Adjuvant Chemoradiotherapy in the Treatment of Extracranial Glioblastomas
Bora uysal, Hakan gamsiz, Ferhat dincoglan, Omer sager, Selcuk demiral and Murat beyzadeoglu
Department of Radiation Oncology, Gulhane Education and Research Hospital, Turkey
Submission: October 25, 2017; Published: November 10, 2017
*Correspondence Address: Bora uysal, Department of Radiation Oncology, Gulhane Education and Research Hospital, Department of Radiation Oncology, Etlik Kecioren 06018 Ankara, Turkey, Tel: +90 312 304 46 89; Fax: +90 312 304 46 89; Email: drborauysal@windowslive.com
How to cite this article: Bora u, Hakan g, Ferhat d, Selcuk d, Murat b. Adjuvant Chemoradiotherapy in the Treatment of Extracranial Glioblastomas. Canc Therapy & Oncol Int J. 2017; 7(5): 555722. DOI: 10.19080/CTOIJ.2017.07.555722
Abstract
Aim: The main goal is to evalaute the role of adjuvant chemoradiotherapy after surgery in the management of extracranial glioblastomas
Method and Materials: Three cases of extracranial glioblastomas that treated with adjuvant chemoraditoherapy after surgery between January 2008 and December 2015 were examined.
Results: All cases were treated with adjuvant chemoradiotherapy after surgery. They were given oral temozolomide for six courses and all tolerated medications.Two of the cases (66.7%) were male and one of the case (33.3%) was female. Mean survival was 13.3 (10-16) months. All cases were followed-up three monthly.
Conclusion: Adjuvant chemoradiotherapy after surgery should be given because of its survival advantage and local control rates.
Introduction
Glioblastomas account for 54% of all gliomas and it is one of the lethal tumors. The patients usually die in first year and only 4-5% live for five years. Symptoms are seizures, neurological findings and increased intracranial pressure. The patients with aggressive surgery have a good prognosis compared to biopsy alone in a prospective study [1]. Extracranial glioblastoma becomes 4% of all central nervous system tumors and 65% of pediatric central nervous system tumors. These tumors classified into intramedullar, intradural extramedullar and extradural [2]. Intradural extramedullar tumors are originated of connective tissue, blood vessels, tissues covering cord or cauda equina. The most seen types are ependimoma, nerve sheath tumors and vascular tumors. Metastatic tumors are often but primary tumors rarely seen in extradural region. Primary extradural tumors are originated of vertebral body and they include benign or malign bone tumors. Nonmetastatic tumors in spinal location are epidural hemangiomas, lipomas, nerve sheath tumors and lymphomas. Intramedullar tumors are originated of self tissue of spinal cord and enroll astrocytoma, ependimoma and oligodendroglioma.
Eventhough cerebral glioblastomas are often seen in midage and older population, extracranial glioblastomas are seen in second and third decades. Spinal glioblastomas are usually located in cervical and cervicothoracic and rarely in lomber region [3]. The dismal prognosis is related to intracranial extension of tumor via cerebrospinal fluid. Spinal glioblastomas are characterized with low overall survival like cerebral glioblastomas. Overall survival is nearly between six and sixteen months [4]. The major reason of death is inevitable local tumor recurrence. The management of extracranial glioblastoma is usage of long term chemotherapy following adjuvant chemoradiotherapy after surgery [5]. The major medication used in chemotherapy is temozolomide and it debulks tumor and also improve overall survival [6]. If the patient has MGMT (O6- methylguanine-DNA methyltransferase metilation) metilation, the benefit of temozolomide increases.
Materials and Methods
We evaluated three extracranial glioblastoma cases treated with adjuvant chemoradiotherapy after surgery between 2008 January and December 2015. They were given oral temozolomidefor six courses after chemoradiotherapy and all tolerated medications. Patient characteristic were shown in Table 1. The mean age of all was 25.6 (21-31). They have similar symptoms like fatigue, seizure and incontinance. The patients were diagnosed firstly with spinal Magnetic Resonance.First patient has a tumor in 9th-10th thoracal location and second one in T6-7th and third in C8-T1st. Wide excision was done for all patients in neurosurgery clinic. Infiltrative tumor was seen in tissue of medulla spinalis. Tumor is originated of atypical glial cells with giant hyperchromatic nucleus. High mitotic index and geographic field of necrosis was seen in pathological specimens. Neoplastic cells are marked with GFAP (Glial fibrilar acidic protein) (Figure 1).
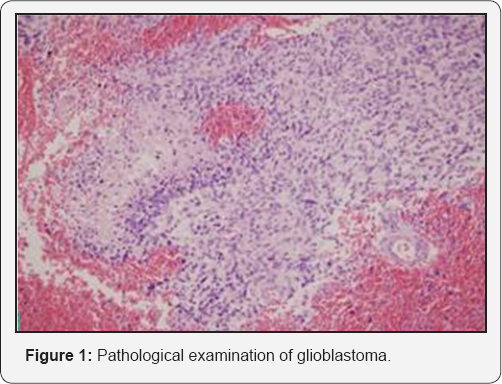
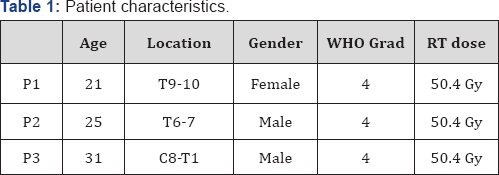
After surgical renovation, adjuvant chemoradiotherapy was given for all three patients by radiation oncologist. 5040 cGy conformal radiotherapy was given in 28 fractions by Lineer Accelerator (ELEKTA SYNERGY UK). Temolozomide was given orally everyday concomitantly with radiotherapy in doses of 75 mg/m2 and 150-200 mg/m2 after chemoradiotherapy session finalized. Adjuvant chemotherapy was given 5 days in a month for six courses.
Results
Two of the cases (66.7%) were male and one of the case (33.3%) was female. Mean survival was 13.3 (10-16) months. All cases were followed-up threemonthly. No recurrence was seen in first follow-up for three patients but it was seen in second and third follow-up. Two patients were given craniospinal radiotherapy because of cerebrospinal fluid positivity and new lesions in different spinal cerebral cerebellar lesions. The first lesion in cerebral location was in right lateral ventricule and second lesion in left cerebellar hemisphere for the other patient. Third patient had a recurrence in spinal canal and no new lesion in cerebral hemisphere but he died of thrombocytopenia.
Discussion
Extracranial glioblastomas are rare tumors. They constitute nearly 1-2 % of all spinal cord tumors and also 1-5 % of all glioblastomas [7]. Spinal glioblastomas are often reported that located in cervical and cervicothoracic region in second and third decades in the literature [8]. Although spinal glioblastomas are primary diseases, they can be the part of extension of intracranial glioblastoma. Differential diagnosis of spinal globlastoma should be discussed for the spinal malignancies. Primary disease or metastasis should be differentiated via craniospinal MR after diagnosis and then treatment algorithm can be made according to extension.
Optimal treatment of glioblastoma is adjuvan chemotherapy following chemoradiotherapy after extensive surgery. Improvement of overall survival in cerebral glioblastoma with temozolomide usage was shown in 2005 by Stupp et al. [9]. Concomitant chemoradiotherapy after total resection was delivered in cervical intramedullary glioblastoma in literature. Temozolomide was used for recurrence in the same location after 25 months. This case was died in 33rd month after surgery. Temozolomide usage was shown to improve overall survival compared to just radiotherapy [10].
Chemoradiotherapy and chemotherapy following local BCNU(carmustine) implantation to the cavity after surgery were given in multicenter study Although there is toxicity risk with usage of local chemotherapy and chemoraditoherapy, complications were not seen and side effects were same with just conventional chemoradiotherapy [11]. Bevacizumab was used for six patients in recurrent glioblastoma in an article. It was well tolerated and toxicity profile was better. Progressive disease was seen in one patient and two of all had a partial response. Stable disease was shown in three patients [12]. Adjuvant chemotherapy after concomitant chemoradiotherapy following surgery was used for six patients in a study. Grade 1 or 2 neutropenia, anemia and infection were shown in three cases. Grade 1-2 nonhematological toxicities were seen in all patients [13].
Drop metastasis of supratentorial glioblastoma was discussed in an article by Tai et al. [14] The patient was treated with concurrent chemoradiotherapy after surgery in supratentoral location and given adjuvant chemotherapy. He had a spinal metastasis 4-years after treatment and delivered local 40 Gy radiotherapy and bevacizumab. In a review by Hernandez- Duran et al. [15], the effectiveness of temozolomide was evaluated and there was a longer but not statistically significant survival difference compared to nontemozolomide group. The poor prognosis is well known for spinal glioblastoma but result of cordectomy for intramedullary glioblastoma showed 12-year survival. The same patient delivered radiotherapy and chemotherapy also [16].
Imaging algorithm for extracranial glioblastoma should be discussed. MRI is better for spinal cord and CT and 18-FDG- PET is valuable for systemic disease and CSF metastasis [17]. Our findings of few cases is consistent with literature. Large population prospective study is needed for the better results of these extracranial rare Who Grad 4 tumors.
Conclusion
Although there are few cases in literature, adjuvant chemoradiotherapy after surgery should be given because of its survival advantage and better local control rates.
References
- Laws ER, Pamey IF, Huang W, Anderson F, Morris AM, et al. (2003) Survival following surgery and prognostic factors for recently diagnosed malignant glioma: data form the Glioma Outcomes Project. J Neurosurg 99(3): 467-473.
- Halperin, Edward C, Carlos A Perez, Luther W Brady (2008) Principles and Practice of Radiation Oncology, (5th edn), Lippincott Williams & Wilkins, USA, pp. 765-777.
- H Shirato, T Kamada, K Hida, Koyanagi I, Iwasaki Y, et al. (1995) The role of radiotherapy in the management of spinal cord glioma. J Radiat Oncol Biol Phys 33(2): 323-328.
- Takara E, Ide M, Yamamato M, Imanaga H, Jimbo M, et al. (1985) A case of the intracranial and spinal dissemination of primary spinal glioma. No Shinkei Geka 13(3): 301-305.
- Al-Mefty O, Al-Rodhan NRF, Phillips RL, Mohammed El-Senossi, John L Fox (1987) Factors affecting survival of children with malignant gliomas. Neurosurgery 20(3): 416-420.
- Yeung YF, Wong GK, Zhu XL, Ma BB, Hk NG, et al. (2006) Radiation induced spinal glioblastoma multiforme. Acta Oncologica 45(1): 87-90.
- Andrews AA, Enriques L, Renaudin J, Tomiyasu U (1978) Spinal intramedullary glioblastoma with intracranial seeding. Arch Neurol 35(4): 244-245.
- Caroli E, Salvati M, Ferranate L (2005) Spinal glioblastoma with brain relapse in child: clinical considerations. Spinal Cord 43(9): 565-567.
- Stupp R, Hegi ME, Mason WP, Van den Bent MJ, Taphoom MJ, et al. (2009) Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol 10(5): 459-466.
- Tseng HM, Kuo LT, Lien HC, Liu KL, Huang CY (2010) Prolonged survival of a patient with cervical intramedullary glioblastoma multiforme treated with total resection, radiation therapy, ad temozolomde. Anticancer Drugs 21(10): 963-967.
- Bock HC, Puchner MJ, Lohmann F, Schutze M, Koll S, et al. (2010) First- line treatment of malignant glioma with carmustine implants followed by concomitant radiochemotherapy: a multicenter experience. Neurosurg Rev 33(4): 441-449.
- Chamberlain MC, Johnston SK (2011) Recurrent spinal cord glioblastoma: salvage therapy with bevacizumab. J Neurooncol 102(3): 427-432.
- Kim WH, Yoon SH, Kim CY, Kim KJ, Lee MM, et al. (2011) Temozolomide for malignant primary spinal cord glioma: an experience of six cases and a literature review. J Neurooncol 101(2): 247-254.
- Tai P, Dubey A, Salim M, Vu K, Koul R (2015) Diagnosis and management of spinal metastasis of glioblastoma. Can J Neurol Sci 42(6): 410-413.
- Hernandez-Duran S, Bregy A, Shah AH, Hanft S, Komotar RJ, et al. (2015) Primary spinal cord glioblastoma treated with temozolomide. J Clin Neurosci 22(12): 1877-1882.
- Viljoen S, Hitchon PW, Ahmed R, Kirby PA (2014) Cordectomy for intramedullary spinal cord glioblastoma with a 12-year survival. Surg Neurol Int 5: 101.
- Ginat DT, Schaefer PW (2014) Imaging guidelines and findings of extracranial glioblastoma. J Neurooncol 118(1): 9-18.






























