Morphometric Approach to the Study of Morphogenesis of a Neuroleptic Cardiomyopathy
Volkov VP*
Tver Center of Judicial Examinations, Russia
Submission: February 22, 2018; Published: March 09, 2018
*Corresponding author: Volkov VP, Tver Center of Judicial Examinations, Russia, Tel: 7-903-800-11-05; Email:
How to cite this article: Volkov VP. Morphometric Approach to the Study of Morphogenesis of a Neuroleptic Cardiomyopathy. Glob J Add & Rehab Med. 2018; 5(2): 555658. DOI 10.19080/GJARM.2018.05.555658
Abstract
Aim: In is a comparative morphometric study of myocardium in each clinical stage of neuroleptic cardiomyopathy.
Methods: Myocardium was histomorphometrically examined in 58 cases of neuroleptic cardiomyopathy and in 22 control persons without cardiac pathology.
Result: The studied micromorphometric parameters describe the condition of three structural components of myocardium (vasculature, intercellular matrix, and parenchyma). In the latent stage the microcirculatory disorders prevail. In the full-scale stage the damages of intercellular matrix come to the forefront. For the terminal stage the atrophic and dystrophic-degenerative changes of cardiomyocytes are characteristic.
Conclusion: In the course of morphogenesis of a neuroleptic cardiomyopathy a certain staging of clinical manifestations of the disease is observed; this staging corresponds to an observed chain of interconnected pathologic shifts in all microstructures of myocardium.
Keywords: Neuroleptic cardiomyopathy; Morphogenesis; Structural changes of myocardium; Morphometric research
Abbreviations: NCMP: Neuroleptic cardiomyopathy; CCF: Chronic Cardiac Failure; RN: Relative Norm; ZPD: Zone of Pericapillary Diffusion; KI: Kernogan Index; CMCs: Cardiomyocytes; SVHC: Specific Volumes of Hypertrophied CMCs
Introduction
Neuroleptic cardiomyopathy (NCMP) is one of serious complications of antipsychotic therapy and is caused by side cardiotoxicity of antipsychotic drugs [1-5]. NCMP belongs to secondary specific metabolic dilated cardiomyopathies [6,7]. The disease is characterized by diffusion damage of a myocardium, sharp decrease in its contractile function and as a result the progressing congestive chronic cardiac failure (CCF)) [8,9].
NCMP passes through 3 stages in its development:
a) A latent one, clinically fully compensated one,
b) A full-scale one, when cardiac disorders are clearly detected, but without evident signs of CCF, and
c) A terminal one, when the clinical picture of CCF comes to the foreground [6].
As you know all changes of function of some or other organs, especially the heart are initially caused by it structural changes which are a physical substrate of pathophysiological shifts and reflect the morphogenesis of pathology [10]. But until now, a deep comparative morphological study of heart condition in each clinical stage of NCMP has not been performed. The aim of the present study is to eliminate - at least, partially - the existing gap.
Material and Methods
Myocardium was histomorphometrically examined in 58 cases of NCMP. The dead persons are in the age from 16 to 77 years. In 24 of dead patients the disease was in the latent stage (group II), in 13 patients it was in the full-scale stage (group III) , and in 21 patients it was in the terminal stage (group IV). As a control, we studied the myocardium of 22 persons in the age from 18 to 82 years who died from non cardiac causes and who did not have any accompanying cardiac pathology and this fact was verified by autopsy (group I). The cardiac parameters, which were received in this group, are taken as a relative norm (RN).
Respective objects were studied in 10 different fields of microscope, with necessary magnifications with the help of an ocular micrometer, the point count method was also used [11,12]. Such parameters as zone of pericapillary diffusion (ZPD), Kernogan index (KI), SPR, RIE were calculated. Karyometry and cytometry of cardiomyocytes (CMCs) were performed, the specific volumes of hypertrophied CMCs (SVHC), of atrophied ones (SVAC), and - by the method of polarization microscopy - the specific volume of dystrophic ones (SVDC) were determined. The above-named parameters describe a condition of three structural components of myocardium: of microvasculature (ZPD and KI), stroma (SPR and RIE) and parenchyma (SVHC, SVAC and SVDC). The received results were statistically processed (by the nonparametric Mann- Whitney's U-criterion) with significance level of distinctions 95% and more (p≤0.05).
Results
A comparison of parameters of myocardium microstructure in the groups, which were studied and monitored, among themselves reveals definite regularities (Table 1). First of all, a considerable and statistically significant difference of all parameters, which were calculated in the case of NCMP, from the same parameters in the case of RN is observed. On the other hand, the parameters, which describe conditions of some or other morphologic structures of myocardium in various stages of NCMP, behave differently. For example, parameters, which describe the microvasculature, do not practically change throughout the whole disease. A certain observed growth of their values statistically remains on the level of a tendency. On the contrary, parameters of intercellular matrix of myocardium in the full-scale and terminal stages of NCMP (groups III and IV) statistically significantly differ not only from RN, but also from these parameters in the latent stage too. The dynamics of changes of CMCs is distinctive too. For example, such parameter as SVHC is the highest in the group II and it subsequently declines and reaches the level of RN in the group IV. As to the values of SVAC and SVDC, they steadily grow in the course of NCMP development and considerably differ in each subsequent group of monitoring from these values in the preceding ones.
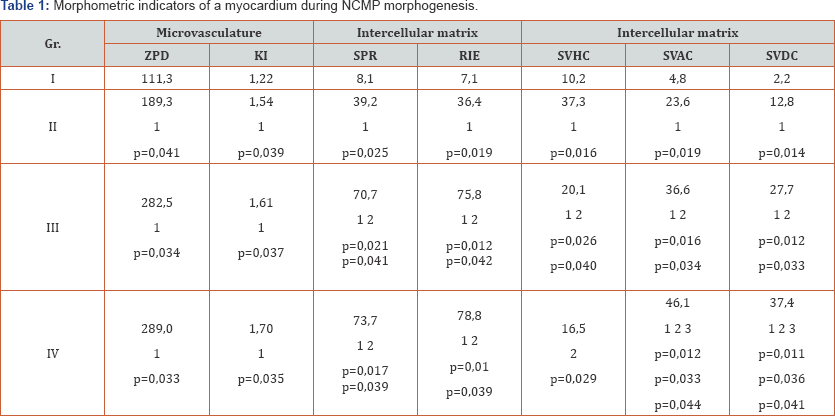
Note 1: statistically significant distinctions with gr. I.
Note 2: statistically significant distinctions with gr. II.
Note 3: statistically significant distinctions with gr.
Discussion
The myocardium microstructure changes in various stages of NCMP morphogenesis are corresponding to the clinical stages of the disease course. In the latent stage of NCMP (group II), first of all, disorders of microcirculation are detected, and this is reflected by growth of the values of ZPD and KI. Vascular changes cause considerable pathologic shifts in intercellular matrix of myocardium which manifest themselves through an increase of an interstitial edema and through development of myofibrosis (growing values of RIE and SPR correspondingly). The result of the described pathologic processes is damages of CMCs, these damages initially have a compensatory-adaptive character in the form of a cellular hypertrophy [13,14]. Atrophic and dystrophic-degenerative parenchymatous changes are observed to a lesser degree. In the full-scale stage (group III) the evidence of pathologic processes in intercellular matrix of cardiac muscle considerably grows - an interstitial edema, that becomes chronic, as well myofibrosis and small-focal (substitutive) cardio sclerosis. Parameters, which describe the condition of microvasculature, do not statistically differ from the ones in the latent stage of NCMP (group II).
Amount of hypertrophied CMCs considerably decreases, although it remains significantly higher than RN. At the same time, dystrophic and atrophic processes, which take place in CMCs, statistically reliably intensify, and these processes are reflected by statistically significant growth of such parameters as SVDC and SVAC. Thus, in the full-scale stage of NCMP the vascular disorders do not play the deciding part in the process of disease morphogenesis on the tissue and cellular levels any more, and the main significance is gained by stromal changes which are initially caused exactly by a pathology of microcirculation and which lead to a considerable imbalance of CMCs' fractions. As the result of the above-said, a further growth of pathologic shifts in myocardium parenchyma take place and the disease passes to the terminal stage (group IV).
In this period the fraction of hypertrophied CMCs continues to decrease and statistically returns to the level of RN. Atrophic and dystrophic-degenerative changes of CMCs distinctly increase and come to the forefront (statistically significant growth of SVAC and SVDC as compared with the group III). These processes are considered as an indisputable indicator of a progressive myocardial dysfunction [13,14]. Values of other parameters of myocardium microstructure fluctuate on the level of a tendency; their differences from a preceding group of research are statistically insignificant. These data are evidence that in the terminal stage of NCMP the atrophy and dystrophy of parenchyma have the main significance, which are an outcome of pathologic processes having earlier taken place in microvasculature and in extracellular matrix of myocardium. The above-named parenchymatous changes form a physical basis of a final myocardial dysfunction which clinically manifests itself through the development of a fatal CCF.
Thus, a chain of pathologic processes, which develop in heart on the tissue and cellular organizational levels in the course of NCMP morphogenesis, is a distinctive quasi relay-race of structural changes of myocardium. In the initial phase (latent stage), microcirculatory disorders are leaders. Then (in the full- scale stage) the damages of intercellular matrix in the form of the interstitial edema and cardio sclerosis join in and come to the forefront. In the final phase of the disease (terminal stage), the atrophic and dystrophic-degenerative changes of CMCs prevail.
Conclusion
The conducted research has proved that in the course of NCMP morphogenesis not only a certain staging of clinical manifestations of the disease is observed, but also a chain of interconnected and interdependent pathologic shifts in all myocardium structures, which corresponds to this staging - shifts in microvasculature, stroma and parenchyma. In addition, in the latent stage of the disease the microcirculatory disorders have the deciding significance in the progression of the pathology; subsequently, they gradually lead to stromal changes and through them to damages of CMCs. In the full-scale stage of NCMP the vascular processes go to the sidelines, and the pathologic shifts in intercellular matrix gain the leading role. In addition, at the same time the damages of parenchyma increase and their compensatory-adaptive character (hypertrophy of CMCs) is replaced by predominance of atrophic and dystrophic- degenerative cellular changes. In the terminal stage the key pathogenetic factors are atrophy and dystrophy of myocardium parenchyma. They are a physical basis for development of a severe CCF and they proceed against the background of earlier changes of microvasculature and stroma of cardiac muscle.
References
- Volkov VP (2010) Cardiotoxicity of phenothiazine neuroleptics. Psichiat psychopharmacother 12(2): 41-45.
- Volkov VP (2009) Phenothiazine dilated cardiomyopathy: Some aspects of clinic and morphology. Clin Med 8: 13-16.
- Buckley NA, Sanders P (2000) Cardiovascular adverse effects of antipsychotic drugs. Drug Saf 23: 215-228.
- Coulter DM, Bate A, Meyboom RHB (2001) Antipsychotic drugs and heart muscle disorder in international pharmacovigilance: Data mining study. Br Med J 322: 1207-1209.
- Mackin P (2008) Cardiac side effects of psychiatric drugs. Hum Psychopharmacol 23(1): 3-14.
- Volkov VP (2013) Clinical characteristic of an antipsychotic cardiomyopathy. In Volkov VP (Edn.) Actual problems of therapeutic clinic: collective scientific monograph. Novosibirsk: SibAC, Russia, pp. 94-116.
- Tereshchenko SN, Jaiani NA (2001) Dilated cardiomyopathy today. Heart failure 3(2): 58-60.
- Volkov VP (2011) To a question of a secondary phenothiazine cardiomyopathy. Clin Med 5: 30-3.
- Volkov VP (2011) Features of the electrocardiogram at a phenothiazine cardiomyopathy. Clin Med 4: 27-30.
- Sarkisov DS, Paltsev MA, Hitrov NK (1995) General pathology of the person. Medicine Publ, Moscow, Russia.
- Avtandilov GG (1990) Medical morphometry: Management. Medicine Publ, Moscow, Russia.
- Avtandilov GG (2002) Fundamentals of quantitative pathological anatomy. Medicine Publ, Moscow, Russia.
- Amosova EN (1999) Cardiomyopathies. Book plus Publ, Kiev, Europe.
- Shumakov VI, Hubutiya M, Ilyinsky IM (2003) Dilated cardiomyopathy. Triad Publ, Tver, Russia.






























