The Use of DRR Designed Fields Is Unnecessarily Toxic and Geographically Inadequate, Analysis of Drr Designed Fields in Preoperative Radiotherapy in Rectal Cancer
Moustafa Al Daly1* and Ahmed Hassan2
1Clinical oncology Department, Cairo University, Egypt
2Clinical Oncology Department, Beni Suef University, Egypt
Submission: August 24, 2018; Published: September 28, 2018
*Corresponding Address: Moustafa Al Daly, Clinical oncology Department, Cairo University, Kasr Al Ainy Hospital.
How to cite this article: Moustafa A D, Ahmed H. The Use of DRR Designed Fields Is Unnecessarily Toxic and Geographically Inadequate, Analysis of Drr Designed Fields in Preoperative Radiotherapy in Rectal Cancer. Canc Therapy & Oncol Int J. 2018; 12(2): 555832. DOI: 10.19080/CTOIJ.2018.12.555832
Abstract
Background: The DRR images and skeletal landmarks are widely used to design treatment portals in preoperative treatment of cancer rectum followed by assessment of isodose lines evaluation, however this practice lacks real volumetric assessment of delivered dose to target volumes and risk organs.
Aim: To assess the dose delivered to target volumes and normal organs with and without contouring.
Methods: 10 cases of treated cancer rectum CTs were selected, previously treated by conventional technique using DRR and skeletal landmarks, same cases were contoured using RTOG atlas to create CTV 45 Gy (Rectum + tumor, mesorectum and LN (presacral, internal iliacs and obturator LN) and then 1 cm was added for final PTV design, urinary bladder as well as bowel bag were also contoured. Two volumes were designed and named PTV contouring and PTV DRR (opposite to DRR isodosline 95%).
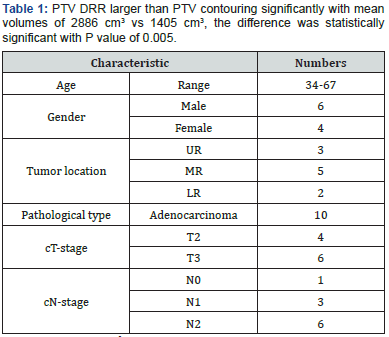
Results: PTV DRR was nearly double PTV contouring with mean volumes 2886 cm3 and 1405 cm3 respectively, p value of 0.005. Coverage was not optimum with mean volume received therapeutic dose 93.5 %. Doses to urinary bladder and bowel was similar to others conventional 2D and may be little bit higher with mean results for urinary bladder V20 100%,30 89%, V40 89%, and bowel V20 51%, V30 32.5, V40 26%.
Conclusion: the use of DRR designed fields, guided by skeletal landmarks, results in over irradiation of normal pelvic structures, and may miss the treatment volume especially for low rectal tumours, visual assessment of isodose lines on non-contoured cuts is significantly misleading.
Introduction
Rectal adencarcinoma is one of the earliest GIT sub sites to benefit from preoperative combined chemo radiotherapy (CCRT). With the results of several randomized trials combined chemo radiotherapy was able to reduce the risk of loco-regional recurrence and chances for sphincter sparing [1-3]. Most of the CCRT trial were performed before the tremendous advances in radiation technology. Two-dimensional radiotherapy using skeletal landmarks was the standard of care at that time, together with the use of three or four fields orientation and use of arbitrary designed corner blocks to protect normal risk organs [4].
Currently there are a lot of published 3D CT based guidelines for delineation of rectal tumors, however and in spite of the availability of CT data, the practice of field design using skeletal landmark on DRR and rechecking CT images for dose distribution still not uncommon practice at many RTH centers in our country especially those with high work load [5]. The aim of our study is to assess DRR guided portal design vs. contouring based. For both Tumor coverage and radiotherapy dose to organs at risk (OAR).
Methods
Between 2013-2014, Ten cases of locally advanced cancer rectum treated at Cairo university oncology center were selected, all patients were treated using DPX machine of Varian medical systems, and planned on Eclipse version8.5, using standard 3-4 fields orientation with the dose of 45 Gy /25 F/5 weeks in a dose of 1.8 Gy /fraction. All those patients were treated without contouring using DRR to define treatment field’s. For all DRRs a new structure was created representing isodose line 95% and considered as treated volume which receive therapeutic radiation dose of 45 Gy/25f/5W. DRR Volume (isodose line 95%) was compared to contouring volume for each patient regarding volumetric measurement as well as geographic miss, Urinary bladder and bowel dose were contoured and V20, V30, V40 as well as mean dose were obtained.
i. DRR Arm: (guided by standard skeletal landmarks to include) [4].
ii. Posterior Field: Upper border L5-S1.
iii. Lower Border: Ischial tuberosity or 2 cm below any lesion whichever lower.
iv. Lateral Pelvic prim+ 1.5 cm to include internal lilacs.
v. Lateral Field: Anterior border: posterior 1/2 Of symphysis pubis unless there is an anterior pelvic organ involvement (border moved to include tip of symphysis)
vi. Posterior border: covering the posterior aspect of the sacrum.
vii. Upper and lower borders: same as for posterior field. MLC blocking was arbitrary added to minimize doses to OAR (corner blocks to minimize dose to bowel and urinary bladder).
viii. Contouring arm: For all previous patients contouring was done following RTOG Anorectal atlas guidelines for both CTV and OAR [5].
ix. Upper landmark: Reaching up to the bifurcation of iliac vessels to internal and external iliacs.
x. Lower landmark: down to pelvic floor muscles or 2 cm below visible tumor by CT or MRI.
The entire rectum is delineated starting from recto sigmoid junction down to anorectal junction plus 2 cm above or below any detected tumor, as well as mesorectal fascia and presacral lymphatics. Common and internal iliac vessels plus obturator group are contoured in all cases, External iliacs are only included for T4 disease with involvement of anterior pelvic organs.
Results
Contouring vs. DRR volume.
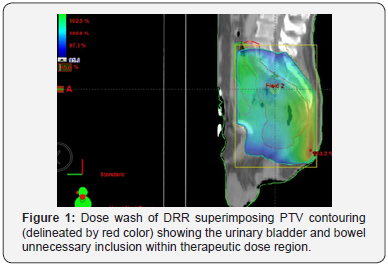
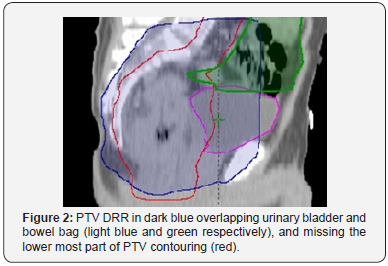
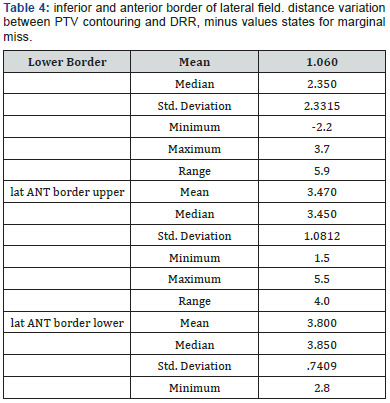
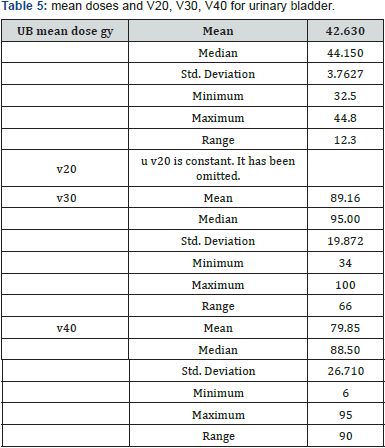
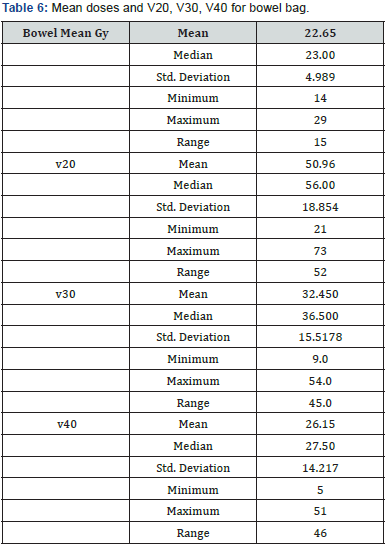
Patients Tables 1-3 patient’s characteristics. All patients were diagnosed as rectal adenocarcinoma mid rectum was the most predominant site and mainly T3N +ve disease. Under coverage was evident near the inferior border, in three cases the lower border of PTV contorting was lower to DRR with a range from 1.3-2.2 cm. in two cases the antro-superior block of the lateral field was close (0.5-0.8 cm). The Anterior border of the lateral field was the most variable border, compared to the upper and posterior borders that relies basically on bony limits. In order to assess variation in position of the anterior border distance from PTV DRR (opposite 95% isodose) till PTV contouring + 0.5 cm (as margin for beam penumbra) was measured. Two levels were selected in upper and lower thirds of the lateral field (Tables 4 & 5). In all 10 cases urinary bladder was contoured and mean dose V20,30,40 were reported. Also bowel bag was contoured for all cases, starting from L5-S1 to the lower most visible loops, excluding the rectum. mean dose V20,30,40 were reported (Table 6) (Figures 1 & 2).
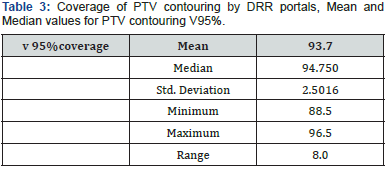
Coverage: PTV DRR vs PTV contouring.
Discussion
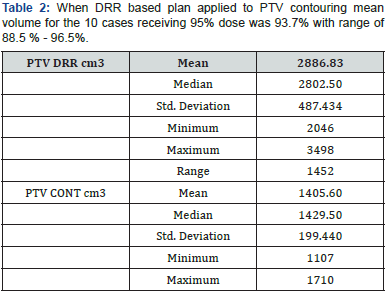
Since the late nineties radiotherapy practice had witnessed progressive replacement of two-dimensional radiotherapies with 3D conformal and latter IMRT, and consequent shift from skeletal marks designed fields towards the CT based radiotherapy, this change resulted in increasing need for more sophisticated volume definition, and more increase in radiotherapy workload [6]. While change in radiotherapy practice was really fast in head and neck and prostatic cancers. other subsites, including rectal cancer, were treated using conventional DRR images and visual assessment isodose lines for dose coverage [7]. While This practice lacks real volumetric data and DVH assessments it remained as standard of care for long time, even some of the land mark trials utilized the 2d definitions for its radiotherapy protocols [8]. In our study the most evident result was the big volumetric difference between DRR arm and contouring arm, were DRR volume was nearly double that of contouring with the mean value of 2886 cm3 for DRR vs 1405 cm3.for PTV contouring. Our results are little bit larger than other similar studies were 2D PTV volume were usually larger but not that much generous [9].
The most variable border between DRR and contouring arms was the anterior border of the lateral field, when the distance between the anterior border of PTV contouring and anterior border of PTV DRR was measured, medium value of added cm was 3.45 cm and 3.8 cm for the upper and lower parts of the field respectively. In spite of apparently more generous field, PTV contouring coverage was not the optimum. mean volume for the 10 cases receiving 95% dose was 93.7% with range of 88.5 % - 96.5%. This could be explained by the under coverage of the lower most part of rectum that could be lower than the Ischial tuberosity, noticed in 3 patients with inadequate borders of 1.3- 2.2 cm. our results coincide with the findings of Corner et al were 58% of the 2D planes were undertreated due to geographic miss in both lower and antro-suprior corner of the lateral field. Similar comment on under coverage was reported by Italian study, under coverage were seen opposite to antro-superior corner of the lateral field opposite to upper most part of rectum and surrounding fascia [9,10].
As a result of big PTV DRR this was reflected on the dose delivered to Organs at risk. we have selected bladder and bowel as representative for normal tissues, significant volumes of gluteal region as well as perineal regions were unnecessarily irradiated however where not included in dosimetric analysis. The mean urinary bladder doses for all patients were 42.6 Gy and mean V40 Gy of 79 %. Our figures where little bit similar to results of NCI Cairo for their study comparing 2D vs 3D radiotherapy in cancer rectum, for 50 patients mean urinary bladder dose and V40 Gy were 43 Gy and 73 % respectively for the 2D arm, in their study 3D was able to reduce urinary bladder mean dose to 32 Gy, and V40 to 50% only [11].
In another study from UK Corner et al reported lower doses to urinary bladder either by 2D or 3D techniques, results of V40 for 2D and 3D were 39 Gy and 34 Gy respectively [9]. For the bowel dose the mean dose were 22.65 Gy range of 14-29. v20, v30 and V40 were 50.9%, 32.4% ,26.5% respectively. In comparison to similarly designed 2D data V20, V30, V40 42.6%, 34.3%, 27.5%, our figures were higher in doses below 20 Gy. Both results were higher when compared to the same study 3D arm that was able to reduce doses to bowel by around 30% with V20, V30, V40 of 28%, 22%. 18 % respectively [9,10].
Conclusion
In preoperative irradiation of cancer rectum proper contouring and DVH data should be considered as routine to improve PTV coverage and minimize the dose to both urinary bladder and bowel. The visual assessment of isodose coverage created by skeletal landmark on DRR can compromise radiotherapy coverage specially opposite lower rectum and upper most part of illic LN and mesorctum, and its potentially more toxic.
References
- Sauer R, Becker H, Hohenberger W, Rodel C, Wittekind C, et al. (2004) Preoperative vs postoperative chemoradiotherapy for rectal cancer. N Engl J Med 351: 1731-1740.
- Gerard JP, Conroy T, Bonnetain F, Bouche O, Chapet O, et al. (2006) Preoperative Radiotherapy with or without concurrent fluorouracil and leucovorin in T3-4rectal cancers: Results of FFCD 9203. J Clin Oncol 24(28): 4620–4625.
- Bosset J, Collette L, Calais G, Mineur L, Maingon P, et al. (2007) EORTC RadiotherapGroupTrial22921. Chemotherapy with preoperative radiotherapy in rectal cancer. N Engl J Med 355(11): 1114–1123.
- Gunderson LL, Sosin H (1974) Areas of failure found atreoperation (second or symptomatic look) following curative surgery of adenocarcinoma of the rectum. Clinic pathological correlation and implications for adjuvanttherapy. Cancer 34(4): 1278–1292.
- M Garofalo, IelNaqa, R Abrams, A Apte, W Bosch, et al. (2009) Elective Clinical Target Volumes in Anorectal Cancer: An RTOG Consensus Panel Contouring Atlas R Myerson. 74(3): 824–830.
- M Kara Bucci, Alison Bevan, Mack Roach (2009) Advances in Radiation Therapy: Conventional to 3D, to IMRT, to 4D, and Beyond. CA Cancer J Clin 55(2): 117-134.
- Chao M, Gibbs P, Tjandra J, Darben P, Lim-Joon D, Jones IT, et al. (2005) Evaluation of the use of computed tomography vs conventional orthogonal x ray simulation in the treatment of rectal cancer. Australas Radiol 49: 122–126.
- Roels S, Duthoy W, Haustermans K, Penninckx F, Vandecaveye V, et al. (2006) Definition and delineation of the clinical target volume for rectal cancer. Int J Radiat Oncol Biol Phys 65(4): 1129–1142.
- Corner C, Khimji F, Tsang Y, Harrison M, Glynne-Jones R, et al. (2011) Comparison of conventional three dimensional conformal CT planning techniques for preoperative chemoradiotherapy for locally advanced rectal cancer. Br JRadiol 84(998): 173-178.
- Maria Gambacorta, Danilo Pasini, Bruce Daniel Minsky, Stefano Arcangeli, Manocci A, et al. (2013) Is two-dimensional field definition sufficient for pelvic node coverage in rectal cancer comparedto technical three-dimensional definition? Tumori 99(2): 191-198.
- Mohamed Mahmoud, Hesham A El-Hossiny, Nashaat A Diab, Marwa A El Razek (2012) Acomparative dosimetric study of neoadjuvant 3Dconformal radiotherapy for operable rectal cancer patients versus conventional 2D radiotherapy in NCI-Cairo. Chinese- German Journal of Clinical Oncology, 11(4): 224-228.






























