Abstract
Background: The first case of COVID-19 in Saudi Arabia was confirmed on March 2, 2020. Our aim in this study is to evaluate our radiotherapy
services during COVID-19 pandemic.
Methods: A retrospective observational study included cancer patients who were on active radiation treatment in our oncology Centre during
the period from March 2020 to February 2021 in comparison with the corresponding period from March 2019 to February 2020.
Results: A total number of 673 patients received radiotherapy in the period from March 2019 -February 2020, 427 (63.4%) patients were
treated with radical intent, 246 (36.6%) patients were treated with palliative intent, majority of patients were diagnosed as: breast cancer (40
%), gynecological cancers (19%), head and neck cancers (10%), 54.8% of patients received three-dimensional conformal radiation therapy
(3D-CRT), 39% of them received more advanced technique intensity modulated radiation therapy (IMRT/VMAT), 5.64% received high dose rate
(HDR) brachytherapy and 3 patients received intraoperative radiotherapy (IORT). For the corresponding months in 2020-2021, A total number
of 592 patients received radiotherapy in the period from March 2019 to February 2020, 395 (66.7%) patients were treated with radical intent,
197 (33.3%) patients were treated with palliative intent, majority of patients were diagnosed as: breast cancer (42%), head and neck cancers
(15%), gynecological cancers (13%), 59.1% of patients received 3D conformal radiotherapy,38.1% of them received more advanced technique
(IMRT/VMAT), 2% received HDR brachytherapy and 4 patients received intraoperative radiotherapy. Only 3 COVID-19 positive patients (0.50%)
were recorded in 2020-2021, all of them were symptomatic, 2 of them were males, average age was 57, 2 of them treated with radical intent and
were receiving concurrent chemotherapy. all of them completed their course of treatment with no disease progression. No significant changes
were recorded in our five departmental key performance indicators between the two mentioned periods.
Conclusion: Our radiotherapy services were not significantly affected by COVID-19 pandemic despite the increasing numbers of COVID-19 cases
in Saudi Arabia. Many lessons were learned from the pandemic and can be applied for any pandemic happening now or in the future without
interrupting radiation oncology care.
Keywords:COVID 19, Radiation Oncology, Pandemic; Radiotherapy; COVID-19 pandemic
Introduction
The global COVID-2019 pandemic has presented a big management dilemma for cancer patients and added many challenges to the field of radiation oncology which is highly dependent on delivering radiotherapy (RT) service on daily basis for a period of up to 8 weeks with increased risk of infection for both healthcare professionals and cancer patients [1]. In addition to the commonly recommended protective measures against COVID-19, there are many measures that have been recommended by radiation oncology societies to reduce the risk of infection and to prevent interruption or delay in the daily radiation treatment course as much as possible [2,3].
First COVID-19 case was reported in Saudi Arabia on 2 March, 20204. As a result, the government of Saudi Arabia has taken many serious steps early in March 2020 in terms of social distancing such as: closing schools, cancelling all large events, halting all national and international flights and isolation of all Saudi citizens who were coming from abroad for 14 days [5]. Between late March and first of June 2020, Umrah (an Islamic ritual done by thousands of Muslims in the holy city of Mecca daily) are suspended along with suspension of the five daily prayers all over mosques of the kingdom [6].
All lockdown measures had been gradually relaxed by first of June, 2020 except in Mecca and many highly crowded districts including Al-Mahjar District where our oncology center is located. This added another unique challenge in front of our radiation oncology department to offer an uninterrupted service to our cancer patients during COVID-19 pandemic. Cancer patients in Saudi Arabia were managed according to their infectious status using specific recommendations provided by the Saudi Arabia National Cancer Institute [7].
Our radiation oncology center is in Al-Mahjar District (south of the city of Jeddah) and affiliated to King Abdullah Medical City (KAMC) which is located in the holy capital (Mecca) and from which we received most of our patients and offering radiotherapy service to the western area of Saudi Arabia. Average number of patients treated each year since we started on 2012 is around 622 patients (Figure 1). Since 2015, our total number of treated patients increased yearly with significant reduction in 2020 which mostly due to COVID-19 pandemic which resulted in disruptions in diagnosis and therapy prior to radiation treatment.
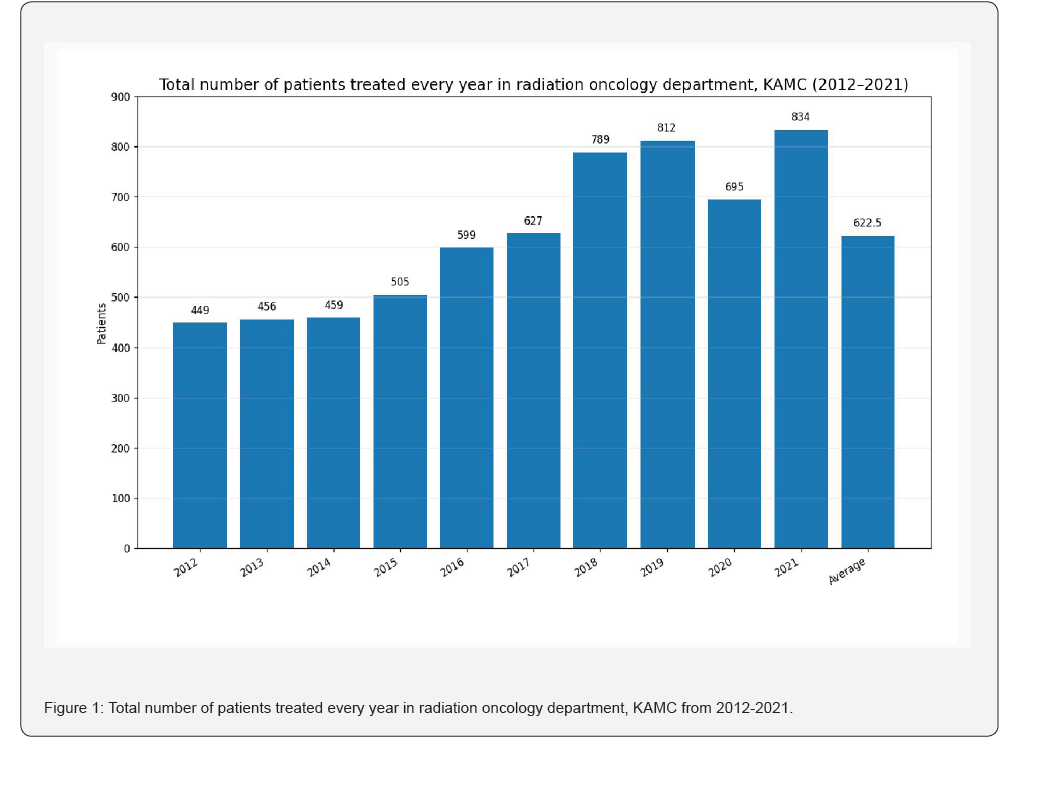
This may be also attributable to preference of patients to avoid or postpone contact with healthcare workers during the pandemic with reduction in the capacity of routine cancer screening programs following governmental lockdown measures in the kingdom. In addition to postponing surgical interventions to maintain sufficient ICU capacity during COVID-19 pandemic [8- 10]. In this study, we are aiming to retrospectively analyze in a simple way the impact of the COVID-19 pandemic and resulting governmental measures on radiotherapy service in Jeddah oncology center, KAMC.
Materials and Methods
A non-interventional comparative observational retrospective study included all cancer patients who were under active radiation treatment in Jeddah oncology center in the period from March, 2020 to February, 2021 in comparison with the corresponding months from March, 2019 to February, 2020. An ethical approval (Registration no. 22-906) was obtained from Institutional Review Board (IRB) in KAMC, registered at the National Biomedical Ethics Committee, King Abdulaziz City for Science and Technology on 04-06-2012(Registration no. H-02-K-001).
To clarify the workload during the above-mentioned periods, we identified all cases received radiation treatment through retrospective review of ARIA radiation system according to their Diagnosis, intent of treatment and type of treatment technique for each patient. Intent of treatment recorded as either curative or palliative. Treated tumor sites included brain, head and neck, thorax, abdomen, pelvis, extremity, and others. Treatment modalities included external beam radiotherapy (EBRT), Brachytherapy (BT) and intraoperative radiotherapy (IORT). Treatment techniques included three-dimensional conformal radiation therapy (3D-CRT), intensity modulated radiation therapy (IMRT), Volumetric modulated arc therapy (VMAT) and Stereotactic radiosurgery (SRS).
We presented the clinical characteristics of patients who were positive COVID-19 during their course of radiotherapy or had history of COVID-19 infection regarding their clinical presentation, COVID-19 symptoms, associated comorbidities with evaluation of the outcomes of these patients including cancer outcomes. We followed the COVID-19 recovery criteria (2 negative RT-PCR tests, 24 hours apart) published in March, 2020 by the Saudi Center for Disease Prevention and Control and the Ministry of Health [11]. In addition to that, we recorded also Patients who had history of positive COVID-19 infection and cured from it before starting radiotherapy.
The impact of COVID-19 pandemic on the five departmental key performance indicators (KPIs) was analyzed including the following:
• First KPI: Compliance rate with fulfilling all weekly
reviews of patients in radiation oncology outpatient clinics for
assessment of any complaint or radiation toxicity during their
course of radiotherapy.
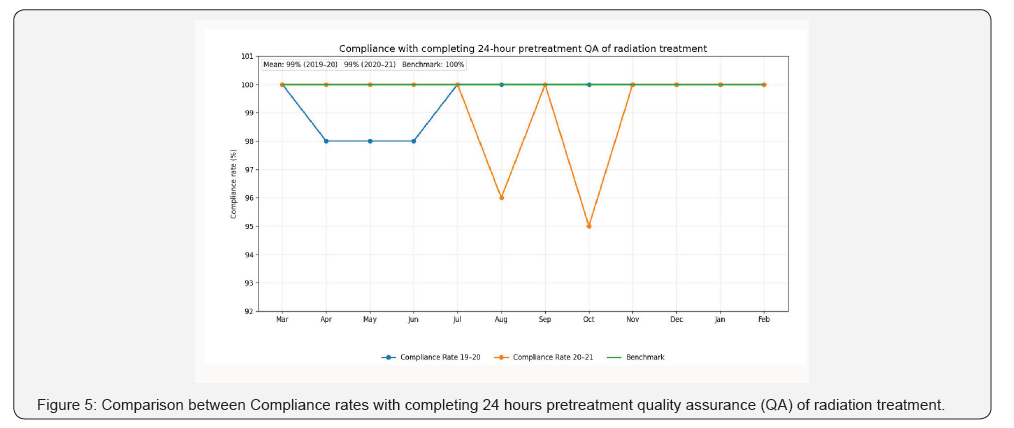
• Second KPI: Compliance rate with completing 24 hours
pretreatment quality assurance (QA) of radiation treatment.
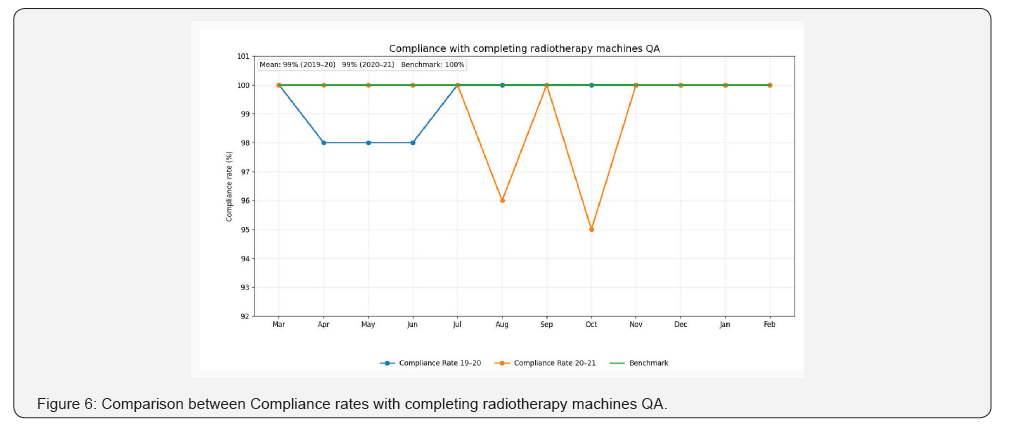
• Third KPI: Compliance rate with completing radiotherapy
machines QA.
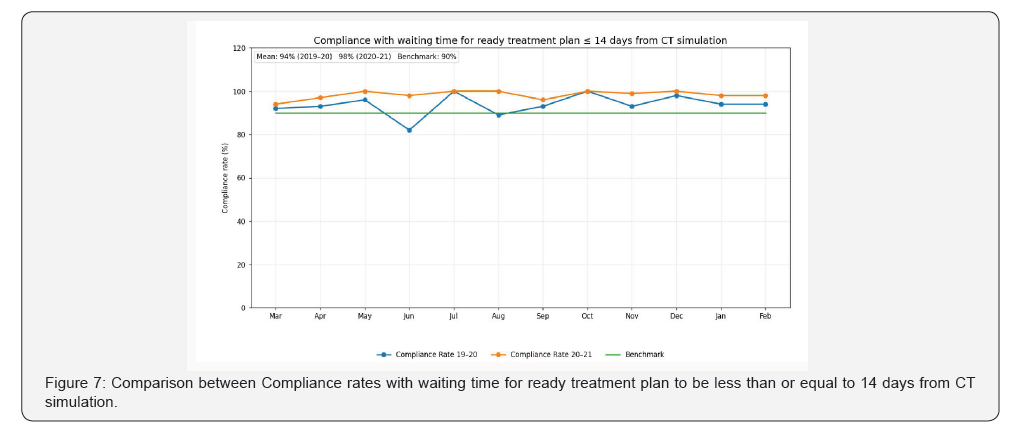
• Fourth KPI: Compliance rate with waiting time for
ready treatment plan to be less than or equal to 14 days from CT
simulation.
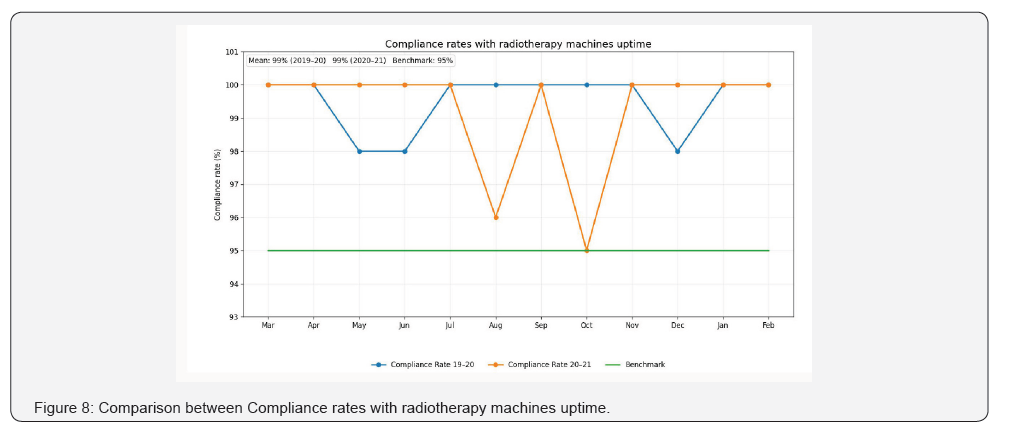
• Fifth KPI: Compliance rate of radiotherapy machines
uptime.
Results
By comparing our radiation treatment activity under ordinary routine conditions within the prepandemic period March, 2019 to February, 2020, with the corresponding time interval from March, 2020 to February 2021, no significant changes were observed in the number of services performed. Significantly, in 2019-2020, 832 new patients prepared for CT simulation and 632 patients treated on Linear Accelerators. In the corresponding pandemic period in 2020-2021, 683 new patients prepared for CT simulation and 576 patients to be treated on Linear Accelerators (Figure 2). A total number of 673 patients received radiotherapy in the period from 2019-2020, 427 (63.4%) patients were treated with radical intent, 246 (36.6%) patients were treated with palliative intent, 54.8% of patients received 3D conformal radiotherapy, 39% of them received more advanced technique (IMRT/VMAT), 5.64% received HDR brachytherapy and 3 patients received intraoperative radiotherapy.
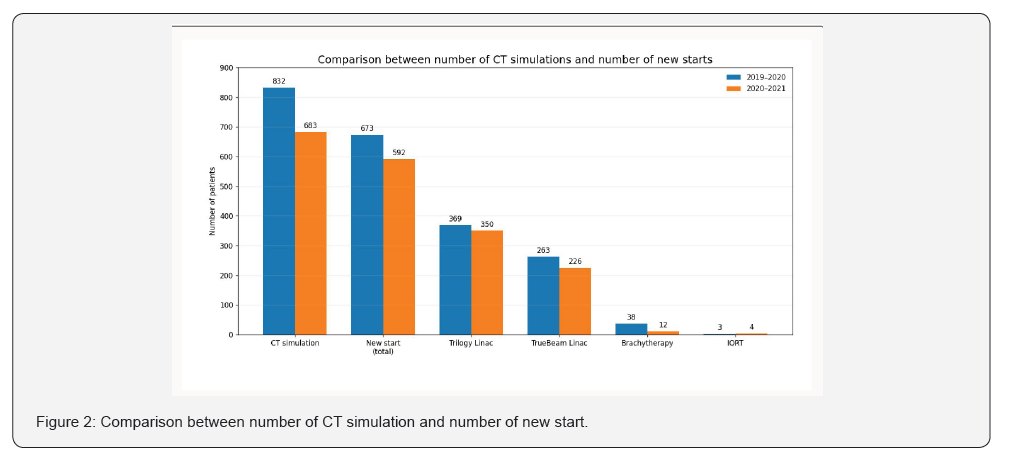
For the corresponding months in 2020-2021, A total number of 592 patients received radiotherapy 395 (66.7%) patients were treated with radical intent, 197 (33.3%) patients were treated with palliative intent, 59.1% of patients received 3D conformal radiotherapy, 38.1% of them received more advanced technique (IMRT/VMAT), 2% received HDR brachytherapy and 4 patients received intraoperative radiotherapy. Furthermore, breast cancer was the most common type of cancer in both prepandemic and pandemic periods. However, head and neck cancer ranked 2nd among the group of 2020-2021 instead of gynecological cancers in 2019-2020 (Figure 3).
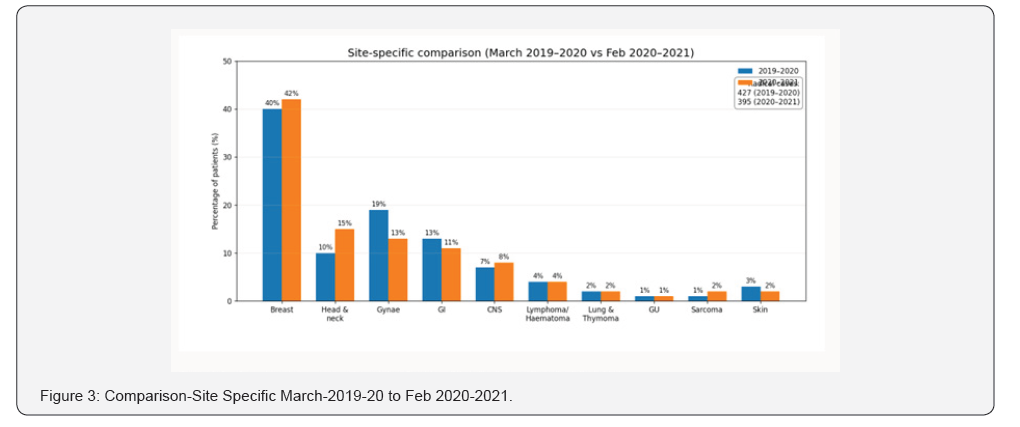
Only 3 COVID-19 positive patients (0.50%) were recorded between March 2020 to February 2021, 2 of them were males, average age was 59, 2 of them treated with radical intent and were receiving concurrent chemotherapy, 2 of them were symptomatic with fever and cough as the common symptoms, one of them had associated diabetes mellitus, diagnosed as: rectal cancer, esophageal adenocarcinoma and recurrent olfactory meningioma. 2 of them needed prolonged hospital stay which interrupted their course of radiotherapy, recovered from COVID-19 and completed their course of radiation treatment. The third one started her palliative radiation treatment while she was still positive for COVID-19 with no symptoms taking into consideration all protective measures to reduce the risk of infection between patients and healthcare workers. All of them reported no disease progression.
We recorded also patients with history of COVID-19 before start of RT between March 2020 to February 2021, we reported 4 patients (0.67%) who were COVID-19 positive two to three months before start of RT, 3 of them were males, average age was 60.7, 3 of them treated with radical intent, 2 of them were receiving concurrent chemotherapy, none of them had associated comorbidities, diagnosed as: basal cell carcinoma, bladder cancer, glioblastoma multiform and recurrent osteosarcoma. All of them completed their RT course successfully with no gaps. Most of them (3 out 0f 4) reported stable disease. The only case treated with palliative intent died from her disease 1.5 year following completion of palliative radiotherapy.
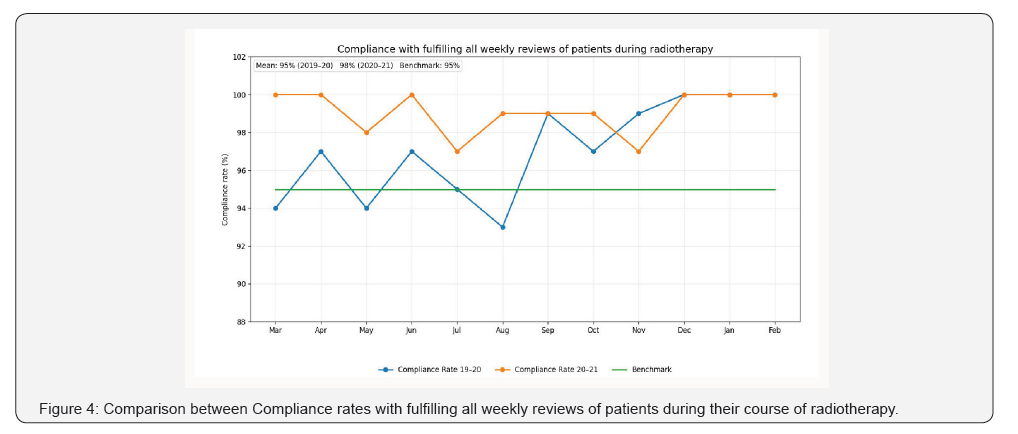
Regarding our five departmental key performance indicators (Figures 4-8). During the pandemic periods (2020-2021), averages of compliance rate to fulfill weekly review for patient during treatment was 98 % which was higher than the designated benchmark (95%) and interestingly it was higher than the average of compliance rates (95%) in the prepandemic periods (2019-2020). Average of compliance rate with waiting time for ready treatment plan to be less than or equal to 14 days from CT simulation was higher in the pandemic period (98% versus 94%) than the prepandemic period (Figure 7). Averages of Compliance rates with completing radiotherapy machines QA, Compliance rates with completing radiation treatment QA 24 hours before start of treatment and Compliance rates with radiotherapy machines uptime were equal (99%) for both pandemic and prepandemic periods and above the designated benchmark (100%, 100% and 95%) respectively (Figures 5,6,8).
Discussion
Jeddah oncology Centre is one of the 5 radiotherapy centers in the western area of Saudi Arabia and equipped with two Linear Accelerators (Linacs), Computed Tomography Simulation (CT simulation) and clinical dosimetry facilities that operate daily for 5 days weekly between 8:00 am to 4:30 pm. Radiotherapy staff consist of 11 doctors, 12 technicians, 9 dedicated physicists, 6 nurses, a social worker, 2 clinical nutrition staff and 2 secretary staff. In response to COVID-19 pandemic, all unnecessary leaves were prevented, and strict social distancing regulations were applied to stop any gatherings.
To reduce exposure of healthcare workers to infection, all administrative rules and medical information regarding COVID-19 pandemic was transmitted through e mails and messaging groups. Important questionnaires were collected electronically and all Tumor boards discussing the management plan for cancer patients was done virtually [12,13]. All appointments for CT simulation or for start of radiation treatment made over the phone by our radiotherapy coordinator.
During the exceptional times of both lockdown and postlockdown phases, we performed a full maintenance of CT simulation, radiotherapy treatment and dosimetry activities with prioritization of radiotherapy according to the published guidelines during COVID-19 pandemic [14]. We preferred to adopt hypo fractionated schemes, when possible, especially for breast, prostate cancers and for palliative treatments [15]. To provide continuous care during the pandemic, radiotherapy staff was divided into two groups, A and B to work with no overlap between the rotating schedules. If any staff member developed symptoms, it is mandatory to notify the hospital to follow until an infection ruled out.
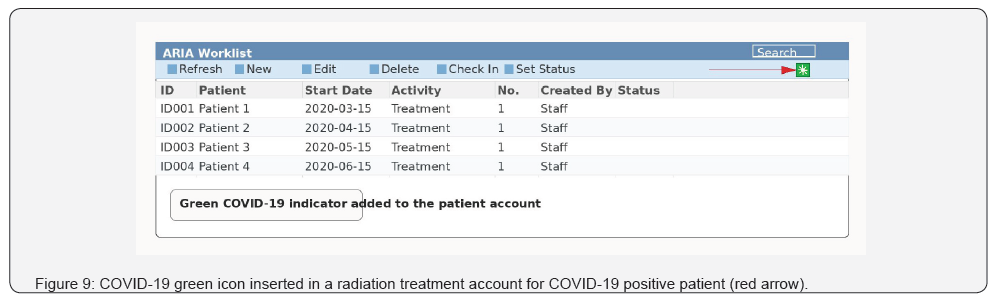
Masks and alcohol-based hand sanitizers were required for all staff, patients and their caregivers when and they would first go through a temperature checkpoint at main gateway. If cough, fever, and dyspnea detected, the patient will be referred to respiratory triage room to be assessed by the assigned physician and nurse and a COVID-19 nasopharyngeal swab will be taken if needed with strict home isolation until results of COVID-19 test. If the patient is critically ill, patient will be referred to the main hospital of KAMC in Mecca and will be and managed accordingly. If the patient confirmed as a positive COVID-19 case, a new green icon will be added to his or her account on radiation oncology treatment and planning system (ARIA) until clearance as illustrated in (Figure 9).
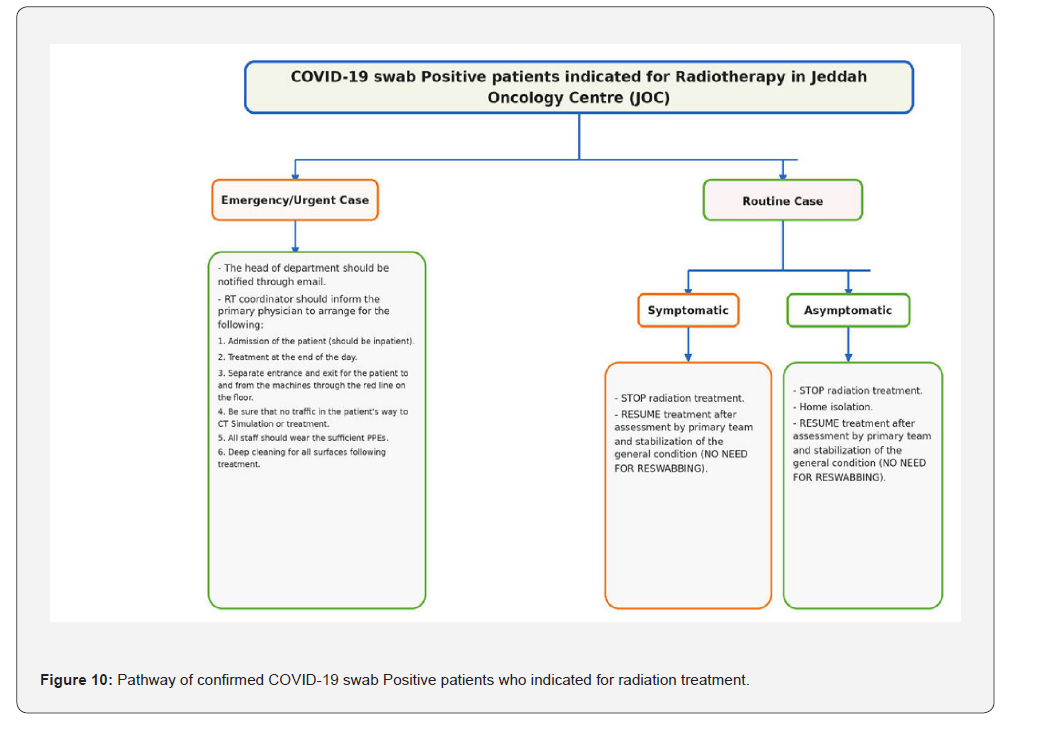
While waiting for radiation treatment, patients instructed to keep interpersonal distance spacing of 2 meters or more watching flash messages to increase their awareness towards COVID-19 protective measures. In order to accommodate disinfecting procedures between treatments, our machine slots reduced to be 3 patients/hour instead of 4 patients/hour per machine before the pandemic. For Patients with confirmed COVID-19 swab Positive patients and indicated for radiation treatment, the priority of radiation treatment assessed by the primary team versus the risk and complications of COVID-19 infection. Only one patient received radiation treatment while she is positive for COVID-19 during the period from March, 2020 to February, 2021 and we followed the pathway to treat her as an urgent case for palliation as illustrated in (Figure 10).
We succeed to offer uninterrupted radiation treatment services and to reduce the risk of transmission of COVID-19, only 0.50% of patients were positive and continued their radiation treatment after recovery from COVID-19 with no disease progression even for patients who needed prolonged hospital stay due to their infection. In our study, recent or history of COVID-19 infection does not significantly affect the course of radiotherapy. However, our number of patients was insufficient to be applied for all infected patients and further studied are needed to clarify the real impact of recent or history of COVID-19 infection on patients under radiotherapy. We also used our KPIs to assess and monitor our performance during COVID-19 pandemic in comparison with the corresponding prepandemic period aiming to improve our quality of care. KPIs also give the chance for medical professionals to make evidence-based decisions based in view of objective quality measures and to highlight the points which need more attention and development [16,17].
There was no negative impact on the all five KPIs. Interestingly, compliance rates for the first and fourth KPIs were higher in pandemic than pre pandemic periods. We thought that higher compliance rate for the weekly review for patients in RT clinic during pandemic periods (first KPI) was related to more tracking of patients under radiotherapy to be seen by the primary physician in the outpatient clinic to assess if there is any complaint or radiation toxicity in addition to tracking of patients who not attended for their daily sessions or weekly clinic by phone to exclude any signs or symptoms of COVID-19 infection. The causes of higher compliance rate for the fourth KPI in the pandemic periods may be due to rotation of the staff in 2 groups, so each group were very keen to finish all their duties in the working week and to endorse well through phone or e-mail to the next group all details for the radiotherapy process in addition to use of our radiotherapy electronic dashboard which is always supplied and updated by all RT values, dates and issues timely warnings.
The second, third and fifth KPIs, averages of compliance rates were equal between pandemic and pre pandemic periods and higher than the designated benchmark in both periods. Causes of noncompliance to the designated benchmarks in some months during the pandemic were due to causes not related to the pandemic itself but related to technical errors in machines which took one or two days to be fixed, orders by physicians to delay start of treatment for more investigations or due to patient’s request to delay the start of treatment. Recent research on the reported performance indicators for radiation oncology service is scarce and the selection of indicators related to radiotherapy is still challenging [18,19]. To our knowledge, our study is the first study to evaluate the impact of COVID-19 pandemic on the quality of radiation oncology service using performance indicators in Saudi Arabia.
Conclusion
Our radiotherapy services were not significantly affected by COVID-19 pandemic despite the increasing numbers of COVID-19 cases in Saudi Arabia. Many lessons were learned from the pandemic and can be applied for any pandemic happening now or in the future without interrupting radiation oncology care. Continuous assessment of the performance indicators facilitates evaluation of quality of radiation oncology service and achievement of objectives even during the exceptional times of pandemics.
Author Contributions
Conceptualization, HG; validation, MA; data curation, AE; methodology, HG, AH, AE and GA; software AH; writing and original draft preparation, HG; review and editing, MA; visualization, AH; supervision, MA All authors have read and agreed to the published version of the manuscript.
Funding
This research did not receive any external funding./p>
Institutional Review Board Statement:
An ethical approval (Registration no. 22-906) was obtained from Institutional Review Board (IRB) in KAMC, registered at the National Biomedical Ethics Committee, King Abdulaziz City for Science and Technology on 04-06-2012(Registration no. H-02-K-001). Informed Consent Statement: Informed consent is waived for this study, due to absence of any individualized related patient data, human participation, animal involvement, clinical trial or any biological tissues.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
Acknowledgment
The authors would like to thank: Mr. Salem Ahmad, Mrs. Sanaa Ahmed, Mrs. Saba Khan, Mrs. Sherwina P. Sanai, Mrs. Rawan Mmotawkel and Mrs. Siti Balamo for their help in data extraction. The authors are also so grateful to their colleagues in department of radiation oncology, KAMC for addressing meticulous care for cancer patients during the exceptional times of COVID-19 pandemic. Great appreciation for Dr. Emad Azhari and Dr. Khalofa Alghamdi for their recommendations and dedicated leadership.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Mangesius J, Arnold CR, Seppi T, Mangesius S, Bruggl M, et al. (2021) Impact of COVID-19 on Radiation Oncology, an Austrian Experience. Curr Oncol 28(6): 4776-4785.
- Combs SE, Belka C, Niyazi M, Corradini S, Pigorsch S, et al. (2020) First statement on preparation for the COVID-19 pandemic in large German Speaking University-based radiation oncology departments. Radiat. Oncol 15(1): 74.
- Tey J, Ho S, Choo BA, Ho F, Yap SP, et al. (2020) Navigating the challenges of the COVID-19 outbreak: Perspectives from the radiation oncology service in Singapore. Radiother. Oncol 148: 189-193.
- Communication Government Center (2020) Saudi Arabia’s Ruthless Fight against Coronavirus.
- Algaissi AA, Alharbi NK, and Hassanain M, et al (2020) Preparedness and response to COVID-19 in Saudi Arabia: building on MERS experience J Infect Public Health 13(6): 834-838.
- Ministry of Health. Coronavirus Disease COVID-19 Guidelines v1.2.
- Ministry of Health (2020) Saudi Arabia National Cancer Institute (2020) Coronavirus Disease 2019 (COVID-19). Caregiver and Facility Clinical Practice Guidelines.
- Abdul-Rahman Jazieh, Abdulrahman Al Hadab, Ashwaq Al Olayan, Ayman AlHejazi, Faisal Al Safi, et al (2020) Managing oncology services during a major coronavirus outbreak: lessons from the Saudi Arabia experience JCO Glob Oncol 518-524.
- Abdul-Rahman Jazieh, Thamer H Alenazi, Ayman Alhejazi, Faisal Al Safi, Ashwaq Al Olayan (2020) Outcome of oncology patients infected with coronavirus JCO Glob Oncol 6: 471-475.
- American Society of Clinical Oncology (2020) A Guide to Cancer Care Delivery During the Covid-19 Pandemic (Chicago: American Society of Clinical Oncology).
- Saudi Center for Disease Control and Prevention (2020) COVID-19 interactive dashboard.
- Azab M (2021) Uninterrupted Neurosurgical Care at a Tertiary Center in Makka amid COVID 19, Asian Journal of Neurosurgery.
- Emad Tashkandi, Ahmed Zeeneldin, Amal AlAbdulwahab, Omima Elemam, Shereef Elsamany, et al (2020) Virtual management of cancer patients in the era of COVID-19 pandemic (preprint) J Med Internet Res 22(6): e19691.
- COVID-19 rapid guideline: delivery of radiotherapy. NICE – National Institute of Health and Care Excellence.
- Simcock R, Thomas TV, Estes C, Filippi AR, Katz MA, Pereira IJ (2020) COVID-19: global radiation oncology's targeted response for pandemic preparedness. Clin Transl Radiat Oncol 22: 55-68.
- Smith PC, Mossialos E, Papanicolas I (2008) Performance measurement for health system improvement: experiences, challenges and prospects. World Health Organisation.
- Mainz J (2003) Defining and classifying clinical indicators for quality improvement. Int J Qual Health Care 15(6): 523-530.
- Van Lent WA, de Beer RD, van Triest B, van Harten WH (2013) Selecting indicators for international benchmarking of radiotherapy centres. J Radiother Pract 12: 26-38.
- Van Lent WA, de Beer RD, van Harten WH (2010) International benchmarking of specialty hospitals. A series of case studies on comprehensive cancer centres. BMC Health Serv Res 10: 253.






























