Hairy Cell Leukemia � A Report of Two Cases
Mamina Bhoi, Sreeya Das, Dipika Mohanty* and Asuthosh Mohapatra
Department of Haematology, Apollo Hospitals, India
Submission: October 03, 2017; Published: October 12, 2017
*Corresponding author: Dipika Mohanty, Department of Haematology, Apollo Hospitals, Bhubaneswar, Odisha, India, Tel: 08093060025 : Email: drdipika_m@apollohospitals.com
How to cite this article: Mamina B, Sreeya D, Dipika M, Asuthosh M. Hairy Cell Leukemia � A Report of Two Cases. Canc Therapy & Oncol Int J. 2017; 7(3): 555714. DOI: 10.19080/CTOIJ.2017.07.555714
Abstract
Hairy cell leukemia (HCL) according to WHO classification is a mature (peripheral), rare chronic B-cell leukemia. Annual incidence of HCL is estimated to be 0.3 cases per 10,000- [1]. This accounts for 2-3% of all leukemic cases, with about 600 new cases being diagnosed in U.S. each year. In India the cases are still very rare. We report 2 cases of Hairy cell Leukemia with different clinical presentation.
Keywords: Hairy Cell Leukemia; Splenomegaly; Bone marrow biopsy; Flow cytometry
Introduction
Hairy Cell Leukemia is known by several names like, Leukemic Reticuloendotheliosis, Lymphoid Marrow Fibrosis, Medullosplenic Histolymphocytosis of primitive appearance and Reticulum cell leukemia [2]. The median age of presentation is around 52 years, with a male predominance, and Ashkenazi Jewish males being more frequently affected (Male: Female=7:1) [3]. HCL tends to be slow growing and the neoplastic B cells infiltrate the marrow and spleen in a characteristic way. The correct identification and diagnosis of HCL is important from the therapeutic point of view due to the availability of effective chemotherapeutic agents. We report 2 cases of Hairy cell leukemia diagnosed over a period of one year in a tertiary care hospital in East India.
Case Report
Case I
A 24 year young male presented with complaints of progressive abdominal distension and intermittent jaundice, and pain abdomen since 4 months. He had swelling of lower limbs, anemia and rashes of 2 weeks duration and breathlessness since 2 days. The preliminary clinical diagnosis was "Chronic Liver Disease, hepato-splenomegaly with pancytopenia. The peripheral smear showed pancytopenia with presence of atypical lymphoid cells. The bone marrow aspirate was a dry tap and bone marrow biopsy revealed extensive infiltration of abnormal lymphocytes with small nuclei and abundant pale staining cytoplasm (Fried egg appearance). The reticulin fibers produce a net-like pattern around individual hairy cells. Immune histochemistry showed positivity of CD20 and CD22 in these cells. So the final diagnosis of Hairy Cell Leukemia was made. However the patient could not afford treatment and was lost to follow up.
Case II
A 51 year old male presented to us with complaints of jaundice, fever, breathlessness and pain and swelling of abdomen since 3 months. He also had features of renal failure. Preliminary diagnosis was, Sepsis with ARDS with unexplained hepato- splenomegaly. Peripheral smear showed Lymphocytosis with atypical lymphocytes exhibiting abundant cytoplasm and "hairy" projections and round to slightly indented nuclei with reticular chromatin and indistinct nucleoli. Since total lymphocyte count was very high, flow cytometry was performed on peripheral blood which showed CD19+,CD20+,CD22+,CD25+,CD103+,CD11c+ confirming the diagnosis of Hairy Cell Leukemia. The patient was treated with Cladrabin and achieved remission. During follow up the spleen size reduced significantly after one and half month, the total leucocyte count was 1.2x103/μl with presence of 28% of lymphocytes and absence of hairy cells.
Details of clinical and hematological findings in these two cases at presentation are given in Table 1.
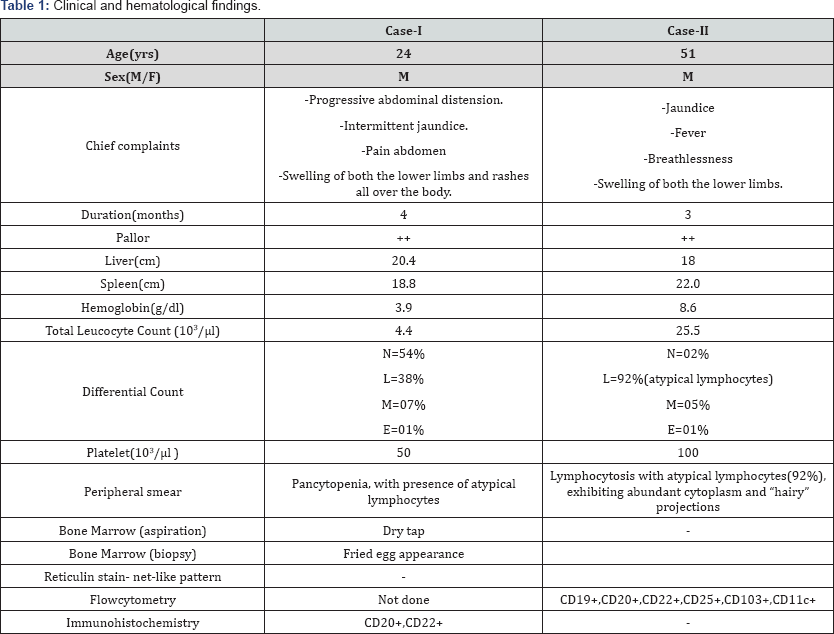
Discussion
The most common presenting feature of HCL is splenomegaly, pancytopenia with few circulating neoplastic cells. Other manifestations include hepatomegaly and recurrent opportunistic infections. While vasculitis, bleeding disorder, neurologic disorders are less common. One third to about half of the patients with HCL have been reported to be asymptomatic at the time of diagnosis. In these two cases discussed here, the clinical presentations were almost similar to each other. Both presented with jaundice and prominent splenomegaly without peripheral lymphadenopathy. But while one case had pancytopenia, the other had thrombocytopenia and lymphocytosis with 92% atypical lymphocytes. He had no history of exposure to radiation or any other toxic agent.
The normal function and precise site of origin in lymphocytic oncogeny of the hairy cell remain unknown. Prior exposure to radiation and organic solvents reportedly is more frequent among HCL patients [4]. However an earlier study on immunoglobulin heavy chain variable (IgVH) genes revealed that majority of HCL cases had somatic mutations, indicating that cells giving rise to HCL pass through germinal centre. HCL usually is associated with extensive reticulin fibers resulting in fibrosis that leads to failed attempts to obtain cellular aspirate smears (dry taps) as in our case.
The hairy cell cytoplasm usually stains strongly positive for TRAP (tartarate resistance acid phosphate). Isoenzyme 5 acid phosphatase, present in the hairy cell cytoplasm, resists decolorization by tartrate. However flowcytometry remins the modality of choice in the diagnosis of HCL with the classic immunophenotype profile consisting of bright expression of CD20 and CD22, presence of monotypic surface immunoglobulin and co-expression of CD103, CD25, CD11c and CD123. Other markers more often evaluated on IHC include DBA 44, Annexin A1, T-bet and cyclin D1. Annexin A1 is most specific marker since it is not expressed in any B cells lymphoma other than HCL. Flow cytometry was done in one of our case which showed the classical pattern of HCL [5].
Cladrabin is the first choice of treatment of HCL and it is possible to achieve long lasting disease free interval. Because of financial constrain only one out of the 2 patients took treatment.He was treated with cladrabin and achieved remission in one and half month. During the follow-up there was a significant reduction in spleen size. HCL must be differentiated from HCL - Variant and Splenic Lymphoma with Villous Lymphocytes. TRAP stain will be positive in HCL, but may or may not be positive in HCL-Variant and Splenic Lymphoma with Villous Lymphocytes. Annexin A1 is positive only in HCL, but will be negative in HCL- Variant and Splenic Lymphoma with Villous Lymphocytes.
Conclusion
It is important to clinically differentiate between HCL and other chronic B-cell lympho-proliferative disorder because of different treatment protocol as HCL is an indolent disease and asymptomatic patient needs no therapy. Indications for therapy are constitutional symptoms due to infections or due to HCL, neutropenia, thrombocytopenia and symptomatic splenomegaly. Morphological details are important to recognize HCL, as in our case, which were suspected on morphology and the diagnosis was confirmed by flowcytometry. Recognizing the features is important to avoid a misdiagnosis of this most successfully treatable leukemia.
References
- Mey U, Strehl J, Gorschuler M, Ziske C, Glasmacher A, et al. (2003) Advances in the treatment of Hairy Cel l Leukaemia. The Lancet Oncology 4(2): 86-94.
- Bouroncle BA, Wiseman BK, Doan CA (1958) Leukemic reticuloendotheliosis. Blood 13(7): 609- 630.
- Staines A, Cartwright RA (1993) Hairy-cell leukaemia: descriptive epidemiology and a case control study. Br J Haematol 85(4): 714-717.
- Oleske D, Golomb HM, Farber MD, Levy PS (1985) A case-control inquiry into the etiology of hairy cell leukemia. Am J Epidemiol 121(5): 675-683.
- Pettit AR, Zuzel M, Cawley JC (1999) Hairy-cell leukaemia: biology and management. Br J Haematol 106(1): 2-8.






























