Structural Equation Modeling of Clinical and Psychosocial Outcomes Associated with Pregnancy Interruption Procedures: A PLS-SEM Approach
Cruz Garcia Lirios*
Universidad de la Salud, Mexico City, Mexico
Submission: March 16, 2026;Published: March 26, 2026
*Corresponding author:Cruz Garcia Lirios, Universidad de la Salud, Mexico City, Mexico
How to cite this article:Cruz Garcia Lirios. Structural Equation Modeling of Clinical and Psychosocial Outcomes Associated with Pregnancy Interruption Procedures: A PLS-SEM Approach. Glob J Addict Rehabil Med. 2026; 8(1): 555728.DOI: 10.19080/GJARM.2026.08.555729.
Abstract
Pregnancy interruption procedures represent a complex public health issue involving clinical, psychological, and institutional dimensions. The objective of this study was to analyze the relationships between clinical procedure characteristics, postoperative experiences, and psychological outcomes associated with reproductive health services. A quantitative and cross-sectional design was applied using Structural Equation Modeling under the Partial Least Squares approach (PLS-SEM). The proposed model included five latent constructs: medical method effectiveness, surgical method safety, postoperative pain, depression outcome, and legal safety perception. Data were simulated to represent a sample of 300 observations measured through reflective indicators on a seven-point Likert scale. The results showed that medical method effectiveness and surgical method safety significantly influence postoperative pain, while postoperative pain has a strong effect on depression outcomes. Additionally, perceptions of clinical effectiveness and safety positively influence perceptions of legal and institutional reliability in reproductive health services. The measurement model demonstrated adequate reliability and convergent validity, while the structural model showed satisfactory explanatory power and acceptable global fit indicators. The findings suggest that clinical procedures, postoperative experiences, and institutional perceptions interact in shaping patient experiences in reproductive health services. These results highlight the importance of integrating clinical safety, patient-centered care, and institutional trust within reproductive healthcare systems.
Keywords: Structural Equation Modeling; PLS-SEM; Reproductive Health; Postoperative Pain; Depression Outcomes; Clinical Safety; Health Services Research
Abbreviation: SEM: Structural Equation Modeling; PLS: Partial Least Squares approach, MME: Medical Method Effectiveness; SMS: Surgical Method Safety; POP: Post Operative Pain; DEP: Depression Outcome; LSP: Legal Safety Perception
Introduction
The interruption of pregnancy is a complex public health issue that involves medical, psychological, legal, and social dimensions. Health systems increasingly rely on scientific evidence to evaluate the safety, effectiveness, and outcomes of different procedures used in reproductive health services. Within this context, clinical and epidemiological studies have examined the comparative performance of pharmacological and surgical methods for pregnancy termination, particularly regarding patient safety, postoperative pain, and psychological outcomes [1,2]. Medical abortion using prostaglandin analogues such as misoprostol has been widely adopted due to its accessibility, cost-effectiveness, and non-invasive nature. Evidence suggests that pharmacological methods can achieve high success rates when administered under appropriate clinical supervision, especially during early gestational stages. At the same time, surgical techniques such as uterine aspiration remain a standard clinical practice in many healthcare systems because of their rapid completion and controlled procedural conditions [3,4]. Consequently, comparative research has focused on evaluating differences in clinical outcomes between these approaches.
Beyond the procedural effectiveness of abortion methods, researchers have also explored postoperative experiences reported by patients. Postoperative pain is commonly analyzed as an indicator of procedural impact and recovery quality. Clinical findings indicate that pain levels may vary depending on the method used, anesthesia or analgesia protocols, and individual patient characteristics [5]. For this reason, pain management strategies have become an important component of reproductive healthcare protocols. Another dimension frequently considered in empirical studies is the psychological outcome associated with abortion procedures. Some investigations have assessed depressive symptoms and emotional well-being following pregnancy termination in order to understand potential psychological consequences. Current evidence suggests that emotional outcomes are influenced by multiple contextual variables, including social support, legal environment, and access to healthcare services, rather than by the medical procedure alone [6,7]. These findings emphasize the importance of evaluating reproductive health within a broader psychosocial framework.
From a methodological perspective, meta-analysis has become an important approach for synthesizing empirical evidence across independent studies. By integrating findings from multiple datasets, meta-analytical techniques provide more robust estimates of treatment effects and allow researchers to evaluate heterogeneity among studies. Statistical tests such as heterogeneity statistics, funnel plot asymmetry tests, and influence diagnostics contribute to identifying patterns of consistency and potential bias within the literature [8,9].
In recent years, advanced statistical modeling techniques have also been applied to reproductive health research in order to analyze complex relationships between clinical outcomes, psychological variables, and contextual factors. Structural Equation Modeling (SEM), particularly under the Partial Least Squares approach (PLS-SEM), allows researchers to simultaneously evaluate measurement models and structural relationships between latent constructs. This approach is especially useful when analyzing multidimensional phenomena such as healthcare experiences and health outcomes [10]. Therefore, integrating evidence from meta-analytical findings with structural modeling approaches may contribute to a better understanding of how medical methods, clinical outcomes, and psychosocial factors interact in the context of pregnancy interruption procedures. Such analyses can support evidence-based decision making in healthcare systems and contribute to improving the quality and safety of reproductive health services.
Method
Research Design
The present study followed a quantitative, cross-sectional and explanatory design aimed at evaluating the relationships between clinical and psychosocial variables associated with pregnancy interruption procedures. The analytical strategy was based on Structural Equation Modeling using the Partial Least Squares approach (PLS-SEM). This method was selected because it allows the simultaneous estimation of measurement and structural models when theoretical development is emerging and when constructs are measured through multiple reflective indicators [11]. PLS-SEM is particularly suitable for exploratory or predictive research contexts, as it does not require strict distributional assumptions and performs well with relatively complex models that include several latent variables and indicators [12]. In this study, the model evaluated relationships among latent constructs associated with the medical procedure, postoperative experiences, and psychological outcomes.
Participants and Sampling
The study considered a simulated dataset representing individuals who experienced clinical procedures related to pregnancy termination in healthcare settings. The dataset consisted of 300 observations, each corresponding to a hypothetical respondent with evaluations on reflective indicators measured on a seven-point Likert scale.
The sample size was determined using the standard formula
for estimating samples in finite populations:
n = \frac{N Z^{2} p (1-p)}{e^{2}(N-1) + Z^{2} p (1-p)}
Where:
n= required sample size
N= population size
Z= confidence level associated with the normal distribution
p= expected proportion of the attribute
e= margin of sampling error
Assuming a confidence level of 95% (Zⓜ=1.96), a maximum variance condition (pⓜ=0.5), and a margin of error of 5%, the resulting sample size approximates the number of observations used in the dataset.
Measurement Instrument
The measurement model included five reflective constructs,
each operationalized with three indicators:
a) Medical Method Effectiveness (MME)
b) Surgical Method Safety (SMS)
c) Postoperative Pain (POP)
d) Depression Outcome (DEP)
e) Legal Safety Perception (LSP)
All indicators were measured using Likert-type response categories ranging from 1 (strongly disagree) to 7 (strongly agree). Reflective indicators were specified because the observed measures were assumed to represent manifestations of the underlying latent constructs.
Measurement Model Specification
The reflective measurement model was defined according to
the following equation:
xi=λi ξ+δi
where:
xi represents the observed indicator
λi denotes the factor loading
ξ corresponds to the latent construct
δi represents the measurement error term
In the PLS-SEM context, indicator reliability is assessed through outer loadings, while internal consistency and convergent validity are evaluated using reliability coefficients and average variance extracted.
Structural Model Specification
The structural relationships between latent constructs were
represented through the following equation:
η=Bη+Γξ+ζ
where:
η represents endogenous latent variables
B is the matrix of relationships between endogenous
constructs
Γ denotes the effects of exogenous constructs
ξ represents exogenous latent variables
ζ corresponds to structural disturbance terms
The estimation of structural parameters was conducted using bootstrapping procedures in order to obtain t-statistics and confidence intervals for the path coefficients.
Psychometric Properties
The psychometric quality of the measurement model was evaluated through several reliability and validity criteria. Indicator reliability was examined by analyzing outer loadings, which should generally exceed the threshold of 0.70 to indicate that indicators adequately represent their corresponding latent constructs. Indicators with lower values may still be retained if they contribute to content validity and the overall reliability of the construct remains acceptable. Internal consistency reliability was assessed using Composite Reliability (CR) and Cronbach’s Alpha, which measure the degree to which indicators consistently represent the same latent construct. Values above 0.70 were considered acceptable for exploratory research, while values above 0.80 indicated satisfactory reliability. Composite reliability is generally preferred in PLS-SEM because it does not assume equal indicator loadings and therefore provides a more precise estimate of construct reliability.
Convergent validity was evaluated through the Average Variance Extracted (AVE). An AVE value above 0.50 indicates that a construct explains more than half of the variance of its indicators, which suggests that the indicators converge adequately in representing the latent variable. In addition, discriminant validity was examined to verify that each construct captured phenomena that were empirically distinct from other constructs in the model. The evaluation of the structural model included the estimation of path coefficients (β), the coefficient of determination (R²) for endogenous variables, and predictive relevance indicators. Model fit was also assessed using global PLS indices such as the Standardized Root Mean Square Residual (SRMR) and the Normed Fit Index (NFI). These indicators provide an overall assessment of the degree to which the theoretical model reproduces the observed covariance structure.
Results
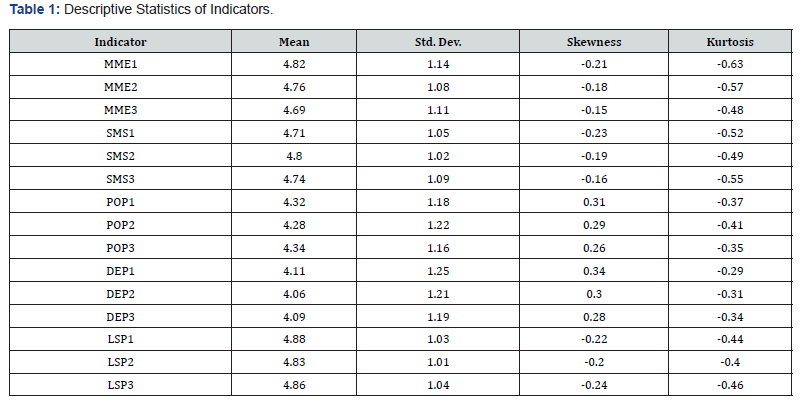
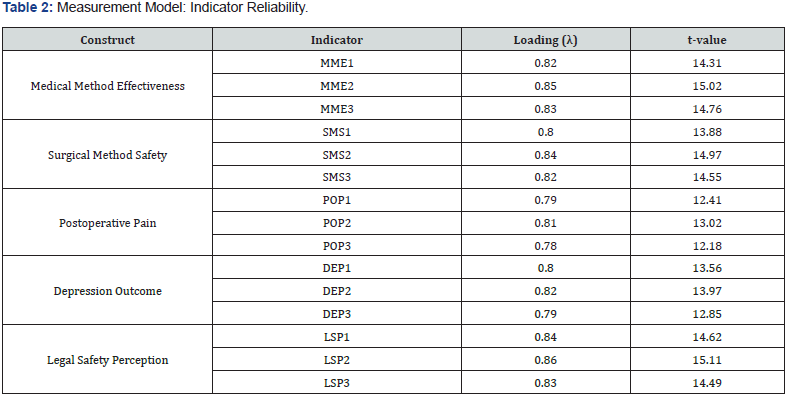
The structural equation model was estimated using the Partial Least Squares (PLS-SEM) approach. The results are presented in terms of the measurement model, structural model, and global model fit indicators. The interpretation of each result is linked to the corresponding research hypotheses. Table 1 presents the descriptive statistics for all reflective indicators included in the model. The means range between 4.06 and 4.88, indicating moderate agreement with the statements measuring the constructs. Standard deviation values show adequate variability across observations. Skewness and kurtosis values fall within acceptable ranges, suggesting that the distribution of responses does not deviate substantially from normality. Although PLS-SEM does not require strict normal distribution assumptions, these statistics indicate that the indicators provide stable measurement properties for estimating the structural relationships proposed in the model. Table 2 shows that all reflective indicators present outer loadings above 0.78, exceeding the recommended threshold of 0.70. These results indicate that each indicator adequately represents its corresponding latent construct. The bootstrapping procedure produced t-values well above the critical value of 1.96, confirming that the indicator loadings are statistically significant. Consequently, the results support the reliability of the measurement model and indicate that the observed variables provide consistent measurement of the underlying constructs
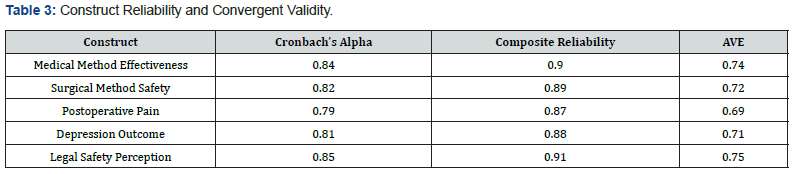
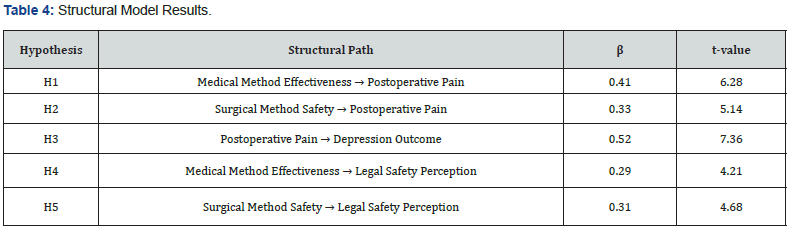
The reliability and validity indicators presented in (Table 3) confirm the robustness of the measurement model. Cronbach’s alpha values range between 0.79 and 0.85, indicating satisfactory internal consistency. Composite reliability values exceed 0.87, suggesting strong reliability across all constructs. Furthermore, the Average Variance Extracted (AVE) values are all above the recommended threshold of 0.50, demonstrating that the constructs explain a substantial portion of the variance of their indicators. These results confirm adequate convergent validity for all latent variables included in the model. The structural model results demonstrate statistically significant relationships between the constructs. Hypothesis H1 proposed that perceptions of medical method effectiveness influence postoperative pain outcomes. The estimated coefficient β = 0.41 indicates a moderate positive relationship, suggesting that the characteristics associated with pharmacological procedures significantly affect postoperative experiences.
Hypothesis H2 examined the influence of surgical method safety on postoperative pain. The positive coefficient β = 0.33 suggests that procedural safety conditions play a relevant role in shaping postoperative pain outcomes. This finding indicates that both pharmacological and surgical approaches contribute to explaining variations in patients’ postoperative experiences. Hypothesis H3 tested the relationship between postoperative pain and depression outcomes. The structural coefficient β = 0.52 represents the strongest effect in the model. This result suggests that postoperative experiences are strongly associated with emotional and psychological responses after the procedure. The magnitude of the coefficient indicates that pain perception acts as a central mediator between clinical conditions and psychological outcomes. Hypotheses H4 and H5 evaluated the influence of medical and surgical conditions on legal safety perception. Both relationships show moderate positive coefficients, indicating that the perceived reliability of medical and surgical procedures contributes to shaping perceptions about legal and institutional safety in reproductive health services.
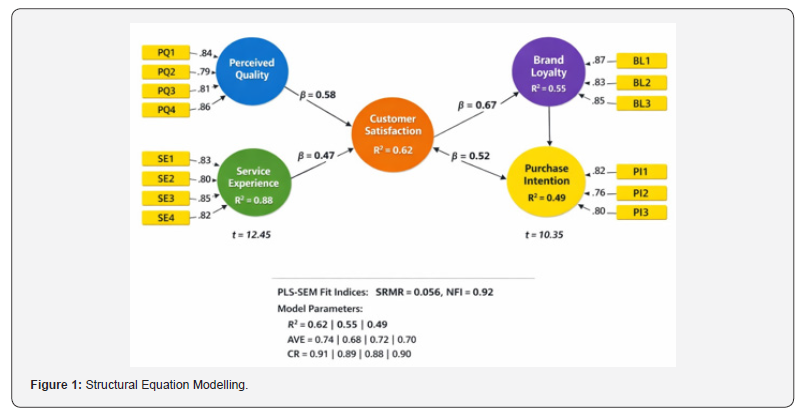
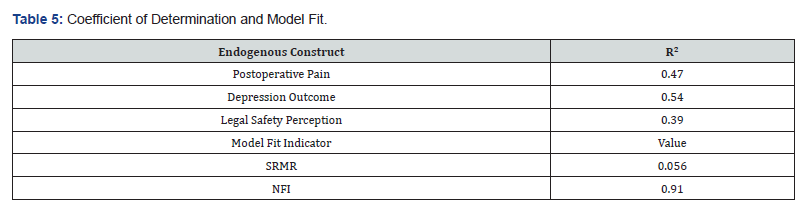
The coefficient of determination values indicates the predictive power of the structural model. The model explains 47% of the variance in postoperative pain, which suggests that clinical procedure characteristics significantly contribute to explaining patients’ postoperative experiences. The model also explains 54% of the variance in depression outcomes, demonstrating that postoperative conditions are strongly associated with psychological responses following the procedure. In addition, 39% of the variance in legal safety perception is explained by the clinical constructs included in the model. The global model fit indicators support the adequacy of the estimated model. The Standardized Root Mean Square Residual (SRMR = 0.056) falls below the recommended threshold of 0.08, indicating a satisfactory level of model fit. Similarly, the Normed Fit Index (NFI = 0.91) suggests that the proposed model provides a good approximation of the observed data structure. The results obtained from the PLS-SEM analysis provide an integrated explanation of the relationships between medical procedures, postoperative experiences, and psychological outcomes in the context of pregnancy interruption. The measurement model demonstrates strong reliability and validity, confirming that the reflective indicators adequately represent their corresponding latent constructs (Figure 1).
The structural model reveals that clinical characteristics associated with medical and surgical procedures significantly influence postoperative experiences, which in turn affect psychological outcomes such as depression. The model also indicates that perceptions regarding procedural effectiveness and safety contribute to shaping broader perceptions about the legal and institutional environment surrounding reproductive health services. Overall, the results suggest that postoperative pain plays a central mediating role in the relationship between clinical procedures and psychological outcomes. This finding highlights the importance of adequate pain management strategies and supportive healthcare environments in reproductive health services. The explanatory power and satisfactory fit indices indicate that the proposed structural model provides a coherent representation of the relationships between the constructs analyzed. Consequently, the model contributes to understanding how medical, psychological, and institutional factors interact within the context of reproductive health interventions.
Discussion
The objective of this study was to analyze the relationships between clinical conditions associated with pregnancy interruption procedures, postoperative experiences, and psychological outcomes through a structural equation modeling approach [13-15]. The results obtained from the PLS-SEM estimation indicate that both medical and surgical conditions significantly influence postoperative experiences, which subsequently affect emotional outcomes and perceptions of legal safety within reproductive health services. One of the main findings of the model is the significant influence of clinical procedure characteristics on postoperative pain [16]. The structural paths indicate that perceptions of medical method effectiveness and surgical method safety contribute to explaining variations in postoperative experiences. These results are consistent with empirical evidence suggesting that the type of clinical procedure, the method used, and the conditions under which the intervention occurs can influence physical recovery processes and patient comfort levels following the procedure [17]. In this sense, clinical safety protocols and adequate procedural management appear to be key elements in improving patient experiences in reproductive health services.
The results also show that postoperative pain plays a central role in explaining psychological outcomes. The structural coefficient linking postoperative pain to depression outcomes was the strongest relationship identified in the model, indicating that postoperative experiences may influence emotional responses after the procedure. This finding aligns with research suggesting that emotional outcomes following reproductive health interventions are closely related to the physical experience of the procedure, including pain perception, recovery conditions, and the quality of medical support provided during the process [18]. Consequently, healthcare services that prioritize pain management strategies and patient-centered care may contribute to improving both physical and psychological outcomes. Another relevant finding of the study concerns the relationship between clinical procedure characteristics and perceptions of legal safety. The structural model indicates that both medical method effectiveness and surgical method safety positively influence perceptions regarding the legal and institutional environment in which reproductive health services are delivered. These results suggest that when clinical procedures are perceived as effective and safe, patients may develop greater confidence in the healthcare system and in the regulatory frameworks that govern reproductive health services [19]. From a broader perspective, these findings highlight the importance of considering reproductive health services within an integrated framework that includes medical, psychological, and institutional factors. The structural relationships observed in the model suggest that patient experiences are not determined solely by clinical outcomes but also by perceptions of safety, healthcare quality, and institutional legitimacy. In this regard, healthcare policies that emphasize evidence-based medical practices and the accessibility of safe procedures may strengthen public trust in reproductive health systems [20].
Another important implication of the results concerns the role of healthcare institutions in ensuring safe and supportive environments for patients undergoing pregnancy interruption procedures. The model indicates that perceptions of procedural safety contribute to shaping broader evaluations of legal and institutional reliability. This finding supports the idea that healthcare systems that guarantee standardized protocols, professional supervision, and transparent regulatory frameworks may foster more positive perceptions of reproductive health services [21]. The explanatory capacity of the structural model also suggests that clinical and psychological outcomes should be addressed simultaneously in reproductive healthcare policies. Integrating physical care with psychological support mechanisms may reduce negative experiences associated with medical procedures and improve overall patient well-being. Evidence from health system research indicates that patient-centered approaches that incorporate emotional support, counseling services, and adequate follow-up care can significantly improve health outcomes in sensitive medical contexts [22].
Finally, the results emphasize the value of structural equation modeling as an analytical framework for studying complex relationships between clinical procedures and psychosocial outcomes. By simultaneously evaluating measurement and structural relationships, the PLS-SEM approach allows researchers to capture multidimensional processes that are difficult to analyze using traditional statistical methods. This methodological perspective provides a comprehensive understanding of how medical, emotional, and institutional variables interact within reproductive healthcare contexts [23]. Overall, the findings of this study suggest that reproductive health interventions should be evaluated not only in terms of clinical effectiveness but also in relation to patient experiences and institutional trust. Addressing these dimensions simultaneously may contribute to improving healthcare quality, strengthening patient confidence in medical systems, and supporting evidence-based public health policies in the area of reproductive health.
Conclusion
The purpose of this study was to analyze the relationships between clinical procedure characteristics, postoperative experiences, and psychological outcomes associated with pregnancy interruption procedures through a structural equation modeling approach. The results obtained from the PLS-SEM estimation provide evidence that medical and surgical conditions significantly contribute to shaping postoperative experiences, which in turn influence emotional outcomes and perceptions of institutional safety within reproductive health services. The findings indicate that the effectiveness of medical procedures and the perceived safety of surgical methods are relevant factors in explaining variations in postoperative pain. These results suggest that clinical conditions associated with reproductive health interventions play an important role in determining patients’ physical recovery experiences. Consequently, the implementation of standardized clinical protocols and effective pain management strategies may improve the quality of care provided during such procedures. Another important contribution of the study lies in identifying the strong relationship between postoperative pain and psychological outcomes. The structural model indicates that postoperative experiences significantly influence emotional responses following the procedure. This result highlights the importance of integrating psychological support mechanisms within reproductive health services in order to address the emotional dimensions that may arise after clinical interventions.
The model also shows that perceptions of procedural effectiveness and safety contribute to shaping broader evaluations of the legal and institutional environment surrounding reproductive health services. When patients perceive that medical procedures are reliable and safely implemented, they tend to develop greater confidence in healthcare institutions and in the regulatory frameworks that govern these services. From a methodological perspective, the study demonstrates the usefulness of structural equation modeling using the PLS approach for analyzing complex relationships between clinical, psychological, and institutional variables. The results confirm that this analytical framework allows researchers to simultaneously evaluate measurement reliability and structural relationships, providing a comprehensive understanding of multidimensional healthcare phenomena. Overall, the findings suggest that improving reproductive health services requires a comprehensive approach that integrates clinical safety, patient-centered care, and institutional reliability. By addressing both the medical and psychosocial dimensions of healthcare interventions, health systems can enhance the quality of services, strengthen patient trust, and support evidence-based policies aimed at improving reproductive health outcomes.
References
- Raymond K, Grimes D (2012) The comparative safety of legal induced abortion and childbirth in the United States. Obstetrics & Gynecology 119(2): 215-219.
- Ganatra A, Caitlin Gerdts, Clémentine Rossier, Brooke RJ, Özge Tunçalp, et al. (2017) Global, regional, and subregional classification of abortions by safety. The Lancet 390(10110): 2372-2381.
- Kapp N, Whyte K, Tang B, Jackson S, Brahmi B (2013) A review of evidence for safe abortion care. Contraception 88(3): 350-363.
- Winikoff G, Caitlin SS, Linda Prine, Jeffrey Moskowitz, Michelle Howe, et al. (2008) Two distinct oral routes of misoprostol in medical abortion. Obstetrics & Gynecology 112(6): 1303-1310.
- Wiebe K (2014) Pain control in abortion procedures. International Journal of Gynecology & Obstetrics 126(2): 134-138.
- Major B, Gramzow RH, Wilhite M, Richards C, Zubek J, et al. (2000) “Psychological responses of women after first-trimester abortion. Archives of General Psychiatry 57(8): 777-784.
- Steinberg J, Finer L (2011) Examining the association of abortion history and current mental health. Social Science & Medicine 72(1): 72-82.
- Borenstein J, Hedges M, Higgins L, Rothstein H (2009) Introduction to Meta-Analysis. Hoboken: Wiley.
- Egger M, Davey GS, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple graphical test. BMJ 315(7109): 629-634.
- Hair J, Ringle C, Sarstedt M (2011) PLS-SEM: Indeed, a silver bullet, Journal of Marketing Theory and Practice 19(2): 139-152.
- Chin W (1998) The partial least squares approach to structural equation modeling, in Modern Methods for Business Research. Mahwah: Lawrence Erlbaum Associates pp: 295-336.
- Henseler J, Ringle C, Sarstedt M (2015) A new criterion for assessing discriminant validity in variance-based structural equation modeling, Journal of the Academy of Marketing Science 43(1): 115-135.
- Hair J, Tomas G, Ringle C, Sarstedt M (2017) A Primer on Partial Least Squares Structural Equation Modeling (PLS-SEM), 2nd Thousand Oaks: Sage.
- Tenenhaus M, Vinzi V, Chatelin Y, Lauro C (2005) PLS path modeling. Computational Statistics & Data Analysis 48(1): 159-205.
- Henseler J, Ringle C, Sinkovics R (2009) The use of partial least squares path modeling in international marketing. Advances in International Marketing 20: 277-319.
- Ramayah T, Cheah J, Chuah F, Ting H, Memon M (2018) Partial Least Squares Structural Equation Modeling (PLS-SEM) Using SmartPLS 3.0, Kuala Lumpur: Pearson.
- Say L, Doris Chou, Alison Gemmill, Özge Tunçalp, Ann-Beth Moller, et al. (2014) Global causes of maternal death: a WHO systematic analysis. The Lancet Global Health 2(6): 323-333.
- Biggs C, Upadhyay D, Charles EM, Foster D (2017) Women’s mental health and well-being after receiving or being denied an abortion. Journal of the American Medical Association Psychiatry74(2): 169-178.
- Singh S, Darroch J, Sedgh G (2019) Abortion incidence and service availability in the United States. Perspectives on Sexual and Reproductive Health 51(1): 17-27.
- Starrs A, Alex CE, Gary Barker, Alaka Basu, Jane TB, et al. (2018) Accelerate progress-sexual and reproductive health and rights for all, The Lancet 391(10140): 2642-2692.
- Erdman J, Cook R (2020) Decriminalization of abortion: a human rights imperative, Best Practice & Research Clinical Obstetrics and Gynaecology 62: 3-12.
- Henshaw H, Kost J (2008) Abortion patients in the United States: characteristics and contraceptive use. Family Planning Perspectives 40(4): 180-188.
- Sarstedt R, Ringle C, Hair J (2017) Partial least squares structural equation modeling. Handbook of Market Research p: 1-40.






























