T-cell Large Granular Lymphocytic Chronic Leukemia: Treatment Experience with Cyclosporine-follow up after COVID 19 Pandemic
Guran Catalina2*, Ilie Alina1, Oros Dacian Nicolae2, Calamar Popovici Despina2 and Ionita Ioana2
1Hematology Department, Emergency Municipal Hospital Timişoara, Romania
2Department of Internal Medicine 1 – Hematology, “Victor Babes” University of Medicine and Pharmacy Timisoara, Romania
Submission: May 19, 2022; Published: June 02, 2022
*Corresponding Address: Guran Catalina, Department of Internal Medicine 1 - Hematology, “Victor Babeş” University of Medicine and Pharmacy Timişoara, Eftimie Murgu Sq. no. 2, 300041, Timişoara, RO; Multidisciplinary Research Center for Malignant Hemopathies, Emergency Municipal Hospital Timişoara, str. Gheorghe Dima no. 5, 300079, Timisoara, Romania
How to cite this article: Guran C, Ilie A, Oros D N, Calamar P D, Ionita I. T-cell Large Granular Lymphocytic Chronic Leukemia: Treatment Experience with Cyclosporine-follow up after COVID 19 Pandemic. Canc Therapy & Oncol Int J. 2022; 21(4): 556066. DOI:10.19080/CTOIJ.2022.21.556066
Abstract
The patient presented herself at the hospital in June 2018 with sever pancytopenia. She underwent bone marrow biopsy and flow cytometry which established the diagnosis of Large Granular T-cell Leukemia. She was given treatment with Ciclosporine 50mg 6cps/day, which was reduced at 3 cps/day because the patient developed pancytopenia at 6cps/day. The blood count tests improved constantly with a suspicion of relapse at 18 months. Relapse was excluded. She has been receiving 4cps/day with a very good evolution and a good hematological response even when the patient has developed Parkinson’s disease. The patient refused COVID19 vaccination but had a mild form of COVID19 infection, maintain a good hematological response throughout this whole period.
Keywords: T- LGL; Cyclosporine
Introduction
T-cell Large Granular Lymphocytic Chronic Leukemia is lymphoproliferative disorder characterized by enlarged lymphocytes, containing noticeable granules. It was described as a clonal disorder involving the invasion of marrow, spleen and liver. Recurrent infections are usually seen in patients with T-LGL leukemia, associated with neutropenia. We can also see anemia, splenomegaly and autoimmune disease, particularly rheumatoid arthritis. We are going to present a case of T-LGL chronic leukemia followed by our team over a period of 36 months.
Case Report
The patient, G.A., 68 years, female, with Rheumatoid Arthritis as associated risk factors, first presented herself at the Emergency Department in June 2018 with severe fatigue, dizziness, tegumentary pallor. She was admitted with severe anemia (Hgb=5,4g/dl), was given blood transfusions. The abdominal echography showed mild hepatomegaly and splenomegaly. In July 2018 she was again admitted with severe anemia and grade III neutropenia, was given blood transfusions and underwent a bone marrow aspirate, which was inconclusive. She was recommended a bone marrow biopsy which was unavailable in the Clinic she was admitted to, therefore the patient presented herself in the Hematology Clinic of the Municipal Emergency Hospital in Timişoara, in November 2018.
She underwent several tests, a bone marrow biopsy (Conclusions: Medullar infiltration ~15-17%, with small T-cell with a phenotype of large granular lymphocytes- T-cell large granular lymphocytic leukemia. Erythroblastic hyperplasia and moderate neutropenia) correlated with flow cytometry (Phenotype: 46% Lymphocytes T CD3+, CD8+, TCRgd-, CD5 weak positive) in November 2018, which established the diagnosis of T-cell large granular lymphocytic leukemia. Due to pharmaceutical limitations (oral Fludarabine and Cyclophosphamide being very difficult to obtain in our country), and per recommendations found in literature, the patient was started with oral Cyclosporine 50 mg 6cps/day in January 2019, associated with prophylactic antibiotics. As seen in reference [1,2], single agent immunosuppressive treatment is the election treatment in LGLL-T. Due to worsening of the blood count test, the dose was reduced at 3 cps/day, meaning 150mg/day. She maintained a level of Hgb~10g/dl, grade II/ III asymptomatic neutropenia, and no thrombocytopenia (Figure 1).
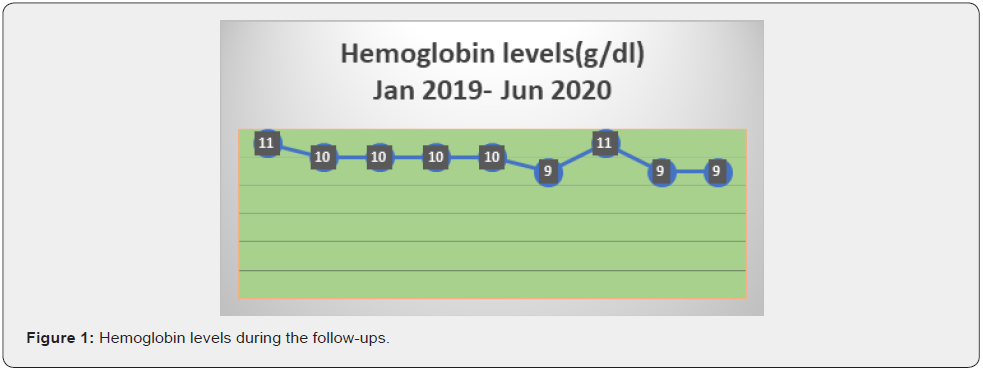
In August 2019 she presented with Hgb< 10g/dl, which allowed us to recommend Erythropoietin treatment. After one month of erythropoietin, she obtained 12 g/dl, and maintained a level over 10g/dl of hemoglobin. At the one year follow up the patient presented herself with grade II asymptomatic neutropenia, without anemia or thrombocytopenia. She was considered in a partial remission and the Cyclosporine treatment was continued with 3cps/day (150mg/day), associated with prophylactic antibiotics (Figures 2 & 3).
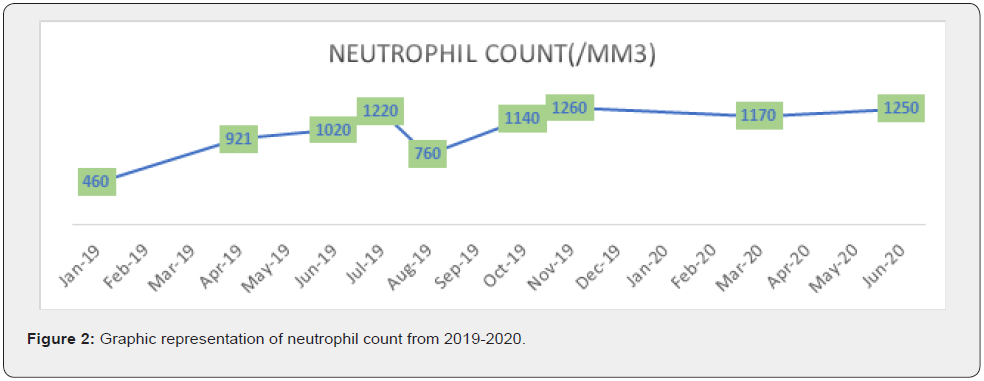

At the 18 months follow-up, the patient presented with pancytopenia, Hgb= 10,3 g/dl, Ne= 1250/mm3, Plt= 118.000/ mm3. We were suspecting a relapse which was infirmed after reevaluating the patient. After being given 4cps/day (200mg/ day), the patient slowly obtained a normal blood count, without secondary infections, and maintained the response. The antibiotics prophylaxis was stopped in 2020 and the patient was monitored at 3 months’ time, even monthly if there were any decreases in her blood count tests. From October 2019 until March 2021, the patient didn’t require any Erythropoietin substitution [3,4].
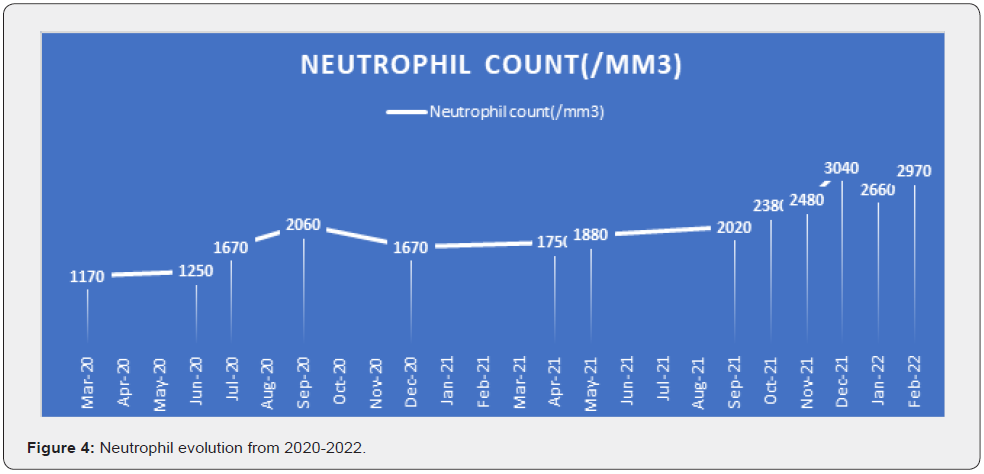
In 2021 the patient was diagnosed with Parkinson’s disease and was started specific treatment, with some adverse reactions to the first line of treatment. After switching to a new course of medication for Parkinson’s, the tremors subsided, and the patient has been feeling very well. Throughout this period, the Cyclosporine was not discontinued. When the COVID19 vaccines became available in Romania, the patient was advised to get vaccinated, but she refused. As shown in Figure 4, there has been an increase in neutrophil count in this case, obtaining normal neutrophil values in September 2021. These normal values have been maintained thus far (Figure 4).
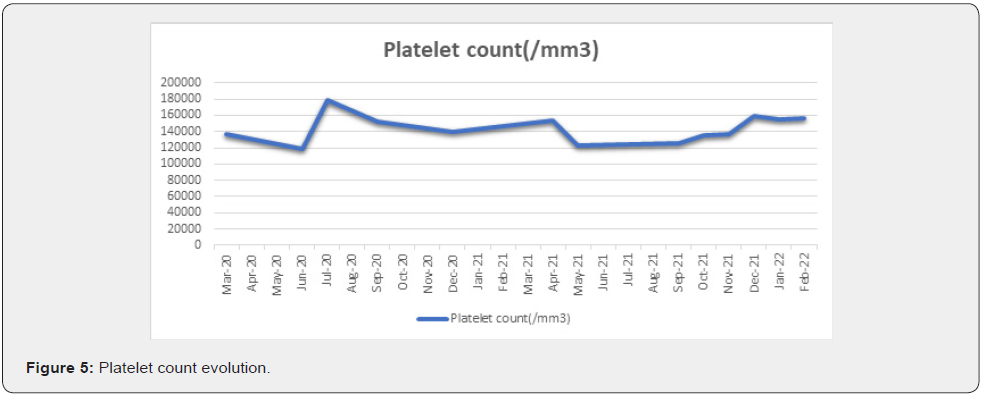
In March 2021 the patient accused shortness of breath, lack of appetite, headaches and fatigue. The clinical examination revealed a decreased concentration of oxygen levels ( SaO2 = 86%), pulmonary crackling sounds at both inferior lobes. She was suspected of COVID19 infection and was referred to the Emergency Department for testing and admission to the hospital. The patient refused both actions and refused to be properly evaluated. Through outpatient care, she tested positive for COVID19 infection through a PCR test and was given prophylactic antibiotic therapy and symptomatic treatment. The Cyclosporine treatment was not discontinued, as there was some data available that Cyclosporine treatment might help inhibit the SARS COV2 virus, as seen in reference [5]. Antiviral medication was not given, as the patient refused to be seen by an infectious disease specialist, and in Romania COVID19 protocols state that specific antiviral medication should be given after being recommended by an infectious disease specialist. She was closely monitored, and after 2 days of treatment, there was a clear improvement in general health and oxygen levels ( SaO2= 94%). The blood tests done at 3 weeks after infection revealed mild anemia, mild thrombocytopenia, mild neutropenia. There were no further complications secondary to the COVID19 infection. This was the only infection with COVID19 documented in this case (Figure 5).
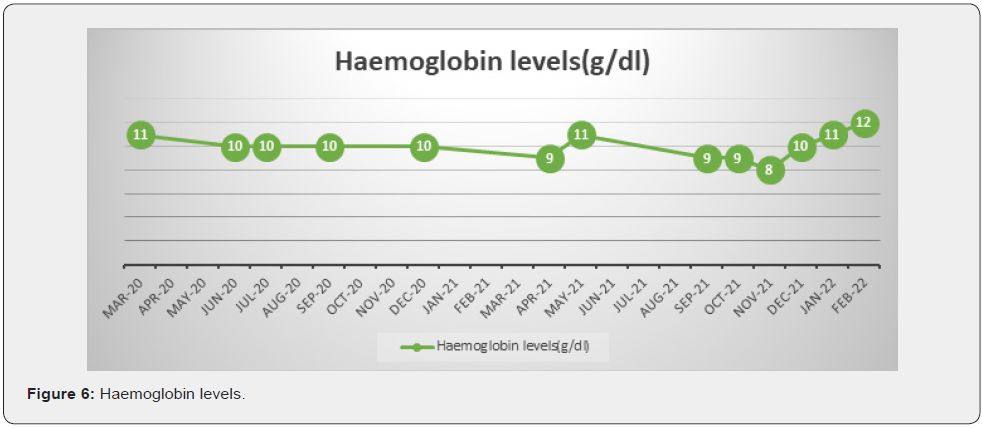
Since then, the patient has not suffered any other infections nor any other complications due to treatment or comorbidities. The dose has been 4cps/day ( 200mg/day) since the 18 months follow-up. In November 2021 the patient presented mild anemia, as seen in Fig. 6 below, and needed Erythropoietin substitution, having an increase of 2g oh hemoglobin after 2 injections. The patient is satisfied with the treatment and quality of life associated with it. We obtained a good hematological response, and as per data available, the immunomodulatory treatment is recommended for chronic use, since the patient has a good response and no secondary complications. A bone marrow biopsy has not been deemed necessary now. Our clinical experience with Cyclosporine in this LGL-T case has been a very successful one, with both hematological response and quality of life being satisfactory (Figure 6).
Conclusion and discussion
i. The response at 36 moths is favorable, the patient achieving a very good hematological response, slightly improved since our 18 months evaluation.
ii. The quality of life during this time was very good, with no clinical symptoms and few complications. This was the goal, we (the patient and medical team) set when starting treatment. For now, the goal has continued to be achieved.
iii. The patient had no need for blood transfusions after the treatment was started, which led to a better compliance to treatment and lower costs. Of course, the lowering of costs of treatment is a factor that we like to keep in mind, but maybe not a decisive factor when deciding on the treatment we give a patient.
iv. The COVID19 infection was easy overcome at this case and did not affect the treatment response, nor did it affect the overall survival of the patient. Although COVID19 infection has a much aggressive impact and has a high mortality rate on other cancer patients, in this case, the infection was easy overcome.
v. Our case, even though one case cannot sustain a theory, supports the data found by our colleagues, as seen in reference [5], that Cyclosporine treatment might help when it comes to COVID19 infection, as the patient was unvaccinated and recovered quickly from the infection, without complications and without antiviral treatment.
vi. The association with Parkinson’s disease did not influence the course of treatment.
References
- Thierry Lamy, Aline Moignet, Thomas P Loughran Jr (2017) LGL leukemia: from pathogenesis to treatment. Blood 129(9): 1082–1094.
- Thierry Lamy, Thomas P Loughran Jr (2011) How I treat LGL leukemia. Blood 117(10): 2764–2774.
- Neha Gupta, Suman Kumar, Gurdeep Singh, Atoshi Basu (2015) Adult T cell large granular lymphocytic leukemia. Med J Armed Forces India 71(Suppl 1): S2725–
- Aline Moignet, Thierry Lamy (2018) Latest Advances in the Diagnosis and Treatment of Large Granular Lymphocytic Leukemia. Am Soc Clin Oncol Educ Book 38: 616-625.
- Nadia Nicholine Poulsen, Albrecht von Brunn, Mads Hornum, Martin Blomberg Jensen (2020) Cyclosporine and COVID-19: Risk or favorable?. Am J Transplant 20(11): 2975-2982.






























