The Cancer Landscape in India- Challenges and Recommendations on Pragmatic Care: An initiative by India Sweden Healthcare Innovation Centre
Puneet Pareek1*, Atul Sharma2, Ebba Hult3, Anil Kukreja4, R S Dhaliwal5 and Pramod Julka6
1Additional Professor, Department of Radiation Oncology, AIIMS Jodhpur, India
2Department of Medical Oncology, AIIMS Delhi, Sri Aurobindo Marg, New Delhi, India
3Head, Vision Zero Cancer, Stockholm School of Economics, House of Innovation, Sweden
4AstraZeneca Pharma India Limited, Karnataka, India
5Scientist G & Head, Non-Communicable Diseases, Indian Council of Medical Research, Delhi, India
6Director-Oncology Daycare Centre, Max Oncology Daycare Centre, Max Institute of Cancer Care, New Delhi, India
Submission: January 31, 2022; Published: February 16, 2022
*Corresponding Address: Puneet Pareek, Additional Professor, Department of Radiation Oncology, AIIMS Jodhpur AIIMS Jodhpur, basni Industrial Area, MIA 2nd Phase, Basni, Jodhpur, Rajasthan 342005, India
How to cite this article: Puneet P, Atul S, Ebba H, Anil K, R S Dhaliwal, et al. The Cancer Landscape in India- Challenges and Recommendations on Pragmatic Care: An initiative by India Sweden Healthcare Innovation Centre. Canc Therapy & Oncol Int J. 2022; 20(5): 556049. DOI:10.19080/CTOIJ.2022.20.556049
Background
Cancer is one of the leading causes of morbidity and mortality worldwide. The GLOBOCAN 2018 has reported an estimated 18.1 million new cases and 9.6 million cancer-related deaths worldwide [1]. Cancer trends in India closely reflect the global landscape. As per the National Cancer Registry Programme (NCRP) Report 2020, India has a cancer burden of over 1.39 million cases. This number is likely to increase to 1.57 million by 2025 — a 12% increase from the current estimated cases. One in 9 Indians will develop cancer during their lifetime. While lung and oral or mouth are the most prevalent cancer types among males, breast and cervix cancers are the most common among females [2,3].
The reasons for the rapid growth in the incidence are complex; however, it can be empirically attributed to aging and population growth. Importantly, increasing adoption of risk behaviors such as unhealthy diets, physical inactivity and harmful use of alcohol and tobacco further add to the rise in the number of cases. According to the World Health Organization (WHO), approximately 70% of deaths from cancer occur in low- and middle-income countries [4]. In India, non-communicable diseases (NCDs) are responsible for more than half of the deaths and cancer is one of the leading contributors [5]. Late-stage presentation, poor access to optimal diagnosis and treatment, and affordability further adds to the escalating burden of cancer-related morbidity and mortality in the country. The recent COVID-19 pandemic has further widened the gaps in cancer care. Changes in health-seeking behaviors and the availability and access to essential services from screening, diagnostics to treatment are likely to have a direct and indirect impact on patient outcomes in the long- and short-term.
Against this backdrop, the roundtable Discussion on Oncology, part of the Sweden-India Health Talks 2020, aimed at addressing some of the critical roadblocks in optimum cancer care in India. Experts from both public and private sector in India and Sweden share their best practices and potential policy interventions focusing on strengthening the current healthcare system to drive efficient outcomes in prevention, diagnosis and management of cancer.
Current Challenges in the Cancer Care Pathway
Delivering equitable and affordable care has been one of the greatest public health challenges in India. Differing cancer profiles, marked socioeconomic diversity, variable access to care, gaps in knowledge, behaviour and attitude of the public combined with resource and infrastructure constraints, complicate timely and efficient delivery of cancer care in the country. A series of gaps and weaknesses in the current cancer care pathway have been identified throughout this discussion.
Limited Awareness
The importance of awareness with respect to prevention cannot be underestimated, particularly in the resource-limited conditions of the country. Among patients, lower recognition of warning signs and suspicious symptoms of cancer is associated with delays in seeking medical help. In addition, emotional barriers such as fear, worry and stigma strongly influence the help-seeking behaviour. Evidence suggests that the awareness on the availability of screening is poor among the Indian population [6].
Treatment direction and long-term prognosis largely depend on the stage at diagnosis. Cancers are usually detected or at least suspected within primary care settings. General Physicians (GPs) act as ‘gatekeepers’ whereby they can assess pre-symptomatic risk, identify early presentations, gather family history and vital patient information and finally decide on investigations or referrals. However, there is a paucity of training and resources for GPs to enable them to detect cancers at early stages or for synthesizing information from a patient’s presentation. This lack of awareness among the public and the primary care providers could explain the advanced stage of disease at diagnosis, commonly observed among cancer patients in India.
Gaps in Reporting
As observed during the ongoing COVID-19 pandemic, mandatory disease reporting plays a critical role in preventing and controlling the spread of disease in populations. Despite the alarming current and projected burden of NCDs such as cancer, their inclusion as a notifiable disease has remained elusive. Compulsory notification of cancer cases facilitates collection of data for population-based cancer registries (PBCRs). Since cancer is not a notifiable disease, registries in India face several challenges in data collection. As per the 2020 report of the NCRP, PBCRs included in the study covered just 10% of the population in India. Another challenge is incomplete and inaccurate certification of cause of death that contributes to the gaps in cancer-related mortality registrations [2]. These limitations in the reach of quality registries hamper systematic collection, analysis and use of epidemiologic data to define sustainable frameworks for cancer control in the community.
Unequal access
Healthcare pushes an estimated 32 to 39 million people to poverty every year. Cancer ranks the highest on hospitalisation spending and out-of-pocket expenditure in the country with a proportional catastrophic financial impact [7].
India is predominately rural in terms of its population concentration. However, there exists a significant inconsistency between demand and supply in rural healthcare in India. Most district hospitals and even regional cancer centers lack necessary facilities to provide quality cancer care. Vast majority of inflicted patients thus travel long distances to the few major cancer centers, predominantly located in big cities. For the patient, this migration significantly adds to their financial burden, and for the cancer centers, this means disproportionate patient load hampering efficient care delivery.
Compared with the developed world, the ratio of incidence to mortality in India is high. Lesser than 30% of patients with cancer survive 5 years or longer after diagnosis [8]. The inadequacies in on-time and affordable diagnosis, high treatment costs and the urban-rural divide are some of the critical factors responsible for the poor access to cancer care in the country.
Resource Constraints
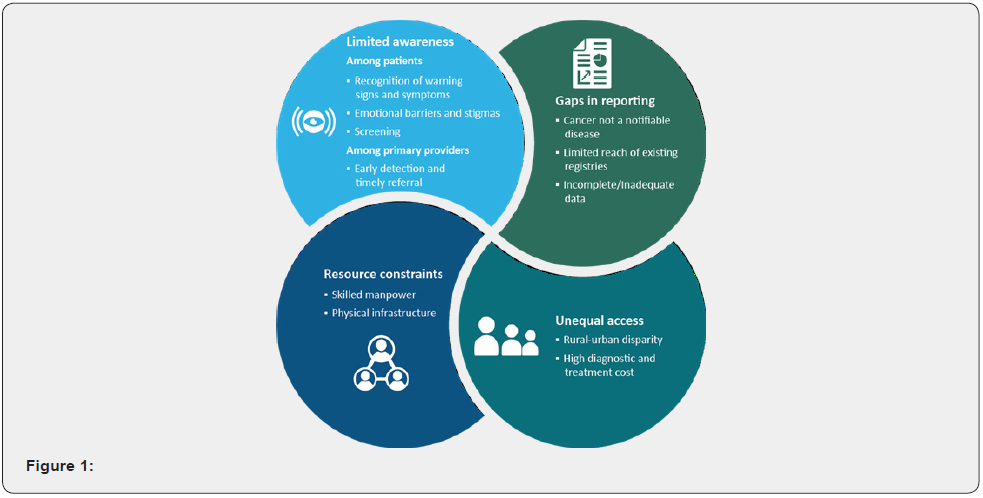
Shortages in health resources — manpower and infrastructure, is the Achilles heel of the cancer care pathway in India. Overall, the density and distribution of skilled primary and secondary healthcare workforce is a significant barrier. There exists an astounding inequality in the distribution of density of doctors in the country, where there are 4 times more doctors in the urban compared with the rural areas [9]. Given their late stage of diagnosis, cancer patients in India often require seeing a medical oncologist for palliative care. Estimates suggest fewer than 350 medical oncologists see an enormous case load of 3000 new cases per year, predominantly in private settings [10]. Besides the human resource limitations, the physical infrastructure required to complement optimal cancer care too remains inadequate in the country (Figure 1).
Recommendations on pragmatic cancer care in India
The Round table discussion on Oncology has identified specific recommendations to address the challenges and barriers to efficient cancer care in India. In many respects they are interconnected and ideally should be considered holistically.
Create targeted initiatives towards cancer prevention
Prevention offers the most cost-effective and long-term strategy for the control of cancer. Modifying or avoiding risk factors and implementation of evidence-based prevention strategies can reduce up to half of cancer deaths.
Appropriate cancer care requires improved awareness and understanding of the disease through effective communication, education and training. To effect positive change in the general population, implement programmes on cancer awareness at the community and individual level.
Education on risk factors, recognition of symptoms and eliminating stigma associated with the disease may help earlier detection and improve survival. In addition to the traditional channels such as mass media, utilize digital such as social media to drive outreach. Careful selection of the target groups such as at-risk and vulnerable population and crafting context-specific communications are the critical determinants to their success. Tobacco consumption is responsible for almost one in 5 cancer deaths and ironically is the single largest preventable cause of cancer deaths [4]. In India, tobacco in various forms, is responsible for 30% to 60% of total cancers among males and 10% to 30% among females [11]. Thus, strict tobacco control measures including policy changes are critical in the prevention of cancer in India.
Promote strategies to early detection as part of comprehensive cancer control
Early detection is cardinal to earlier stage diagnosis, survival and improvement in the quality of life of patients. Existing infrastructure in the public and private sector needs to better enable early detection approaches. Considering the resource limitations, geographic spread and population density in the country, high-risk and endemic regions can be strategically prioritized for timely and routine screening, for instance, the North East for tobacco related cancers. In fact, proven screening mechanisms exist for 3 of the most prevalent cancers in the country – mouth or oral, cervix and breast. Efficient utilization of existing screening programmes can be utilized for cancer control. For example, medical social workers such as accredited social health activist (ASHA) can be trained to teach women breast selfexamination and conduct PAP smear which can be sent to the district hospitals for investigations.
Artificial intelligence (AI)-based risk assessment models can help identify patients who are at elevated risk and should be enrolled in screening programmes for disease prevention and early detection. As a long-term strategy, tap into the potential of AI and machine learning for early detection research. Another important consideration is linking primary to tertiary health centres with the objective of facilitating earlier diagnosis. Application of rational models such as connecting the health and wellness centres under the Ayushman Bharat initiative to the regional cancer centre (RCC) in a hub-and-spoke, could potentially strengthen the rural connectivity and fasten the time to diagnosis and delivery of efficient care.
Leverage technology such as telemedicine, teleradiology and telepathology to improve access to care. Patients from remote areas can be tested and diagnosed in a single visit to the nearest healthcare facility such as an RCC and avoid multiple trips to a distant urban centre, which is often the case in conventional settings. This door step or point-of-care-diagnostics would not only reduce the time to diagnosis, but also the cost to treatment.
Make cancer a notifiable disease
Clinically led quality registries in cancer are indispensable to improve treatment outcome, gather real-world evidence, and enable new research. Cancer registries under the NCRP have consistently provided valuable estimation of cancer occurrence in the country, the foundation for the national cancer control programmed. In the short-term, initiation of new and expansion of the existing PBCRs is recommended to include the remotest of the areas in the country. Quality control measures are necessary to maintain the accuracy and completeness of information, including information on diagnostic and treatment modalities as well as mortality. Over the longer term, with the objective of improving surveillance and outcome, create a unified national registry integrating with Ayushman Bharat, hospital information systems and mortality databases.
Implement a systematic approach for effective management of cancer
Effective cancer management entails fostering outcomedriven partnerships between those delivering care and driving treatment compliance with those receiving it. Multidisciplinary care is recommended as a best practice in the treatment planning and care for cancer patients. From the time a patient enters the care pathway, an integrated team of medical professionals such as surgical, radio and medical oncologist should consider all relevant treatment options and collaboratively develop an individualized treatment and care plan for each patient. Better survival, shorter time to diagnosis and to treatment and receiving guidelinebased care are some of the prudent advantages this approach can offer a patient. RCCs can collaborate and connect with virtual multidisciplinary teams or tumour boards to provide optimal cancer care at remotest tertiary centre.
Non-compliance to cancer treatment is multidimensional and can involve a combination of patient, and healthcare related factors. These include health literacy, stage at diagnosis, lack of access to good care, cost of treatment, ineffective communication and inadequate training of the healthcare providers, etc. It can be said that the most prevalent ones in the country are usually health literacy, cost and access related. A standardized, comprehensive cancer care plan should be developed that can be tailored to the patient and their specific barriers.
Employ mobile-based and digital channels such as social media to make relevant information available to help patients understand the disease and decision making. Use technologybased supportive services such as tele-oncology or social health workers to contact patients and motivate them to complete treatment. Cost-effective treatment alternatives such as simple chemotherapy combinations, metronomic chemotherapy and radiotherapy should be preferred over expensive options to bolster the poorer patients to complete treatment. Drive partnerships with government, private providers, NGOs and international corporations to create innovative models for remote outreach and facilitate proactive cancer care at grassroot level. This can also help build cancer centre wings at each regional government and/ or private medical college by leveraging grants as per NCCP.
Augment affordability and value of cancer treatment
Pragmatic cancer care guidelines that promote optimal utilization of resources and reduce over reliance and over consumption of diagnostics are fundamental to making cancer care affordable. An evidence-based approach with implementation of harmonized and standardized clinical protocols should be promoted across the continuum of cancer care. Current Cancer medicines lie in the 12% bracket of GST. Even in the pre-GST era, there were excise & VAT exemptions given by states like Maharashtra, Assam etc which led to an effective tax of 5% on Cancer medicines. But with implementation of GST regime this has added a 7% increase in cost burden on patients OR loss of almost one month therapy which is very crucial from a patient perspective. Hence placing Cancer medicines in the NIL or 5% tax slab is desirable. Doctors and allied staff should be educated to best utilize available resources for treatment without compromising quality of care and patient safety. They should combine early diagnosis with precision medicine to become, in the long-term, less resource intensive, more comprehensive and more accurate.
Palliative care should be initiated as early in the patient care journey as possible and continued throughout the course of the disease. Implementing a holistic interdisciplinary approach, palliative care should encompass psychosocial, emotional, coping and caregiver needs to improve the overall quality of life of the patient. Digitally driven patient support programmes can effectively supplement treatment with at-home care such as required for pain management or rehabilitation, during or after cancer treatment.
Invest in skill and capacity building
Healthcare resources in the country, human as well as physical infrastructure, need to be augmented to maximize outreach to the population. Building capability of the rural healthcare staff through focused training and upskilling can be of incremental value. For example, medical social workers should be educated and trained to drive patient awareness, screening and motivation among general population. Next, there is a pressing need for oncologists and primary care providers to be on the same page on the significance of early detection and prompt referral. For example, GPs should be continually trained on identifying and addressing modifiable risk factors, referral for pre-cancerous conditions or suspected cancer. Training general surgeons in medical colleges and district hospitals on common onco-surgical procedures can be considered. Standardized referral pathways at all levels of care, from the primary level, have the potential to not only reduce the cost of treatment, but also improve survival. Adopt technology to make the most of available physical infrastructure. For instance, hub-and-spoke model that links the tertiary care hospitals to medical colleges as well as district hospitals through digital connectivity like telepathology and tele oncology can provide quality cancer care closer to home.
Way forward
Cancer is a significant contributor of mortality and morbidity in India. Late-stage diagnosis and poor treatment outcomes heavily burden the cancer care pathway in the country. Targeted efforts are required to ensure prevention, early-stage detection and equitable access for cancer care in the country. The following approach should guide action: (Figure 2).
Acknowledgment
I would like to express my very great appreciation to all the coauthors who have shared their inputs and thoughts for this report. I would like to offer my special thanks to Dr. Shaleen Kumar, Director – State Speciality Cancer Institute and Dr. Umesh Mahantshetty Director, Homi Bhabha Cancer Hospital & Research Centre for sharing their thoughts during our panel discussion which enabled us to create this report. I would also like to appreciate indigene and team of India-Sweden Healthcare Innovation centre for the efforts in doing the research and structuring the report.

Declarations
Funding: India-Sweden Healthcare Innovation Centre
Conflict of interest: None
References
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, et al. (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6): 394-424.
- Mathur P, Sathishkumar K, Chaturvedi M, Priyanka Das, Kondalli Lakshminarayana Sudarshan, et al. (2020) ICMR-NCDIR-NCRP Investigator Group. Cancer statistics, 2020: report from national cancer registry programme, India. JCO Glob Oncol 6: 1063-1075.
- India against cancer (2021) GLOBOCAN 2018: India factsheet. Cancer India Web site. Globocan 2018: India factsheet.
- Cancer (2021) Key facts. WHO website. Cancer (who.int).
- Non-communicable diseases (2021) National Health Portal Website. Non-communicable Diseases | National Health Portal of India.
- Veerakumar AM, Kar SS (2017) Awareness and perceptions regarding common cancers among adult population in a rural area of Puducherry, India. J Educ Health Promot 6: 38.
- Kastor A, Mohanty SK (2018) Disease-specific out-of-pocket and catastrophic health expenditure on hospitalization in India: do Indian households face distress health financing? PLoS One 13(5): e0196106.
- Mallath MK, Taylor DG, Badwe RA, Goura K Rath, V Shanta, et al. (2014) The growing burden of cancer in India: epidemiology and social context. Lancet Oncol 15(6): E205-E212.
- The health workforce in India (2021) WHO website.
- Sengar M, Fundytus A, Hopman WM, Sudeep Gupta, C S Pramesh, et al. (2019) Medical oncology in India: workload, infrastructure, and delivery of care. Indian J Med Paediatr Oncol 40: 121-127.
- Gandhi AK, Kumar P, Bhandari M, Bharti Devnani, Goura Kishor Rath, et al. (2017) Burden of preventable cancers in India: time to strike the cancer epidemic. Journal of the Egyptian National Cancer Institute 29(1): 11-18.






























