Complete Remission of Metastatic Melanoma with Nivolumab and Complete Remission of Hepatitis C with Ledipasvir
Ying Y Zhong1, Michael Kozminsky2 and Benjamin M Brady3*
1Royal Melbourne Hospital, Australia
2Genesis Medical Centre, Australia
3Department of Medical Oncology and Haematology, Cabrini Health, Australia
Submission: August 03, 2017; Published: August 08, 2017
*Corresponding author: Benjamin M Brady, Department of Medical Oncology and Haematology, Cabrini Hospital, Level 2, Area E, 183 Wattle tree Road, Malvern, VIC, 3144, Australia, Tel: +61 3 95086161; Fax: +61 3 9509 5644; Email: bbrady@cabrini.com.au
How to cite this article: Ying Y Z, Michael K, Benjamin M B. Complete Remission of Metastatic Melanoma with Nivolumab and Complete Remission of Hepatitis C with Ledipasvir. Canc Therapy & Oncol Int J. 2017; 6(3): 555689. DOI: 10.19080/CTOIJ.2017.06.555689
Abstract
Trials for programmed death 1 receptor (PD-1) inhibitors to treat melanoma have excluded patients with chronic hepatitis C virus (HCV) infection. Here, we describe a patient with metastatic melanoma and co morbid chronic HCV, which had previously failed interferon therapy. Complete remission of metastatic melanoma was achieved after 1 year of therapy with PD-1 inhibitor nivolumab, after progression of melanoma on cytotoxic T-lymphocte antigen 4 (CTLA-4) inhibitor ipilimumab. The patient's HCV viral load remained elevated but stable during treatment with iplimumab and nivolumab. Following complete remission of melanoma with nivolumab, the patient underwent 12 weeks of targeted HCV therapy with ledipasvir and sofosbuvir, resulting in a complete virological response. The patient has ongoing complete remission of metastatic melanoma at 2 years and 9 months of nivolumab and an undetectable HCV viral load. This case highlights the ability to safely achieve a good clinical outcome for co morbid metastatic melanoma and chronic HCV with PD-1 inhibitors and new targeted HCV treatment.
Keywords: Melanoma; PD-1; Nivolumab; Hepatitis C; Remission
Abbreviations: CTLA-4: Cytotoxic T Lymphocyte Antigen 4; PD-1: Programmed Death 1 Receptor; FNA: Fine Needle Aspirate; PET: Positron Emission Tomography; MRI: Magnetic Resonance Imaging; ALT: Alanine Transaminase; AST: Aspartate Aminotransferase; HCV: Hepatitis C Virus; CT: Computed Tomography; FDG: Fludeoxyglucose
Introduction
In recent years, advances in the treatment of metastatic melanoma have been made with immune checkpoint inhibitors [1-4]. These include cytotoxic T lymphocyte antigen 4 (CTLA-4) inhibitor ipilimumab and programmed death 1 receptor (PD-1) inhibitor nivolumab. However, most clinical trials for immune checkpoint inhibitors have excluded patients with a history of active hepatitis C virus (HCV) infection, thus data on their use in patients with HCV is limited. Here we report a good outcome following nivolumab treatment of metastatic melanoma, in a patient with chronic HCV.
Case Report
A 66 year old Caucasian male presented to his General Practitioner with a right axillary mass in September 2013. A fine needle aspirate (FNA) identified malignant cells. An excisional lymph node (20mm) biopsy demonstrated metastatic melanoma. No primary melanoma was identified on physical examination. No V600 mutation was detected. Staging with a positron emission tomography (PET) and magnetic resonance imaging (MRI) of the brain confirmed stage III disease. He proceeded to an axillary completion lymphadenectomy of which 2/22 nodes were involved. Adjuvant therapy of high dose interferon was discussed however he opted for active surveillance. Past medical history was notable for HCV diagnosed in 2006 following elevated alanine transaminase (ALT) (433 IU/L) and aspartate aminotransferase (AST) (227 IU/L) levels. This occurred in the context of intravenous drug use.
HCV-specific characteristics included a high viral load (1 175 820 IU/ml) at diagnosis and 1A genotype. Other clinical parameters included IL28B polymorphism CT genotype, chronic active hepatitis but no fibrosis. In 2007 and 2008, he was treated with 6 months of pegylated-interferon monotherapy, then 48 weeks of pegylated-interferon and ribavirin combination therapy respectively. He relapsed both times post-therapy. Following this, his HCV viral load and ALT/AST continued to be monitored. They remained elevated but stable. Other significant medical history included past infection with Hepatitis B documented in 2003, and transurethral resection of prostate for benign prostatic hypertrophy.
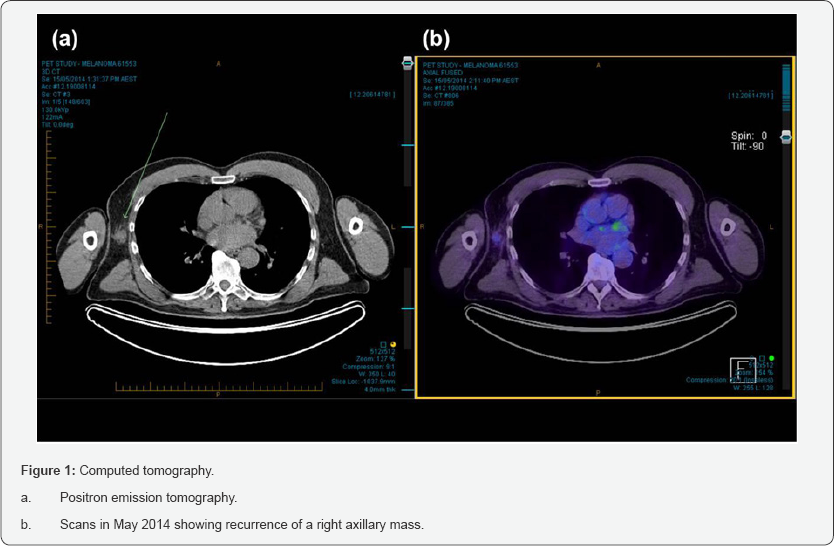
Surveillance computed tomography (CT) scan in May 2014 identified a 21mm right axillary soft tissue mass and a new 5mm left upper lung nodule (Figure 1). PET scan showed fludeoxyglucose (FDG) avidity in the right axilla and FNA of the right axillary mass confirmed melanoma recurrence. MRI brain did not demonstrate metastatic disease. The patient was treated with ipilimumab (3mg/kg, every 3 weeks). The patient's clinical course was complicated by immune-mediated hypophysitis after three cycles. Ipilimumab was discontinued. The hypophysitis resolved with dexamethasone, but the patient had persisting panhypopituitarism requiring replacement thyroxine, testosterone and cortisol. Restaging scans at this stage also showed disease progression with an increase in the size of the right axillary lesion (27mm) and multiple new pulmonary nodules in both lungs.
The patient was commenced on nivolumab (3mg/kg, every 2 weeks) in August 2014. Restaging scans after 6 months showed reduction in the axillary lesion (11mm) and lung lesions became imperceptible on CT scan. Restaging scans after 1 year showed a complete metabolic response on PET, with an ongoing complete response at 2 years. The patient elected to continue with nivolumab treatment for another year. HCV viral load & ALT/AST remained stable during nivolumab treatment. After 2 years of nivolumab with complete response, the patient commenced a 12 week course of ledipasvir (N5SA inhibitor) and sofosbuvir (viral RNA polymerase inhibitor). He achieved complete virological response and liver function tests normalized, with no evidence of cirrhosis. At the time of reporting, he has ongoing complete response after 2 years and 9 months of nivolumab and an undetectable HCV viral load.
Results and Discussion
In this case, a good clinical outcome has been achieved with complete remission of metastatic melanoma and co-morbid chronic HCV infection, using a PD-1 inhibitor and new targeted HCV therapy. Two previous cases have reported that it is safe to treat with PD-1 inhibitor pembrolizumab in chronic HCV, although in both cases there was melanoma progression or only partial response [5]. Recently, a phase 1 trial has indicated that PD-1 inhibitors may also have some activity against HCV [6]. These suggest that chronic HCV should not preclude patients with metastatic melanoma from receiving PD-1 inhibitor treatment, given the capacity to achieve good treatment outcomes.
References
- Robert C, Long GV, Brady B, Dutriaux C, Maio M, et al. (2015) Nivolumab in Previously Untreated Melanoma without BRAF Mutation. New England Journal of Medicine 372(4): 320-330.
- Weber JS, D'Angelo SP, Minor D, Hodi FS, Gutzmer R, et al. (2015) Nivolumab versus chemotherapy in patients with advanced melanoma who progressed after anti-CTLA-4 treatment (CheckMate 037): a randomised, controlled, open-label, phase 3 trial. The Lancet Oncology 16(4): 375-384.
- Hodi FS, O'Day SJ, McDermott DF, Weber RW, Sosman JA, et al. (2010) Improved survival with ipilimumab in patients with metastatic melanoma. The New England journal of medicine 363(8): 711-723.
- Robert C, Thomas L, Bondarenko I, O'Day S, Weber J, et al. (2011) Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N Engl J Med 364(26): 2517-2526.
- Davar D, Wilson M, Pruckner C, Kirkwood JM (2015) PD-1 Blockade in Advanced Melanoma in Patients with Hepatitis C and/or HIV. Case reports in oncological medicine 2015: 737389.
- Gardiner D, Lalezari J, Lawitz E, DiMicco M, Ghalib R, et al. (2013) A randomized, double-blind, placebo-controlled assessment of BMS- 936558, a fully human monoclonal antibody to programmed death-1 (PD-1), in patients with chronic hepatitis C virus infection. PLoS One 8(5): e63818.






























