- Case Report
- Abstract
- Introduction
- The role of Antiplatelet Agents in Patients with COVID- 19
- Results of research studies on antiplatelet therapy in patients with COVID-19
- The beneficial mechanisms of antithrombotic low-dose aspirin treatment
- Timing of aspirin initiation in hospitalized patients with COVID-19
- Other antiplatelet agents in patients with COVID-19
- Conclusion
- References
A Rare Case of Adrenocortical Carcinoma Recurrent and Disseminated
Manoj Kumar Suman1*, P Gaur2 and Mukesh Ghoslya3
1Senior Resident of Department of Radiation Oncology, Dr. S. N. Medical College, India
2Senior Professor & Head of Department of Radiation Oncology, Dr. S. N. Medical College, India
3Junior Resident of Department of Radiation Oncology, Dr. S. N. Medical College, India
Submission: May 20, 2022; Published: June 10 2022
*Corresponding Address: Manoj Kumar Suman, Senior Resident of Department of Radiation Oncology, Dr. S. N. Medical College, India
How to cite this article: Manoj Kumar Suman, P Gaur, Mukesh Ghoslya. A Rare Case of Adrenocortical Carcinoma Recurrent and Disseminated. Canc Therapy & Oncol Int J. 2022; 21(4): 556070. DOI:10.19080/CTOIJ.2022.21.556070
- Case Report
- Abstract
- Introduction
- The role of Antiplatelet Agents in Patients with COVID- 19
- Results of research studies on antiplatelet therapy in patients with COVID-19
- The beneficial mechanisms of antithrombotic low-dose aspirin treatment
- Timing of aspirin initiation in hospitalized patients with COVID-19
- Other antiplatelet agents in patients with COVID-19
- Conclusion
- References
Abstract
Adrenocortical Carcinoma is an extremely rear tumor and a few cases so far been reported in the literature. We hereby present one case report. A 38-Year-old Indian female house wife presented with a complaint of occasional Headache and left flank pain last two to three months . Associated with weakness, fever, and anorexia. She had history of left Adrenalectomy on 15.08.2018. Her routine investigation and CT Thorax and abdomen MRI lumbosacral spine, USG abdomen and pelvis, immune histopathology and tumor marker were performed, diagnosis of recurrent Adrenocortical carcinoma with Lung, liver spleen and retroperitoneal lymph nodes metastasis was established. Staged IV according to AJCC. Performance score ECOG -2. We planned palliative chemotherapy with best supportive care. She was discharge in stable condition with follow for next cycle.
Keywords: Adrenocortical carcinoma; Cachexia; Polymenorrhoea; Cortsiol; Immunohistochemistry; Adrenalectomy
Abbreviations: ACC; CT; DHEAS; ACTH; ECOG; AJCC; LN; ENSAT
- Case Report
- Abstract
- Introduction
- The role of Antiplatelet Agents in Patients with COVID- 19
- Results of research studies on antiplatelet therapy in patients with COVID-19
- The beneficial mechanisms of antithrombotic low-dose aspirin treatment
- Timing of aspirin initiation in hospitalized patients with COVID-19
- Other antiplatelet agents in patients with COVID-19
- Conclusion
- References
Introduction
Adrenocortical Carcinoma is a very rare disease. The incidence is 1 to 2 per million per year [1]. The median is of diagnosis is fifth to sixth decade of life [2]. The ratio of female and male ranges from 1.5:1. Aside from genetic (Li Fraumeni syndrome, Lynch Syndrome) predisposition no risk factors have been established. According to national modality follow back Survey (1986) smoking is Male and contraceptive in Female before age of 25 is also risk factors [3]. Patient many presented with complain of the clinical features of hormone excess and present with nonspecific symptoms like local tumor growth, abdominal pain, abdominal fullness, early satiety [4] and rarely presented with cachexia and night sweats, Paraneoplastic syndromes [5]. Hormone relative symptoms also appear when there excess in hormone- secreting ACCs. At the time of diagnosis, the initial evaluation should include a thorough physical examination, detail history. Basic biochemical evaluation includes RFT, LFT, CBC, Hormone assay. Imaging modalities include CT, MRI of abdomen/pelvis and CT Thorax.
For staging of tumor we followed AJCC, TNM Staging :-
Stage 1:- Tumor 5cm or less with no spread to surrounding tissues or lymph nodes without distant metastasis.
Stage 2:- Tumor>5 cm with other stage 1 characteristics.
Stage 3:- Tumor invading nearby tissues and/or spread to nearby lymph nodes.
Stage 4:- Distant metastasis.
In our case study in stage 4
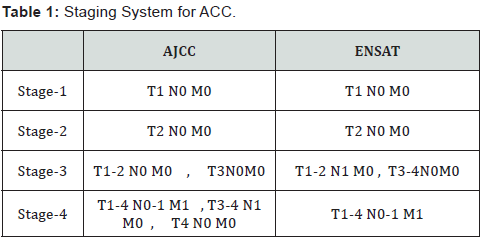
There is newly introduce European Network for the study of Adrenal Tumor (ENSAT) system become widely used by ACC community. Stage group as Table 1
She was diagnosed in 2016 outside the hospital august 2016. Patient was evaluated With a CECT Scan which showed enhancing mass lesion in Lt Suprarenal with multiple areas of Necrosis.
Left adrenal not separately visualized. Inferiorly abutting upper left kidney, no infiltration, Sub cm LN seen in retroperitoneum along the celiac artery. Calcific segment 7 of Liver. ? Adreno cortical carcinoma. Patient underwent left Adrenalectomy on 15.08.2018, histopathology report shown gross-capsulated soft tissue mass 500 gm 11x9x6.8 cm. Histology shows tumor cells round to polygonal with arrangements of sheets, Extensive necrosis and tumor emboli seen in sinusoids and a thin-walled vessel in capsule with Capsular invasion, Mitosis 3-4/50 HPF. Histological feature in favor of Adrenocortical carcinoma 5 Celiac lymph nodes with reactive Hyperplasia. Pan CK, Vimentin, chromogranin and CD10 are negative. Carelentin, Melan A are positive. KI 67+10-15% post of USG was normal, no residual mass.
Post OP DHEA
52.3. Patient has been on follow-up with serial USG which is insignificant, follow-up USG done on 11.06.2019 was s/o an illdefined mass lesion 4.6*5 cm left suprarenal region ? Recurrence Patient also complains of Polymenorrhoea. Cervical pep smear done in December 2018 which is negative for malignancy. USG done December 2018 showed thickened endometrium with small follicles in ovaries b/L.? Anovulatory cycles.
Examination
ECOG-1, Patient well oriented to time, place, person, pulse rate 86/minute, BP-180/110 mm Hg., RR-18/minute., P/A-Soft, Vague mass palpable in left suprarenal region, no orgenomegaley, Prominent abdominal aortic pulsations present, Post OP Scar Health. No dehiscence.
Investigation
CBC, RFT, LFT, Urine VMA, Serum, Cortisol, Serum ACTH, Se. Electrolytes.
CT Thorax and abdomen
Multiple parenchymal nodules and masses of varying sizes are seen in both lungs, largest measuring 3.5x3.4x3.0 cm (APxTRxCC) in lower love of left lung. There is a large lobulated heterogeneously enhancing mass seen in left suprarenal region. Left adrenal is not seen separately. It shows loss of fat planes with left crus of diaphragm medially. Posteriorly it is involving posterior pre renal space and infiltrating posterior renal fascia. Upper pole of left kidney is not demarcated separately likely involve the mass. Surgical staples are seen engulfed within the lesion. Anteriorly there is focal loss of planes with spleen. Surgical staples also noted in retroperitoneum. A small deposit is seen in right perihepatic region along segment VI. Minimal free fluid in POD with mild enhancement and modality? Metastasis.
MRI Lumbosacral Spine
Variable disk desiccation small well defined suspicious non enhancing T1/T2/STIR hypointense signals noted in L4 vertebral body, no evidence of involvement of posterior and lateral elements. Lung, liver spleen and retroperitoneal lymph nodes metastasis.
Management
As she presented to us with metastatic disease (Liver, Lung, Spleen, Retroperitoneum Lymph nodes Metastatic). We thoroughly evaluate the patient by physical, clinical examination and essential biomarker with imaging and start palliative chemotherapy (Etoposide, Carboplatin, Doxorubicin with G-CSF support). After two chemotherapy we further evaluate for the patient for response. In evaluation diseases progressive in nature and we planned for tablet metoten which is not available in market hence we continue the palliative chemotherapy with the best supportive management.
- Case Report
- Abstract
- Introduction
- The role of Antiplatelet Agents in Patients with COVID- 19
- Results of research studies on antiplatelet therapy in patients with COVID-19
- The beneficial mechanisms of antithrombotic low-dose aspirin treatment
- Timing of aspirin initiation in hospitalized patients with COVID-19
- Other antiplatelet agents in patients with COVID-19
- Conclusion
- References
Conclusion
Adrenocortical Carcinoma is a very rare neoplasm. More common in female. ACC with disseminated metastases has very poor prognosis. Hence early diagnosis and complete tumor resection is only curative intent. Adjuvant chemotherapy helps improve survival and decrease the chance of recurrence and relapse rates. Multiple disseminated metastasis has no significant advantage of chemotherapy but a recent phase 3 trial (FIRM- ACT, First International Randomized Trial in Metastatic Adrenocortical carcinoma Treatment) EDPM regimen is most efficient. Single agent Mitotane can be considered as palliative intent. Over all the ACC is a rare neoplasm and require early detection, correct diagnosis and multimodality approach including total excision, adjuvant chemotherapy.
- Case Report
- Abstract
- Introduction
- The role of Antiplatelet Agents in Patients with COVID- 19
- Results of research studies on antiplatelet therapy in patients with COVID-19
- The beneficial mechanisms of antithrombotic low-dose aspirin treatment
- Timing of aspirin initiation in hospitalized patients with COVID-19
- Other antiplatelet agents in patients with COVID-19
- Conclusion
- References
Discussion
Adrenocortical carcinoma is a rare malignancy with worst prognosis with incidence is 1 to 2 per million per year. More common in female (58.7%Predilection) [1], fifth to sixth decade of life. ACC occurs with increased frequency in Beckwith Wiedman syndrome and Li-Fraumani syndrome. However , most of the tumors are sporadic [6]. Diagnosis will be established by clinical, biochemical markers, imaging and histological features. ACC has unfavorable prognosis. Tumor characteristics of malignancy and velocity of tumor growth are usually related to a decreased survival. Distant metastasis and number of organs involved in metastatic disease, confers a poor prognosis [7]. Only curative approach to ACC is complete tumors resection. The evidence that Surgery for recurrent disease indicated in when disease confined to one site or organ [8]. Adjuvant Chemotherapy aim to minimize the chance of recurrence. In unrespectable or metastatic ACC palliative care and palliative chemotherapy should be consider. Mitotane remain the only drug approved by U.S. Food and Administration for adjuvant and palliative indent [9]. Dose of mitotan 1g. twice daily with increase every 4 to 7 days by 0.5 g/d till maximum 5 to 7 g. [10] Chemotherapy is currently a mainstay of treatment for advanced and metastatic ACC. EDPM (Etoposite, doxorubicine, Cisplatin, Mitotan ) regimen is most effective regimen [11].
- Case Report
- Abstract
- Introduction
- The role of Antiplatelet Agents in Patients with COVID- 19
- Results of research studies on antiplatelet therapy in patients with COVID-19
- The beneficial mechanisms of antithrombotic low-dose aspirin treatment
- Timing of aspirin initiation in hospitalized patients with COVID-19
- Other antiplatelet agents in patients with COVID-19
- Conclusion
- References
References
- Allolio B , Fassnachat M (2006) Clinical review : Adrenocortical carcinoma: Clinical update. Clin endocrinol metab 91(6): 2027-2037.
- Bellanone R, Ferrant A, Boscherini M , Lombardi cp, Crucitte P, et al. (1997) Role of reopreration in recurrence of adrenal cortical carcinoma: Result from 188case collected in the Italian National registry for Adrenal cortical Carcinoma. Surgery 122: 1212-1218.
- Hsing AW, Nam jm, co chien HT, Mclaughlin jk, Fraumeni jf jr (1996) Risk factor for Adreanal cancer:an exploratory study. Int j cancer 65(4): 432-436.
- Fassnacht M Allolio B (2009) clinical management of adrenocortical carcinoma. Best Pract res clin Endocrinol metab 23(2): 273-289.
- Luton jp, Cerdas, Billaud L, G Thomas, B Guilhaume, et al. (1990) clinical feature of adrenocortical carcinoma,prognostic factor, and the effect of mitotan therapy. N Engl med 322(17): 1195-1201.
- Kock ca, Paka k, chrousos GP (2002) Molecular pathogenesis of hereditary and sporadic adrenocortical and adrenomedullary tumor. J cli Endocrino Metab 87(12): 5367-5384.
- Assie G, antoni G, tissier F, Bernard Caillou, Gwenaelle Abiven, et al. (2007) Prognostic parameters of metastatic adrenocortical carcinoma. Clin endocreinol Metab 92(1): 148-154.
- Erdogan I, deutschbin T, Jurowich C, Matthias Kroiss, Christina Ronchi, et al. (2013) The role of surgery in the management of recurrent adrenocortical carcinoma. J clin endocrinol Metab 98(1): 181-191.
- Schteingart DE, Doherty GM, Gauger PG, T J Giordano, G D Hammer, et al. (2005) managment of patient with adrenal cancer :recommendationsof an international consensus conference. Endocr relat cancer 12(3): 667-680.
- Terzolo M, Ardito A, Zaggia B, F Laino, A Germano, et al. (2012) Management of adjuvant mitotane therapy. endocrine 42(3): 521-525.
- Flack MR, Pyle rg, Mullen nm, B Lorenzo, Y W Wu, et al. (1993) treatment of metastatic adrenal cancer. J clin endocrinol metab 76(4): 1019.






























