2019) Mitochondrial dysfunction in neurodegenerative diseases and drug targets via apoptotic signaling. Mitochondrion 49: 35-45.
- Thuyle TT, Thuy TTV, Hai H, Kawada N (2017) Role of oxidative and nitrisative stress in hepatic fibrosis. Chapter (16) in Book “Liver Pathophysiology”, Academic Press, 213- 224.
- Sana S, Ghosh S, Das N, Sarkar S, Mandal AK (2017) Vesicular melatonin efficiently downregulates sodium fluoride-induced rat hepato- and broncho- TNF-α, TGF-β expressions, and associated oxidative injury: A comparative study of liposomal and nanoencapsulated forms. Int J Nanomed 12: 4059-4071.
- Xie S, Fan W, He H, Huang F (2020) Role of melatonin in the regulation of pain. J Pain Res 13:331-343.
- Calvo JR, Maldonado MD (2016) The role of melatonin in autoimmune and atopic diseases. AIMS Mol Sci 3(2): 158-186.
- Tekbas OF, Ogur R, Korkmaz A, Kilic A, Reiter RJ (2008) Melatonin as an antibiotic: New insights into the actions of this ubiquitous molecule. J Pin Res 44(2): 222-226.
- Claustrat B, Brun J, Chazot G (2005) The basic physiology and pathophysiology of melatonin. Sleep Med Rev 9: 11-24.
- Benot S, Molinero P, Soutto M, Gonerna R, Guerrero JM (1998) Circadian variation in the rat serum total antioxidant status: Correlation with melatonin levels. J Pineal Res 25: 1-4.
- He R, Cui M, Lin H, Zhao L, Wang J, et al. (2018) Melatonin resists oxidative stress- induced apoptosis in nucleus pulposus cells. Life Sci 199: 122-130.
- Reiter RJ, Tan DX, Erren TC, Fuentes-Broto L, Paredes SD (2009) Light-mediated perturbations of circadian timing and cancer risk: A mechanistic analysis. Integr Cancer Ther 8: 354-360.
- Gupta M, Gupta YK, Agarwal S, Aneja S, Kalaivani M, et al. (2004) Effects of add-on melatonin administration on antioxidant enzymes in children with epilepsy taking carbamazepine monotherapy: A randomized, double-blind, placebo-controlled trial. Epilepsia 45: 1636-1639.
- Rodriguez C, Mayo JC, Sainz RM, Antolin I, Herrera F, et al. (2004) Regulation of antioxidant enzymes: A significant role for melatonin. J Pineal Res 36: 1-9.
- Hirata F, Hayaishi O, Tokuyama T, Seno S (1974) In vitro and in vivo formation of two new metabolites of melatonin. J Biol Chem 249: 1311-1313.
- Rosales Corral S, Tan DX, Reiter RJ, Valdivia-Velazquez M, Martnez-Barboza G, et al. (2003) Orally administered melatonin reduces oxidative stress and pro-inflammatory cytokines induced by amyloid-beta peptide in rat brain: A comparative, in vivo study versus vitamin C and E. J Pineal Res 35: 80-84.
- Yokota O, Terada S, Ishizu H, Ishihara T, Ujike H, et al. (2003) Cyclo-oxygenase-2 in the hippocampus is up-regulated in Alzheimer’s disease but not in variant Alzheimer’s disease with cotton wool plaques in humans. Neurosci Lett 343: 175-179.
- Jang MH, Jung SB, Lee MH, Kim CJ, Oh YT, et al. (2005) Melatonin attenuates amyloid beta 25-35-induced apoptosis in mouse microglial bv2 cells. Neurosci Lett 380: 26-31.
- Wang J, Xiao X, Zhang Y, Shi D, Chen W, et al. (2012) Simultaneous modulation of cox-2, p300, akt, and apaf-1 signaling by melatonin to inhibit proliferation and induce apoptosis in breast cancer cells. J Pineal Res 53: 77-90.
- Menendez-Menendez J, Hermida-Prado F (2019) Deciphering the molecular basis of melatonin protective effects on breast cells treated with doxorubicin: Twist1 a transcription factor involved in emt and metastasis, a novel target of melatonin. Cancers 11: 1011.
- Ekmekcioglu C (2006) Melatonin receptors in humans: Biological role and clinical relevance. Biomed Pharmacother 60: 97-108.
- Emet M, Ozcan H, Yayla M, Halici Z, Hacimuftuoglu A (2016) A review of melatonin, its receptors and drugs. Eurasian J Med 48: 135.
- Pandi Perumal SR, Trakht I, Srinivasan V, Spence DW, Maestroni GJ, et al. (2008) Physiological effects of melatonin: Role of melatonin receptors and signal transduction pathways. Prog Neurobiol 85: 335-353.
- Comai S, Gobbi G (2014) Unveiling the role of melatonin MT2 receptors in sleep, anxiety and other neuropsychiatric diseases: A novel target in psycho pharmacology. J Psychiatry Neurosci JPN 39: 6-21.
- Nosjean O, Frrro M, Coge F, Beauverger P, Henlin JM, et al. (2000) Identification of the melatonin-binding site MT3 as the quinine reductase2. J Biol Chem 275: 31311-31317.
- Carlberg C (2000) Gene regulation by melatonin. Ann N Y Acad Sci 917: 387-396.
- Garcia JA, Volt H, Venegas C, Doerrier C, Escanes G, et al. (2015) Disruption of the nf- kappa b / nlrp3 connection by melatoninrequires retinoid-related orphan receptor-alpha and blocks the septic response in mice. FASEB J 29: 3863-3875.
- Cardinali DP, Freire F (1975) Melatonin effects on brain. Interaction with microtubule protein, inhibition of fast axoplasmic flow and induction of crystalloid and tubular formations in the hypothalamus. Mol Cell Endocrinol 2: 317-330.
- Melendez J, Maldonado V, Ortega A (1996) Effect of melatonin on beta-tubulin and map2 expression in nie-115 cells. Neurochem Res 21: 653-658.
- Macias M, Escames G, Leon J, Coto A, Sbihi Y, et al. (2003) Calreticulin-melatonin. An unexpected relationship. Eur J Biochem 270: 832-840.
- Benitez King G, Anton-Tay F (1993) Calmodulin mediates melatonin cytoskeletal effects. Experientia 49: 635-641.
- Benitez King G, Huerto-Delgadillo L, Anton Tay F (1991) Melatonin modifies calmodulin cell levels in mdck and nle-115 cell lines and inhibits phosphodiesterase activity in vitro. Brain Res 557: 192-289.
- Benitez King G, Rios A, Martinez A, Anton Tay F (1996) In vitro inhibition of Ca2 / calmodulin-dependent kinase ii activity by melatonin. Biochim Biophys Acta 1290: 191- 196.
- Juybari KB, Pourhanifeh MH, Hosseinzadeh A, Hemati K, Mehrzadi S (2020) Melatonin potentials against viral infections including COVID-19: Current evidence and new findings. Virus Res 287: 198108.
- Tarocco A, Caroccia N, Morciano G, Wieckowski MR, Ancora G, et al. (2019) Melatonin as a master regulator of cell death and inflammation: Molecular mechanisms and clinical implications for newborn care. Cell Death Disease 10: 317.
- Boga JA, Caballero B, Potes Y, Perez-Martinz Z, Reiter RJ, et al. (2019) Therapeutic potential of melatonin related to its role as an autophagy regulator: A review. J Pineal Res 66: e12534.
- Ma Q, Yang J, Huang X, Guo W, Li S, et al. (2018) Poly (Lactide-co-Glycolide)- monomethoxy-poly- (Polyethylene Glycol) nanoparticles loaded with melatonin protect adipose-derived stem cells transplanted in infracted heart tissue. Stem Cells 36: 540-550.
- Xiao L, Lin J, Chen R, Huang Y, Liu Y, et al. (2020) Sustained release of melatonin from GelMA liposomes reduced osteoblast apoptosis and improved implant osseointegration in osteoporosis. Oxid Med Cell Longev 6797154.
- Moretti E, Favero G, Rodella LF, Razzani R (2020) Melatonin’s antineoplastic potential against glioblastoma. Cells 9: 599.
- Rahbarghazi A, Siahkouhian M, Rahbarghazi R, Ahmadi M, Bolboli L, et al. (2021) Role of melatonin in the angiogenesis potential; highlights on the cardiovascular disease. J Inflam 18: 4.
- Chen D, Zhang T, Lee TH (2020) Cellular mechanisms of melatonin: Insight from neurodegenerative diseases. Biomol 10: 1158.
- Si M, Sun Q, Ding H, Cao C, Huang M, et al. (2020) Melatonin-loaded nanoparticles for enhanced antidepressant effects and HPA hormone modulation. Adv Polym Technol 4789475.






























