Accessing the Health Needs of Adolescents and Young Adults with Cancer in Brazil
Sáhlua Miguel Volc1* and João Lucas Volc2
1Medical Doctor, AC Camargo Cancer Center, São Paulo, Brazil
2Medicine student UFPR, Curitiba-Paraná, Brazil
Submission: January 19, 2023; Published: January 30, 2023
*Corresponding Address: Sáhlua Miguel Volc, Medical Doctor, AC Camargo Cancer Center, Barretos Cancer Hospital, Pius XII Foundation, City of Barretos, Rua José Getúlio 474 apt 102, Liberdade, São Paulo, Brasil
How to cite this article: Sáhlua Miguel V, João Lucas V. Accessing the Health Needs of Adolescents and Young Adults with Cancer in Brazil. Canc Therapy & Oncol Int J. 2023; 23(2): 556106. DOI:10.19080/CTOIJ.2023.23.556106
Abstract
Adolescents and young adult cancer patients have unique characteristics and specific needs that, when properly comprehended, can improve quality of life during and after the oncologic treatment.
Objective: verify those that would be the main health needs among this group of patients.
Method: cultural and linguistic validation of a canadian questionnaire regarding the theme, with posterior application on 252 patients afflicted by malign neoplasms, with ages 15-39 undergoing oncological treatment or having finished their treatment in the last 5 years.
Results: we have verified differences and similarities when comparing the results from Brazil and Canada. Some needs had the same level of importance, such as preoccupations with healthy diets, while other presented disparities that reflect cultural differences between the two groups.
Conclusion: based on the gathered results, we indicated what would be the specific needs of this demographic, guiding adequations to physical space, interdisciplinary follow-ups and the supplying of information relevant to the target groups in question.
Keywords: Adolescentes; Young adults; Cancer; Health care
Introduction
In the last three decades, the group formed by adolescents and young adults with cancer has been gaining notoriety among health professionals who work in an interdisciplinary way to minimize the biopsychosocial impacts that accompany the diagnosis of a neoplasm. The age group in question finds its lower limit at 15 years old, while its upper limit varies regionally, ranging from 18 to 39 years old [1]. Among the most frequent malignant neoplasms are leukemias, lymphomas, central nervous system tumors, germ tumors, sarcomas and melanomas [2]. In Brazil, cancer in adolescents and young adults corresponds to the second cause of death, with cervical cancer being the main cause of mortality in females aged 25 to 29 years [3]. It is clear that the survival of this group is lower than that of children and adults, however, the reasons for this phenomenon are varied, some of which are well established. Among the main ones, we found the low participation in treatment protocols, lack of uniformity of treatment for the most incident neoplasms and the high biopsychosocial impact during and after treatment [4].
Specialized oncological care for adolescents and young adults, called oncoebiatrics, has a relatively recent history, with the first units specializing in this type of care appearing in the United States and the United Kingdom, later arriving in Canada, Italy and Australia. Usually, in many countries, including Brazil, these patients have been treated both in pediatric oncology services and in clinical oncology, which makes it difficult to standardize treatment protocols and interdisciplinary follow-up [5]. This population has peculiar characteristics and specific demands, which, when well understood, can improve quality of life during and after cancer treatment. The objective of this study is to verify what would be the main health needs for adolescents and young adults who are undergoing oncological treatment or who have already completed it, providing a solid substrate for organizing health services that can better serve these patients.
Material and Methods
We carried out the cultural and linguistic validation, according to Beaton [6], as described below, of a questionnaire applied to adolescents and young adults with cancer in the city of Toronto (Canada), which addresses the main oncological pathologies in this age group [7]. Initially, the questionnaire was translated from the original in English into Portuguese by two Brazilians who speak fluent English. In sequence, the two versions were synthesized into a single version. This was then back-translated into English by two native translators from English-speaking countries who speak Portuguese as a second language. Next, a committee of experts reviewed the translated versions to produce a final version that was pilot tested. For the pilot test, the questionnaire was applied to 30 patients to adapt the linguistic terms used and the degree of understanding of the analyzed population.
The study included 252 patients between 15 and 39 years of age treated both at the Barretos Cancer Hospital and at the Children’s and Youth Cancer Hospital belonging to the Pio XII Foundation, who were undergoing oncological treatment or who had received treatment in the last 5 years. There was no restriction regarding the type of tumor or clinical situation. The sample size was defined for convenience.
The formula used to obtain the sample size was for descriptive studies of dichotomous variables. In the work cited above [7], 4 questions received 80% high marks. Thus, considering a significance of 5% and a desired precision of the confidence interval of 10%, we defined the sample size as a minimum of 246 respondents [8].
Patients were evenly divided into 3 age groups: 15 to 18 years old, 19 to 25 years old and 26 to 39 years old. We analyzed sociodemographic, clinical and behavioral variables (categorical) in part A of the interview, and continuous variables (questionnaire) in part B. In the latter, we addressed information about the disease, sedentary lifestyle, access to support groups, sexuality, relationship with children and parents , religiosity, academic background, use of drugs, alcohol and smoking. The results were reported descriptively (mean, median, standard deviation, percentiles and minimum and maximum values). Furthermore, they were compared according to age groups. For the comparison between these groups, the ANOVA test was used (or Kruskall-Wallis, depending on the normality of the data). In every study, a significance level of 5% was considered. All participants over 18 years of age signed an informed consent form (TCLE), those aged 15 to 17 years and 11 months signed a Term of Assent, as well as their parents or guardians signed an TCLE. The project was approved by the Research Ethics Committee (CAAE 45709615.9.0000.5437).
Results
Among the participants, 44% (n=111) were male patients and 56% (n=141) were female. Age ranged from 15 years to 39 years, with the mean age being 25 years and the median being 23 years. All 252 patients had malignant neoplasms, 65.5% (n=165) were undergoing cancer treatment at the time and 34.5% (n=87) had already completed treatment less than 5 years ago. When evaluating the types of neoplasms, 22% (n=56) were hematologic neoplasms and the remainder solid tumors. Of the latter, bone tumors were the main ones (16%; n=32), followed by soft tissue tumors (9.5%; n=19), central nervous system tumors (9%; n=18), cancer breast cancer (8.7%; n=17), melanoma (7.5%; n=15), germ cell tumors (5.5%; n=11) and thyroid tumors (5%; n=10 ). In the interview, 79% (n=199) of the patients reported not having any physical or mental difficulties besides the cancer. Of the 17% (n=43) who reported some difficulty, the majority (43%; n=20) of the reports concerned emotional causes, followed by cardiovascular (32%; n=15) and orthopedic (18%; n) alterations =8). As for use and customs, 2% (n=5) reported being smokers and 5% (n=13) used alcohol periodically. No patient admitted the use of illicit drugs. Only 28% (n=71) of the patients were married or cohabiting at the time of the interview, 61% (n=154) lived with their parents and 71% (n=179) declared not having children. We specifically asked patients about the availability of a family doctor who could attend to them. Only 14% (n=36) of the patients answered that they had a family doctor for this purpose. Of these, 75% (n=27) said they consulted this doctor for general health issues and 97% (n=35) were satisfied with the care they received.
However, when asked about follow-up after oncological treatment, patients stated that they felt more comfortable being followed up by oncologists than by a family health team. We asked the patients about the relationships they had with other cancer patients in their age group, 50% (n=126) said they knew other cancer patients their age and 50% (n=126) said they did not. Of those who did not know other patients, 71% (n=90) responded that they would like to meet young people with the same health condition as them. Of the latter, 30% (n=27) would like to talk in person, 21% (n=19) in a group and 11% (n=10) only on social networks. When questioned about the importance of having a dedicated space for cancer care for patients their age, the majority (66.5%; n=168) considered that it would be important to have a place especially for them. The continuous variables referring to each target question of the second part of the questionnaire of this study were valued according to a scale of 1 to 10, where 1 refers to the question being of little importance to the interviewee and 10 as being extremely important (Table 1).
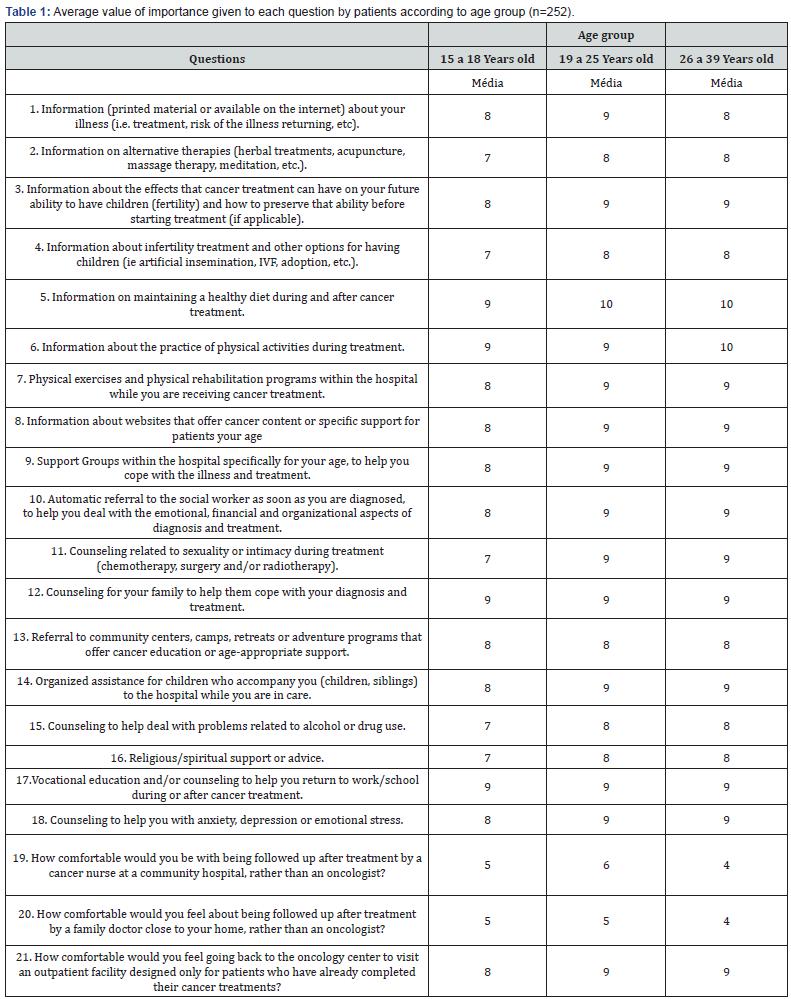
For those under 18 years of age, the highlights were information regarding a healthy diet, physical activity during treatment, counseling for their family to help them deal with their diagnosis and treatment, and returning to work or school during or after cancer treatment. Information on how to maintain a healthy diet during and after cancer treatment was at the forefront of concerns for the 19- to 25-year-old age group. For those over 26 years old, in addition to a healthy diet, the practice of physical activities during treatment was also highly relevant. The most important information, for all age groups, was about healthy diet and exercise during treatment. Next came concerns about counseling the family to deal with the illness and how to return to work or study during and after treatment. Fertility information proved to be more important for those over 18 years old, as well as information about sexuality and psychological changes during cancer treatment.Nenhuma das questões abordadas foram consideradas irrelevantes pelos pacientes entrevistados.
Discussion
Both adolescence and the young phase of life present unique challenges, and cancer can be an important complicating factor, including one of the main causes of death in these age groups [4]. The phases of adolescence and young adulthood constitute a period of transition between childhood and adult life, and for this very reason, pediatric and clinical oncology share a large proportion of these patients. However, in recent decades, treatments based on pediatric protocols have demonstrated greater survival, often with expressive values, as in the case of acute lymphocytic leukemia, where the advantage can reach up to 30% of overall survival [9]. Cure and survival rates in both children and adults have increased. However, for the age group in question, the tendency has not been this, but a decrease [10]. There are several factors that can influence this unsatisfactory statistic, adherence to treatment is undoubtedly one of these factors. If we can meet the main demands of these patients, we could offer conditions that would favor permanence and satisfaction during treatment, contributing both to survival and cure rates. By culturally validating a questionnaire that guided the organization of a program for adolescents and young adults in Canada, we provided an objective tool to implement similar programs in Latin America, particularly in Brazil [6]. With the participation of 252 adolescent and young adult patients with cancer, we were able to have a broad view of what would be the main demands with which we would work to increase the quality of life of this population, whether adapting a specific physical space or organizing a program of interdisciplinary care, during and after treatment.
Rating the proposed questions from 1 to 10, according to the degree of importance, we will be able to understand which factors would be more urgent than others, guiding us in the sequence of organization of care for these patients. We found that emotional problems were reported by 43% (n=109) of patients who reported having some alteration besides cancer, which makes the presence of psychological support a vital part of cancer treatment. Knowing the psychological condition of all patients right after diagnosis should be encouraged when considering comprehensive patient care. Demands referring to anxiety, depression or emotional stress proved to be of interest, both in Brazil and in Canada. Reinforcing the need for psychological care from the moment the patient arrives for treatment can minimize emotional sequelae. We found that information about cancer, whether in written form or online, or even in groups, is desirable. With the globalization of information, much is found about cancer on the internet. We suggest curating this material, avoiding false information and forming a solid reference base for patients and family members.
For all ages assessed, information about a healthy diet was at the top of the list of concerns, which makes the participation of the nutrition team a key part both in direct patient care and in the preparation of informative materials. Canadians share the same level of interest in this regard.
Information about physical exercise and rehabilitation during and after treatment was relevant to patients. Meeting these demands is important not only for patients who have some motor sequelae due to cancer, but also for all adolescents and young adults, since self-image is paramount at this stage of life and can be greatly altered by the disease and the treatment itself. This relevance was also found in the study carried out in Canada. The concern for the family is expressed through the importance that all ages have given to specific counseling services, as well as to monitoring social assistance. Brazilians gave greater value to these items than Canadians. School and work represent living and socializing spaces, therefore they function as factors of concern and occupy a prominent place in all age groups, in the two countries evaluated. With regard to fertility preservation, or even the treatment of infertility, those over 18 showed greater concern. This type of care is not generally provided by the Unified Health System, so it is a difficult topic to approach in our country.
Canadians show greater interest in this topic than Brazilians. We can infer that this fact is due to economic and technological differences between countries in North and South America. Regarding the physical space, we verified, through the answers obtained, that it is important to have a place for adolescents and young adults, which can be achieved without much cost, reserving a space for this population within pediatric oncology services. It is important to remember that there are siblings and even children of patients, who would be healthy children present in the outpatient environment often enough for us to think of an adequate place to receive them. Undoubtedly, minor companions are always present during treatment and welcoming them means welcoming the family as a whole, one of the objectives of the current interdisciplinary view. Canadians gave less importance to this factor than Brazilians, suggesting that they have better economic and family support than our patients. Information about alcohol and drugs received comparatively lower average scores in both Canada and Brazil. We infer that there may be interference because this is a delicate question and that the answer may not match reality, simply because it is a questionnaire, where the patient may not feel free to be honest. However, we believe that this topic is still quite relevant to be addressed with these patients.
When we compare our results with the Canadian work we are based on, we see some significant differences. [7]. In our midst, spiritual or religious counseling did not obtain a high average, however, it was much higher than that of Canadians, which denotes cultural differences between the studied populations. Chaplaincy services are not present in most Brazilian hospitals, which is a marked deficiency, given the cultural importance of the topic for Latin Americans in general.
Conclusion
In this work, we present the main demands of adolescents and young adults with cancer, validated for our cultural reality, an objective and easy-to-use tool for those medical services that want to better serve this specific public. Adolescents and young adults with cancer are urgently required to find health services that meet their main demands. Starting with an oncological treatment that achieves better cure and survival rates. Physical spaces designed for patients and their families are rarely found in Brazil. We suggest that pediatrics embrace a large number of these patients, especially those under 25 years of age, adapting existing spaces and formatting an interdisciplinary service that responds to the demands listed here.
The presence of pediatric oncologists composing the clinical staff of adult oncology services allows adolescents and young adults treated at these services to be included in pediatric protocols that have proven to achieve better cure rates. The interaction between these two oncological worlds, that of adults and that of children, is beneficial to the patient and the entire health team, bringing reciprocal learning and greater patient safety.
Acknowledgment
We thank the members of the Research Support Center (NAP) of the Pio XII Foundation, Barretos, SP, Brazil. Special thanks to Dr. Carlos Paiva and Dr. Edenir Inez Palmiero, for her support throughout the work within the Pio XII Foundation.
References
- Close AG, Dreyzin A, Miller KD, Seynnaeve BKN, Rapkin LB (2019) Adolescent and young adult oncology-past, present, and future. CA: a cancer journal for clinicians 69(6): 485-946.
- Bleyer A, Ferrari A, Whelan J, Barr RD (2017) Global assessment of cancer incidence and survival in adolescents and young adults. Pediatric blood & cancer 64(9).
- Camargo B, Oliveira J F P, Santos M O, Rebelo M S, Reis, R S (2017) Incidencia, mortalidade e morbidade hospitalar por câncer em crianças, adolescentes e adultos jovens no brasil: informações dos registros de câncer e do sistema de mortalidade Rio de Janeiro, INCA 2017: 35.
- Shaw PH, Reed DR, Yeager N, Zebrack B, Castellino SM, et al. (2015) Adolescent and Young Adult (AYA) Oncology in the United States: A Specialty in Its Late Adolescence. Journal of pediatric hematology/oncology 37(3): 161-169.
- Zebrack BJ (2011) Psychological, social, and behavioral issues for young adults with cancer. Cancer. 117(10 Suppl): 2289-2294.
- Guillemin F, Bombardier C, Beaton D (1993) Cross-cultural adaptation of health-related quality of life measures: literature review and proposed guidelines. J Clin Epidemiol 46(12): 1417-1432.
- Gupta AA, Edelstein K, Albert-Green A, D'Agostino N (2013) Assessing information and service needs of young adults with cancer at a single institution: the importance of information on cancer diagnosis, fertility preservation, diet, and exercise. Support Care Cancer 21(9): 2477-2484.
- Munnangi S, Boktor SW (2020) Epidemiology of Study Design. Treasure Island, FL, USA.
- Ram R, Wolach O, Vidal L, Gafter-Gvili A, Shpilberg O, et al. (2012) Adolescents and young adults with acute lymphoblastic leukemia have a better outcome when treated with pediatric-inspired regimens: systematic review and meta-analysis. American journal of hematology 87(5): 472-478.
- Bleyer A (2007) Young adult oncology: the patients and their survival challenges. CA: a cancer journal for clinicians 57(4): 242-55.






























