Attachment Issues in Cancer patients Co-morbid to Addiction: Intervention based Case study
Guru Prasanna Lakshmi*
Department of Clinical Psychology, Sweekaar Academy of Rehabilitation Sciences, India
Submission: September 18, 2017; Published: September 26, 2017
*Corresponding author: Guru Prasanna Lakshmi, Department of Clinical Psychology, Sweekaar Academy of Rehabilitation Sciences, India, Tel: 9515690010; Email: guru.psychologist@gmail.com
How to cite this article: Guru P L. Attachment Issues in Cancer patients Co-morbid to Addiction: Intervention based Case study. Glob J Add & Rehab Med.005 2017; 4(1): 555629.DOI:10.19080/GJARM.2017.04.555629
Abstratct
The use of substances that alter mood, behavior and cognitions have been a part of human life across numerous social contexts throughout the history. Invariably, there are some individuals whose use of such substances may lead to abuse and eventual Psychological, Social, or Physical harm [1]. Tobacco is used in India in many forms. Smoking of Cigarettes and Beedis (Tobacco wrapped in dried leaves of special trees) is one form of tobacco use. Smokeless tobacco use consists of chewing pan (mixture of lime, pieces of areca nut, tobacco and spices wrapped in betel leaf), chewing gutkha or pan masala (scented tobacco mixed with lime and areca nut, in powder form), and mishri (a kind of toothpaste used for rubbing on gums) [2]. Using data from the National Family Health Survey second round (NFHS II, 1998-99), prevalence of tobacco use in India was estimated to be 37 percent among the population of 15 years and above [3].
This article discusses how the addicted behavior lead to isolation of an individual in all the aspects and through intervention could enhance the quality of life by improving interpersonal relationship. Pre and Post assessments were used by administering distress thermometer with questionnaire, Quality of marital life scale, Hamilton Depression rating scale and the results on pre intervention stage - Distress thermometer (10 - extreme distress) and screening tool scores (18), On HDRS, the patient score was 19 which shows significant with moderate level of depression, Quality of Marital Life scale - Score 179 indicates the higher distress in marital life. On post intervention the scores were found to be non significant in all the assessments, which showed beneficial of using integrated approach.
Keywords: Attachment issues; Cancer; Gutkha Addiction
Introduction
It may seem strange but the substance dependence is in itself a recognized psychiatric illness. Research studies are looking in to the mental health illness leading to addiction and the addiction leading to psychiatric and physical morbidity vice versa. According to the review of research for the factors involved in addiction behavior has been discussed rigorously and still it is going on. Addiction has been considered as a disease condition with lots of co morbidities in the physical, psychological and social scenarios. Tobacco use is determined and influenced by several kinds of factors:
a. Individual factors (perceptions, self-image, peers);
b. Social factors (societal norms);
c. Environmental factors, such as advertising and economics; and
d. Cultural factors, such as traditional uses of tobacco, acculturation, and the historical context of the tobacco industry in various communities.
The term "smokeless tobacco" refers to the consumption of unburned tobacco, in the form of chewing, spitting, dipping, and snuff. Consumers chew the tobacco in the mouth and spit out the juice that builds up. Nicotine and other constituents are absorbed in the lining of oral cavity [4]. People of many regions, including India, Pakistan, other Asian countries, and North America, have a long history of smokeless tobacco use. Approximately 28 chemical constituents present in smokeless tobacco are carcinogenic in nature, among which nitrosamine is the most prominent [5]. Gutkha is sweet in taste, and children consider it to be a form of candy. Many people believe that gutkha is a mouth freshener, but its pleasant taste and sweetness aggregate microbes, causing damage to teeth. The use of paan and gutkha is difficult to control in most countries where it is widespread, and their extensive use leads to oral cancer [6]. The use of gutkha has been shown to have genotoxic and clastogenic properties [5].
Biological factors
Areca nut has been classified as a known human carcinogen by the International Agency for Research on Cancer [7] the development of various cancers in gutkha chewer due to genotoxic effect of chemical present in gutkha as N-nitrosamines eugenol, sodium carbonate, ammonia, ammonium carbonate [8-10]. Human susceptibility to cancers caused by tobacco carcinogens is determined by genes involved in metabolism of carcinogens and repair of damaged DNA. In a study on polymorphism at GST gene loci, Buch et al., reported that the GST M1 null genotype is a major risk factor for the development of oral cancer among tobacco chewers [11].
Social factors
Initiation of gutka use: Most participants initiated gutka/ tambaku paan in their adolescent years (14-17 years), some initiated as young adults (22-26 years), while a handful initiated as adults (40-45 years) [12]. The initiation may be due to some of its perceived symptoms, like relieves from boredom, reduces stress, gives relaxation and also increases alertness. These things were expressed by the gutka users. Some people expressed as a form of curiosity, initiation was taken place. Some of them influenced by the peer group and so on. The reasons for the initiation were varied, but one of the factor could be easily available and the society acceptance.
Psychological factors
There are also numerous studies in the literature that have focused on other approaches. There is strong evidence of an association between tobacco consumption and a personality factor characterized as the need to experience stimulating sensations (sensation seeking) [13]. The sensation seeking dimension can be defined as the 'search for new, varied, complex and intense sensations and experiences, together with the predisposition to take physical, social, legal, and financial risks in order to have such experiences' [14]. The existence of the sensation seeking dimension is also substantiated by biological findings. Individuals with high scores in this factor present low levels of cortical stimulation [15]. There seems to be a strong association between the sensation seeking factor and traits of impulsivity. The definition of impulsivity incorporates elements such as the tendency to get into situations or rapidly respond to stimuli for potential reinforcement, without much planning and without considering the potential risks of punishment or loss of gratification. The impulsivity factor can be considered a deficit in the capacity of inhibiting dangerous behaviors, seeking gratification [13].
Method
A. Participant's information
Patient M was a 37 years old, male, Muslim, married Completed Polytechnic and working as a mechanic, hails from Suburban, Middle socio economic strata. Presented with the chief complaints of severe pain in localized area even after medication dose, sleep decreased, appetite decreased, Crying spells since 15 days increased with overall duration of 11/2 year. Patient is under Morphin dose of 60mg which was increased from 30 to 60 mg prior to 20 days due to his symptoms and pain. At present during Home visit patient was so desperate for the change of medications or the increase of dose. Food intake decreased drastically since 2 days due to pain. Sleep was limited to 2- 3 hours and most of the crying (sibling observation) and not responding to others even after calling.
According to the history of presenting illness, patient was a habitant of tobacco when he was in Polytechnic studies and gradually become dependent i.e increase of sachets intake been increased from 5 to 25. All the time used to involve in chewing and only the sleeping time was a period where he would rest his mouth. He also reported of alcohol consumption once in a month during (Daawath) parties. He says that "the pleasure he gets by chewing will not be the same by the alcohol so not interested much in that ". He was obedient in home affairs and responsibilities, supportive to the family financially. He learnt to manage in fulfilling the roles and responsibilities since after his father death. He got married at the age of 24 years of age, with a intimate relationship of 5 years thereafter slowly spouse used to have a frequent visits to her mother's house. On inquiry with the spouse she said that "he smells a lot and all the time in anger mood, scolds for no reason most of the times." " I asked him to stop taking tobacco so many times and he raises his voice which leads to a fight between us and I would leave to my mother's home in helpless condition." after 10 days of every fight he comes to there or calls my mother to send back to here.
11/2 year back he was having severe pain in the Right Lower Jaw, so then consulted a doctor and on further reference visited to cancer hospital. Doctor reported a small lump, and asked us to go for a biopsy for diagnosis and treatment. Biopsy report revealed that Right side Buccal mucosa IInd grade asked us to go for Radiation therapy for 24 - 26 sessions i.e 5 days a week. Due to the adversive effects like nausea, vomiting, sleeping difficulties and also doctors asked to stop the tobacco intake thus the patient used to be irregular to the treatment. Spouse reported even during treatment he was not abstinent from tobacco. After 10 months doctors informed that his tumor cannot be treated, due to irregular compliance to the treatment (he stopped taking RT after 6th session) and the continuous usage of tobacco (10 - 15 sachets per day), and he was shifted to Palliative care department. Since 8 months he is under pain medication started Morphin with 20 mg but gradually dose had been increasing. He is regular in medication intake and for doctor consultations. Recently since 1 month stating that the medications were not working for him, and need a medication to be changed or dose has to increase during home visits.
Measures
Distress Thermometer and Screening Tool
Distress screening is a comprehensive process that achieves the quality care standard of whole-patient care, which is the integration of both psychosocial and biomedical cancer care. The NCCN recommends using the validated Distress Thermometer (NCCN-DT), a visual analogue scale that allows patients to rate their perceived level of distress in the last 7 days on a scale of 0 ("no distress") to 10 ("extreme distress"). Patients clarify the source of distress using a 39-item problem list with 5 categories: practical, family, emotional, spiritual/ religious, and physical. A score of 4 or greater has been established as the cutoff point for providers to further assess identified patients and their need for treatment.
Quality of marital life scale (QOL)
This scale consists of 50 items, 4- point likert scale measures the severity/frequency of important aspects of the marital relationships on the following areas, Support, Openness, Intimacy, Connectedness , Autonomy, Empathy, Love, Dominance and Conflict. The scoring has two dimensions i. e some questions were mentioned as positively worded items and some of the questions were scored reverse which were mentioned as negatively worded items [16].
Hamilton Depression rating scale (HDRS)
The HDRS (also known as the Ham-D) is the most widely used clinician-administered depression assessment scale. The original version contains 17 items (HDRS17) pertaining to symptoms of depression experienced over the past week. Although the scale was designed for completion after an unstructured clinical interview, there are now semi-structured interview guides available. The HDRS was originally developed for hospital inpatients, thus the emphasis on melancholic and physical symptoms of depression.
Design
A single case experimental design with pre- and postassessment was used, to evaluate the changes in the patient in response to the intervention.
A. Procedure: The pre-assessment (i.e., pre intervention) was carried out following the presenting symptoms, history and clinical observation. Based on the assessment profile and considering her goals to be focused an integrative intervention approach was developed to address distress in marital life and improve quality of life. The program consisted of sessions held 2 times a week during beginning and continued for once in a week on followed sessions for a period of 2 months, each session lasting on an average for 45 minutes. A total of 10 sessions were conducted in the hospital setting on an out-patient basis. During this period, the patient and the family were also psycho educated and counseled. The completion of the program was followed by a post-assessment (i.e post- intervention).
Results
a) Distress Thermometer score (10 - extreme distress) and screening tool scores (18) were significant with problems mentioned in the areas of emotional, physical, and financial aspects.
b) Hamilton Depression rating scale (HDRS) - On administering HDRS, the patient score was significant i.e 19 indicating moderate level of depression.
c) Quality Of Marital Life Scale (QOL) - Score 179 indicates the higher distress in marital life.
A. Therapeutic Techniques
a. Conceptualization and treatment plan: Treatment was scheduled for 10 - 12 sessions. Therapy is focused on how to cope up with the stress related to his health and to regularize his daily activities.
b. Psycho-education: Family members were made to understand the cause for the symptoms, what exactly happens with the patient, targeting stigma related issues, Prevalence rate about the condition, person's ability to recover, the suffering and problems can be reduced with treatment, importance of therapy compliance.
c. Cognitive Behavioral Therapy (CBT): Cognitive- behavioral therapy is based on the interrelationship of thoughts, actions, and feelings. In order to work with feelings of depression, this model establishes the importance of identifying the thoughts and actions that influence mood. In this manner the person learns to gain control of his/her feelings [17].
d. Couple Therapy is to focus on encouraging positive sentiment over ride and to improve effective communication skills. To help partners negotiate behavior change.
e. Supportive Psychotherapy: Supportive expressive therapy is applicable to those patients with chronic illness. Supportive psychotherapy is a dyadic treatment that uses direct measures to ameliorate symptoms and maintain, restore, or improve self-esteem, ego function, and adaptive skills
f. JPMR (Jacobson's progressive muscular relaxation technique): Relaxation can help to relieve the symptoms of stress. Although the cause of the anxiety will not disappear, but probably feel more able to deal with it, once one have released the tension in body and cleared the thoughts. Jacobson's progressive muscular relaxation technique involves contracting and relaxing the muscles to make person feel calmer. It is a skill that needs to be learned and it will come with practice. Once one have mastered it will be able to use it throughout one's life.
g. Content of the Intervention :
I. Session -1: Patient was discussed about Psychological assessments results, distress was addressed. All the family members and the patient was Psycho educated by providing factual information about the disease and also the condition in which the patient is undergoing. The emotional status and the maladaptive coping which is making him to feel distress. Acknowledged their emotional aspects, understanding their perspective, Appreciated for being supportive and Empathetic.Patient was explained about the advantages of JPMR and Ist Session of JPMR was given. Feedback was taken to know his feeling about the session.
II. Session - 2: CBT model was explained by taking practical examples in schematic way, how the thoughts and beliefs lead to inferences and dysfunctional assumptions, with all these emotional distress as a consequence (Figure 1). The patient was allowed to ventilate and was given Reassurance, Encouraging positive behaviors asked him to identify the cognitions. By engaging in useful tasks to improve problem solving and judgmental abilities. The 2nd Session of JPMR training was given; the patient was seeking assurance for the health, acknowledged his emotions.
III. Session - 3: Patient was discussed about the importance of the medicines and the adequate diet. He was reinforced with CBT model and was allowed for catharsis. During this time patient expressed his emotions and concerns. 3rd session of JPMR training was given, and was asked to list out the positive things in him.
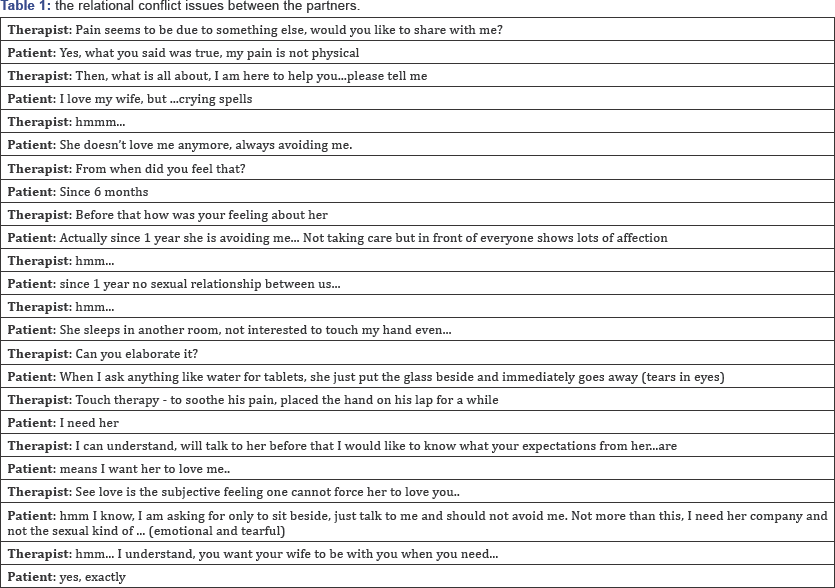
a. Emotional focused Couple therapy: Cycle Deescalation: In this step the main goal was to identify the relational conflict issues between the partners (Table 1).

IV. Session - 4: Patient was seems to be stable and was seeking reassurance. In this session patients wife was asked to speak about her understanding of the disease and also her concerns. During the conversation, she expressed about the stigma related to the disease, i.e., could be inflammatory and may affect her by touch, and hence she is avoiding him. Her misconceptions were discussed giving practical examples and evidences. She was also discussed about her concerns, being empathetic towards her, appreciated for the efforts she is making. She also shared her emotional burden i.e., anticipatory thoughts about her spouse disease condition. She underwent catharsis...
V. Session - 5: In this session patient and his spouse were dealt with the techniques like -Reflection, evocative questions and heightening. In which therapist first revealed the expectations of both on one another. Patient got angry and said - I am her husband and she has to take care of me which she does not understand. Spouse of the patient : I am also a human being , I too have a feelings , intimate relationship will not develop on sudden
a. Therapist: I do understand both of your concerns , firstly you two shall understand that please keep a side of role and responsibilities and think about one another by showing empathy , look in to the intention and the emotion involved, then you people can help yourselves.
Patient is asking for the companionship and it can be fulfilled by basic humanity sense. He is asking only you because your presence makes him feel secured. As I said earlier you are supporting him very well he has a trust on you.
b. Spouse of the patient: hmm, ok madam what should I do ?
c. Patient : Smile
a. Therapist: I will only guide you, ultimately you both has to decide yourselves.
b. Patient : Ok madam
a. Therapist: You also should understand her , the reason behind her behaviour rather being judgmental Distress Thermometer was used to see his distress level and the score (6 - moderate distress)
VI. Session - 6: Cognitive Therapy: Cognitive distortions were explained, Judgmental, Magnification and minimization, Absolutist, dichotomous thinking. Cognitive Triad was discussed, how depressed thinking makes person to view negative towards self and world and future.
VII. Session - 7 & 8: Communication skills: Be specific in understanding before generalizing it globally like I am not happy, you are responsible and step back to know what does it look like? And what causes the discomfort? Expressing Positive Feelings typically goes better if the praise is offered for a relatively specific behavior instead of a generic attribute such as being a "terrific person" Be flexible in resolution of problems between individuals requires give and take. Although a plan to resolve the problems may have been developed before the actual discussion began, it is important to consider others' ideas before selecting a solution.
VIII. Session - 9 & 10: Patient was stable with the practice of tasks given and also by change of his perception. Spouse of the patient was cooperating towards therapy, Morphine dose was came down to 30mg and he is managing well with good sleep but the diet intake was not improved, so the spouse was asked to soften the food and give and the patient was asked maintain a good oral care.
a. Cognitive Restructuring: Influencing his mood, by changing what is under control was discussed by depression and the healthy management reality. Explained about the concepts of Objective world and Subjective world and no one controls either of these 2 worlds completely, but however we can learn how to gain more control over them. When any individual feel depressed , at that situation feels have no control so to overcome that need to understand the ways to gain more control:
i. Altering Objective world with : Activities , Social contacts , Assertive communication
ii. Altering Subjective world with : More healthy / helpful thinking , Less unhealthy / harmful thinking
b. Chunks of time: This technique was explained to engage in the pleasant activities which makes he to feel less distress and helps oneself to become emotionally healthier. Thus better you feel, the more you do for yourself and others.
IX. Session - 11: Patient was coping well with being emotionally stable, post assessment was done.
a. Post assessment Results:
i. Distress Thermometer score (2 - mild distress) and screening tool scores (9) were in significant in psychological and family but due to medical condition distress level is found to be mild in Physical aspect.
ii. Hamilton Depression rating scale (HDRS) - On administering HDRS, the patient score was significant i.e 7 indicating insignificant.
iii. Quality Of Marital Life Scale (QOL) - Score 63 indicates satisfactory in marital life.
Discussion
The present study examined a correlation between the attachment issues and the coping mechanism which helps in improving quality of life. Holistic approach of treating a patient suffering with cancer secondary to addiction, who is under double effect will have problems in physical, psychological and social aspects and giving only medication is not the solution. Cancer is a life threatening disease. Its psychological impact on patients has been an important aspect for health professional involved in the treatment process. The diagnosis itself and subsequent treatment of cancer can be emotionally distressing. It is still considered synonymous with death, pain and suffering [18].
Emotional distress is a multi factorial unpleasant experience of emotional, cognitive, behavioral & spiritual nature that interfere the ability to cope effectively with cancer. It extends in continuum ranging from common normal feeling of vulnerability, sadness and fear to problems that can become disabling anxiety, panic, social isolation and depression [15]. Early recognition of the emotional requirements by the Oncologist or the health professional involved in the treatment process not only decrease the cost burden of cancer treatment but at the same time improve quality of life [18].
The psychological need of the person varies at different stages of Cancer, Anxiety, Depression and severe level of distress which will decline their quality of life. During the beginning stages of diagnosis, patient may be in denial but as the disease gets progress and in helpless condition he will reach to the level of acceptance and the definition of needs changes drastically. Learns to satisfy with minimal and basic things where he marginalizes to short term. The present case dealt the same, where the patient intention was to get least attention from loved ones, but the treatment was concentrated only on physical aspects, thus his quality of life was deteriorated. Therapy made him satisfied and made him realize how to cope up with the stressful situations. Even though he is not going to survive for longer period but whatever the days he will spend with good amount of quality of life.
Conclusion
Our study findings indicated that the need of assessing the psychiatric morbidity by understanding the perpetuating factors. By the holistic approach one can minimize the emotional distress which enhances the medical compliance. Therapy was intended to add the life to the days rather days to the life.
References
- Robin J Davidson (1998) The Treatment of Substance Abuse and Dependence.
- Akansha Singh, Laishram Ladusingh (2014) Prevalence and Determinants of Tobacco Use in India: Evidence from Recent Global Adult Tobacco Survey Data.
- Rani M, Bonu S, Jha P, Nguyen SN, Jamjoum L (2003) Tobacco use in India: Prevalence and predictors of smoking and chewing in a national cross sectional household survey. Tob Control 12: e4.
- Kamal Niaz (2017) Smokeless tobacco (paan and gutkha) consumption, prevalence, and contribution to oral cancer. Epidemiol Health 39: e2017009.
- Banerjee SC, Ostroff JS, Bari S, D'Agostino TA, Khera M, et al. (2014) Gutka and Tambaku Paan use among South Asian immigrants: a focus group study. J Immigr Minor Health 16: 531- 539.
- Shah G, Chaturvedi P, Vaishampayan S (2012) Arecanut as an emerging etiology of oral cancers in India. Indian J Med Paediatr Oncol 33: 71-79.
- (2004) International Agency for Research on Cancer. Betel-quid and areca-nut chewing and some areca-nut derived nitrosamines. IARC Monogr Eval Carcinog Risks Hum 85:1-334.
- Chang YC, Yang SF, Tai KW, Chou MY, Hsieh YS (2002) Increased tissue inhibitor of metalloproteinase-1 expression and inhibition of gelatinase A activity in buccal mucosal fibroblasts by arecoline as possible mechanisms for oral submucous fibrosis. Oral Oncology 38: 195- 200.
- Das RK, Dash BC (1992) Genotoxicity of 'gudakhu', a tobacco preparation. II. In habitual users. Food and Chemical Toxicology 30: 1045-1049.
- Dave BJ, Trivedi AH, Adhvaryu SG (1992) In vitro genotoxic effects of areca nut extract and arecoline. Journal of Cancer Research and Clinical Oncology 118: 283-28 8.
- Bhisey RA (2014) on Saturday, March 29, 2014, IP: 68.58.206.221.
- Smita C Banerjeeet (2013) J Immigrant Minority Health (2014) 16: 531-539.
- Regina de Cassia Rondina , Ricardo Gorayeb , Clovis Botelho (2007) Psychological characteristics associated with tobacco smoking behavior. J Bras Pneumol 33(5): 592-601.
- Zuckerman M, Kuhlman DM (2000) Personality and risk-taking: common biosocial factors. J Pers 68(6): 999-1029.
- Carton S, Le Houezec J, Lagrue G, Jouvent R (2000) Relationships between sensation seeking and emotional symptomatology during smoking cessation with nicotine patch therapy. Addict Behav 25(5): 653-662.
- Powe BD, Finne R (2003) Cancer fatalism: the state of the science. Cancer Nurs 26: 454-465.
- Carlson L, Bultz B (2003) Cancer distress screening: needs, models and methods. J Psychosom Res 55: 403-409.
- Manjeet Santre (2014) Prevalence of Emotional Distress in Cancer Patients. IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) 13(6): 9-14.






























