Clinical and Sociodemographic Variables Associated With Learning Process Deficits in Crack-Cocaine Abstinent Users
Priscila P Almeida1, Gerardo Maria de Araujo Filho1*, Paulo J Cunha2, Stella M Malta1, Priscila D Gonçalves2, Bernardo dos Santos3, Ana Cecilia RP Marques4, Ronaldo R Laranjeira4, Rodrigo A Bressan1 and Acioly LT Lacerda1
1Department of Psychiatry, Federal University of Sao Paulo (UNIFESP), South America
2Department of Psychiatry (IPq), Faculty of Medicine, University of Sao Paulo (FMUSP), South America
3CEAPPesq, Institute of Mathematics and Statistics (IME), Department of Psychiatry, South America
4Department of Psychiatry, Federal University of Sao Paulo (UNIFESP), South America
Submission: August 04, 2017; Published: August 15, 2017
*Corresponding author: Gerardo M. de Araujo Filho, LiNC - Labóratorio Interdisciplinar de Neurociências Clí'nicas, Rua Pedro de Toledo, 669 - 3° andar - Fundos, São Paulo-SP, Brazil. Tel:04039-032; Email: filho.gerardo@gmail.com
How to cite this article: Priscila P A, Gerardo M d A F, Paulo J C, Stella M M, Priscila D G, et al. Clinical and Sociodemographic Variables Associated With Learning Process Deficits in Crack-Cocaine Abstinent Users. Glob J Add & Rehab Med. 2017; 3(1): 555604. DOI: 10.19080/GJARM.2017.03.555604
Abstract
Background: Assessing decision-making deficits in crack-cocaine dependence is relevant since these impairments have been associated to worse global functioning, lower treatment retention rate and persistence of substance-seeking behavior.
Objective: The present study described the clinical and sociodemographic variables of abstinent patients with crack-cocaine dependence and verified the impact of those factors on a decision-making task performance (Iowa Gambling Test - IGT), compared with matched controls.
Methods: Thirty in patients with crack-cocaine dependence and 30 controls were enrolled in this study. Groups were evaluated through DSM-IV criteria and through neuropsychological tests, including IGT. In patients' group, clinical and sociodemographic variables were correlated with performance on IGT.
Results: Although groups did not differ on IGT total score, analysis involving net scores in blocks of picks during trials showed significant differences in learning processes in patients with crack cocaine dependence. Factors associated with a worse performance on IGT were lower IQ, more depressive symptoms and clinical and social alcohol-related issues.
Conclusion: These findings suggest that learning process deficits in abstinent patients with crack-cocaine dependence would be associated to variables beyond crack-cocaine use itself, highlighting the importance of interventions that consider such issues in treatment programs.
Keywords : Crack-Cocaine; Neuropsychological evaluation;Iowa Gambling Test; Learning process
Introduction
Crack-cocaine dependence is an important public health problem worldwide. In last year's, the global prevalence of cocaine use in developed countries have remained stable at 0.30.4% of the population aged 15-64 (between 13 and 19.5 million users) while in Brazil there was a perceived increase in cocaine use, and particularly through smoking route of administration (crack-cocaine) (United Nations Office on Drug and Crime [1] . Such disorder is characterized as a relapsing brain disease that has been associated, among other clinical and sociodemographic (SD) variables, to changes in the reward system and impaired decision-making and learning functions, such as loss of control over substance use [2]; American Psychiatric Association 1994).
Decision-making refers to the ability of selecting the most adaptive choice among a set of possible actions [3,4]. Studies have observed that subjects with substance dependence could present decision-making and learning difficulties to incorporate negative health and social consequences of their seeking and taking substance behavior [3-5]. Additionally, decision-making deficits have been associated to a worse global functioning and a lower treatment retention rate [6]. Studies have reported decision-making deficits in cocaine dependence subjects using the Iowa Gambling Task (IGT), a paradigm which models real- life decision-making and assesses cognitive (non-planning) impulsiveness [7,8]. Thus, describe the clinical and SD variables, as well as investigate the existence of possible correlated deficits in decision-making and learning processes in patients with crack-cocaine dependence seems to be clinically relevant, since these impairments may contribute to the persistence of the substance-seeking behavior despite a pattern of adverse consequences associated with its misuse.
Although decision-making deficits have been reported in cocaine users, only few studies have examined patients who used the smoking route of administration (crack-cocaine), the possible persistence of those deficits after resolution of withdrawal syndrome and association of such deficits to clinical and SD variables beyond crack-cocaine use. The main aim of the present study was to verify the neuropsychological performance on IGT of four-week abstinent participants with crack-cocaine dependence in order to evaluate their decision-making and learning processes, as well as to disclose the possible association of such deficits to possible clinical and SD variables beyond crack-cocaine use.
Methods
Participants
Thirty patients with crack-cocaine dependence, who were male inpatients of a detoxification hospital unit at Federal University of S�o Paulo, were consecutively recruited through an invitation at the moment of admission from March to November 2015. Although this unity can receive patients for voluntary and/or involuntary detoxification, all participants included accepted to participate the study after a process of informed consent in accordance with the recommendations from the Declaration of Helsinki. As crack-cocaine dependent group was in a controlled environment, they were not submitted to drug screen tests. The control group (n=30), recruited from community through newspaper and internet advertisement, was composed of males without any history of use of psychoactive substance and current diagnosis of Axis I DSM-IV disorders, with the exception of nicotine dependence and low risk alcohol use (no more than 14 drinks per week). All controls were submitted to drug screen analysis. The cocaine dependence group was assessed in early abstinence (between 3 and 10 days of abstinence - mean of 6.1 ± 2.0 days) in order to minimize neuropsychological alterations associated to withdrawal syndrome [9]. After four weeks (one-month abstinence), they were re-assessed using the same neuropsychological battery. The control group was also evaluated at baseline and after four weeks.
Procedure
Participants (cocaine dependence group and controls) were interviewed by a trained professional, using Structured Clinical Interview for DSM IV Disorders (SCID-I) to assess eligibility [10]. Participants were all males, aged 18 to 50 years, and were included if they met DSM-IV criteria for crack-cocaine dependence [11]. Exclusion criteria included current diagnosis of other DSM-IV axis I disorder, with the exception of nicotine abuse and/or dependence and alcohol abuse (but not dependence), due to high rates of alcohol and nicotine abuse comorbidity with cocaine dependence; current use of psychotropic drugs; neurological diseases affecting Central Nervous System; history of head trauma with loss of consciousness; less than four years of education; and intellectual disability (IQ < 70). Exclusion criteria for the control group were the same as for cocaine dependence group.
All participants provided written informed consent approved by local Institutional Review Board. The Short Alcohol Dependence Data (SADD) was used do evaluate problems with alcohol use [12]. Data on frequency, amount, and pattern of use were collected by using the Time Line Follow Back [13]. Socioeconomic status scale was used to assess subject economic level [14]. Annette Handedness Inventory was used to determine subject handedness [15]. Depression symptoms were assessed by using Brazilian version of Beck Depression Inventory (BDI) [16,17].
Neuropsychological assessment
Estimated IQ was assessed by using Vocabulary and Block Design subtests from Wechsler Adult Intelligence Scale (WAIS-III) [18]. WAIS-III was translated and adapted for use in Brazil [19]. Vocabulary is a WAIS III subtest composed of a list of 35 words with increasing difficulty. Subjects need to explain the meaning of words, scoring 2, 1 or 0, according to answer. This subtest is considered a good measure of verbal ability and premorbid intellectual functioning. Block Design subtest is composed of nine cubes with sides colored in red, white and red/white and nine cards with printed figures made of the arrangements of the cubes. Each arrangement card has a time limit and scores vary according to task complexity and how quickly subjects can build the model. This task measures visuo construction ability [20].
The Brazilian version of IGT was used to evaluate impulse control and decision making [21]. Four virtual decks of cards on a computer screen were presented to the participants. It consists of four decks that differ in two ways: (a) the outcome across time, whereas decks A and B are poor long-term choices and decks C and D are advantageous long-term choices; and (b) the frequency of immediate reward and punishment irrespective of longterm outcomes, whereas decks A and C are worse choices due to frequent punishments/infrequent rewards and decks B and D are better and safer choices due to infrequent punishments/ frequent rewards. The objective is to win as much money as possible through choosing advantageous cards (better and safer choices). The total score (net score) is obtained subtracting "bad decks" from "good decks" values ([C+D] - [A+B]). Evolution of net score over consecutive blocks of 20 picks provides a measure of learning processes during the task. The Brazilian version of IGT was translated, adapted, and validated for use in Brazil [21].
Statistical Analyses
Data were analyzed by using Statistical Package for Social Sciences (SPSS 18.0, Chicago, Illinois). Chi-square test was used to assess group differences involving categorical variables. Student's t test was used to perform comparisons involving sociodemographic and clinical variables with normal distribution and Mann-Whitney test for comparisons involving non-normally distributed clinical or sociodemographic data. Repeated measures analysis of variance (ANOVA) with trial blocks (five consecutive blocks of 20 picks) as within-subject factor and subject groups (crack-cocaine and controls) as between-subject factor were used to compare performance on IGT. In addition, an analysis considering separated groups was made by repeated measures ANOVA with trial blocks as within- subject factor.
A multivariate analysis through a logistic regression model was performed in order to identify possible clinical and sociodemographic predictors of a worse performance on IGT test at one-month abstinence assessment. Variables included in the initial model were age, amount of cocaine use, years of cocaine regular use, age at onset of cocaine regular use, type and number of substances used, IQ value, BDI scores and presence of related social and clinical alcohol-related issues through SADD. The odds-ratio (OR) was calculated for significant risk factors. Statistical significance was established as p<0.05 (two tailed) for all analyses.
Results
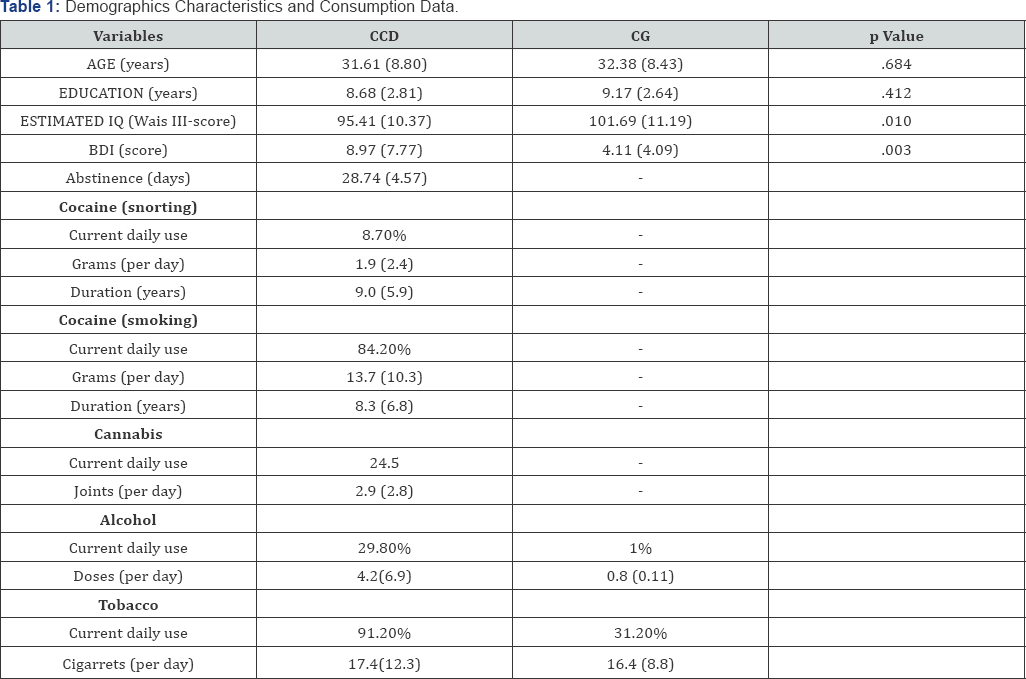
Groups were matched for age and years of education, but differed in both SOFAS (p<0.01) and BDI (p=0.003). Although group with crack-cocaine dependence have presented higher BDI scores, correlations involving IGT and BDI scores were non significant (p>0.05). Such data and self-reported measures of substance consumption are summarized in Table 1. Almost all patients of the crack-cocaine dependence group started using cocaine by snorting at the mean age of 19.3±6.2 years, but only 8.7% are current daily cocaine users (mean of 1.9±2.4 grams per day). They started using crack at the mean age of 23.3±8.8 years, have used crack for 8.3±6.8 years at a mean amount of 13.7±10.3 grams per day and were examined with an average of 28.7 days of abstinence. In patients' group, 91.1% were tobacco smokers, and the mean alcohol use was of 4.2 drinks per day in approximately 30% of them. Marijuana was used by 25% of patients (2.9±2.8 joints per day). None of subjects reported ecstasy, LSD or amphetamine use in last year and they had never used opiates or heroin.
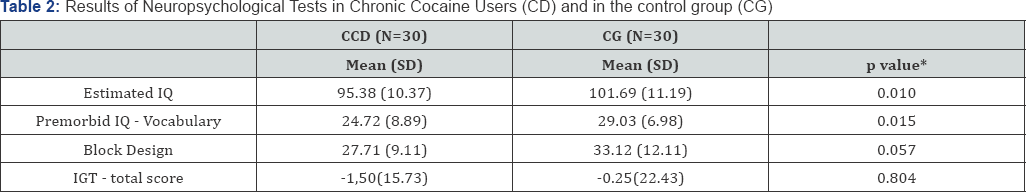
* Student t-test for independent samples.
Note: Numbers express means and (standard deviations) for quantitative variables.
Table 2 shows neuropsychological data for both groups. Groups differed on estimated IQ (p=0.01), whose values ranged from 79 to 125 in the control group and from 75 to 117 in the crack-cocaine group. Groups also differed on premorbid IQ as measured by subtest Vocabulary. Comparing the mean values of IGT total score between both groups, significant differences were not observed. However, analysis involving net scores in blocks of 20 picks during 100 trials showed significant differences in learning, whereas controls showed a greater improvement during the task. Differences between trials 2 and 5 were significant (2-way repeated measures ANOVA; F=4.0; df=1; p<0.05).
Based on sociodemographic observations during the study, other statistical analyses were performed. Group with crack-cocaine dependence was divided into two subgroups, accordingly to SADD score: 1) subjects without any related social and clinical issues associated to alcohol use (n=12); 2) subjects with alcohol-related social and clinical issues (n=18). Subgroups did not differ in age, years of education, estimated IQ and Table 3: Risk factors associated with a worse performance in Iowa Ga of a logistic regression model.
premorbid IQ (p>0.05). It was observed that patients without alcohol-related problems showed a better learning processing, which differed significantly when comparing trial 3 versus trial 5 (F=7.3; df=1; p=0.011) net scores for the subgroup with alcohol- related problems, when compared to the other group, remained negative and revealed a decline in the last two blocks of 20 trials.
A multivariate logistic regression model was performed in order to identify possible clinical and socio-demographic risk factors associated with a worse neuropsychological performance on IGT at one-month abstinence assessment. The final adjusted model (sensitivity 71.4%; specificity 82.6%; positive predictive value 64.5%; negative predictive value 73.3%; area under the curve 0.758) Table 3observed that lower IQ (OR=3.12; p=0.009), higher scores on BDI (OR=3.35; p=0.008) and presence of clinical and social alcohol-related issues (OR=3.27; p=0.01) appeared as significant risk factors for a worse performance. Analyses involving the other neuropsychological tests were not significant.
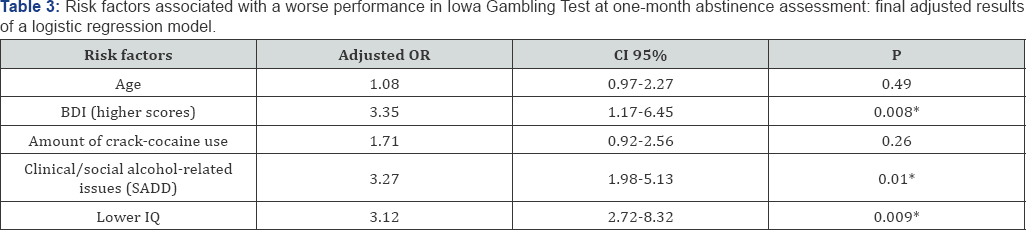
BDI: Beck Depression Inventory; CI: confidence interval; IQ: Inteligence Quocient; OR: odds ratio; SADD: Short Alcohol Dependence Data; * P < 0.05
Discussion
The present study aimed to evaluate the performance of group of patients with crack-cocaine dependence on a decisionmaking task, associating possible deficits to clinical and sociodemographic variables. Although no differences emerged from analyses involving IGT net scores, the patients' group showed impairments in IGT learning measures. The subgroup with alcohol-related problems made more disadvantageous choices on the IGT in comparison to the subgroup without alcohol-related problems. Additionally, lower IQ, higher scores on BDI and presence of clinical and social alcohol-related issues appeared as significant risk factors for a worse performance on IGT at four weeks of abstinence.
Studies have investigated the possible role of cocaine consumption on decision-making deficits [22] have conducted a study which aimed to examine the association between cocaine and marijuana exposure and performance on IGT, observing that amount of use of both cocaine and marijuana was inversely correlated with performance on IGT. However, only cocaine users showed decision making impairment in comparison to healthy controls [22]. In a more recent study, authors also have found that the degree of severity on decision-making deficits measured through IGT are directly associated to treatment relapse in cocaine-dependent outpatients [23]. Furthermore, studies have reported that decision-making deficits are present even in recently exposed or in recreational cocaine users [24-27]. Despite these evidences, there is still a scarcity of studies measuring the decision-making deficits specifically in individuals with crack dependence [28].
In accordance with statistical analyses, present data suggest an additive negative effect of cocaine and alcohol on neurocognitive processes. Bolla et al. [29] examining chronic cocaine users with and without concomitant use of alcohol, found dose-related deficits in neurobehavioral performance after 1-3 days of abstinence, which persisted after four weeks of abstinence [29]. In addition, DSclafani et al. [28] examined cognitive functioning in abstinent crack dependence subjects with and without comorbid alcohol dependence after 6 weeks and 6 months of last exposure. Both groups showed severe and persistent neuropsychological deficits over a wide range of domains even after 6 months of abstinence. Decision-making tasks, however, were not assessed in both studies [28].
This study investigated the possible role of clinical and sociodemographic variables associated with worse performance on IGT in patients with crack-cocaine dependence. It was observed that lower IQ, higher scores on BDI and presence of clinical and social alcohol-related issues appeared as significant risk factors for a worse performance on IGT at four weeks of abstinence. Despite the scarcity of studies that measured the association of those variables on neuropsychological performance, to our knowledge this is the first study that assessed the association of clinical and sociodemographic factors on a worse performance on a decision-making task in patients with crack-cocaine dependence, highlighting the importance of a comprehensive evaluation of these patients as well as the importance of interventions that consider such issues in treatment programs.
The present findings should be interpreted with caution since many limitations were present. Generalizability of findings is limited in view of characteristics of sample, which included only males, inpatients and long-term users. The strict selection criteria that excluded other axis I psychiatric disorders usually associated with substance use disorders, such as depression, may have also affected generalizability of findings. The relatively short duration of abstinence had precluded the discussion about reversibility of neurocognitive deficits. Finally, neuropsychological assessment of impulsivity was not performed in the present study. Recent studies have observed that high levels of impulsivity, a hallmark characteristic of substance use disorders, would be a predictor of treatment relapse and shorter treatment retention [24,30-32].
In conclusion, the present study did not observe significant statistical differences from comparisons involving IGT net scores between a results suggest that a relatively large group of patients with crack-cocaine dependence and matched controls. However, the subgroup with alcohol-related problems made more disadvantageous choices on the IGT in comparison to the subgroup without alcohol-related problems, suggesting that comorbid alcohol use disorder might have independent, additive and enduring neurotoxic effects in neural circuits involved in decision-making tasks. Additionally, lower IQ, higher scores on BDI and presence of clinical and social alcohol-related issues appeared as significant risk factors for a worse performance on IGT at four weeks of abstinence. Although different sources of evidence have demonstrated neurotoxicity associated to cocaine exposure, mechanisms underlying abnormalities in different brain functions, particularly through the smoking route of administration, still aren't well elucidated. Thus, further longitudinal studies examining possible decision-making deficits in patients with chronic crack-cocaine dependence may be informative to confirm the present findings.
Financial Disclosure
This work was supported by Funda^ao de Amparoa Pesquisa do Estado de Sao Paulo (FAPESP), number 2008/09009-2. The funder had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Authors Contribution
ALTL and RAB were responsible for the study concept and design. PPA contributed to the acquisition of data. ALTL, PPA, PJC, SMM, PDG, BS, and ACRPM assisted with data analysis and interpretation of findings. PPA drafted the manuscript. GMAF prepared the final version of the manuscript. ALTL, RAB, SMM, PJC, GMAF and RRL provided critical revision of the manuscript for important intellectual content. All authors critically reviewed content and approved final version for publication.
Conflict of Interest
Authors revealed no conflicts of interest. The authors alone are responsible for the content and writing of the present manuscript. The authors state that this manuscript has not been published elsewhere and has not been submitted simultaneously for publication elsewhere
References
- Abdalla RR, Madruga CS, Ribeiro M, Pinsky I, Caetano R, et al. (2014) Prevalence of cocaine use in Brazil: data from the II Brazilian national alcohol and drugs survey (BNADS). Addict Behav 39(1): 297-301.
- Leshner AI (1997) Addiction is a brain disease, and it matters. Science 278(5335): 45-47
- Lezak M, Howieson D (2004) Neuropsychological Assessment. Oxford University Press, New York, USA.
- Bechara A, Tranel D, Damasio H (2000) Characterization of the decision-making deficit of patients with ventromedial prefrontal cortex lesions. Brain 123: 2189-2202.
- Lucantonio F, Stalnaker TA, Shaham Y, Niv Y, Schoenbaum G (2012) The impact of orbitofrontal dysfunction on cocaine addiction. Nat Neurosci 15(3): 358-366.
- Verdejo-Garcia A, Betanzos-Espinosa P, Lozano OM, Vergara-Moragues E, Gonzalez-Saiz et al. (2012) Self-regulation and treatment.
- Bechara A (2005) Decision making, impulse control and loss of willpower to resist drugs: a neurocognitive perspective. Nat Neurosci 8(11): 1458-1463
- Bechara A, Dolan S (2002) Decision-making and addiction (part II): myopia for the future or hypersensitivity to reward? Neuropsychologia 40(10): 1690-1705.
- Woicik PA, Moeller SJ, Alia-Klein N, Maloney z, Lukasik TM, et al. (2009) The neuropsychology of cocaine addiction: Recent cocaine use masks impairment. Neuropsychopharmacology 34: 1112-1122.
- First MB, Spitzer RL, Gibbon M, Williams JBW (1995) Structured clinical interview for DSM-IV axis I disorders-patient edition (SCID- I/P), version 2. Psychiatric Institute: Biometrics Research, New York, USA.
- (1994) American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. New York, USA.
- Jorge MR, Masur J (1985) The use of the short-form Alcohol Dependence Data questionnaire (SADD) in Brazilian alcoholic patients. Br J Addict 80(3): 301-305.
- Sobel LC, Sobel MB (1992) Time line follow back: a technique for assessing self-reported alcohol comsuption. Psychosocial and Biochemical Methods. N. J. Totawa, Human Press p. 41-72.
- . Associagao Brasileira dos Institutos de Pesquisa de Mercado (ABIPEME) (2008) Criterio de classificagao socioeconomico do Brasil (CCSEB). Sao Paulo: ABA, ANEP, ABIPEME.
- Annett M (2002) Handedness and brain asymmetry. The right shift theory, New York, USA.
- Gorenstein C, Andrade L (1996) Validation of a Portuguese version of the Beck Depression Inventory and the State-Trait Anxiety Inventory in Brazilian subjects. Braz J Med Biol Res 29(4): 453-457.
- Cunha J (2001) Manual em portugues das Escalas Beck. Sao Paulo: Casa do Psicologo.
- Wechsler D (1997) WAIS-III: Administration and scoring manual. San Antonio, PsyCorp.
- Nascimento E (2000) Adaptagao e validagao do teste WAIS-III para um contexto brasileiro. Tese de Doutorado, Curso de Pos-graduagao em Psicologia, Universidade de Brasflia.Brasflia, DF.
- Wechsler D (1997) Wechsler adult intelligence scale, technical manual third edition, San Antonio, PsyCorp.
- Malloy-Diniz LF, Leite WB, Moraes PH, Correa H, Bechara A et al. (2008) Brazilian Portuguese version of the Iowa Gambling Task: transcultural adaptation and discriminant validity. Rev Bras Psiquiatr 30(2): 144148.
- Verdejo-Garcia A, Benbrook A, Funderburk F, David P, Cadet JL, et al. (2007) The differential relationship between cocaine use and marijuana use on decision-making performance over repeat testing with the Iowa Gambling Task. Drug Alcohol Depend 90(1): 2-11.
- Verdejo-Garcia A, Albein-Urios N, Martinez-Gonzalez JM, Civit E, de la Torre R, et al. (2014) Decision-making impairment predicts 3-month hair-indexed cocaine relapse. Psychopharmacology 231(21): 41794187.
- Hulka LM, Eisenegger C, Preller KH, Vonmoos M, Jenni D et al. (2014) Altered social and non-social decision-making in recreational and dependent cocaine users. Psychol Med 44(5): 1015-1028.
- Kjome KL, Lane SD, Schmitz JM, Green C, Ma L, et al. (2010) Relationship between impulsivity and decision making in cocaine dependence. Psychiatry Res 178(2): 299-304.
- Barry D, Petry NM (2008) Predictors of decision-making on the Iowa Gambling Task: independent effects of lifetime history of substance use disorders and performance on the Trail Making Test. Brain Cogn 66(3): 243-252.
- Bechara A, Dolan S, Denburg N, Hindes A, Anderson SW, et al. (2001) Decision-making deficits, linked to a dysfunctional ventromedial prefrontal cortex, revealed in alcohol and stimulant abusers. Neuropsychologia 39(4): 376-389.
- Di Sclafani V, Tolou-Shams M, Price LJ, Fein G (2002) Neuropsychological performance of individuals dependent on crack-cocaine, or crack- cocaine and alcohol, at 6 weeks and 6 months of abstinence. Drug Alcohol Depend 66(2): 161-171.
- Bolla KI, Funderburk FR, Cadet JL (2000) Differential effects of cocaine and cocaine alcohol on neurocognitive performance. Neurology 54(12): 2285-2292.
- Stevens L, Verdejo-Garcia A, Goudriaan AE, Roeyers H, Dom G, et al. (2014) Impulsivity as a vulnerability factor for poor addiction treatment outcomes: a review of neurocognitive findings among individuals with substance use disorders. J Subst Abuse Treat 47: 5872.
- Stevens L, Verdejo-Garcia A, Roeyers H, Goudriaan AE, Vanderplasschen W (2015) Delay discounting, treatment motivation and treatment retention among substance-dependent individuals attending an in inpatient detoxification program. J Subst Abuse Treat 49: 58-64.
- Hulka LM, Vonmoos M, Preller KH, Baumgartner MR, Seifritz E, et al. (2015) Changes in cocaine consumption are associated with fluctuations in self-reported impulsivity and gambling decisionmaking. Psychol Med 45: 3097-3110.






























