Dosimetric Evaluation of Breathing-Adapted Radiotherapy for Right-Sided Breast Cancer
*Selcuk Demiral, Omer Sager, Ferrat Dincoglan, Bora Uysal, Hakan Gamsiz, Yelda Elcim, Bahar Dirican and Murat Beyzadeoglu
Department of Radiation Oncology, University of Health Sciences, Turkey
Submission: October 03, 2017; Published: October 12, 2017
*Correspondence Address: Selcuk Demiral, Associate Professor, University of Health Sciences, Gulhane Medical Faculty, Department of Radiation Oncology, Gn.Tevfik Saglam Cad. 06018, Etlik, Kecioren Ankara, Turkey, Tel: +90 312 304 4689; Fax: +90 312 304 4680; Email: drs.demiral@hotmail.com
How to cite this article: Selcuk D, Omer S, Ferrat D, Bora U. Dosimetric Evaluation of Breathing-Adapted Radiotherapy for Right-Sided Breast Cancer. Canc Therapy & Oncol Int J. 2017; 7(3): 555713. DOI: 10.19080/CTOIJ.2017.07.555713
Abstract
In the context of breast cancer radiotherapy, there is scant data regarding the use of Active Breathing Control (ABC) system for breathing-adapted right-sided breast cancer radiotherapy. Herein, we report a case of right-sided breast cancer treated using breathing- adapted radiotherapy with the ABC system. We report a 45-year-old woman suffering from right-sided breast cancer who received precision radiotherapy with moderate deep inspiration breath holding (mDIBH) by use of the ABC system. Two different radiation treatment plans (with and without breath holding) were generated, and dose-volume histograms were used for dosimetric comparison of dose-volume parameters in both free breathing (FB) and mDIBH plans. In our case, dosimetric comparison of free breathing and mDIBH plans revealed clearly improved critical organ sparing through incorporation of mDIBH with the ABC system, which may have potential implications for routine adoption of breathing maneuvers for radiation treatment of both left and right sided breast cancer patients.
Keywords: Breast Cancer; Radiotherapy; Active Breathing Control; Breath holding
Abbreviations: ABC: Active Breathing Control; mDIBH: Moderate Deep Inspiration Breath Holding; FB: Free Breathing; DVH: Dose-Volume Histograms; CT: Computed Tomography
Introduction
Breast cancer is the most common cancer in females worldwide as a major health concern [1-3]. Radiation therapy plays a central role in the management of breast cancer with its benefit in terms of local control and survival [4-8]. Radiation therapy for breast cancer typically targets the breast or the chestwall and lymph nodes when indicated. Since these targets are located in vicinity of critical structures such as the lungs, heart and vessels, radiation-induced toxicity and morbidity may be considered as important concerns for long-term survivors of breast cancer.
Minimizing radiation-induced adverse effects has become a more important focus given that more patients are diagnosed with early stage breast cancer due to improved screening and life expectancy is longer in the era of more effective management alternatives. Thus, incorporation of recent technology into clinical practice is gaining utmost priority for contemporary breast cancer radiotherapy. Primary goal of radiation therapy is to achieve effective doses in the target volumes with thorough sparing of normal tissues for an optimal therapeutic ratio. A variety of adaptive radiotherapy techniques and breathing maneuvers such as active breathing control may be utilized to improve treatment precision and outcomes of radiotherapy [912].
In the context of breast cancer radiotherapy, several studies have reported improved critical organ sparing and dosimetric results with adoption of breathing maneuvers particularly for left-sided breast cancer patients [11-14]. Herein, we report a case of right-sided breast cancer treated using breathing- adapted radiotherapy with Active Breathing Control (ABC) system.
Case Report
A 45-year old female patient with right-sided invasive ductal breast cancer was referred for adjuvant radiotherapy after subcutaneous mastectomy. Two radiotherapy treatment plans were generated for the patient with and without incorporation of moderate deep inspiration breathe holding (mDIBH) using the Active Breathing Control (ABC) system. Before computed tomography (CT)-simulation for radiation treatment planning, the patient received a brief training session to improve compliance with the ABC system (ABC, Elekta, UK) and to detect customized mDIBH level which was set at 75% of maximum inspiratory capacity. The patient was informed about the breath holding procedure and expected benefits. The patient received verbal instructions and practiced mDIBH since a steady breathing pattern was assured. Her mDIBH threshold and tolerated mDIBH duration was noted to be used throughout the radiation treatment course. ABC system was used to monitor breathing trace by use of the patient mouthpiece connected to the system. For CT simulation, two sets of CT images were acquired both at free breathing (FB) and mDIBH to be able to assess dosimetric impact of the ABC process.
Patient immobilization was performed by use of an angled breast-board in supine position with both arms above the head. After patient training, immobilization and positioning procedures; radiation treatment simulation was performed at the CT-simulator (GE Light speed RT, GE Healthcare, Chalfont St. Giles, UK). First CT scan was acquired at mDIBH using the ABC system which was followed by a second CT scan at free breathing (FB) to use for comparative dosimetric assessment. Slice thickness was set at 3.75 mm for both FB and mDIBH scans. Images acquired at CT simulation with both FB and mDIBH conditions were then sent to the delineation workstation by use of the network. Delineation procedures including target and critical organ contouring were performed by using the Advantage Sim MD simulation and localization software (Advantage SimMD, GE, UK). The same window level was used for contouring and same physician and physicist conducted treatment planning processes with and without mDIBH to improve consistency and concordance.
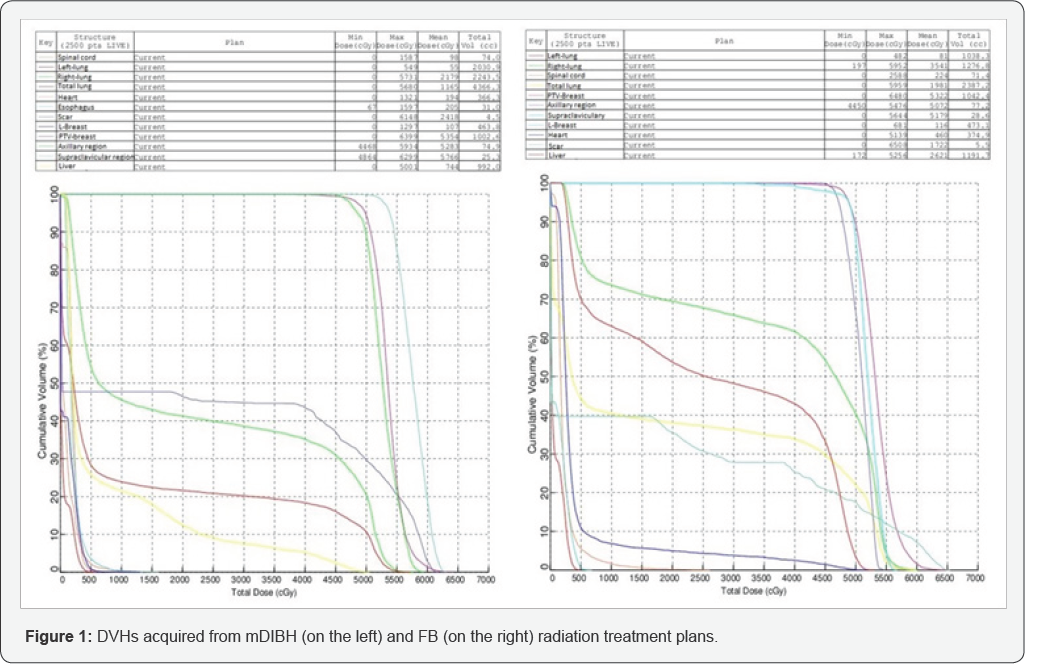
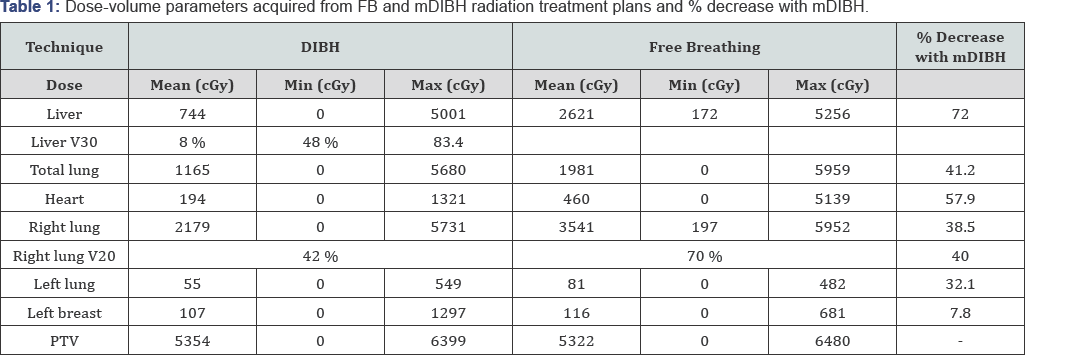
Two different radiation treatment plans (with and without mDIBH) were generated using the Precise PLAN (Elekta, UK) Treatment Planning System by use of identical beam organizations, wedges, and beam angles. Comparison of the 2 different radiation treatment plans was achieved by use of dose- volume histograms (DVH). The patient was treated using a dose of 50 Gy in 25 fractions by use of a linear accelerator (Synergy, Elekta, UK). Dose-volume parameters including mean heart doses, mean liver doses, liver V30, mean lung dose (MLD) and lung V20 parameters were extracted from the two different DVH for dosimetric comparison of FB and mDIBH radiation treatment plans. Figure 1 shows DVHs acquired from mDIBH (on the left) and FB (on the right) radiation treatment plans and Table 1 shows the dose-volume parameters acquired from FB and mDIBH radiation treatment plans and % decrease with mDIBH (Figure 1).
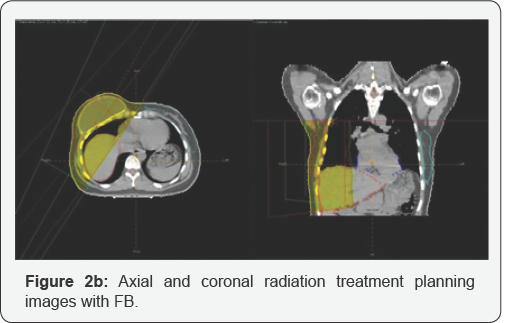
Axial and coronal radiation treatment planning images with mDIBH and with FB are shown in Figures 2a & Figure 2b, respectively.

Discussion
Dosimetric comparison of FB and mDIBH radiation treatment plans revealed improved critical organ sparing with incorporation of breath holding using the ABC system (Table 1 and Figure 1). Several studies have typically focused on left-sided breast cancer patients and reported improved critical organ sparing and dosimetric results with adoption of breathing maneuvers [11-14]. In this context, our encouraging results may have implications for adoption of breathing-adapted radiotherapy with Active Breathing Control for right-sided breast cancer patients given the scant data in the literature. Breast cancer is common among female patients and radiation- induced toxicity and morbidity is gaining more importance with improved survival of patients due to increased public awareness and more effective therapies. In this regard, methods to improve critical organ sparing are widely accepted in the discipline of radiation oncology in the modern treatment era.
ABC system has been shown to be a viable method for management of respiratory motion for precision radiotherapy and several studies have reported improved critical organ sparing by use of ABC, we have rapidly adopted this system in our clinic for both conventionally fractionated treatments and stereotactic irradiation in an effort to improve radio therapeutic outcomes [10-16]. In our case, dosimetric comparison of FB and mDIBH plans revealed clearly improved critical organ sparing through incorporation of breath holding at moderate deep inspiration with the ABC system, which may have potential implications for routine adoption of breathing maneuvers for radiation treatment of both left and right-sided breast cancer patients.
Conclusion
In conclusion, breath holding at mDIBH with the ABC system has proved to yield a favorable dosimetric advantage in our patient with right-sided breast cancer and our encouraging results may have potential implications for routine adoption of breathing maneuvers for radiation treatment of right-sided breast cancer patients in addition to left sided breast cancer patients. Further supporting evidence is clearly warranted before widespread clinical adoption of this technique.
References
- Hortobagyi GN, de la Garza Salazar J, Pritchard K, Amadori D, Haidin- ger R, et al. (2005) The global breast cancer burden: variations in epidemiology and survival. Clin Breast Cancer 6(5): 391-401.
- Coughlin SS, Ekwueme DU (2009) Breast cancer as a global health concern. Cancer Epidemiol 33(5): 315-318.
- Torre LA, Islami F, Siegel RL, Ward EM, Jemal A (2017) Global Cancer in Women: Burden and Trends. Cancer Epidemiol Biomarkers Prev 26(4): 444-457.
- Overgaard M, Jensen MB, Overgaard J, Hansen PS, Rose C, et al. (1999) Postoperative radiotherapy in high-risk postmenopausal breast-can- cer patients given adjuvant amoxifen: Danish Breast Cancer Cooperative Group DBCG 82c randomised trial. Lancet 353(9165): 1641-1648.
- Whelan TJ, Julian J, Wright J, Jadad AR, Levine ML (2000) Does locore- gional radiation therapy improve survival in breast cancer? A meta-analysis. J Clin Oncol 18(6): 1220-1229.
- Clarke M, Collins R, Darby S, Davies C, Elphinstone P, et al. (2005) Effects of radiotherapy and of differences in the extent of surgery for early breast cancer on local recurrence and 15-year survival: an overview of the randomised trials. Lancet 366(9503): 2087-2106.
- Ragaz J, Olivotto IA, Spinelli JJ, Phillips N, Jackson SM, et al. (2005) Lo- coregional radiation therapy in patients with high-risk breast cancer receiving adjuvant chemotherapy: 20-year results of the British Columbia randomized trial. J Natl Cancer Inst 97(2): 116-126.
- Danish Breast Cancer Cooperative Group, Nielsen HM, Overgaard M, Grau C, Jensen AR, et al. (2006) Study of failure pattern among high-risk breast cancer patients with or without postmastectomy radiotherapy in addition to adjuvant systemic therapy: long-term results from the Danish Breast Cancer Cooperative Group DBCG 82 b and c randomized studies. J Clin Oncol 24(15): 2268-2275.
- Sager O, Beyzadeoglu M, Dincoglan F, Demiral S, Uysal B, et al. (2015) Adaptive splenic radiotherapy for symptomatic splenomegaly management in myeloproliferative disorders. Tumori 101(1): 84-90.
- Sager O, Beyzadeoglu M, Dincoglan F, Oysul K, Kahya YE, et al. (2012) Evaluation of active breathing control-moderate deep inspiration bre- ath-hold in definitive non-small cell lung cancer radiotherapy. Neoplasma 59(3): 333-340.
- Dincoglan F, Beyzadeoglu M, Sager O, Oysul K, Kahya YE, et al. (2013) Dosimetric evaluation of critical organs at risk in mastectomized left-sided breast cancer radiotherapy using breath-hold technique. Tu- mori 99(1): 76-82.
- Sager O, Beyzadeoglu M, Dincoglan F, Oysul K, Kahya YE, et al. (2012) The role of active breathing control-moderate deep inspiration bre- ath-hold (ABC-mDIBH) usage in non-mastectomized left-sided breast cancer radiotherapy: a dosimetric evaluation. UHOD - Uluslararasi He- matoloji-Onkoloji Dergisi 22 (3): 147-155.
- Lin A, Sharieff W, Juhasz J, Whelan T, Kim DH (2017) The benefit of deep inspiration breath hold: evaluating cardiac radiation exposure in patients after mastectomy and after breast-conserving surgery. Breast Cancer 24(1): 86-91.
- Remouchamps VM, Vicini FA, Sharpe MB, Kestin LL, Martinez AA, et al. (2003) Significant reductions in heart and lung doses using deep inspiration breath hold with active breathing control and intensity modulated radiation therapy for patients treated with locoregional breast irradiation. Int J Radiat Oncol Biol Phys 55(2): 392-406.
- Gamsiz H, Beyzadeoglu M, Sager O, Demiral S, Dincoglan F, et al. (2015) Evaluation of stereotactic body radiation therapy in the management of adrenal metastases from non-small cell lung cancer. Tumori 101(1): 98-103.
- Gamsiz H, Beyzadeoglu M, Sager O, Dincoglan F, Demiral S, et al. (2014) Management of pulmonary oligometastases by stereotactic body radiotherapy. Tumori 100(2): 179-183.






























