Endolymphatic sac tumor (ELST): A rare Radiological case report and review of literature
Dr Amani Saleh Hadi Saeed*
Specialist of Clinical Oncology and Nuclear Medicine, National Oncology Center-Aden, Yemen
Submission: June 26, 2022; Published: July 13, 2022
*Corresponding Address: Dr. Amani Saleh Hadi Saeed, Specialist of Clinical Oncology and Nuclear Medicine, National Oncology Center-Aden, Head of health education unit for Arab Council of Academic and Competencies- branch of Yemen, Yemen
How to cite this article: Dr Amani Saleh Hadi Saeed. Endolymphatic sac tumor (ELST): A rare Radiological case report and review of literature. Canc Therapy & Oncol Int J. 2022; 21(5): 556075. DOI:10.19080/CTOIJ.2022.21.556075
Abstract
An endolymphatic sac tumor (ELST) is a rare indolent but locally aggressive tumor arising in the posterior petrous ridge of temporal bone. which can be encountered sporadically or in Von Hipple-Lindau (VHL) diseased. With less than 200 case reported. Although ELST presents benign appearance in histopathology, it can present aggressive destructive behavior in clinical. Treatment for ELST is complete surgical excision. there is still controversy about other treatment, such as radiotherapy and gamma knife surgery. Chemotherapy salvage therapy in trials of neoplasm of associated syndrome has targeted angiogenesis with variable response. We present case of endolymphatic tumor in 62-year-old man. he presented with right -side skull swelling post trauma. Surgical excision was performed, and diagnosis of the endolymphatic sac tumor was made without VHL. Endolymphatic tumor is Lowe grad adenocarcinoma that originate from the endolymphatic sac. the definitive diagnosis requires combination of clinical features, radiological finding and pathological correlation. Discussion: we discuss the radiological features and histopathology of this rare tumor.
Keywords: Endolymphatic sac tumor; Radiation therapy; Surgery; Temporal bone; Prognosis; Von Hipp-Lindau
Introduction
Endolymphatic sac tumor is rare form of benign tumor arising from endolymphatic duct and sac (EDS) [1]. Endolymphatic sac tumors are known to occur more in frequently in patients with VHL diseased, with up to 16 percent of patients with VHL diseased harboring an ELST [2]. Patients withVHL diseased are more likely to have bilateral ELSTs. VHL diseased is autosomal dominate syndrome due to dilation or mutation in the VHL gen located on short arm of chromosome 3 (3p25-p26) [3,4]. The tumor was first identified during sac decompression surgery in 1984 [5]. Because of the rarity of this tumor, it can easily be confused
With other tumors such as:
Middle ear carcinoma
Choroid plexus papilloma
Para ganglioma
Papillary ependymoma
Metastatic renal cell carcinoma
Metastatic thyroid papillary carcinoma, kidney, breast and lung
The tumor is unencapsulated, destructive lesion, showing simple, coarse papillae within cystic spaces lined by cells that are low cuboidal to columnar. The neoplastic cell is positive with CK7, CAM5.2, CAIX. While focally positive with S100protien but negative with thyroglobulin, TTF-1, RCC and transthyretin. patients characteristically present with unilateral sensor-ineural hearing loss, tinnitus, otalgia, otorrhea, vertigo, ataxia and facial nerve paresis. Symptom typically progress over a period of several year [6,7].
Radiological finding
The imaging hallmark of ELST is a retro labyrinthine mas with associated with osseous erosion. CT imaging show tumor with bone destruction. MRI scans of hypo -intensity on both T1 and T2 images with strong post-gadolinium enhancement [8].
Case Presentation
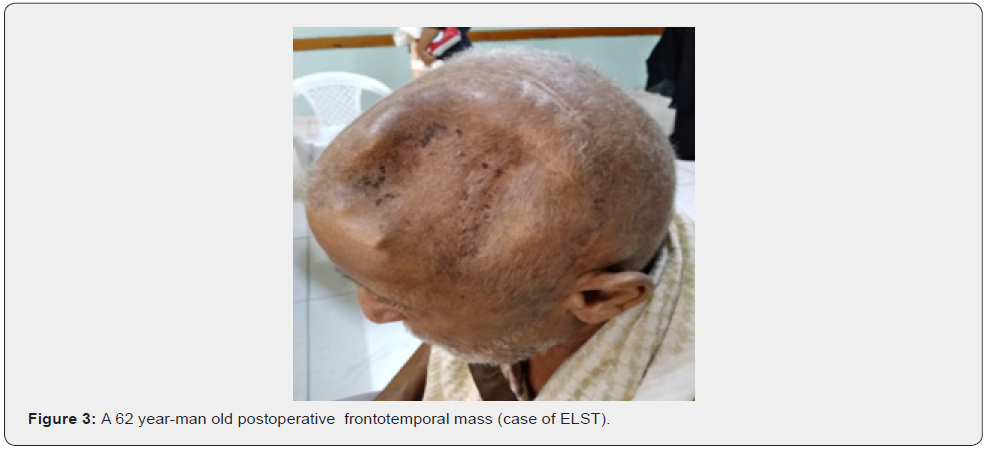
A 62-years -old man present with a chief complaint of headache and skull swelling post trauma. There was no tinnitus, otalgia, otorrhea, vertigo or facial nerve paralysis. The patient was operated by craniotomy. The whole tumor was removed, fat and fascia lata were used to close the defect and achieve a watertight closure. The muscle was approximated, and the incision was closed in standard fashion (Figure 3).
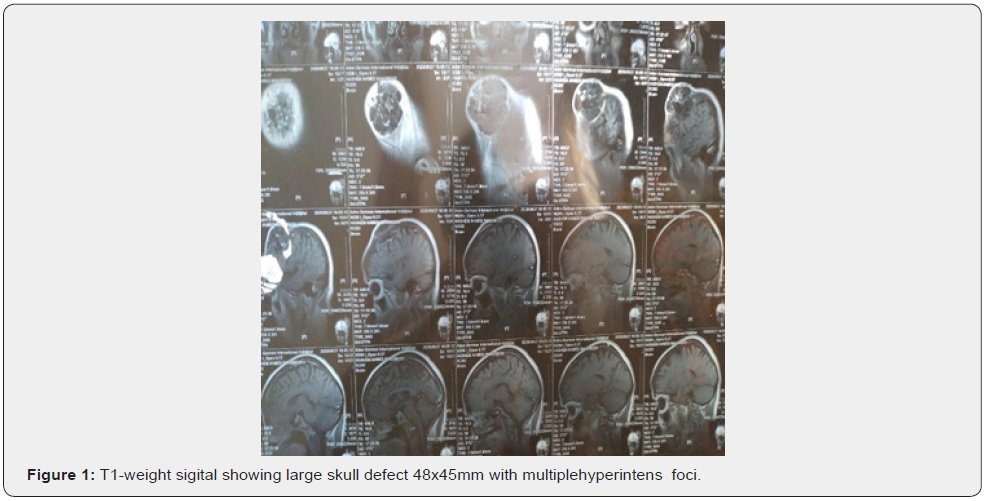
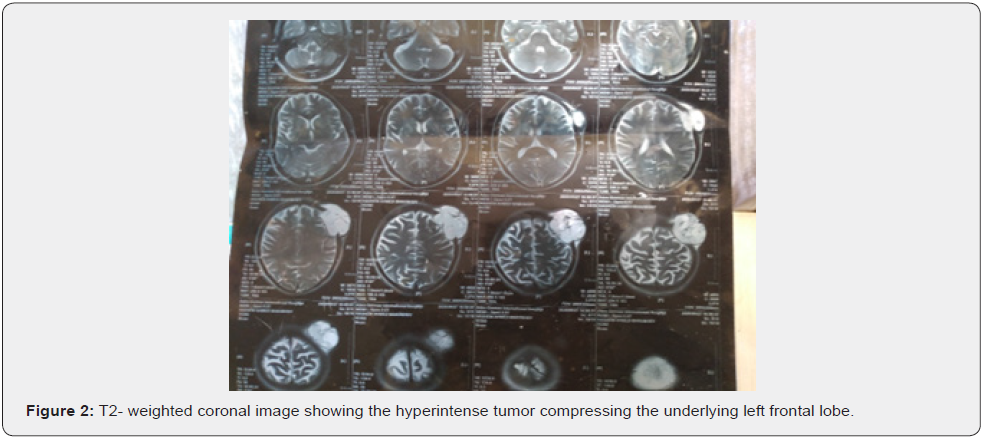
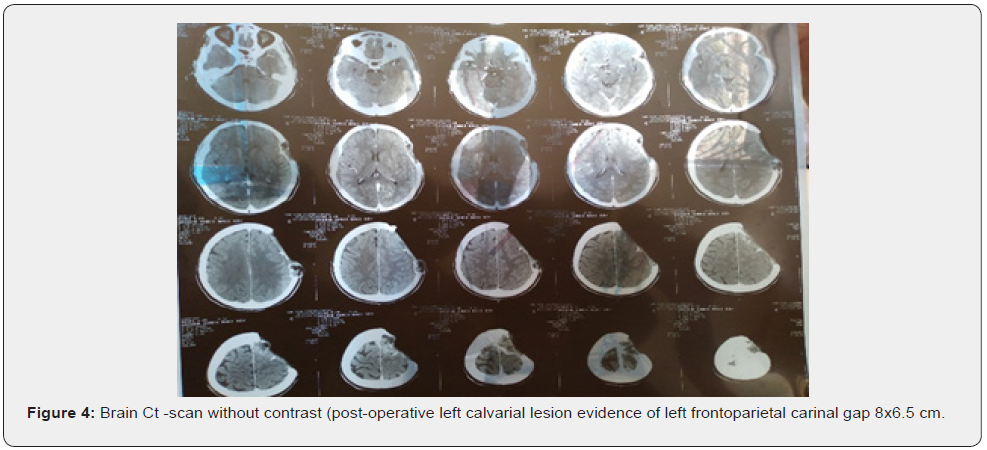
(Figures 1 and figures 2 & 6) A magnetic resonance imaging (MRI) scan26/9/2020 showed well defined calvarial mass in left frontoparietal bones measured about 58mmx60x61mm in its maximal. Anterio-posterior, transver & cranio-caudal dimension respectively, the lesion has large extracranial and intracranial components destruction of the intervening bones forming large skull defect measured about 48x45mm, the lesion appear heterogenous hypointense with multiple hyperintense foci in T1,and hyperintense in T2weigheted,in postcontrast administration, the intracranial component exerting significant mass effect compressing the underlying left frontal lobe with no remarkable ventricular obliteration or midline shifting the possibility of intradiploic calvarial neoplasm in left frontoparietal bones suggestive of dermoid cyst. Post-operative CT scan 18/11/2020 show total removal of the lesion (Figure 4). evidence of smooth liner enhancing dura at surgical bed, no focal recurrence, no collection seen or mass.
Pathological findings (7/11/2020)
Gross Description: 1- A solid -cystic mass with gray-tan outer surface measuring 7x6x2,5 cm. cross sectioning shows multiple cystic spaces separated by white -tan septa and filed with yellowish-red fluid.
2. Apacie of gray-tan tissue measuring 3x3x1.3 cm, along with multiple pieces of gray-tan soft tissue and bone measuring in aggregate 4x4x2cm. representative sections submitted for examination
3. multiple pieces of gray-tan soft tissue and bone measuring in aggerate 6x6x2cm. representative section submitted for examination.
Micro Description
section show an ill-defined tumor formed of irregular microcystic /tubulocystic structures variably lined by bland to mildly atypical flattened, cuboidal, and columnar cell epitheliums with frequent intraluminal projection and pink secretions surrounded by a fibrous stroma with mild to moderate desmoplastic reaction. The tumor invades the surrounded soft tissue and bone. Recommend radiotherapy and fellow up, in 29/6/2021 evualtion done by Ct scan brain with contrast was showed: large ill defined, lobulated septate cystic lesion with enhanced peripherally and internal septation noted in left frontotemporal region with underline cranial destruction measured about 59x38x60mm in temporal region and second lobulated lesion measured about 27x40x28 mm in frontal region, these lesions mildly compressed underlie brain parenchymal.
Cytology Report17/3/2021(scalp mass, lumpectomy)
Macro: two fragment of tissue biopsies the largest 5x4x3 cm and the smallest 4x3x2 cm irregular and brownish. cut section multiple small cysts (spongy like). Micro: microscopic examination reveals large mass formed by multiple irregular space lined by columnar to low cuboidal cells, and some spaces are closely packed and other spaces show vague papillary like growth and these spaces appears separated by fibrous stromal with focal areas of bone metaplasia and all appears surrounded by fragmented mature bone. diagnosis as recurrent Endolymphatic sac tumor.
7/9/2021 : brain CT scan
Well-defined heterogenous enhancing structure measure about 29x24 mm seen in the posterior end of the surgical bed of the fronto-parietal scalp region, in addition to there is thicking and heterogenous enhancing area measured about 37x23mm seen in the high region of anterior frontal scalp surgical bed as well as there is erosion of adjacent bone, picture of recurrent versus metastatic changes in the surgical bed and skull bone.
Chest CT scan 7/9/2021
Multiple variable sizes nodules scattered in both lung fields, the largest measured in right side 20x15mm in posterior segment of right upper lung lobe and the largest measured in left side 11x8 mm in in anterior segment of left upper lung lobe, picture metastatic pulmonary changes.
Abdomen CT scan 7/9/2021
Well-defined hertogenose enhancing lesion measured about 8x7x7 cm with lobulated outline and peripherally enhancing as well as foci of calcification component in which this lesion infiltered the right hepatic lone segments VI, VII and VII with reduction of volumes of lobe, picture first possibility of hepatic metastatic changes.
Expansile and lytic lesion involving left iliac bone in which the affected area measure about26x28x19mm, picture of metastatic bony changes. Normal other organs, no fluid collection or sizable lymphadenopathy in abdominal and pelvic cavity. At that time , his laboratory were all with in normal limits’ remained (Performons status score 0) ECGO, he was then started on pazopanib 400mgx 2tab,which was well tolerated for nine month until publish this article with zoledronic acids 4mg monthly. CT-scan after three months of pazopanib was show stationary course for recurrent brain mass and lung metastasis , no any complain for headache or facial palsy or cough only complain bon pain, continue on pazopanib and zoledronic acid till publish this article with stabilize his condition
Brian CT scan with contrast 27/3/2022
Evidence of craniotomy of left fronto-temporal=-parietal with resection tumor with evident residual tumor at peripheral edge of craniotomy seen as heterogonous lobulated on upper partial measure about 23x20mm ,and left temporal measured about 25x 20mm,normal ventricular system with no midline shift ,normal posterior fossa structures (Figure 5).
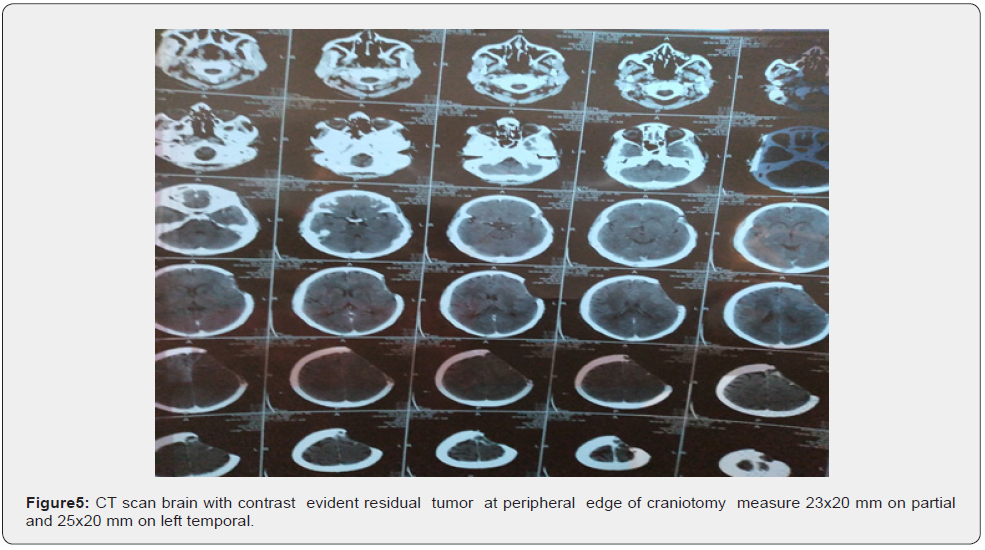
Chest and Abdomen CT scan with contrast 27/3/2022
Evidence of multiple variable size pulmonary nodules largest on in posterior segment of right upper lobe measure about 20x13mm.multiple heterogenous well define, lobulated focal hepatic lesion largest one seen in right hepatic lobe with calcify spots measured about 70x63 mm bulgy to inferior liver surface. Destructive lytic lesion with soft tissue component seen in left rib 5th, in left iliac bone and lower sacrum, also lytic lesion in inD1, D3.no other abnormality detected. In compere to pervious study dated in 7/9/2021 their progression course informs increase metastatic bone lesion (Figures 1-5).
Discussion
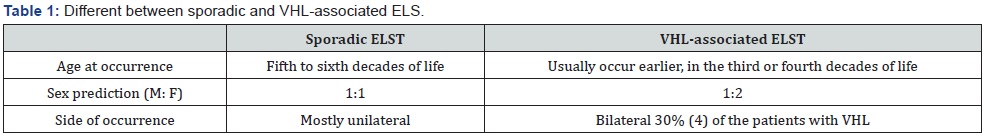
With 200 reported case date [9]. ELTSTs are rare and most commonly occur in fifth and sixth decades of life. They may be sporadic or associated with VHL syndrome (Table 1). Treatment of ELST involves local resection of the tumor or radical mastoidectomy alone, or in combination with radiotherapy. early surgical excision is the best treatment when tumor is small. Local recurrence after surgery can occur. Bambakidis et al. [10] devised a grading system to plan the surgical approach (Table 2).
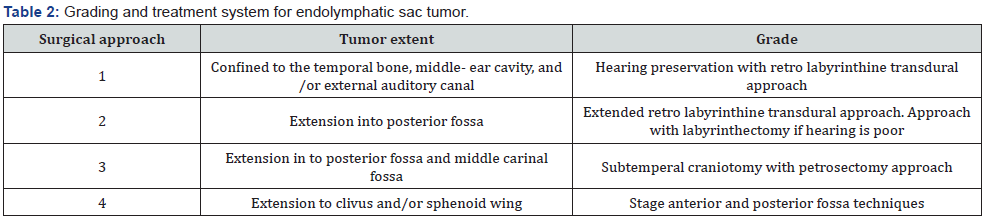
In our case complete removal of tumor was possible because of small mass than did not need preoperative embolization (Figures 3 & 4). The curative effect of radiation and gamma knife surgery remain controversial [4]. Recommendation from some literatures and postoperative radiotherapy may be effective as adjuvant treatment for cases of recurrent or difficult resection [6,7]. In our case radiotherapy given for recurrent mass. Metastases from ELST are very rare. In this case develop metastases to bone and lung and multiple focal hepatic lesion. patient treated with pazopanib 800mg tab daily for six months with stabilize his condition and patient alive till publish this article. There is no standard or established chemotherapeutic regimen ,which is especially problematic for patients in whom resection is subtotal or not possible due to structural limitation or vascular compromise .however, a posited role of antiangiogenic agent such as sunitinib and bevacizumab in the management of VHL may provide alternative treatment for ELSTs [10-13]. For patient in whom these agents are ineffective or not tolerated ,novel agent such as pazopanib a multi-kinase inhibitor and angiogenic may provide new avenues for treatment. More recently Jonasch et al. demonstrated in phase II, single center trial that patient with diagnosed VHL may response to tumors of multiple organs when started on pazopanib therapy [14].
Conclusion
Endolymphatic sac tumor are rare tumors of the temporal bone. due to rare cases reported A multidisciplinary treatment approach including neurosurgeon, radiologists, neuropathologists and radiation oncologists should provide to patients with ELST to achieve adequate control of these locally aggressive tumors.
References
- Micheal L (2007) Orgin of endolymphatic sac tumor. Head Neck Pathol 1(2): 104-111.
- Choo D Shotland L, Mastroianni M, Gladys Glenn, Carter van Waes, et al. (2004) Endolymphatic sac tumors in Von Hipple Lindau diseased Neurosurgery 100(3): 480-487.
- Friedirch CA (1999) von HippleLindau syndrome. Pleomorphic condition cancer 86: 2478-2482.
- Cheng X, qin S, Wang X, Li P, Shrestha Wang, et al. (2011) Gamma knife treatment of an endolymphatic sac tumor: unique features of a case and review of the literature. Neurol india 59(4): 608-611.
- Hassard AD, Boudreau SF, Cron CC (1984) Adenoma of the endolymphatic sac. Otolaryngology J 13(4): 213-216.
- Kuppferman ME, Bigelow DC, Carpentieri DF, Billlaniuk LT, Kazahaya K (2004) Endolymphatic sac tumor in 4year-old boy. Otol Neurotol 25(5): 782-786.
- Folker RJ, Meyerhoff WL, Rushing EJ (1997) Aggressive papillary adenoma of the cerebellopontine angle: case report of endolymphatic sac tumor. Am JOtolaryngol 181(2): 35-39.
- HoVT, Rao VM, Doan HT, D O Mikaelian (1996) Lowe grad adenocarcinoma of probable endolymphatic sac origin: CT and MR appearance. AJNR Am JNeuroradiol 17(1): 168-170.
- Wick CC, Manzoor NF, Semaan MT, Megerian CA (2015) Endolymphatic sac tumor. Otolaryngology Clin North Am 48(02): 317-330.
- Bambakidis NC, Megerian CA, Ratcheson RA (2004) Differential grading of endolymphatic sac tumor extension by virtue of vonHippel-Landau disease status. OtoNeurotol 25(5): 773-781.
- Alkhotani A, Butt Khalid M, Binmahafoodh M, Al-said Y (2019) Endolymphatic sac tumor at cerbllopontine angle: a case report and review of literature. Int J Surg Case Rep 58: 162-166.
- Jimeenez C, Cabanillas MS, Santarpia L (2009) use of the tyrosine kinase inhibitor sunitinib in patient with von hipple-Landau disease: targeting angiogenic factors in pheochromocytoma and other VonHipple -Landau disease -related tumors. Clin Eendocrinol Metab 94(2): 386-391.
- Jonasch E, McCutcheon IE, Waguespack SG, S Wen, D W Davis, et al. (2011) Pilot trial of sunitinib therapy in patient with VonHipple Lindau disease. Ann Oncol 22(12): 2661-2666.
- Jonasch E, McCutcheon IE, Gombos DS et al. (2018) Pazopanib in patients with Von Hipple Lindau disease: single arm. single -center, phase II trial A phase II, single-center trial of pazopanib in patients with diagnosed VHL that demonstrated response of multiple tumor types to this agent. Lancet Oncol 19(10): 1351-1359.






























