A Conceptual Model for Treating Alcohol and Other Drug Disorders
Patrick McKiernan*
Professor of Psychology, Behavioral Sciences Department, California Southern University, USA
Submission: February 01, 2018; Published: March 05, 2018
*Corresponding author: Patrick McKiernan, Professor of Psychology, Behavioral Sciences Department, California Southern University, USA, Tel: 502-439-9210; Email: patrickmckiernan@att.net
How to cite this article: Patrick McKiernan. A Conceptual Model for Treating Alcohol and Other Drug Disorders. Glob J Add & Rehab Med. 2018; 5(2): 555657. DOI: 10.19080/GJARM.2018.05.555657.
Short Communication
The National Institute of Drug Abuse is a leader in the field of alcohol and other drug treatment regarding the effects drugs have on the human brain. Notably this Federal Agency has dedicated entire training modules to educate the public on how drugs impact the brain. Significant effects include but are not limited to cerebral cortex and limbic regions areas responsible for cognition, problem solving, memory, emotional processing, and rewards [1]. These two areas represent significant areas of function necessary to healthy functioning and of equal importance active participation in treatment for substance use disorder. NIDA's research indicates that the lasting effective or impairment to the brain can take up to 12 months before normal functioning is restored. That merits repeating it can take up to 12 months to achieve normal brain function. Lewis [2] found that grey matter returns to its normal baseline level after six months to a year of abstinence. The prefrontal cortex has a key role in cognitive functions involved in decision-making, including, but not limited to, memory, attention, emotion, working memory, outcome expectation, and planning. Impairment of decisionmaking is a key feature of addiction [3]. Why is this important? Because relapse rates at 12 months follow up are as high as 58% [4].
In short, we have a population that is relapse prone due to a range of factors that center on a brain that is impaired to repeated exposure to toxic substances. The human brain has the ability to heal and return to normal functioning given sufficient time and support. The image below represents conceptually our traditional approach. While not all programs follow this design, it is representative of what is referred to as treatment as usual. Take note of the general flow of services and how most are offered during the time when the brain is experiencing great impairment (Figure 1).

Conceptual Image of the traditional treatment design
The next image provides a conceptual image of how treatment could be delivered. This approach accounts for the noted prefrontal cortex malfunction and reduces expectation for higher level functions. Rather the focus is on support, simple routines, and developing coping skills. In this model the client could reside in a low-cost recovery house or if the environment was supported stay at home. The focus would be on engaging in social support networks (making non-substance using friends), developing skills to improve coping such as discussing difficulties with everyday challenges, and employment. As the brain heals so then would the level of intervention. Lawson et al. [5] found that 96.5% of those with alcohol or other drug disorders experience at least one traumatic event in their lifetime. While everyone may not require therapy the ability to benefit from therapy improves with greater stability and improved mental function. The ability to focus on resolving the issue would increase and the possibility that the trauma will trigger a relapse would like decrease (Figure 2).
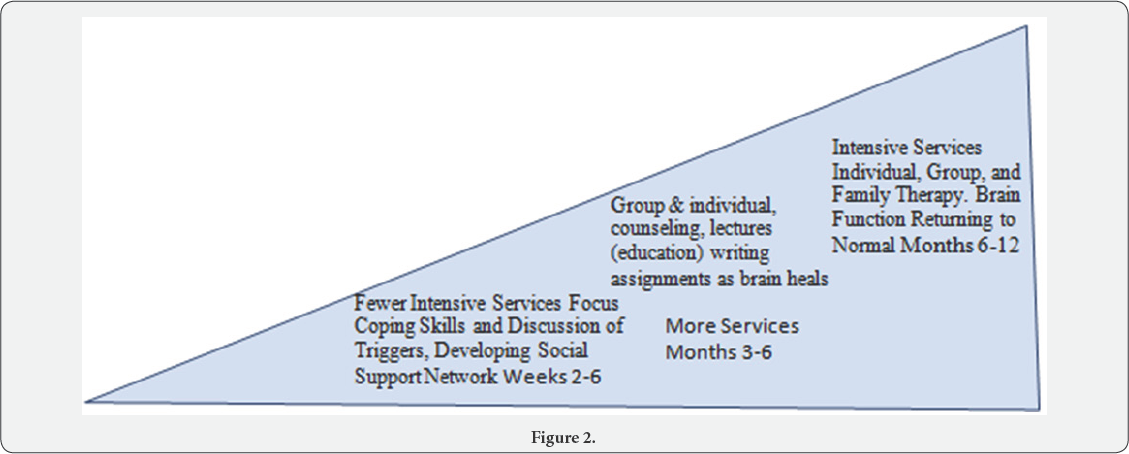
Conclusion
This is meant to provide a conceptual framework for rethinking the approach to treatment of substance use disorder. NIDA [6] suggests that treatment lasting less than 90 days is less effective and that longer treatment stays in residential or outpatient programs produce better outcomes. Rethinking the approach also falls in line with Recovery Oriented Systems of Care which advocates moving from the acute treatment model to the chronic care model [7].
References
- NIDA (2014) Drugs, Brains, and Behavior: The Science of Addiction.
- Lewis MD (2015) The biology of desire: Why addiction is not a disease. Public Affairs, New York, USA.
- George O, Koob GF (2010) Individual Differences in Prefrontal Cortex Function and the Transition from Drug Use to Drug Dependence. Neuroscience and Bio behavioral Reviews 35(2): 232247.
- Blum K, Schoenthaler SJ, Oscar Berman M, Giordano J, Madigan MA, et al. (2014) Drug abuse relapse rates linked to level of education: Can we repair hypodopaminergic-induced cognitive decline with nutrient therapy? Phys Sports med 42(2): 130-145.
- Lawson KM, Back SE, Hartwell KJ, Maria MMS, Brady KT (2013) A Comparison of Trauma Profiles among Individuals with Prescription Opioid, Nicotine or Cocaine Dependence. The American Journal on Addictions / American Academy of Psychiatrists in Alcoholism and Addictions 22(2): 127-131.
- (2018) National Institute on Drug Abuse; National Institutes of Health; US Department of Health and Human Services. Principles of Effective Drug Treatment. A Research-Based Guide (3ri edn).
- White WL (2008) Recovery Management and Recovery-oriented Systems of Care: Scientific Rationale and Promising Practices.






























