The Demagogic Water Bag-Chorioamnionitis
Anubha Bajaj*
Histopathologist in A B Diagnostics, New Delhi, India
Submission: April 29, 2022; Published: June 16 2022
*Corresponding Address: Anubha Bajaj, Histopathologist in A B Diagnostics, New Delhi, India
How to cite this article: Anubha Bajaj. The Demagogic Water Bag-Chorioamnionitis. Canc Therapy & Oncol Int J. 2022; 21(5): 556071. DOI:10.19080/CTOIJ.2022.21.556071
Preface
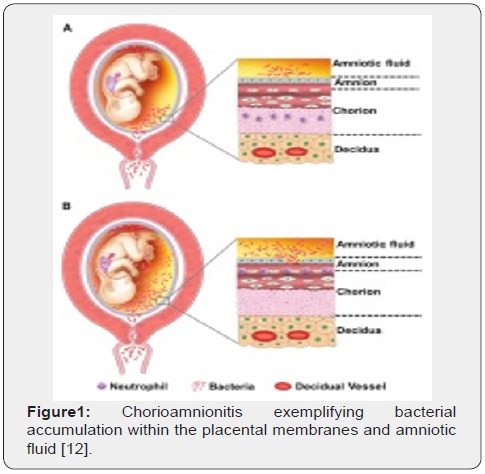
Chorioamnionitis is an inflammation of foetal membranes wherein the infection may occur prior to labour, during labour or following delivery. The terminology is derived from Greek “chorion” and “amnion” whereas chorioamnionitis may be discerned during delivery or as a post-mortem condition upon histological assessment of placenta and umbilical cord. Majority of subjects with chorioamnionitis are in labour or exhibit ruptured membranes. The condition is additionally designated as acute chorioamnionitis, histologic chorioamnionitis, chorionitis, subchorionitis and subacute chorioamnionitis. Chorioamnionitis is associated with inflammation of amniochorionic placental membranes occurring because of microbial invasion. Diffuse neutrophilic infiltration of maternal chorion is accompanied by sub-chorionic deposition of fibrin whereas neutrophils emerge from inter-villous spaces or post-capillary venules of the decidua. Untreated chorioamnionitis may engender maternal and foetal morbidity and mortality. Also, severe neonatal morbidity and mortality is associated with disease occurrence within preceding gestations. Pertinent antibiotic therapy decimates disease incidence and severity of maternal and neonatal chorioamnionitis. The condition is alleviated in a majority of incriminated subjects and antibiotic therapy following delivery is usually unrequired.
Disease Characteristics
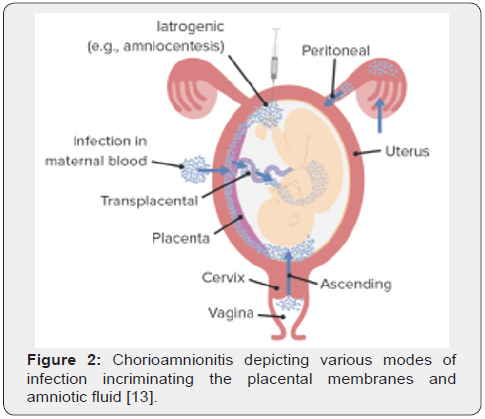
Commonly, chorioamnionitis is associated with maternal ascending infection, spontaneous preterm or prolonged labour, prolonged rupture of membranes (PROM), consumption of tobacco, nulliparous pregnancy, meconium-stained fluid, multiple vaginal examinations following rupture of membranes and in females with previously established bacterial or viral infections [1,2]. Nevertheless, the condition may arise at term and in females devoid of preceding infections. Occasionally, chorioamnionitis may be associated with foetal inflammatory response along with chorionic vasculitis and funisitis [1,2]. The infection may arise within the chorion or sub-chorion and exhibits activation of inflammatory pathways by diverse microbial agents along with neutrophilic infiltration of placental membranes. Besides, placental leukocyte engendered, cytokine- induced systemic consequences may be observed [1,2]. Chorioamnionitis can be categorized as
• acute chorioamnionitis
• subacute chorioamnionitis
• chronic chorioamnionitis.
Chorioamnionitis is an infectious, inflammatory process where the in-utero inflammation is concordant with conditions such as preterm birth, brain anomalies or retinopathy [1,2]. Subacute chorioamnionitis occurs due to extensive infection emerging with minimally virulent pathogens. Chorioamnionitis or the sub-acute variant may be associated with infant chronic pulmonary disease. Of obscure an etiology, chronic chorioamnionitis is associated with delayed preterm delivery. Chronic chorioamnionitis is a common condition associated with retinopathy occurring within premature, very low birth weight babies with impaired brain development. The condition is common in young women or in subjects with infected amniotic fluid and is rarely infectious at term delivery [1,2]. Infection may arise due to bacterial, fungal or viral agents. Bacterial agents inducing chorioamnionitis pertain to population and geographic location of the disease. Bacteria inducing chorioamnionitis are comprised of group B streptococcus, Mycoplasma pneumoniae, Ureaplasma, Gardnerella vaginalis, Escherichia coli or Bacteroides spp commonly, infection arises due to combination of two or more microbial agents. Ascending bacterial infection occurs due to genital mycoplasma as Ureaplasma urealyticum or Mycoplasma hominies, anaerobic organisms as Gardnerella vaginalis or Bacteriodes or aerobic organisms as group B Streptococcus, Escherichia coli or Fusobacterium nucleatum [3,4].
Fungal agents as Candida spp may engender chorioamnionitis with consequent preterm birth and adverse foetal outcomes. Parasitic agents as Trichomonas spp initiate chorioamnionitis in adolescents with sexually transmitted infections (STIs) [3,4]. Chorioamnionitis may be associated with vertical transmission in pregnancy. Quantifiable per- vaginal examinations during labour influences the incidence of chorioamnionitis. However, maternal infection with human immunodeficiency virus (HIV) is non-concordant with occurrence of chorioamnionitis [3,4]. Chorioamnionitis occurs in an estimated 4% of term deliveries. Nevertheless, disease frequency is enhanced in preterm birth or premature rupture of membranes (PROM) [3,4]. Pertinent staging of chorioamnionitis may be achieved by Maternal inflammatory response delineated as
i. Stage 1 composed of acute subchorionitis or chorionitis
ii. Stage 2 comprised of acute chorioamnionitis (polymorphonuclear leukocytes extend into fibrous chorion or amnion)
iii. Stage 3 is constituted of necrotizing chorioamnionitis depicting karyorrhexis of neutrophils, necrosis of amniocytes or hyper-eosinophilia of amniotic basement membrane [3,4].
Foetal inflammatory response is denominated as
i. Stage 1 comprised of chorionic vasculitis or umbilical phlebitis
ii. Stage 2 which incriminates the umbilical vein and singular or dual umbilical arteries
iii. Stage 3 exhibits necrotizing funisitis Grading of maternal chorioamnionitis is designated as
• Grade 1 composed of non-severe instances
• Grade 2 exemplifying severe disease comprised of confluent neutrophils or associated with sub-chorionic micro-abscesses.
Grading of foetal chorioamnionitis is defined as
• Grade 1 or non-severe disease
• Grade 2 or severe disease with almost confluent, intramural neutrophils along with attenuation of vascular smooth muscle [3,4].
Clinical Elucidation
Acute chorioamnionitis exhibits cogent disease representation wherein the amniotic fluid may be incorporated within the inflammatory process. The asymptomatic, clinically silent histologic chorioamnionitis is associated with sterile placental or amniotic fluid cultures [5,6]. Symptomatic chorioamnionitis displays an intense concurrence between histologic chorioamnionitis and clinical features as pyrexia, uterine tenderness, meconium aspiration syndrome and foulsmelling vaginal discharge. Histologic chorioamnionitis with vasculitis depicts an enhanced incidence of premature rupture of membranes and preterm delivery [5,6]. Chorioamnionitis occurring in term deliveries is associated with prolonged rupture of membranes (PROM) or failure of progression of labour.
Chorioamnionitis accompanying preterm labour may terminate in preterm delivery [5,6]. Chorioamnionitis associated with ascending infections originates within lower genitourinary tract as cervix or vagina and migrates towards the amniotic cavity. Vertical transmission may be induced by bacterial or viral agents wherein infection is transmitted to the fetus [5,6]. Chorioamnionitis is associated with pyrexia, elevated white blood cell (WBC) count, uterine tenderness, abdominal pain, foul-smelling vaginal discharge along with foetal and maternal tachycardia [5,6]. The condition may induce foetal infection, neonatal sepsis, stillbirth, spontaneous preterm birth and foetal central nervous derangements. Foetal inflammatory reaction is comprised of multi-organ injury, chronic pulmonary disease, periventricular leukomalacia and cerebral palsy [5,6]. Appropriate clinical discernment of chorioamnionitis necessitates discernment of pyrexia between 100.4 F and 102.2 F within 30 minutes in accompaniment with minimally a singular, clinical symptom [5,6].
Histological Elucidation
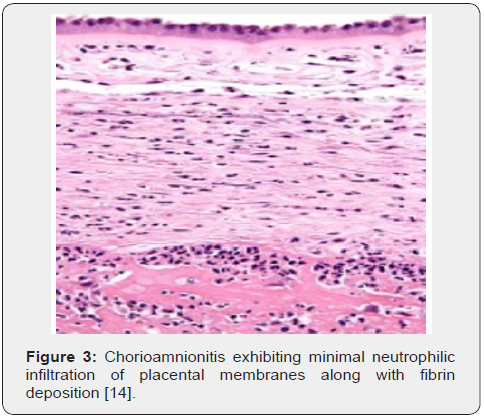
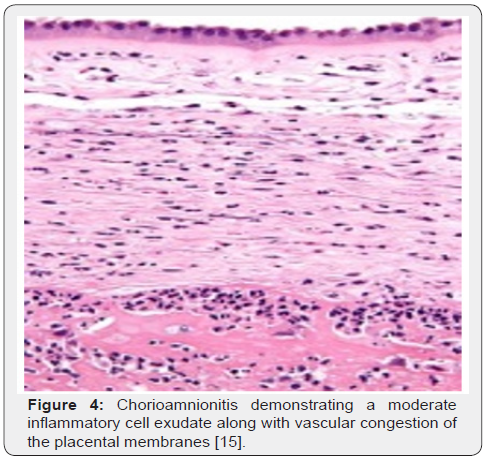
Upon gross examination, dull, opaque, yellow-green placental membranes and cloudy or purulent amniotic fluid is observed. Preterm birth is associated with acute, marginal haemorrhage. Chorioamnionitis arising due to infection with Candida albicans displays multifocal abscesses [6,7]. The inflammatory chorioamnionitis appears as a mild to severe infection. Term or preterm gestation may exhibit morphologic features consistent with chorioamnionitis [6,7]. The condition is associated with normal or infected foetal membranes. Amniotic fluid can be clear or cloudy [7,8]. Upon microscopy, decidua enunciates an acute inflammation with infiltration of neutrophils. Severe instances depict configuration of microabscesses. Neutrophils accumulating within the amniotic cavity are contributed from the foetus. Chorioamnionitis arising within extremely premature infants depict an infiltration of admixed maternal and foetal neutrophils confined to the amniotic cavity [7,8]. Upon microscopy, neutrophilic infiltrate of placental membranes and superimposed chorionic plate is observed. A variable foetal inflammatory reaction is delineated with chorionic plate vasculitis, umbilical phlebitis, umbilical arteritis and concentric umbilical peri-vasculitis [7,8]. Subacute chorioamnionitis exhibits a mixed inflammatory cell infiltrate composed of neutrophils and mononuclear cells as macrophages [7,8]. Inflammatory exudate is predominantly confined to the amnion and upper chorion. Polarization of mononuclear cells may occur towards the amnion. Severe disease enunciates necrosis of the amnion [7,8]. Occasionally, acute intervillositis may ensue due to Listeria monocytogenes, peripheral funisitis arises because of infection with Candida and acute deciduitis emerges within preterm deliveries [7,8]. Chronic chorioamnionitis preponderantly displays lymphocytic infiltration of chorioamnion [7,8] (Figures 1-8).
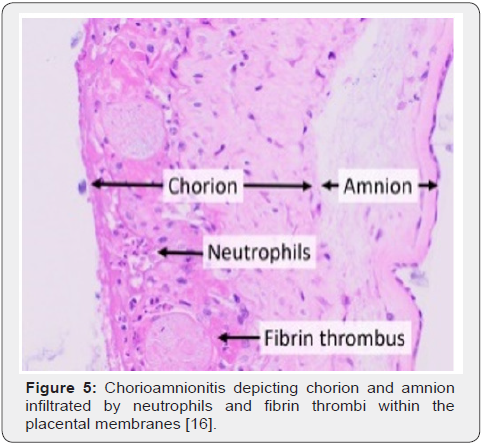
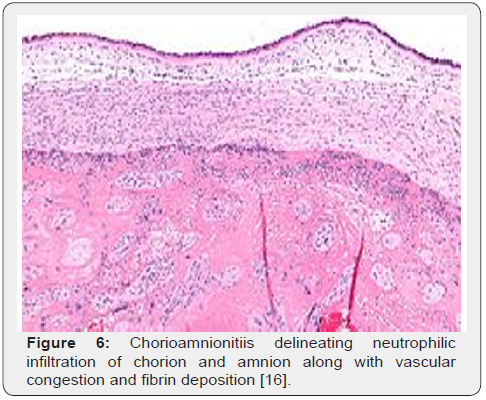
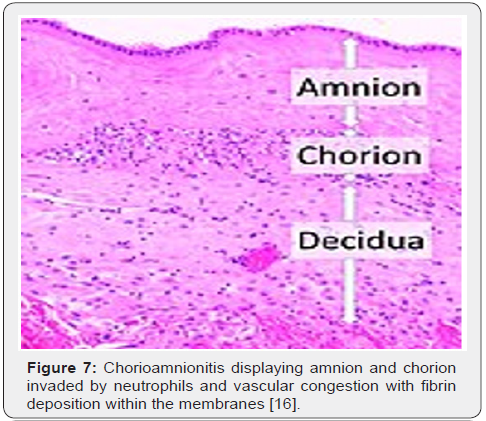
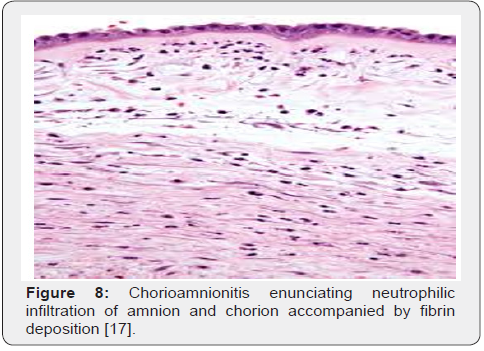
Differential Diagnosis
Chorioamnionitis requires a segregation from conditions that engender abdominal pain, pyrexia, uterine tenderness or tenderness during labour. Demarcation is necessitated from common infections such as appendicitis, urinary tract infection, pyelonephritis or pneumonia. Appropriate distinction can be obtained with comprehensive history, cogent physical examination and additional, ancillary investigations [9,10].
Investigative Assay
Preliminary diagnosis of chorioamnionitis necessitates precise clinical assessment of mother and foetus. Evaluation of amniotic fluid and maternal hematological parameters is required [9,10]. Comprehensive clinical history describing maternal age, gestational age, parity, complications of pregnancy, status of membranes (ruptured or intact), occurrence of meconium, associated sexually transmitted infections (STIs), urinary tract infections (UTIs) and recent illnesses is required [9,10]. Competent physical examination with assessment of vital parameters and state of abdomen, vagina and uterus is mandated [9,10]. Although ascertained, maternal white blood cell (WBC) count is inadequate in assessing microbial invasion or inflammation of amniotic cavity, especially in subjects with premature rupture of membranes (PROM). Bacterial cultures of the cervix are non concurrent with infections secondary to chorioamnionitis. Microbial cultures of amniotic fluid may aid in isolating the causative organisms [9,10]. Periodic acid Schiff (PAS) and Gomori methanamine silver (GMS) stains can be adopted to demonstrate blastopores and hyphal forms of Candida spp. Gram stain is usually non conclusive [9,10]. Chorioamnionitis or infection of amniotic fluid occurring due to maternal inflammatory reaction is appropriately assessed with cogent tissue sampling of the placenta [9,10].
Therapeutic Options
Chorioamnionitis is preponderantly managed by pertinent maternal and foetal antibiotic therapy. Commonly, ampicillin and gentamicin are efficacious. Alternatively, clindamycin, cefazolin and vancomycin may be employed in subjects allergic to penicillin. Additional broad-spectrum antibiotics may be mandated contingent to clinical status of incriminated subjects [10,11]. Chorioamnionitis may engender endometritis whereas postpartum antibiotics may not decimate possible endometritis following chorioamnionitis [10,11]. Maternal sequelae of chorioamnionitis emerge as severe pelvic infections, subcutaneous wound infection, preterm or operative delivery, postpartum haemorrhage and maternal sepsis. Besides, chorioamnionitis is associated with vertical transmission of human immune deficiency virus (HIV) infection in pregnancy (10,11]. The neonate incriminated with chorioamnionitis may be afflicted with premature birth, cerebral palsy, retinopathy of prematurity, neurologic anomalies, respiratory distress syndrome, and bronchopulmonary dysplasia arising within premature infants, neonatal sepsis and neonatal mortality. Neonatal sepsis associated with chorioamnionitis exhibits a culture- negative bacteremia in majority (99%) instances [10,11]. Perinatal listeriosis is associated with enhanced morbidity wherein contemporary antibiotics appear ineffectual in treating listeriosis-accompanying chorioamnionitis [10,11]. Acute sub-chorionitis exhibits a favorable prognosis whereas appearance of necrotizing chorioamnionitis is associated with an inferior prognostic outcome [10,11].
References
- Fowler JR, Simon LV (2022) Chorioamnionitis. Stat Pearls Int Treasure Island, Florida.
- Bennet L, Dhillon S, Chris A Lear, Lotte van den Heuij, Victoria King et al. (2018) Chronic inflammation and impaired development of the preterm brain. J Reprod Immunol 125: 45-55.
- Maki Y, Fujisaki M, Yuichiro Sato, Hiroshi Sameshima (2017) Candida Chorioamnionitis Leads to Preterm Birth and Adverse Foetal-Neonatal Outcome. Infect Dis Obstet Gynecol 9060138.
- Palmsten K, Nelson KK, Louise C Laurent, Soojin Park, Christina D Chambers, et al. (2018) Subclinical and clinical chorioamnionitis, foetal vasculitis and risk for preterm birth: A cohort study. Placenta 67: 54-60.
- Bierstone D, Wagenaar N, Dawn L Gano, Ting Guo, Gregory Georgio et al. (2018) Association of Histologic Chorioamnionitis With Perinatal Brain Injury and Early Childhood Neurodevelopmental Outcomes Among Preterm Neonates. JAMA Pediatr 172(6): 534-541.
- Garcia-Flores V, Romero R, Derek Miller, Yi Xu, Bogdan Done, et al. (2018) Inflammation-Induced Adverse Pregnancy and Neonatal Outcomes Can Be Improved by the Immunomodulatory Peptide Exendin-4. Front Immunol 9: 1291.
- Huber BM, Meyer Sauteur PM, Wendy W J Unger, Paul Hasters, Marcel R Eugster, et al. (2018) Vertical Transmission of Mycoplasma pneumoniae Infection. Neonatology 114(4): 332-336.
- Suzuki S (2019) Association between clinical chorioamnionitis and histological funisitis at term. J Neonatal Perinatal Med 12(1): 37-40.
- Kim CJ, Romero R, Roberto Romero, Piya Chaemsaithong, Noppadol Chaiyasit, Bo Hyun Yoon, et al. (2015) Acute chorioamnionitis and funisitis: definition, pathologic features, and clinical significance. Am J Obstet Gynecol 213(4 Suppl): S29-S52.
- Conti N, Torricelli M, Chiara Voltolini, Silvia Vannuccini, Vicky L Clifton, et al. (2015) Term histologic chorioamnionitis: a heterogeneous condition. Eur J Obstet Gynecol Reprod Biol 188: 34-38.
- Shanks AL, Mehra S, Gil Gross, Ryan Colvin, Lorie M Harper, et al. (2016) Treatment Utility of Postpartum Antibiotics in Chorioamnionitis Study. Am J Perinatol 33(8): 732-737.
- Image 1 Courtesy: Science direct
- Image 2 Courtesy: Lecturio.com
- Image 3 Courtesy: Libre Pathology
- Image 4 Courtesy: Springer link.com
- Image 5,6 and 7 Courtesy: Wikipedia.com
- Image 8 Courtesy: Wikimedia commons






























