Mean Platelet Volume to Platelet Ratio as an Early Predictor of ICU Admission in Hematological Malignancies
Nahla A M Hamed1*, Omar Gallab1 and Reham Abdel Halim2
1Internal Medicine Department (Hematology Unit), Faculty of Medicine, Alexandria University, Alexandria, Egypt
2Clinical Pathology Department, Faculty of Medicine, Alexandria University, Alexandria, Egypt
Submission: August 12, 2021; Published: August 27, 2021
*Corresponding Address: Nahla A M Hamed, Internal Medicine Department (Hematology Unit), Faculty of Medicine, Alexandria University, Alexandria, Egypt Cancer
How to cite this article: Nahla A M H, Omar G, Reham Abdel H. Mean Platelet Volume to Platelet Ratio as an Early Predictor of ICU Admission in Hematological Malignancies. Canc Therapy & Oncol Int J. 2021; 19(4): 556018. DOI: 10.19080/CTOIJ.2021.19.556018
Abstract
Background & objective: The development of rapidly progressive complications and the high fatality rate in COVID-19 patients with hematological malignancies make it urgently needed to use readily available markers for early predicting of patients who need ICU admission. For these reasons, we aimed at identifying the usefulness of mean platelet volume to platelet ratio (MPR) and other indexes of inflammation as early predictors for the need of ICU admission in COVID-19 patients with hematological malignancies.
Methods: This study included 2 groups of hospitalized hematological malignancies patients: confirmed COVID-19 (18 patients) and COVID-19 negative (18 patients) of matched age, sex and bone marrow suppressive chemotherapy. Seven COVID-19 positive health care providers were included to determine MPR cutoff point of disease severity. MPR; Neutrophil to lymphocyte ratio; derived neutrophil to lymphocyte ratio; platelet to lymphocyte ratio; monocyte to lymphocyte ratio; neutrophil to lymphocyte x platelet ratio; systemic inflammation response index; systemic immune-inflammation index (SII) and aggregate index of systemic inflammation were calculated.
Results: Thirteen COVID-19 hematological malignancies cases were intermediate to severe and five cases were critical. Myeloid malignancies represent 55.56% of the cases. Acute leukemias constituted 72.22% (13 patients). ICU admission and deaths were more among acute leukemia. MPR was the only significantly different ratio between both hematological groups (p=0.001) and between ICU admitted and non-ICU admitted COVID-19 positive cases (p=0.010). MPR ≤ 0.0339 was an early indicator for ICU admission (sensitivity: 88.9%, specificity: 75%).
Interpretation & conclusion: MPR is the only reliable marker for the need of ICU admission in COVID-19 hematological malignancies. Mean platelet volume to platelet ratio must be calculated at COVID-19 diagnosis and at regular intervals to predict early need for ICU admission
Keywords: COVID-19; Hematological malignancies; Mean platelet volume to platelet ratio; Critical cases; Early biomarker
Introduction
COVID-19 positive cancer patients develop serious complications rapidly [1] and have higher fatality rate than the general population [2]. Patients with hematological malignancies are of concern for several reasons: a. they may have underlying immune system cancer, b. they develop chemotherapy induced bone marrow suppression with increased susceptibility to infections, c. there is similarity between their disease symptoms and COVID-19 infection symptoms [3] and, d. there is high rate of false negative SARS-CoV-2 RT-PCR in hematological malignancies either due to inability of the weakened adaptive immune system to respond to infection or the development of symptoms with smaller viral load below PCR detection limit [4].
For these reasons, it is urgently needed to use readily available markers for early assessment of COVID-19 associated inflammatory processes. CBC parameters can aid in early diagnosis of COVID-19 [5] and predicting its severity [6]. The lymphocyte count [7], the platelet count [8], red cell distribution width (RDW) [9], neutrophil to lymphocyte ratio is all prognostic value in COVID-19 infected patients [10]. This study aimed at evaluating the usefulness of mean platelet volume to platelet ratio (MPR)and other blood cell index of inflammation as early predictors for the need of ICU admission in COVID-19 hospitalized hematological malignancies patients.
Patients
Study population
The hematological data of 18 hospitalized patients with confirmed COVID-19 infection hematological malignancies were compared with that of 18 comparable COVID-19 negative patients of matched age, sex and bone marrow suppressive chemotherapy. Patients’ data were collected during the period from 5 September to 20 December 2020. Seven COVID-19 positive health care providers (6 mild and 1 moderate) were included to determine mean platelet volume to platelet ratio (MPR) cutoff point in relation to disease severity.
Data collection
Data were collected from the patient file system at the time of developing symptoms. COVID-19 diagnosis was based on lung CT and VIASURE SARS-CoV Real Time PCR of nasopharyngeal swab (CerTestBiotec, Spain) in all cases. Cases with clinical or radiological suspicious of COVID-19 without COVID-19 RT-PCR positive test were excluded. The disease severity was based on the National Health Committee of China clinical Classification [3].
Methods
Blood cell count inflammation parameters
Complete blood counts were measured in aseptic venous blood sample using automated counter ADVIA 2120 hematology system (Siemens Healthcare Diagnostics, USA).
Blood cell derived inflammation indexes were then calculated
Mean platelet volume to platelet ratio (MPR)= mean platelet volume/ platelet ratio; neutrophil to lymphocyte ratio (NLR) = neutrophil / lymphocyte ratio; derived neutrophil to lymphocyte ratio (dNLR)= neutrophils / (white blood cell- neutrophils); platelet to lymphocyte ratio (PLR)= platelet / lymphocyte ratio; monocyte to lymphocyte ratio (MLR)= monocyte / lymphocyte ratio); NLPR= neutrophils/(lymphocyte x platelet ratio); systemic inflammation response index (SIRI)= (neutrophils x monocytes)/lymphocytes; systemic immune-inflammation index (SII) = (neutrophils x platelets)/lymphocytes, and aggregate index of systemic inflammation (AISI) = (neutrophils x monocytes x platelets)/lymphocytes [11].
Statistical Analysis
Data were analyzed using IBM-SPSS version 21 (SPSS, Inc., Chicago, IL, USA). The normality of data distribution was tested using single sample Kolmogorov-Smirnov test. For normally distributed data, continuous variables were expressed as mean ± SD and were compared using Student's t test. Categorical variables were expressed as number (%) and were compared using chi-square (X2) or Fisher as appropriate. For non-normally distributed data, continuous variables were presented as median and interquartile range and compared using Mann-Whitney test. Correlation between MPR and different variables were done using Pearson's correlation. A receiver-operating characteristic curve (ROC) was generated. The area under the curve (AUC) and 95% CI were calculated. P value <0.05 was considered significant.
Results
Demographic and clinical data
Both hematological malignancies groups were age (p=0.798) and sex (p=0.738) matched. Seven patients (38.89%) were in the age group 20-30 years in both groups. Acute leukemias constituted 72.22% of COVID-19 positive cases (13 patients) (Table 1). All patients presented with acute nonspecific symptoms such as fever (38-38.5°C) and dyspnea. ICU admission (80%, 4 cases) and deaths (100%, 6 cases) were more in acute leukemia.

Hematological profile and blood cell-derived inflammation indexes
Comparison of hematological profile and blood cell -derived inflammation indexes between COVID-19 positive versus negative patients with hematological malignancies are shown in Tables 2 & 3. MPR was the only significantly different ratio between both groups (p=0.001) (Table 3). MPR was inversely correlated with platelets (r=-0.655, p=0.021). The cut-off points for MPR value ≤ 0.0339 (AUC=0.806; p=0.034; 95%CI: 0.594 -1) was associated with ICU admission (sensitivity: 88.9%, specificity: 75%) (Figure 1).
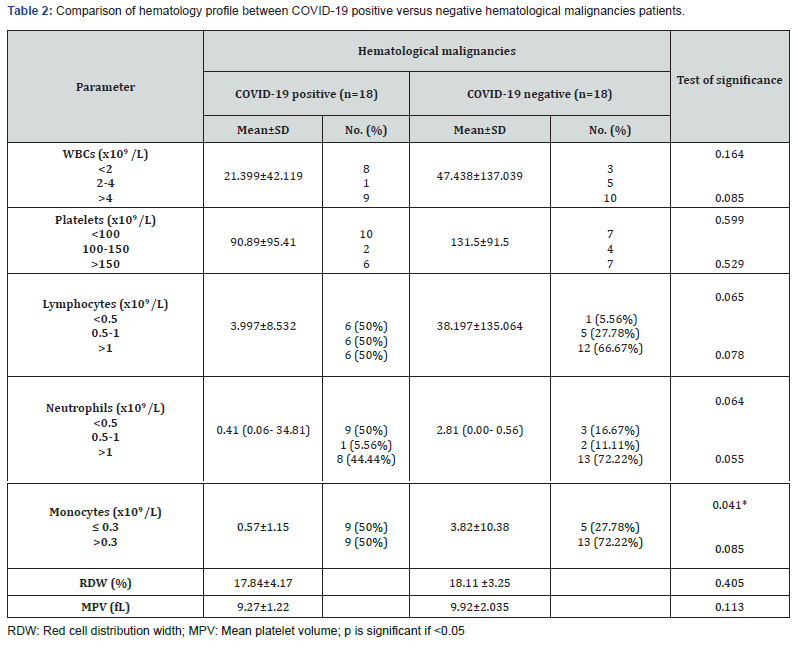
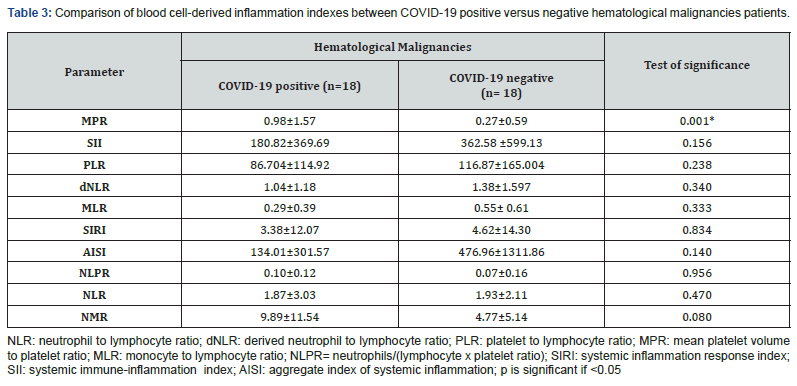
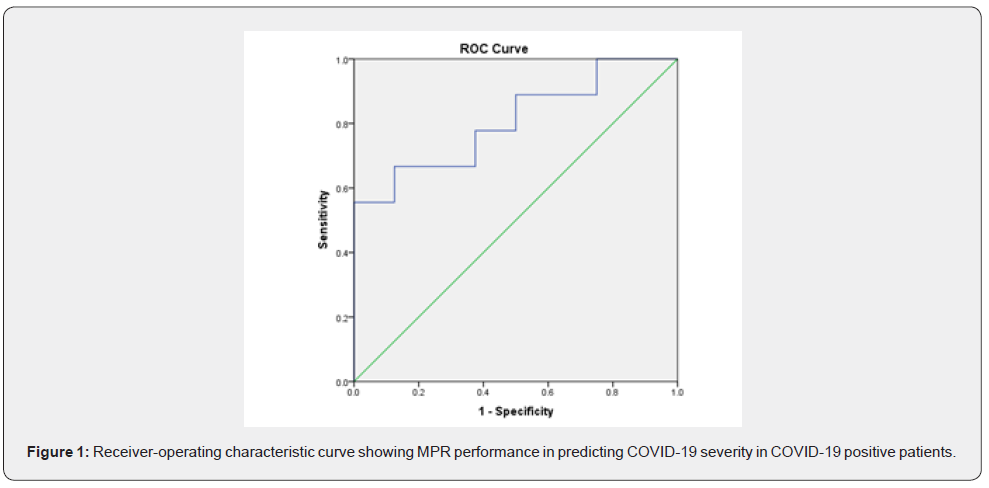

Table 4 shows comparison between COVID-19 positive non-ICU admitted (13 intermediate/ severe cases, 72.22%) and ICU admitted (5 critical cases, 27.78%). Absolute lymphopenia (> 0.6 x109/L) was present in 3 (60%) of ICU admitted cases.
Discussion
There is no association between COVID-19 infection and immune system cancer as more myeloid malignancies (55.56%) than lymphoid malignancies (44.44%) were COVID-19 positive in our cases. Acute leukemias comprise 72.22% of COVID-19 positive patients with the majority being AML (76.92%) perhaps due to more AML cases in this age group. COVID-19 associated hematological changes are indicators of systemic inflammatory response [12]. This inflammatory response is also common in cancer patients and is responsible for its progression [12]. This lessens the diagnostic significance of changes in some blood parameters in COVID-19 infected cancer patients. The main change in blood cell parameters in our COVID-19 positive patients are neutropenia, monocytopenia and higher MPR. Leucopenia, lymphopenia, and thrombocytopenia are present in nonmalignant COVID-19 positive cases [13] as well as in hematological malignancies due to several causes. Fifty percent of our COVID-19 cases had neutropenia which is mainly attributed to chemotherapy side effect and aggravated by neutrophil degranulation and lysis during severe infection [14]. Neutrophilia was present in only one patient with refractory acute monocytic leukemia. On the contrary, neutrophilia is a common finding in severe COVID-19 non-malignant cases due to immune dysregulation and superimposed bacterial infection [15].
Another important CBC parameter is RDW. Although RDW more than 14.5 at admission was associated with increase COVID-19 mortality risk from 11 to 31% in COVID-19 positive non-cancer patients [13], it is of less prognostic value in our COVID-19 positive cases. Insignificant increase in RDW was present in both hematological groups. This increase in RDW in cancer patients was explained by malnutrition, inhibition of gastrointestinal iron transport, the associated chronic inflammation [16] as well as anisocytosis resulting from decreased erythropoietin and increased cytokines and hepcidin [17].
The only significant blood cell-derived inflammation index between our groups was MPR. MPR is a combination of MPV and platelet counts. MPV was within the normal range (7.5-12 fl) [18] in both hematological groups. MPV value is variable in cancer patients being high in the majority and low in some cancers [18]. MPR was inversely correlated with the platelet counts in our COVID-19 cases. Thrombocytopenia was present in 55.56% of our COVID-19 positive patients. Thrombocytopenia (as high as 57%) was present in non survivors COVID-19 positive non cancer patients [15]. Thrombocytopenia in our cases is explained by disease process, chemotherapy side effect, or COVID-19 complications including COVID-19 invasion of bone marrow hematopoietic cells or stromal cells [7].
Comparing ICU admitted and non-ICU admitted cases revealed presence of lymphopenia (>0.6 x109/L) in 60% of our ICU cases which is against its use as an early indicator of ICU admission as proposed by Fan et al in nonmalignant cases [19]. MPR was the only significantly different index between our COVID positive ICU admitted and non-ICU admitted cases. MPR value ≤ 0.0339 had sensitivity: 88.9% and specificity: 75% in early diagnosis of those in need for ICU admission.
Conclusion
Our findings indicate that MPR was the only reliable marker in COVID-19 positive cases. It must be calculated at COVID-19 diagnosis and at regular intervals to predict early need for ICU admission
Funding
No funding was received by the authors for conducting this study.
Compliance with Ethical Standards
Conflict of Interest: the authors declare they have potential conflicts of interest, neither financial nor non-financial
Human and animal Rights
The study was conducted using human blood samples and an approval by the Ethics Review Board of Alexandria University, Faculty of Medicine was obtained.
References
- Toledo SL, Nogueira LS, Carvalho M, Eios DRA, Pinheiro M (2020) COVID-19: review and hematologic impact. Clinica Chimica Acta 510: 170-176.
- Yu Z, Wang P, Chen B, Zhang Z, Jiang J, Zhuang Y (2020). Clinical, inflammatory and immune differences between COVID-19 patients with and without cancer. A protocol for systematic review and meta-analysis. Medicine 99(45): e23015.
- He W, Chen L, Chen L, Yuan G, Fang Y, et al (2020) COVID-19 in persons with hematological cancers. Leukemia 34: 1637-1645.
- Niu A, Ning B, Socola F, Safah H, Renolds T, et al (2020) COVID-19 in patients with hematologic malignancies: High false negative rates with high mortality. Blood 136: 3.
- Usul E, San I, Bengoz B, Sahin A (2020) Role of hematological parameters in COVID-19 patients in the emergency room. Biomark Med 14(13): 1207-1215.
- Henry BM, Benoit JL, Benoit S, Pulvino C, Berger BA, et al (2020) Red blood cell distribution width predicts COVID-19 severity: A prospective, observational study from the Cincinnali SARS-CoV-2 emergency department cohort. Diagnostics 10(9): 618-624.
- Qu R, Ling Y, Zhang Y, Wei L, Chen X, et al. (2020) Platelet-to-lymphocyte ratio is associated with prognosis in patients with coronavirus disease-19. J Med Virol 92(9): 1533-1541.
- Rahi MS, Jindal V, Sandra-Patrucco Reyes, Kulothungan Gunasekaran, Ruby Gupta, et al. (2021) Hematologic disorders associated with COVID-19: A review. Ann Hematol 100(2): 309-320.
- Hu D, Lippi G, Montagnana M (2020) Diagnostic and prognostic value of red blood cell distribution width in sepsis: A narrative review. Clinical Biochemistry 77: 1-6.
- Liu X, Shen Y, WangH, Ge Q, Fei A, (2016) Prognostic significance of neutrophil-to- lymphocyte ratio in patients with sepsis: A prospective observational study. Mediators of Inflammation 2: 1-8.
- Fois AG, Paliogiannis P, Scano V, Cau S, Babudieri S, Perra R, et al. (2020) The systemic lnflammation lndex on admission predicts in-hospital mortality in Covid-19 patients. Molecules 25(23): 5725-5738.
- Chen L, Kong X, Yan C, Fang Y, Wang J (2020) The research progress on the prognostic value of the common hematologic parameters in peripheral venous blood in breast cancer. OncoTargets and Therapy 13: 1397-1412.
- Foy BH, Carlson JCT, Reinertsen E, Valls RPI, Lopez RP, et al. (2020) Association of red blood cell distribution width with mortality risk in hospitalized adults with SARS-CoV-2 infection. JAMA Network Open 3(9): e2022058.
- Anurage A, Jha PK, Kumar A (2020) Differential white blood cell count in the COVID-19: A cross -sectional study of 148 patients. Diabetes & Metabolic Syndrome: Clinical Research & Reviews 14: 2099-2102.
- Sahu KK, Siddiqui AD (2020) From hematologist's desk: the effect of COVID-19 on the blood system. Am J Hematol 95(8): E213.
- Herraez I, Bento L, Campo RD, Sas A, Ramos R, Ibarra J, et al. (2020) Prognostic role of the red blood cell distribution width in Hodgkin lymphoma. Cancer 12(11): 3262.
- Korniluk A, Koper-Lenkiewics OM, Kaminska J, Kemoa H, Dymicka-Piekarska V (2019) Mean platelet volume: new perspectives for an old marker in the course and prognosis of inflammatory conditions. Mediators of Inflammation 2019: 9213074.
- Ai L, Mu S, Hu Y (2020) Prognostic role of RDW in hematological malignancies: a systematic review and meta-analysis. Cancer Cell Int 18: 61.
- Fan BE, Chong VCL, Chan SSW, Lim GH, Lim KGE, et al. (2020) Hematologic parameters in patients with COVID-19 infection. Am J Hematol 95(6): E131-34.






























