Surface Radiation Dose Measurement with Mosfet for Head and Neck Cancer using Phantom
Vivek Mishra*, Shreekripa Rao and Rechal Nisha D’Souza
Department of Radiotherapy and Oncology, Manipal College of Health Professions, India
Submission: February 09, 2021; Published: March 05, 2021
*Corresponding Address: Vivek Mishra, Department of Radiotherapy and Oncology, Manipal College of Health Professions Udupi, Karnataka, India
How to cite this article: Vivek Mishra, Shreekripa Rao,Rechal Nisha D’Souza. Surface Radiation Dose Measurement with Mosfet for Head and Neck Cancer using Phantom. Canc Therapy & Oncol Int J. 2021; 18(2): 555984. DOI:10.19080/CTOIJ.2021.18.555984
Abstract
Aim: The focus of this study was on the surface dose received by the patients during radiation treatment.1.2.
Materials & Method: MOSFET (“Metal-Oxide-Semiconductor Field-Effect Transistor”) detector due to its small size and greater reproducibility and sensitivity was used. Calibration of MOSFET was done to check for its accuracy and linearity along with field size dependence, dose-rate dependence, and angular dependence. Patient plans with Head & Neck cancer were taken and loaded onto the MOSFET. VMAT (“Volumetric-Modulated Arc Therapy”) and 3DCRT (“3-Dimensional Computed Radiation Therapy”) both techniques plans were taken.
Result: Angular, field size, and dose-rate dependence was found to be ±1%, ±2.76%, and ±1.64% respectively.
Conclusion: The measured values from MOSFET agreed with TPS (Treatment Planning System) calculated values for surface dose with 95% confidence.
Keywords: Metal; Oxide; Semiconductor; Transistors; Electronic; and Radiotherapy Dosage
Abbreviations: MOSFET: Metal-Oxide-Semiconductor Field-Effect Transistor; QA: Quality Assurance; EBRT: External Beam Radiation Therapy; SSD: Source to Skin Distance; MLC: Multileaf Collimator; VMAT: Volumetric-Modulated Arc Therapy; 3DCRT: 3-Dimensional Computed Radiation Therapy; IMRT: Intensity Modulated Arc Therapy; SRS: Stereotactic Radiosurgery; SBRT: Stereotactic Body Radiation Therapy; PBC: Pencil Beam Convolution; CC: Collapsed Cone; AAA: Analytical Anisotropic Algorithm
Introduction
In Teletherapy or External Beam Radiation Therapy (EBRT) radiation enters from external to the patient body to deliver a dose to the tumor. Ideally, all the radiation should be delivered to the tumor but practically a part of the radiation is attenuated on the surface while radiation enters the patient body. This attenuated part contributes to what is known as Surface Dose. Attenuation of radiation beam causes radiation damage in any of the three layers of the skin which are the Subcutaneous tissue, Dermis, and Epidermis. The damage can be Late skin reaction and Early skin reaction [1]. Measurement of surface dose portrays a greater technical challenge since the distance to the superficial layer is small. MOSFET with a very small size and ease of use make them excellent candidates for clinical patient measurements [2]. The dose to the surface mainly depends on the field size, source to skin distance (SSD), beam energy, beam angle, and beam modifiers such as multileaf collimator (MLC), block systems, and types of beam used to treat the tumor [3-5]. Currently, for clinical purposes three types of radiation
beams are being used 1) photon beam, 2) electron beam, 3) proton beam. For the photon beam, the surface dose is 20% - 40% of the prescribed dose. For the proton beam, the surface dose is 40% - 50% of the total prescribed dose. For the electron beam, the surface dose is 60% - 80% of the total prescribed dose. As the surface dose increases, the dose to the nearby surrounding organ also increases resulting in unnecessary damage to the organ [6-8]. As the principle of radiotherapy says that ‘for an efficient treatment maximum dose should be given to the tumor while minimizing the dose to the nearby normal tissue’. An increment in the surface dose will violate the fundamental radiotherapy principles.
Materials and Methods
Computed Tomography
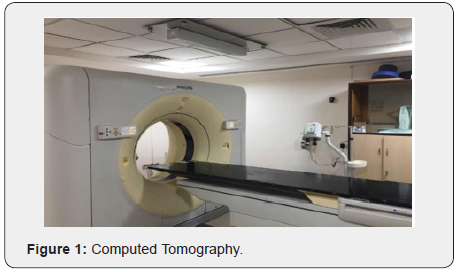
(Figure 1) “Philips Brilliance Big bore 16 slice CT” is a machine that was used to image the setup used for the study and images taken were sent to the TPS via DICOM. It has a ring of detectors and an X-ray tube. The tube circle around the patient and the low energy X- ray is detected by the detector ring. The construction of the CT image is done by a matrix of relative linear attenuation coefficients. CT images can be taken either slice- by-slice or helical geometry. A transverse 2D image taken by CT is reconstructed in a 3D image using the software. The bore diameter of 85 cm with a gantry tilt of -300 to +300 with 0.50 increments.
SP-34 slabs -
RW3-PL phantom was used for the setup (Figure 2). These are water equivalent material with a density of 1.045 g/cm3. The electron density of the material is 1.012 times higher than that of water. These slabs are used to measure the dose. They are made up of polystyrene C8H8 containing 2% TiO.

Linear Accelerator
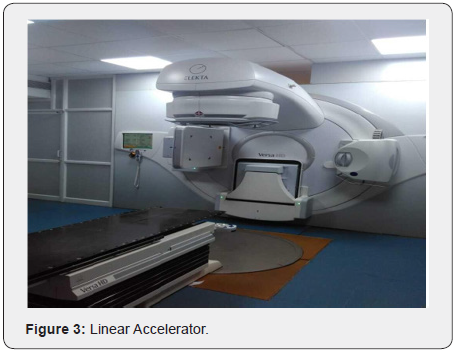
LINAC (“Elekta Versa HD”) is a device that is used for this study (Figure 3). It produces photon and electron beam in the energy range useful for clinical purposes. Linac consists of many components such as an electron gun, focusing cup, anode, source, primary and secondary collimator, and many more. Linac is a device used as EBRT in the treatment of cancer. It accelerates charged particles to high energies. Clinical Linac accelerates an electron to high energies which are used to treat superficial cancer. This high-energy electron can be made to strike on the Tungsten source to produce photon beams that are used to treat a deepseated tumor. Photon energies are 6MV, 10MV, 15MV, 6MVFF, and 10MVFFF while electron energies are 4MeV, 6MeV, 8MeV, 10MeV, 12MeV, and 18Mev. The treatment techniques available are 2D-3DCRT, VMAT, IMRT (Intensity Modulated Arc Therapy), SRS (Stereotactic Radiosurgery), and SBRT (Stereotactic Body Radiation Therapy). It has 80 pairs of MultiLeaf Collimator of 0.5 cm thickness at isocentre.
MOSFET
“Portable Dosimeter TN-RD-90” dosimeter is a small handheld device that was used for measuring the intensity and for direct reading of radiation exposure (Figure 4). Since it is based on the MOSFET transistor, the principle of operation is the same as that of semiconductor detectors. Its major benefit is its small dimension, which is less than 4 mm2. In radiation dosimetry, TLD dosimeters are often replaced by MOSFET dosimeters since they offer immediate readout [9]. It comes with an active area of 0.2x0.2 mm2. Resolution of 0.1 mV over an accumulated total of 20,000 mV. The radiation that passes through the detector ionizes semiconductor atoms, forming pairs of electron-hole. Electronhole pairs are formed by incident radiation within the depletion layer [10]. Electron mobility in SiO2 at room temperature is around four orders larger than holes, move rapidly out of the gate electrode while holes move stochastically to the Si/SiO2 interface where they are stuck in long-term locations, creating a negative voltage shift (VTH) that can persist for years [11]. The difference in the voltage change can be measured before and after exposure and is proportional to the dose.

Treatment Planning System
Monaco TPS is used to plan external beam irradiation with photon and electron beams. This software can plan for SBRT, SRS, VMAT, 3DCRT, and IMRT. The software works on the algorithm to find out the dose distribution to desired volumes and structure. It also tells about doses received by any organs during radiation treatment and defines the region of hot and cold spots within and outside the planning volume. The algorithms it uses are PBC (Pencil Beam Convolution), CC (Collapsed Cone), AAA (Analytical Anisotropic Algorithm), and Monte Carlo.
Procedure
Computed Tomography Scanner
CT scans of the SP-34 slabs with MOSFET were taken with the same setup as in the linac [12]. Two CT scans were taken with and without the build-up cap on the MOSFET. For Head & Neck cancer often 3mm slice CT scans are taken so for this study also CT scans were taken with 3mm slice thickness and voltage was kept at 120kV. Scans were sent to the TPS via DICOM.
MONACO Treatment Planning System
The study’s purpose is to investigate the surface dose in Head & Neck cancer. So, plans of the Head & Neck cancer patients were selected irrespectively of gender. Pre-planned cases were taken for the conduction of this study. These plans were taken from the Monaco Treatment Planning System (TPS) [12]. In this department for Head & Neck cancer, 3D-CRT or VMAT is a preferred technique hence an equal number of cases were taken for both 3D-CRT and VMAT.
CT scans of the setup were loaded on the TPS in Quality Assurance (QA) mode. Pre- planned selected cases of the patients were loaded on the CT scan of the setup. While loading the data on the setup scan gantry and the couch angles were locked to zero degrees. For each patient two QAs were planned with and without a build-up cap. After loading the patient plan, the dose calculation was done and the dose to the surface of the MOSFET was noted down by using the Volume cursor.
MOSFET
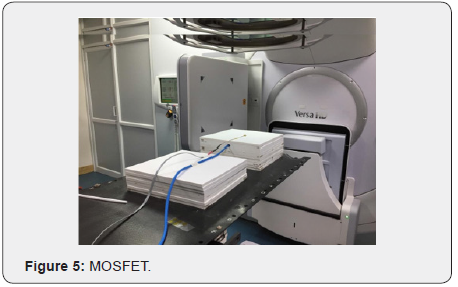
For study purposes, calibration of MOSFET was done to check its dependence on energy, angle, dose-rate, and field size (Figure 5). For calibration purposes, MOSFET was placed on the top of the SP-34 slab phantom and cross-calibrated against 0.66 cc Farmer chamber [3,13]. 10 SP-34 slabs were used for the backscattering. SSD was kept 100 cm on the surface of MOSFET with a field size of 10x10 cm2.
To check for the dependence of the angle Readings were taken for gantry angle 00, 900, 1800, 3600. MOSFET was irradiated with 50 cGy. For field size dependence MOSFET was irradiated with 50 cGy for various field sizes from 5x5 cm2 to 40x40 cm2 in the step of 5x5cm2 [14,15]. For dose-rate dependence, MOSFET was irradiated with 100 cGy for dose-rates ranging from 100 MU/min to 600 MU/min in steps of 100 MU/min with field size opened 10x10 cm2 [16,17]. The linearity of MOSFET was checked to make sure its response is linear with the dose delivered. For this MOSFET was irradiated with 100 cGy with varying monitor unit from 10 MU to 410 MU in the step of 50 MU and the response was noted down [18,19]. For surface dose measurement using MOSFET, 10 SP-34 slabs were set for the backscattering, and MOSFET was kept on the surface of the SP-34 slabs. SSD was kept 100cm on the surface of MOSFET. Patient plans were selected from Mosaiq and loaded to Integrity overriding the gantry and couch angles to zero degrees. Before executing the plans, the MOSFET calibration factor was set (The ratio of the measured voltage difference value (ΔV) to the radiation dose delivered determines the calibration factor) and MOSFET was operated on the manual mode. The START button was pressed on the MOSFET before coming out of the treatment room, and the plans were executed.
For 3DCRT, readings were taken for each gantry angle. Similarly, VMAT readings were taken for each arc. Once the dose was delivered for an angle or an arc reading were taken by pressing either the Read 1 or Read 2 button on the MOSFET and after reading, the START button was pressed so that the next reading could be taken. The dose measured by MOSFET was noted down in cGy. Likewise, with the same setup and the same patient plans, readings were taken with a build-up cap on the MOSFET. This was done to get the build-up dose.
Data Analysis
In general, in this study, there are two groups of data on the surface dose, and the motive of this study is to compare and inform which data is reliable. So, for this study for data analysis one-tailed T-test is used with the Null hypothesis that there is no difference between the two data and the Alternate hypothesis that there is a significant difference between the two data.
Result
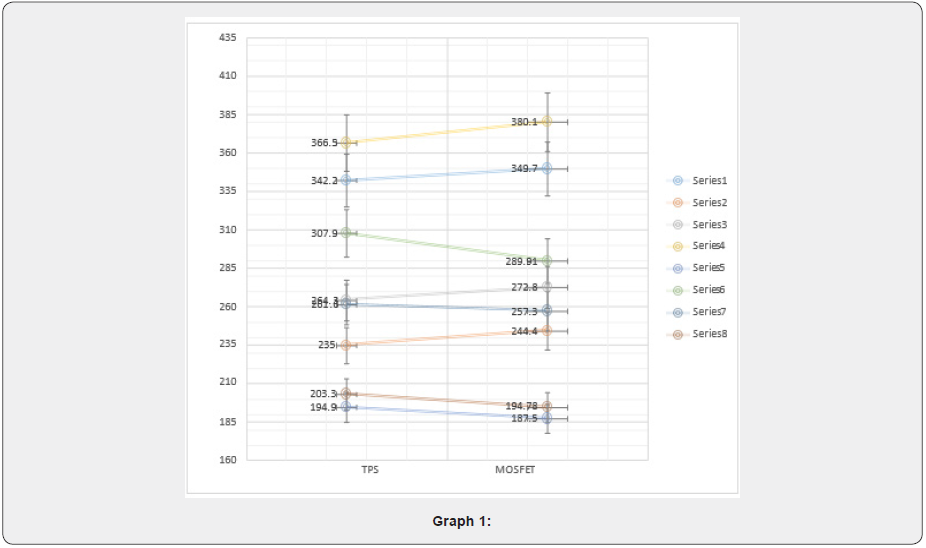
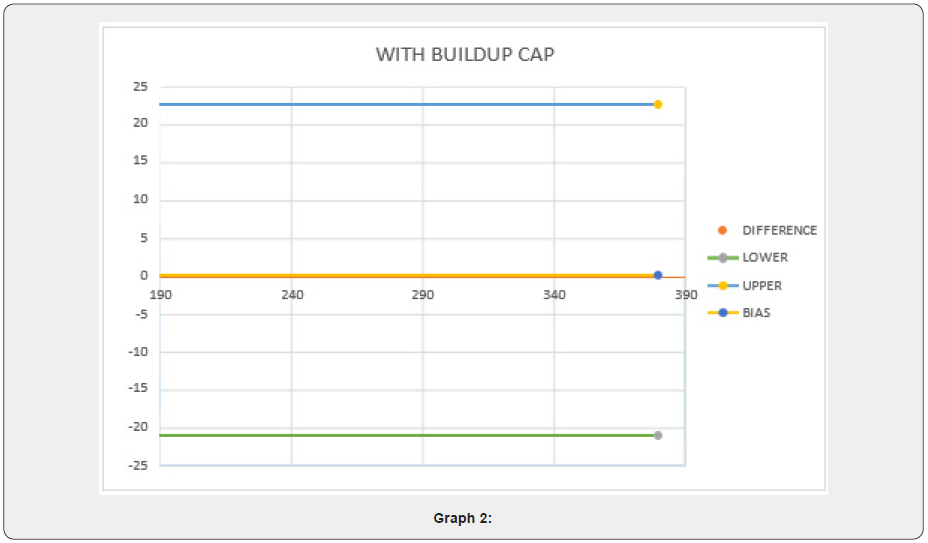
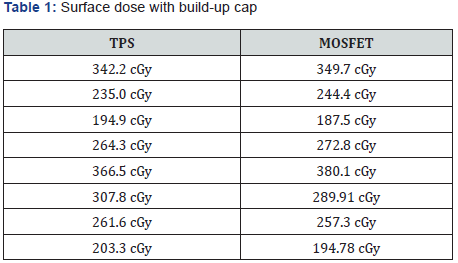
On doing a single-tailed t-test on the above-shown data (Table 1). The difference in the Surface dose between TPS (Mean = 271.95; SD = 62.49) and MOSFET (Mean = 272.06; SD = 67.74) was significant (t(8) = -0.00341; p = 0.498662 > 0.05) with 95% confidence interval as shown in graph 2 using Bland Altman plot with 2-SD. Since the p-value for this data is greater than 0.05 so, it is elucidating that the null hypothesis is correct, and the alternate hypothesis is wrong. This signifies that the difference between the two data on the surface dose of MOSFET and TPS is within the limit of ±5% (Graphs 1 & 2) (Table 2).
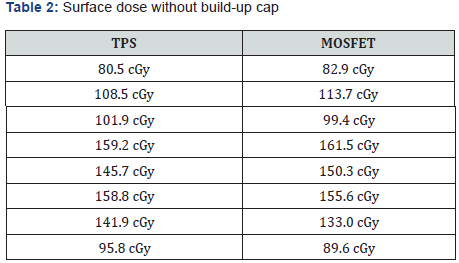
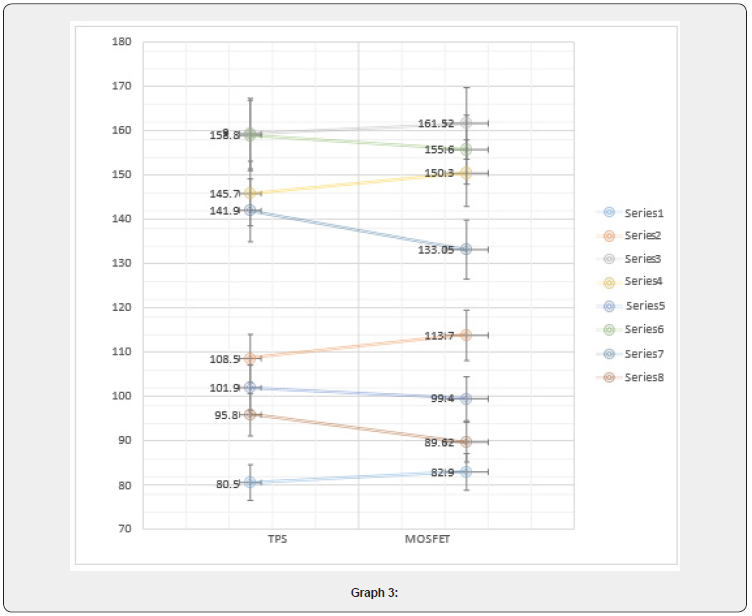
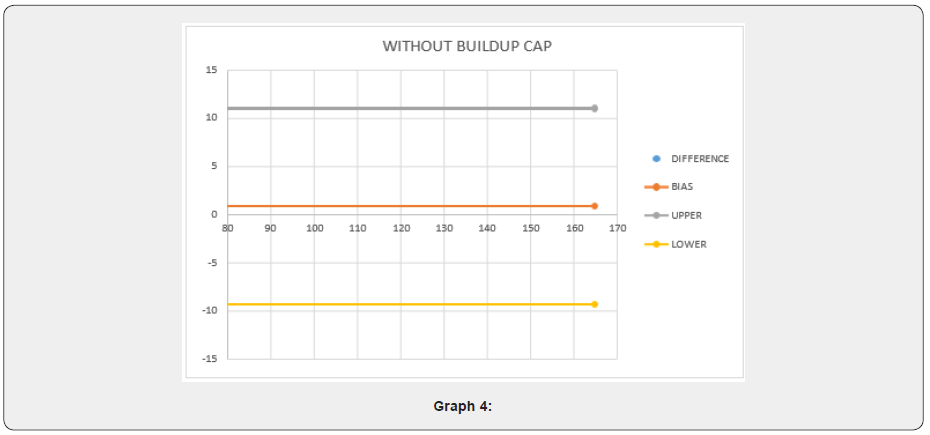
On doing a single-tailed t-test on the above-shown data. The difference in the Surface dose between TPS (Mean = 124.04; SD = 30.83) and MOSFET (Mean = 123.25; SD = 31.06) was significant (t(8) = 0.05088; p = 0.480 > 0.05) with 95% confidence interval as shown in graph 4 using Bland Altman plot with 2-SD. Since the p-value for this data is greater than 0.05 so, it is elucidating that the null hypothesis is correct, and the alternate hypothesis is wrong. This signifies that the difference between the two data on the surface dose of MOSFET and TPS is within the limit of ±5% (Graphs 3 & 4).
Discussion
The higher surface dose is a critical issue and a great challenge in the field of Radiation Therapy. Since the Head & Neck region consists of many important organs higher surface doses to this region can enhance the chances of radiation-induced damage to these crucial organs. Higher surface doses possess complications to the skin such as erythema, telangiectasia, necrosis, epilation, and desquamation. The first outcome of this study indicates that there is no significant difference in the reading of MOSFET and TPS calculation for the surface dose and the difference is within ±5% of the percentage deviation as given in Table 2. This means that the TPS plan is accurate and the surface dose knowledge has been taken into consideration. Inadequate knowledge of the surface dose can affect the dose uniformity in planning volumes. Laurence E. Court et al. [5] reported an agreement between measured skin dose and calculated skin dose of ±20% for 95% of all the measured data.
Similarly, the data present in Table 1 shows no significant difference between readings and the calculated values of the dose on the surface of MOSFET with a build-up cap the difference is within ±5% of the percentage deviation. This signifies that the doses at a certain depth (less than or equal to 0.6cm) have not a significant difference, and which is within measurement uncertainty. This agrees with Zhen-Yu Qi et al. [1] report. Since VMAT and 3D-CRT both cases were taken in this study and execution of the plan was done with gantry and couch set at zero. Small overestimation was found in the dose calculated for VMAT by TPS for both with and without a build-up cap. The reason for this could be the continuous changes in the fluence as the Multi- Leaf Collimator (MLC) was moving continuously. The number of plans in this study is less so there is a possibility of change in the outcome with increasing the number of plans. Since the study was done on the phantom, the results may vary when doing on the patients.
Conclusion
During radiation treatment, a significant amount of dose is absorbed on the surface of the patient which leads to serious complications on the skin. This surface dose is of more consideration when treating Head & Neck cancer since this region has many radiosensitive organs.
Seeing that the skin anatomy is very small around 0.07mm in the dimension, recording a dose at this depth is a challenging issue. As the size of MOSFET is very small compared to most of the detectors its use for surface dose measurement leads to a very precise reading. The surface doses found from TPS and MOSFET can differ and this could lead to improper planning of treatment. So, this study aid in understanding the correlation between the TPS and MOSFET and predict which treatment technique can be better in reducing the surface dose. MOSFET, in general, can sometimes give absurd readings because of fading-out or physical damages. This can mislead the results, so MOSFET should be calibrated before proceeding with readings. The result of this study was that the differences in the readings were within the limit and VMAT TPS readings had a small overestimation compare to 3DCRT TPS readings.
References
- Qi ZY, Deng XW, Huang SM, Zhang L, He ZC, et. al. (2009) In vivo verification of superficial dose for head and neck treatments using intensity‐modulated Medical physics 36(1): 59- 70.
- Verhaegen F, Lemire M, Hallil A, Hegyi G (2008) Surface dosimetry in a CT scanner using MOSFET detectors and Monte Carlo simulations. InJournal of Physics (Vol. 102, No. 1, p. 012026).
- Akbas U, Donmez Kesen N, Koksal C, Bilge H (2016) Surface and buildup region dose measurements with Markus parallel-plate ionization chamber, GafChromic EBT3 film, and MOSFET detector for high-energy photon beams. Advances in High Energy Physics.
- Dias AG, Pinto DF, Borges MF, Pereira MH, Santos JA, et. al. (2019) Optimization of skin dose using in‐vivo MOSFET dose measurements in bolus/non‐ bolus fraction ratio: A VMAT and a 3 DCRT Journal of applied clinical medical physics 20(2): 63-70.
- Court LE, Tishler RB, Allen AM, Xiang H, Makrigiorgos M, et. al. (2008) Experimental evaluation of the accuracy of skin dose calculation for a commercial treatment planning system. Journal of applied clinical medical physics 9(1): 29-35.
- Vlachopoulou V, Malatara G, Delis H, Theodorou K, Kardamakis D, et. al (2010) Peripheral dose measurement in high-energy photon radiotherapy with the implementation of MOSFET. World journal of radiology 2(11): 434-439.
- Jong WL, Ung NM, Wong JH, Ng KH, Ishak WW, et. al. (2016) In vivo skin dose measurement using MOSkin detectors in tangential breast radiotherapy. Physica Medica 32(11): 1466- 1474.
- Legge K, Greer PB, O’Connor DJ, Wilton L, Richardson M, et. al (2017) Real-time in vivo rectal wall dosimetry using MO Skin detectors during linac based stereotactic radiotherapy with rectal displacement. Radiation Oncology 12(1): 41.
- Peet DJ, Pryor MD (1999) Evaluation of a MOSFET radiation sensor for the measurement of entrance surface dose in diagnostic radiology. The British journal of radiology 72(858): 562-568.
- Gotoh s, takagi z (1964) Silicon Surface Barrier Detector. Journal of Nuclear Science and Technology 1(8): 311-315.
- Sors A, Cassol E, Latorzeff I, Duthil P, Sabatier J, et. al. (2014) An optimized calibration method for surface measurements with MOSFETs in shaped-beam radiosurgery. Physica Medica 30(1): 10-17.
- Eng KY, Kandaiya S, Yahaya NZ (2017) Radiotherapy dose verification on a customized head and neck perspex phantom. InJournal of Physics: Conference Series (Vol. 851, No. 1, p. 012020).
- Butson MJ, Cheung T, Peter KN (2005) Peripheral dose measurement with a MOSFET detector. Applied Radiation and Isotopes 62(4): 631-634.
- Qin S, Chen T, Wang L, Tu Y, Yue N, et. al. (2014) Angular dependence of the MOSFET dosimeter and its impact on in vivo surface dose measurement in breast cancer treatment. Technology in cancer research & treatment 13(4): 345-352.
- Mattar EH, Hammad LF, Al-Mohammed HI (2011) Measurement and comparison of skin dose using One Dose MOSFET and Mobile MOSFET for patients with acute lymphoblastic leukemia. Medical science monitor: international medical journal of experimental and clinical research 17(7): MT51-MT55.
- Kumar AS, Sharma SD, Ravindran BP (2014) Characteristics of mobile MOSFET dosimetry system for megavoltage photon beams. Journal of medical physics/Association of Medical Physicists of India 39(3): 142-149.
- Jong WL, Ung NM, Tiong AH, Rosenfeld AB, Wong JH (2018) Characterization of a MOSFET-based detector for dose measurement under megavoltage electron beam radiotherapy. Radiation Physics and Chemistry 144: 76-84.
- Gopiraj A, Billimagga RS, Ramasubramanian V (2008) Performance characteristics and commissioning of MOSFET as an in-vivo dosimeter for high energy photon external beam radiation therapy. Reports of Practical Oncology & Radiotherapy 13(3) :114-25.
- Denia PM, García MD, García CM, Higueras JD, de Marco Blancas N, et. al. (2019) Comparison of detector performance in small 6 MV and 6 MV FFF beams using a Versa HD accelerator. PloS one 14(3).






























