Case Report: 77 Year old Female with Post-Menopausal Bleeding
Sushila B Ladumor*
Clinical Imaging Department, Weil Cornel Medical College, Qatar
Submission: November 18, 2017; Published: December 07, 2017
*Corresponding author: Sushila Ladumor B, Consultant Radiologist, Clinical Imaging Department, Hamad Medical Corporation, HGH, Doha, Qatar, Assistant Professor in Clinical Radiology, Weil Cornel Medical College, Doha, (WCMC-Q) Qatar, Email: drsbladumor@yahoo.com
How to cite this article: Sushila B L. Case Report: 77 Year old Female with Post-Menopausal Bleeding. Canc Therapy & Oncol Int J. 2017; 8(2): 555734. DOI: 10.19080/CTOIJ.2017.08.555734
Abstract
About 90% of endometrial cancer is adenocarcinoma which arises from uterine epithelium. Rest of 10% are comprises of adenocarcinoma with squamous differentiation, adenosquamous carcinoma, clear cell carcinoma, and papillary serous carcinoma. Rare tumors of mesenchymal origin (Uterine sarcomas) are approximately 2-6% of all uterine malignant tumors [1]. Papillary serous adenocarcinoma of the uterus is a tumor seen as papillary projections and many times demonstrates psammoma bodies that can calcify [2]. Majority of papillary serous adenocarcinomas are seen in the ovary, CT can easily demonstrate calcified psammoma bodies. Serous adenocarcinoma is uncommon in the endometrium [3]. We report a case of a serous adenocarcinoma of the endometrium with incidentally noted mucinous cystadenoma of the ovary.
Keywords: Uterine serous carcinoma; MRI; Diffusion restriction; ADC CT; US; CA 125
Case Report
77 year old female with complaint of post-menopausal bleeding. Known case of Diabetes mellitus and hypothyroidism. Had US outside shows enlarged endometrial cavity and left adnexal cyst. Initially endometrial curettage dome: Specimen labeled as "endometrial curettage". It consists of multiple tan fragments in aggregate of about 3.5 x 3 cm. Histopathology diagnosis came: Serous carcinoma. MRI of pelvis and CT Chest and Abdomen recommended for staging. Elevated tumor marker: CA 125* H 1,580 U/mL (HI) Normal Low 0 Normal High 35 CA 15-3 H 31 U/mL (HI), CA 19-9 * 36 U/mL.
Imaging

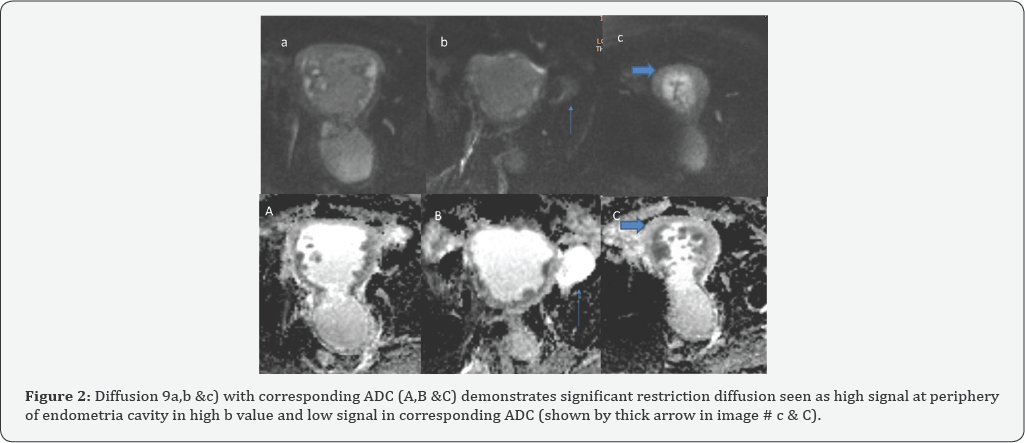
There are numerous polypoid soft tissue lesions seen along the periphery of the endometrial cavity abutting the junctional zone, the largest measuring 2.8 x 2 cm at the right lateral uterine wall (Figure 1). They demonstrate intermediate low T2 signal intensity (shown by thick arrow in image #b,c,d,e &f). The junctional zone appears infiltrated mainly on right side, no evidence of definite myometrial invasion. Parametrial fat is preserved. Urinary bladder is minimally distended. Distended cervical canal with narrowing of cervico-vaginal region (shown by thin arrow in image (a). Incidentally noted left adnexal cystic lesion with high T2 signal (shown by vertical arrow in image #b) multiple small sigmoid diverticula (shown by curved arrow in image a & b) and lower lumbar spine degenerative changes (shown by triangle in image # a) (Figure 2). Left adnexal cyst show no diffusion restriction (thin arrow in Image # b) and reveals sign through artifact in corresponding ADC (thin arrow in image # B).
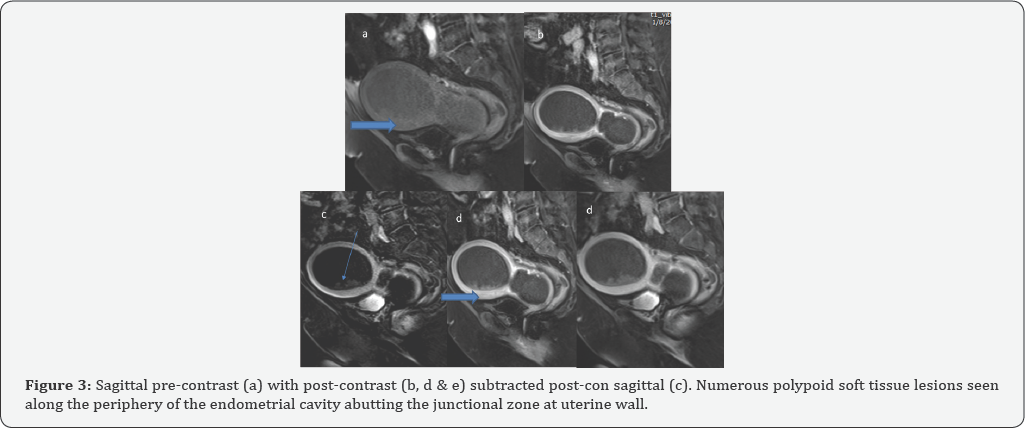
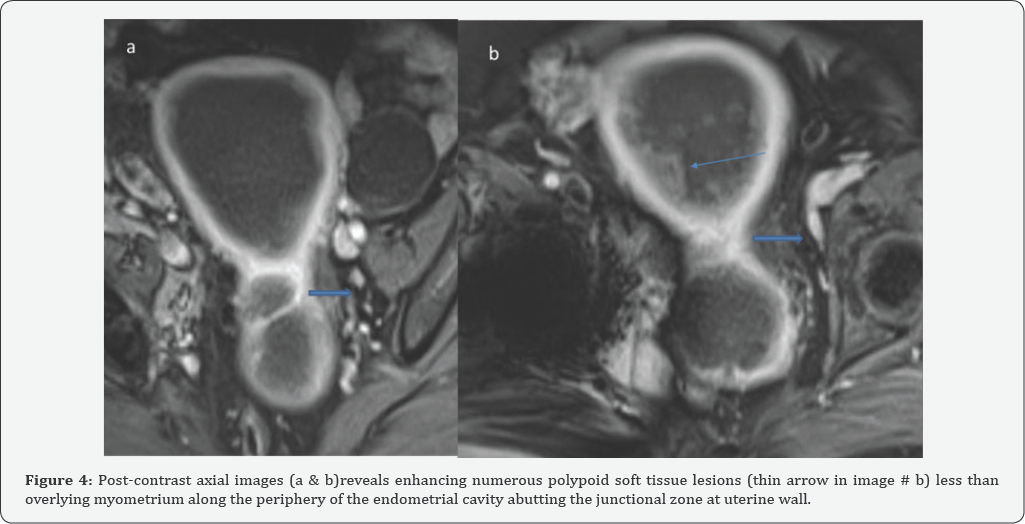
They demonstrate intermediate low T1 fat sat signal intensity (shown by thick arrow in image #a) (Figure 3). It demonstrates mild increased enhancement in the post-contrast dynamic sequences less than the overlying myometrium. The junctional zone appears infiltrated mainly on right side, no evidence of definite myometrial invasion (Figure 4). Small left pelvic lymph nodes (shown by thick arrow in image # a & b). Parametrical fat appears preserved. Re-demonstration of left adnexal non-enhancing cystic lesion (seen in Image # a). Parametrical fat appears preserved. Re-demonstration of left adnexal non-enhancing cystic lesion (vertical arrow in Image # b) (Figure 5). Incidentally noted multiple non-complicated gall stones (Thin arrow in image # a) and sigmoid diverticula (arrow head in image # b, c & d). No lung metastasis or mediastinal or abdominal lymph nodes (images are not shown).

Conclusion of MRI Pelvis
i. Distended endometrial and cervical cavity with numerous polypoid lesions along its periphery, no definite parametrial invasion. Imaging findings suggest endometrial cancer stage I. Possible stenosis at tip of cervix.
ii. Left adnexal cystic lesion, no features of malignancy.
iii. Multiple sigmoid diverticula.
Surgery was done: Report from System
Procedure: Radical hysterectomy and bilateral salpingo-ooo- phorectomy and Omentectomy Specimen Source
a. Omentum 340 gms
b. Left ovarian cyst and left ovary
c. Uterus and fallopian tubes and right ovary
d. Left extenal iliac LNs
e. Left internal iliac LNs
f. Left commen iliac LNs
g. Right internal iliac LNs
Diagnosis
a. Omentum, Omentectomy;
i. Benign mature adipose tissue.
ii. Negative for metastatic carcinoma.
b. Left ovarian cyst, left ovary, left fallopian tube, and Left salpingo-oophorectomy:
i. Mucinous cystadenoma, 6.0 cm.
ii. Minute microscopic focus of endometriosis seen.
iii. Fallopian tube with no specific histopathologic findings.
iv. Negative for malignancy.
c. Uterus, Right Tube and Ovary, Hysterectomy and Right Salpingooophorectomy (274.0 grams)
i. Serous carcinoma of the endometrium.
*Tumor size: Greatest dimension 5.0 cm
*Tumor histologic type: Serous carcinoma
*Tumor histologic grade: High grade
*Myometrial invasion: Tumor invades less than 50% of myometrial thickness
*Extent of involvement of cervix: Tumor extends to the mucosa of the anterior endocervix. Ectocervix is uninvolved by tumor
*Extent of involvement of other organs: Omentum and bilateral fallopian tubes and ovaries are uninvolved by tumor
*Margins: Uninvolved by tumor
*Lymphovascular invasion: Not identified
*Perineural invasion: Not identified
*Left External iliac lymph node, Excision: One lymph node, negative for metastatic carcinoma (0/1)
*Left Internal iliac lymph node, Excision: One lymph node, negative for metastatic carcinoma (0/1)
Discussion
Endometrial cancer is one of the common pelvic gynecologic malignancy and accounts for 13% of all cancers in women. The most common endometrial cancer is endometroid carcinoma and accounts for 75-80% and is associated with estrogen related endometrial hyperplasia. Serous carcinoma is uncommon type of endometrial cancer that comprises only 5-10% of endometrial carcinoma which usually seen in older age compared to endometrioid cell type and arises from atrophic endometrium and psamomma bodies are found in one third of cases [3]. MRI is more helpful for diagnosis and proper local staging while CT shows non-specific findings usually as enlarged heterogeneous endometrial cavity with heterogeneous enhancement. If calcification present CT is best in detection of calcification. In our case there was no calcification seen by CT. No evidence of metastatic disease seen. Incidentally noted left adnexal cyst with benign imaging feature and histopathologically proven Mucinous cysta- denoma.
Serous papillary adenocarcinoma of the endometrium can be misdiagnosed as a metastatic ovarian carcinoma due to psammoma bodies as well as this endometrial malignancy demonstrates many of the same clinical features as ovarian cancer, including a high metastatic potential and response to platinum-based chemotherapy; serum CA 125 level is a useful indicator of disease response or progression in patients with papillary serous carcinoma of the endometrium [2,4]. It is considered type II endometrial adenocarcinoma and has a clinically aggressive form with an early extension of the tumour via Fallopian tubes into the peritoneum and peritoneal seeding which accounts for its poorer prognosis compared to the other adenocarcinomas of the uterus [5].
In conclusion uterine serous carcinoma (USC) is considered type II endometrial adenocarcinoma as uncommon histologic type of mainly seen in post-menopausal women, that may present with extra uterine spread, resulting in high relapse rate and poor prognosis. MRI is most reliable in evaluation of endometrial carcinoma and evaluation of myometrial invasion, parametrial extension and cervical extension as well as lymph node detec-tion. MRI is excellent modality of choice for staging, patient selection for treatment and detection of disease recurrence.
References
- Sung Eun Rha, Jae Young Byun, Seung Eun Jung, Soo Lim Lee, Song Mee Cho, et al. (2003) CT and MRI of Uterine Sarcomas and Their Mimickers. AJR 181(5).
- IM Van Mieghem, S Gryspeerdt, M Baekelandt, B Van Holsbeeck, P Lefere, et al. (2004) Papillary Serous Adenocarcinoma of the Endometrium: CT-Pathologic Correlation. AJR 182(6).
- Prasad K Shetty (2010) Uterine Papillary Serous Carcinoma with Mature Cystic Teratoma of Left Ovary. Cogprints
- Abramovich D, Markman M, Kennedy A, Webster K, Belinson J (1999) Serum CA-125 as a marker of disease activity in uterine papillary serous carcinoma. J Cancer Res Clin Oncol 125(12): 697-698.
- Evis Sala, Suzanne Wakely, Emma Senior, David Lomas (2007) MRI of Malignant Neoplasms of the Uterine Corpus and Cervix. AJR 188(6).






























