Prevalence of Wernicke Encephalopathy in Alcohol Dependent Patients Admitted to Tertiary Care Hospitals
Ramya Balasubramanian1, Jitendra Ingole2 and Harshal Tukaram Pandve3*
1Smt. Kashibai Navale Medical College & General Hospital, India
2Department of Medicine, Smt. Kashibai Navale Medical College & General Hospital, India
3Department of community Medicine, Associate Professor, Smt. Kashibai Navale Medical College, India
Submission: July 01, 2017; Published: July 13, 2017
*Corresponding author: Harshal Tukaram Pandve, Department of community Medicine, Associate Professor, Smt. Kashibai Navale Medical College, Narhe, Pune, Maharashtra state, India, Email: dr_harshalpandve@yahoo.co.in
How to cite this article: Ramya B, Jitendra I, Harshal T, Pandve. Glob J Add & Rehab Med. 2017; 2(4): 555592. DOI: 10.19080/GJARM.2017.02.555592.
Abstract
Introduction: Wernicke Encephalopathy is an acute neuropsychiatric syndrome resulting from thiamine deficiency which is associated with significant mortality and morbidity. It is characterized by a triad of acute mental confusion, ataxia and ophthalmoplegia. Alcohol abuse is one of the most serious problems in public health and Wernicke Encephalopathy is one of the gravest consequences of alcoholism. Despite the disease being preventable and treatable, it is often undiagnosed during life.
Objective: Although western literature has published many studies on the prevalence of Wernicke Encephalopathy; in Indian context in tertiary care hospitals, little amount of data is available. The aim of the study is to find out the prevalence of the disease in alcohol dependent patients presenting to tertiary care hospitals.
Methodology: A cross sectional study was conducted in Smt. Kashibai Navale general hospital, Pune on 100 patients admitted to the medicine wards. All patients that were alcoholics according to DSM V classification were included in the sample. A pretested semi-structured questionnaire was used to note their responses. Based on their responses and appearance of any two of the three signs viz.
- Eye signs
- Cerebella dysfunction
- Either an altered mental state or mild memory impairment, the clinical diagnosis of Wernicke Encephalopathy was made. The study was subsequently analysed using appropriate statistical methods.
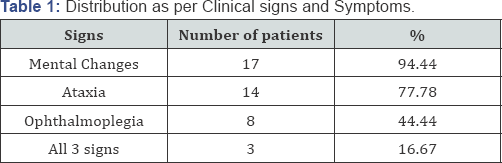
Results: Out of 100 patients 18 were diagnosed with Wernicke Encephalopathy based on clinical signs and symptoms supported by MRI reports. Out of the 18 patients diagnosed with Wernicke Encephalopathy, mental changes (100%; n=9) was most common sign followed by Ataxia (88.9% patients; n= 8) and Ophthalmoplegia (44.4%; n= 4). Number of patients exhibiting all the three signs were 33.3%, n=3.
Conclusion: Thus the prevalence of Wernicke encephalopathy in alcohol dependent patients admitted to tertiary hospitals is 18%.
Introduction
Wernicke Encephalopathy is an acute neuropsychiatric disorder resulting from thiamine deficiency that is associated with significant mortality and morbidity [1]. Alcohol abuse is one of the most serious problems in public health and Wernicke Encephalopathy is one of the gravest consequences of alcoholism [2]. Despite the disease being preventable and treatable, it is often undiagnosed during life. Although the western literature has published many studies on the prevalence of Wernicke Encephalopathy, in Indian context in tertiary hospitals, it has not been estimated yet. Alcoholism is the most common cause of thiamine deficiency around the world [3,4]. It can cause variety of spectrum of disorders such as Beriberi, Korsakoff’s psychosis, or Wernicke Encephalopathy Wernicke Encephalopathy is a neurologic disorder characterized by a triad of acute mental confusion, ataxia and ophthalmoplegia.
Poor diet associated with unhealthy lifestyle, impaired thiamine storage, chronically compromised thiamine absorption from the gastrointestinal tract and reduced thiamine metabolism are some of the additional contributing factors for this condition [4,5]. Alcoholism is one of the major etiologies responsible for vitamin B1 deficiency; its effects are related to the complications of liver cirrhosis such as problems with the gastrointestinal tract with low absorption rate at the mucosal level and consequent malnourishment [6]. Thiamine turnover and glucose oxidation, in a certain brain region such as thalamic nuclei, mammillary bodies, and nerve cells, make the patients susceptible to selective damage causing Wernicke's encephalopathy [7,8]. The clinical diagnosis of Wernicke Encephalopathy requires the presence of two of the three signs i.e. eye signs, Cerebella dysfunction and either altered mental state or mild memory impairment [8-10]. Given the high prevalence of Inpatients with Alcohol dependence, we decided to conduct the study for the prevalence of Wernicke Encephalopathy in our institute.
Methodology
Study design and oversight
This Prospective type, Observational, Cross-sectional study was aimed at determining the prevalence of Wernicke Encephalopathy in Alcoholics at tertiary care teaching institute in Pune city, Maharashtra state, India. The protocol was approved by the institutional ethics committee at the participating hospital. All patients with alcoholic disorders such as Alcoholic liver disease, Alcoholic withdrawal, Alcoholic liver cirrhosis and Alcoholic gastritis/pancreatitis etc. that were alcoholics according to DSM-V classification were included in the sample. A pretested semi-structured questionnaire was used to note their responses. All patients provided oral informed consent. Based on the responses to the structured questionnaire and appearance of any two of the three signs viz. Eye signs, Cerebella dysfunction or either altered mental state or mild memory impairment [8-10] the clinical diagnosis of Wernicke Encephalopathy was made. The diagnosis of Wernicke Encephalopathy in these patients was made based on clinical signs and symptoms. MRI findings were used to support the diagnosis.
Inclusion And Exclusion Criteria
The Inclusion criteria are based on the criteria given by DSM-V manual for Alcoholism. Exclusion criteria were patients having a history of stroke, psychiatric disorders, Ophthalmoplegia (due to Thyroid diseases, stroke, brain tumor or trauma, meningitis), other, causes of ataxia not related to alcoholism viz. Vestibular vertigo, Spinocerebellar ataxia, Friedreich's ataxia etc, Dyselectrolytemia and Critically ill patients.
Results
Patients
From April 2016 to September 2016, a total of 100 patients were enrolled in the study conducted in Smt. Kashibai Navale general hospital. They were in-patients admitted to the Medicine wards for Alcohol-related disorders. An informed consent was obtained from them. The age of the patients ranged from 30 to 68 years, mean age is 49 years (Tables 1 & 2).
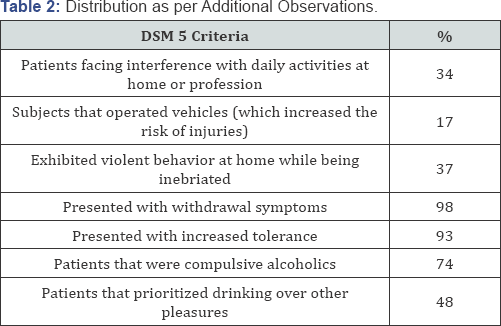

Prevalence of Wernicke Encephalopathy
18 were diagnosed with Wernicke Encephalopathy based on clinical signs and symptoms supported by MRI reports.
Discussion
Thiamine deficiency in the Western world has been reported in 30-80% of alcoholics [11]. Although chronic alcoholism is becoming an increasing problem in the Third World [12] there is little prospective data on WE from these countries. In the alcoholic patient, many factors contribute to a thiamine- deficient state which may predispose to brain damage [13]. Intake of thiamine is reduced and absorption impaired by alcohol or malnutrition. The Liver disease itself leads to reduced body stores and impaired metabolism of thiamine [13].This may explain the high prevalence of in our study in which all patients had severe liver disease.
So much attention is directed to the overt clinical problem that deterioration in the mental state is often attributed directly to the presenting illness, to hypoglycemia, delirium tremens or hepatic encephalopathy rather than to the development of Wernicke's encephalopathy. Furthermore, less detail is paid to neurological assessment in the alcoholic as these demands a more co-operative patient: the symptom of generalized weakness with inability to walk or confinement to bed may conceal a more specific gait disturbance (peripheral neuropathy/ataxia). For these reasons, a high index of suspicion is required in mentally obtunded or uncooperative patients, especially in those with an alcoholic background.
Conclusion
In conclusion, it appears that Wernicke’s encephalopathy is easily diagnosed when neurological deficits accompany mental changes, and when it is the sole presenting illness. This entity is a common accompaniment in alcohol-related disease. However, it is probably overlooked as a cause of mental deterioration in many of these patients because of non-specific symptoms and the difficulty in eliciting neurological signs in the ill patient. A greater clinical awareness is therefore demanded in these patients.
Thiamine should form part of the routine management in the alcoholic patient with liver disease, pancreatitis or any other alcohol related disorder, even in the absence of neurological deficit.
References
- Victor M (1976) The Wernicke-Korsakoff syndrome in: PJ Vinken, GW Bruyn (Eds.) Handbook of clinical neurology 28: 243-270.
- Manzo L, Locatelli C, Candura SM (1994) Nutrition and alcohol neurotoxicity. Neurotoxicology 15(3): 555-565.
- Luxemburger C, White NJ, ter KF, Singh HM, Allier-Frachon I, et al. (2003) Beri-beri: the major cause of infant mortality in Karen refugees. Trans R Soc Trop Med Hyg 97(2): 251-255.
- Thomson AD (2000) Mechanisms of vitamin deficiency in chronic alcohol misusers and the development of the Wernicke-Korsakoff syndrome. Alcohol Alcohol 35(1): 1-2.
- Thomson AD, Marshall EJ (2006) The natural history and pathophysiology of Wernicke's Encephalopathy and Korsakoff's Psychosis. Alcohol Alcohol 41(2): 151-158.
- Thomson AD (2000) Mechanisms of vitamin deficiency in chronic alcohol misusers and the development of the Wernicke-Korsakoff syndrome. Alcohol and Alcoholism Supplement 35(1):2-7.
- Renthal W, Marin-Valencia I, Evans PA (2014) Thiamine deficiency secondary to anorexia nervosa: An uncommon cause of peripheral neuropathy and Wernicke encephalopathy in adolescence. Pediatr Neurol 51(1): 100-103.
- Aasheim ET (2008) Wernicke encephalopathy after bariatric surgery: a systematic review. Ann Surg 248(5): 714-720.
- Caine D, Halliday GM, Kril JJ, Harper CG (2007) Operational criteria for the classification of chronic alcoholics: identification of Wernickes encephalopathy. J Neurol Neuro-surg Psychiatry 62(1): 51-60.
- Singh S, Kumar (2007) A Wernicke encephalopathy after obesity surgery: a systematic review. Neurology 68(11): 807-811.
- Edwards G (1983) Drinking problems. Putting the Third World on the map. Lancet 2(8139): 402-404.
- Thomson AD, Ryle RR, Shaw GK (1983) Ethanol, thiamine and brain damage. Alcohol Alcoholism 18(1): 27-43.
- Thomson AD, Jeyasingham MD (1987) PrattNutrition and alcoholic encephalopathies. Acta Med Scand 717: 55-65.






























